- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Meningitis claimed 259,000 lives globally in 2023: The Lancet

Credit: Canva
Meningitis – the inflammation of the brain and spinal cord lining – has claimed 259,000 lives worldwide in 2023, according to a new study, published in The Lancet Neurology.
A total of 2.5 million people globally were infected with meningitis, which is also the leading infectious cause of neurological disabilities.
Importantly, children accounted for a third of the deaths, many of which were in Africa, according to research that described itself as the most comprehensive global assessment of meningitis yet.
The study comes amidst a “unprecedented” meningitis outbreak in the UK’s Kent, where two people died, and many were infected.
Meningitis: Achieving WHO 2030 goals
According to the study, global vaccination campaigns since 2000, played a significant role in reducing the number of infections and deaths by bacterial meningitis, in both high-income and low-income countries.
The Global Burden of Disease study led by an international team of researchers led by those from the University of Washington, showed that although mortality and incidence have declined significantly since 1990, progress is insufficient to meet the WHO 2030 targets.
The WHO targets a 50 percent reduction in meningitis infections and 70 percent reduction in deaths by 2030. However, a substantial meningitis burden persists. It also lags behind other vaccine-preventable diseases.
The driving factor are:
- common pathogens such as S pneumoniae and N meningitidis
- emerging non-bacterial pathogens such as Candida spp
- drug-resistant fungi.
Also read: Bacterial Meningitis May Cause Long-term Fatigue, Vision Problems, Raise Suicide Risk: Study
What Is Meningitis?
Meningitis is a serious medical condition that affects the protective membranes covering the brain and spinal cord, the meninges. While fever is not always present, it is usually considered as one of the classic symptoms of meningitis.
It is important to know the varied symptoms, causes, and treatments of meningitis for early diagnosis and proper management of the disease.
Meningitis is an infectious illness that brings about inflammation in the meninges. The most common cause of such inflammation is bacterial or viral infections, though other causes are also possible including fungal, parasitic, or non-infectious causes (autoimmune disease, head injury, or brain surgery).
Meningitis may also be caused by bacterial meningitis, which the Centers for Disease Control and Prevention (CDC) indicates can be so severe and bring about conditions like hearing loss, vision problems, and death if not received on time.
Also read: From Vaping to Worm Attack: 5 Unimaginable Ways to Contract Meningitis
Meningitis: Risk factors
As per the Lancet study, the greatest risk factors for deaths was
- low birthweight
- premature birth
- air pollution (both household and atmospheric).
Streptococcus pneumoniae, Neisseria meningitidis, non-polio enteroviruses, and other viruses were the leading causes of death, while non-polio enteroviruses caused the most cases.
To achieve further reductions in the disease globally, the researchers called for greater efforts, including:
- expanding vaccination programs,
- greater antibiotic stewardship,
- improving access to care,
- strengthening diagnostics and monitoring for meningitis.
Also read: Unique Symptoms Of Meningitis That Caused An Outbreak In Kent University
Common Symptoms Of Meningitis
- Rash
- Headaches
- Neck stiffness
- Fever
- Drowsiness
- Nausea or vomiting
- Increased sensitivity to light.
Study Shows Ebola Virus May Persist In Breast Milk For Over 3 Months After Recovery

Credit: Canva
Even after recovery, the deadly Ebola virus (EBOV) can persist for a longer duration — more than three months — in breastmilk, according to a case report.
Ebola virus disease (EVD) is a severe viral illness that has a 25 percent – 90 percent fatality rate.
Ebola in pregnancy raises significant complications ranging from spontaneous abortion to maternal and neonatal death.
In a case report published in the New England Journal of Medicine, a team of researchers from the Republic of Congo and Senegal shared the case history of a 23-year-old woman in whom Ebola was still detectable in breast milk at 14 weeks.
The case reported the rare occurrence of a pregnant woman who survived EVD with no complications, neither to the mother nor the baby. However, the deadly virus was still present in the mothers' breast milk, which cited the potential risk of post-illness transmission to infants.
What Is Ebola Virus Disease?
As per the World Health Organization (WHO), EVD is a rare but severe illness in humans and is often fatal.
