- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Michael Clarke Reveals Skin Cancer Surgery, Sparking Urgent Reminder: How To Spot The Signs Early?

Credits: Instagram/Michael Clarke
Former Australian cricket captain Michael Clarke has once again faced a health struggle that affects millions around the globe, skin cancer. Clarke, 44, posted on social media that he recently had surgery to have a suspicious growth removed from his nose. His post was not just about healing, but also an appeal: get your skin checked.
This reminder from a sports legend underscores a pressing global health issue. Skin cancer is the most common cancer diagnosed in the United States, Australia, and many other parts of the world. The good news is that when detected early, most cases are highly treatable but that early detection depends on awareness knowing what skin cancer looks like and when to seek medical help.
Clarke's recent diagnosis is not his initial experience with skin cancer. In 2006, doctors operated on him to remove suspicious marks on his face and chest. They removed them surgically before they were able to do further damage. Again in 2019, he had surgery to have cancerous tumors removed from his forehead.
Now, in 2025, his post-surgery update again emphasizes how skin cancer can be a recurring aspect for those at risk. Clarke had penned, "Skin cancer is real! Particularly in Australia. Another one removed from my nose today. A friendly reminder to have your skin checked. Prevention is better than the cure but in my case, regular check-ups and early detection is the key."

Australia has some of the highest rates of skin cancer on the planet because of high levels of UV radiation. However, Clarke's experience sounds off far beyond his native soil. In the United States alone, more than 5 million instances of skin cancer are treated annually, the American Cancer Society says.

What Is Skin Cancer?
Skin cancer occurs when skin cells grow out of control, penetrating surrounding tissue and occasionally spreading to other organs. The sun's ultraviolet (UV) light is the primary cause, though indoor tanning is also a culprit. There are three types of skin cancer with varying risks and appearances:
Also Read: Measles Alert Issued In Brisbane After Traveller Returning From Bali Tests Positive
Basal Cell Carcinoma (BCC): The most frequent one. BCC typically appears as a flesh-colored bump, pearl-like growth, or pinkish lesion. It usually develops on sun-exposed sites such as the face, neck, and arms. Although it does not spread much, if left untreated, it can produce extensive local destruction.
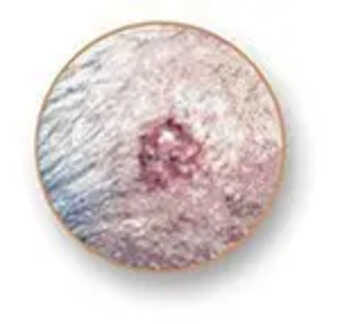
Squamous Cell Carcinoma (SCC): The second most frequent type. SCC can be a hard red bump, scaly area, or sore that closes up and reopens. It often occurs on sun-exposed areas like the ears, lips, and face. If left alone, SCC can grow and invade deeper tissues.

Melanoma: The most life-threatening form. Melanoma can develop in a pre-existing mole or as a new dark spot that appears different from surrounding markings. It grows more quickly than other skin cancers, so catching it early is paramount.

SCC can develop from a precancerous skin growth: Actinic keratoses are primarily caused by cumulative sun exposure and tend to develop on areas of the body that get the most sunlight, including the face, scalp, neck, hands, and forearms. People with fair skin are more likely to develop these patches, but they can occur in anyone with a history of significant sun exposure.

What Does Skin Cancer Look Like?
One of the difficulties with skin cancer is that its early signs are simple to overlook or assume to be harmless. However, being in a position to recognize these alterations can be the difference between life and death. General warning signals are:
- A new growth that looks like a mole, bump, or scab.
- An open sore that does not heal.
- A patch of skin that is rough or scaly.
- Alterations in a mole getting larger, darker, or becoming irregular in shape.
- Persistent itching or pain around a skin spot.
Doctors recommend following the ABCDE rule for melanoma:
Asymmetry: One half doesn’t match the other.
Border: Edges are irregular or blurred.
Color: Uneven colors—brown, black, red, or white patches.
Diameter: Larger than 6mm (about the size of a pencil eraser).
Evolving: Any mole or spot that changes in shape, size, or symptoms.
Where Skin Cancer Can Appear?
Most individuals think that skin cancer only occurs on sun-exposed skin. Although it is correct that the scalp, face, neck, arms, and hands are the most susceptible, cancers can occur on less visible locations:
- Under the toenail or fingernail.
- On the palms or soles of the feet.
- Around the genitals.
- On the back, which individuals might seldom examine themselves.
This is particularly the case for individuals with darker skin. In these individuals, melanoma and other types tend to appear on less sun-exposed areas, i.e., under nails or on the feet.
Who Is at Greatest Risk?
Anyone may get skin cancer, but certain individuals have a higher risk based on specific characteristics. People with fair skin, light hair, and light eyes are at greater risk, as are those with past histories of severe sunburns, particularly blistering. Frequent sun exposure with poor protection and tanning bed use also increase the risk of skin cancer. An inheritance pattern of the illness or compromised immune system further increases the risk. Michael Clarke's years of cricket playing in the strong Australian sunlight emphasize how long-term exposure to the sun can dramatically raise the risk of skin cancer.
Is Skin Cancer Preventable?
While you cannot alter your genes or your skin type, you can lower your risk considerably:
- Use sunscreen daily with SPF 30 or better. Apply every two hours when you're outside.
- Wear protective gear, wide-brimmed hats, sunglasses, and long sleeves.
- Seek shade between 10 a.m. and 4 p.m. when the sun's rays are strongest.
- Steer clear of tanning beds, which release cancer-causing UV radiation.
- Have your skin checked regularly, both at home and by a dermatologist.
Clarke's focus on early diagnosis is echoed in medical guidance: the sooner you detect changes, the greater the potential for effective treatment.
Why Regular Checkups Are So Important?
Skin cancer often develops silently. A small bump today may not cause pain but could evolve into something dangerous over time. Clarke’s case illustrates why vigilance is critical even after previous treatments. Recurrence is possible, and only regular screenings can catch issues before they progress.
The American Academy of Dermatology recommends annual full-body skin checks for most adults, and more frequent exams for those with higher risk factors.
Michael Clarke's candor regarding his diagnosis puts a spotlight on a public health problem that affects the entire world. His tale is not merely that of an athlete undergoing another surgery it is a reminder to all, wherever they may be in the world, that skin cancer exists, is prevalent, and is frequently preventable.
Virus Without Vaccine Hits California; No Need To Worry, Say Public Health Officials