People can get infected with the virus if they touch an infected animal when preparing food, or touch body fluids of an infected person such as saliva, urine, feces or semen, or things that have body fluids of an infected person like clothes or sheets.
Ebola enters the body through cuts in the skin or when one is touching their eyes, nose or mouth. Early symptoms include fever, fatigue and headache.
What Was The Case
The woman from the Democratic Republic of the Congo (DRC) contracted EBOV during pregnancy in 2019.
Soon after, she was administered monoclonal antibody therapy and was discharged after three negative reverse-transcriptase–polymerase-chain-reaction blood tests for EBOV.
The woman delivered a healthy baby at 42 weeks of gestation. No evidence of EBOV infection was found in maternal blood, amniotic fluid, vaginal secretions, or the newborn.
Ebola Detectable In Breast Milk At 14 Weeks
Yet surprisingly, the EBOV virus persisted in the placenta and breast milk.
Tests revealed that while the mother’s blood remained negative, viral RNA was still detectable in breast milk at 14 weeks after illness onset. To protect the newborn from transmission, clinicians used the drug bromocriptine to suppress lactation.
As per the World Health Organization (WHO) guidelines, the mother was also isolated from the baby and not breastfed. A prophylactic (preventive) monoclonal antibody was also given to the newborn. During follow-up, the infant exhibited no signs of infection.
Ebola Virus: WHO Guidelines
During the 2018–2020 EVD outbreak in the northeast of DRC, 3,481 confirmed cases were reported. Of these, nearly 60 percent occurred in females, and about 45 percent occurred in children below 18 years of age.
Current WHO guidance recommends that Ebola survivors avoid breastfeeding until viral clearance is confirmed.
The global health body advises women with suspected or confirmed Ebola to immediately stop breastfeeding and be prioritized for diagnostic testing.
Children exposed to Ebola through breast milk
- Must be placed under care,
- Closely monitored for symptoms over 21 days
- Fed with an appropriate breast milk substitute.
- Restarted on breastfeeding after two consecutive negative tests of breast milk.
World Doctors’ Day: Date, Origin And Significance

Credit: Canva
World Doctors’ Day is celebrated every year on March 30 to honor physicians for their dedication and compassion in saving lives and ensuring healthy communities.
Doctors are often regarded as God as they work tirelessly to save lives, even amidst conflicts or pandemics, without counting their own lives.
Often referred to as a noble profession, their mission transcends boundaries and also showcases profound human values rooted in compassion, dedication, and responsibility.
They play a significant role in building resilient, healthy societies and the world.
While there is no universally declared theme to mark the day, several campaigns are held focusing on the well-being and resilience of doctors, especially in the post-pandemic era.
World Doctors’ Day: History
World Doctors’ Day is the same as US National Doctors Day.
It was first observed in 1933 in Georgia and officially recognized in 1990 when George H. W. Bush signed it into law.
The first Doctors' Day was initiated by Eudora Brown Almond, wife of Dr. Charles B. Almond, and was adopted by the Barrow County Alliance.
The day was also observed to mark the anniversary of the first use of general anesthesia in surgery by Dr. Crawford W. Long in Jefferson, Georgia, in 1842.
The idea was then presented to the Georgia State Medical Alliance in 1933 by E. R. Harris of Winder, president of the Barrow County Alliance.
On May 10, 1934, the resolution was adopted at the annual state meeting in Augusta, Georgia.
Later, it was resolved by the Senate and House of Representatives of the US in Congress to designate March 30 as “National Doctors’ Day.”
The symbol for Doctors' Day is often the red carnation, chosen for its color that represents love, charity, and sacrifice — that highlights the profession.
The US reportedly has over 985,000 to 1 million practicing physicians.
World Doctors’ Day: Significance:
The day honors physicians' commitment, service, and contributions to healthcare, often highlighting their role in patient care. Their role is also in medical innovations that have given life to people across the globe.
It also highlights challenges faced by the physician community, like burnout, workforce shortages, and rising health demands.
Doctors are also overburdened with increasing patient load and staff shortages. Some also face workplace violence and safety concerns.