Credits: Canva
Sick days are again piling up with a respiratory disease, not COVID-19 or the flu. This disease is most likely the one Americans have not heard of. This is HMPV or human metapneumovirus. Doctors have asked people to stay vigilant as seasonal flu virus could lead to pneumonia and bronchitis, and it is spreading in California wastewater and around the country. However, as per public health officials, there is nothing to get worried at this point.
Also Read: Is There A Link Between Your Kidney Health And Other Chronic Diseases? Study Says Yes
As per the public database WasterwaterScan Dashboard, high levels of HMPV were detected across Northern California cities. The highest levels were reported in Redwood City, whereas elevated levels were found in San Francisco Bay Area and Napa's Wine Country. What's more dangerous is that this virus is without a vaccine.
The good news is that in other parts of country HMPV remains lower. However, the Centers for Disease Control and Prevention (CDC) noted that data from October 2025 shows the cases are trending up, especially during winter and spring.
Dr. Matthew Binnicker, director of the Clinical Virology Laboratory at Mayo Clinic, as reported by The Independent said, "In the late winter, early spring, it can account for five percent to 10 percent of all the respiratory infections that we diagnose in the United States. So it's definitely out there." Experts explain that other viruses like HMPV or influenza get a chance when COVID is quieter.
Read: HMPV Virus Cases Surging In California, New Jersey: Is It Dangerous?
Virus Without A Vaccine: What Is HMPV?
HMPV was first discovered in 2001 and is part of the Pneumoviridae family along with the Respiratory syncytial virus (RSV).
HMPV most likely spreads from an infected person to others through:
- the air by coughing and sneezing
- close personal contact, such as touching or shaking hands
- touching objects or surfaces that have the viruses on them, then touching the mouth, nose, or eyes
In the US, HMPV circulates in predictable patterns each year, typically beginning in winter and lasting through spring.
The usually self-limiting and mild symptoms typically last 4 to 5 days. These include:
- cough
- fever
- nasal congestion
- shortness of breath
People at risk include:
- elderly people
- children
- people with comorbidities
"The HMPV is not deadly, and there is no evidence of mortality or a severe transmission rate," former Indian Council of Medical Research (ICMR) scientist, Dr. Raman Gangakhedkar, told IANS, during the virus's outbreak in India in 2025.
“The virus may cause pneumonitis-like illness, but the mortality rates are almost unknown so far. HMPV has a global prevalence of about 4 per cent,” he added.
While no vaccine or treatment can prevent HMPV infection, to avoid the infection, individuals must:
Practice good hygiene and cover your mouth and nose with a tissue when coughing or sneezing, or use your elbow, not your hands, for it. And wash your hands properly, especially in healthcare settings.
Why Are People Hearing About The Virus Without Vaccine Now?
The reason people have not heard about it before is because its symptoms are nearly indistinguishable from other respiratory infections, so often it could go undiagnosed. Furthermore, earlier the COVID cases and influenza cases sparked up, which deviated the attention from HMPV. Now, with the season gone, and increased awareness around respiratory illnesses, greater attention to viruses like HMPV is also paid.
1 In 7 Indians Affected By Mental Health Disorders; Govt To Launch NIMHANS-2 To Boost Care