Notably, digital healthcare and evolving technologies have also added pressures and an additional burden to their practice.
Countries Celebrating World Doctors’ Day
World Doctors’ Day is celebrated on March 30 in the US, the UAE, and Australia.
India celebrates National Doctors’ Day on July 1, commemorating the birth and death anniversary of renowned physician Dr. Bidhan Chandra Roy.
Libevitug: China Rolls Out World's First Hepatitis D Monoclonal Antibody Drug
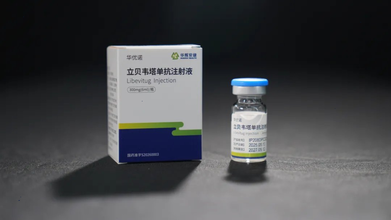
Credit: @ChinaScience/X
China has become the world’s first country to approve a monoclonal antibody drug called Libevitug to treat hepatitis D — a severe, chronic liver disease.
The drug, which was rolled out at a Beijing hospital recently, was granted conditional approval by China's National Medical Products Administration in January 2026 following priority review, Science and Technology Daily reported.
Libevitug is a monoclonal antibody developed by a team from Tsinghua University and the Beijing-based biopharmaceutical company Huahui Health.
It works by blocking hepatitis B and D viruses from entering liver cells.
Clinical trials on Libevitug demonstrated significant efficacy in virological response and normalization of liver function, with particularly notable benefits for patients with cirrhosis.
What Is Hepatitis D? What Are The Key Symptoms?
Hepatitis D, or HDV, is different from the others—it can't infect the liver by itself. It only exists in those already infected with hepatitis B, employing the outer shell of the HBV virus to replicate.
When HBV and HDV infect the liver concurrently (a co-infection) or if HDV is contracted later on superimposition of pre-existing HBV (a superinfection), the immune system is twice assaulted. The liver has to cope with more intense inflammation, resulting in more rapid fibrosis progression and a much increased risk of cirrhosis and hepatocellular carcinoma.
In individuals with co-infection, liver injury is more severe, and complications arise years sooner than in HBV mono-infection. There are no specific therapies for HDV currently, and its management relies mostly on the control of hepatitis B.
It is also possible to prevent HBV infection and thereby hepatitis D by vaccination. Antiviral therapy and close follow-up can likewise decrease the chances of serious HDV complications in those already infected with HBV.
Simultaneous infection with HBV and HDV can lead to mild-to-severe hepatitis, with signs and symptoms typically appearing 3–7 weeks after initial infection and include:
- fever,
- fatigue,
- loss of appetite,
- nausea,
- vomiting,
- dark urine,
- pale-colored stools,
- jaundice (yellow eyes)
- fulminant hepatitis.
Also read: Hepatitis On Rise In India: What Is Causing It?
How Does Libevitug Work?
Of the over 254 million chronic hepatitis B carriers worldwide, approximately 5 percent are co-infected with the hepatitis D virus, and patients with co-infection have long lacked effective targeted therapies.
Clinical trials for the drug began in 2018, with an international multi-center study launched in 2023 among patients with chronic co-infection.
The drug previously received "Breakthrough Therapy Designation" from both the Center for Drug Evaluation (CDE) of the China NMPA and the US Food and Drug Administration (FDA).
Also read: Hepatitis A To E: How Each Virus Affects Your Liver?
"Libevitug demonstrates outstanding clinical efficacy and significantly improves liver stiffness, with particularly remarkable efficacy in patients with HBV/HDV-related cirrhosis," stated Professor Niu Junqi, principal investigator of the Libevitug trial from the First Hospital of Jilin University.
"This drug aligns with the core objectives of China's Action Plan for the Prevention and Control of Viral Hepatitis (2025–2030), which aims to improve diagnosis and treatment rates for viral hepatitis and reduce the incidence of liver cancer and mortality," Junqi added.
Junqi noted that Libevitug is expected to effectively lower the risk of disease progression to advanced severe diseases such as liver cancer, drive the diagnosis and treatment of HDV in China, as well as advance the goal of eliminating viral hepatitis as a public health problem by 2030.
© 2024 Bennett, Coleman & Company Limited