Credit: Canva
One in seven Indians, or over 14 percent of the population, suffers from some form of mental health disorder. Amid an increasing treatment gap -- up to 90 percent -- seen in several states, especially in North India, the government today reiterated the plan of launching a second National Institute of Mental Health and Neurosciences (NIMHANS) in the northern states.
NIMHANS-2 was first announced by Finance Minister Nirmala Sitharaman during the Union Budget 2026-27, to deliver specialized care for mental health and neurological disorders in north India.
Health experts and policymakers, as part of the government-led Post-Budget Webinar series, highlighted the growing burden of mental and neurological disorders in India and also stressed the urgent need to strengthen institutional capacity to meet emerging healthcare demands.
"One in seven Indians is affected by mental health disorders, while several states continue to face a treatment gap ranging from 70 to 90 percent," the experts said.
Noting that Non-Communicable Diseases (NCDs) account for over 60 percent of deaths in the country, they added that "neurological and mental health conditions are among the leading contributors to disability-adjusted life years (DALYs)," among the citizens.
Need For Tertiary Neuro-psychiatric Care
To address these, the experts called for ramping up tertiary mental health institutions and expanding specialized services.
The session, moderated by Vijay Nehra, Joint Secretary, Ministry of Health and Family Welfare, highlighted that North India currently lacks adequate tertiary neuro-psychiatric care facilities. These include areas such as:
- advanced neuroimaging,
- neurocritical care,
- specialized neurological services
Further, making a virtual address at the Post-Budget Webinar, Union Health Minister JP Nadda also highlighted the government’s focus on strengthening mental healthcare services in the country.
"NIMHANS-2 will be established in North India to expand advanced clinical care, training, and research," Nadda said.
"In addition, the Central Institute of Psychiatry, Ranchi, and the Lokopriya Gopinath Bordoloi Regional Institute of Mental Health, Tezpur, will be upgraded as regional apex institutions to strengthen mental healthcare services in the eastern and north-eastern regions," he added.
Meanwhile, the experts also stressed the need to improve services in underserved and geographically remote regions, including the northeastern states, through better infrastructure, capacity building, and targeted deployment of trained mental health professionals.
They also discussed strategies for expanding advanced neuro-psychiatric care and reinforcing India’s overall mental healthcare ecosystem. They proposed:
- Adopting a hub-and-spoke model supported by digital health platforms
This would allow tertiary institutions and centers of excellence to provide technical guidance, specialist consultations, and clinical support to district hospitals and community-level health facilities.
"Such a model would strengthen referral pathways and ensure that specialized mental health services are accessible to people even in remote and rural areas," the experts said.
- Integrating services under Tele-MANAS
Both existing and upcoming campuses of NIMHANS must be integrated , as this will enable a robust nationwide tele-mental health network that ensures
- timely counselling,
- psychological support,
- specialist consultations
- Digital follow-up systems
The experts called for the seamless integration of healthcare facilities, aligned with the vision of the Ayushman Bharat Digital Mission and the ABHA ID ecosystem. This, they said, will
- enable continuity of care,
- Improve monitoring of patients,
- Lead to better clinical outcomes
- A national Brain-Mind Cloud Network
The Network proposed under the National Health Mission would connect premier institutions such as All India Institute of Medical Sciences (AIIMS), state medical colleges, and primary healthcare centers through a digitally integrated platform.
It could also facilitate
- unified mental health records,
- AI-based screening tools,
- data-driven clinical decision support systems,
- tele-neuro-psychiatric hubs at regional centers.
HMPV Virus Cases Surging In California, New Jersey: Is It Dangerous?
Credit: Canva
California and New Jersey in the US are seeing an uptick in cases of human metapneumovirus (HMPV) -- a virus with no vaccine or treatment.
According to the US Centers for Disease Control and Prevention (CDC), HMPV can cause upper and lower respiratory disease. There is currently no vaccine to prevent it, and no specific antiviral therapy to treat it.
"Most people will recover on their own," the agency noted, but advised people who get sick to drink plenty of liquids, stay home, and rest.
As per the CDC's respiratory dashboard, the cases of HMPV steadily ticked up since November 2025. It accounted for over 5 percent of positive tests the week of February 14 through February 21.
While HMPV is not a "new" virus, having first been discovered in 2001, cases haven't spiked to this level in the US since an outbreak in April 2025, USA Today reported.
The New Jersey Respiratory Surveillance Report cited that about 4 percent of residents in the state are testing positive for HMPV. The HMPV cases, accompanied by RSV, COVID, and flu cases, are surging, increasing the number of people seeking emergency medical care.
As per the public database, WastewaterScan Dashboard, HMPV is rampant in Northern California -- specifically San Francisco, Marin, Vallejo, Napa, Novato, Santa Rosa, Sacramento, and Davis, the Independent UK reported.
What Is HMPV? Is It Dangerous?
HMPV was first discovered in 2001 and is part of the Pneumoviridae family along with the Respiratory syncytial virus (RSV).
HMPV most likely spreads from an infected person to others through:
- the air by coughing and sneezing
- close personal contact, such as touching or shaking hands
- touching objects or surfaces that have the viruses on them, then touching the mouth, nose, or eyes
In the US, HMPV circulates in predictable patterns each year, typically beginning in winter and lasting through spring.
The usually self-limiting and mild symptoms typically last 4 to 5 days. These include:
- cough,
- fever,
- nasal congestion,
- shortness of breath
People at risk include:
- elderly people,
- children,
- people with comorbidities
"The HMPV is not deadly, and there is no evidence of mortality or a severe transmission rate," former Indian Council of Medical Research (ICMR) scientist, Dr. Raman Gangakhedkar, told IANS, during the virus's outbreak in India in 2025.
“The virus may cause pneumonitis-like illness, but the mortality rates are almost unknown so far. HMPV has a global prevalence of about 4 per cent,” he added.
While no vaccine or treatment can prevent HMPV infection, to avoid the infection, individuals must:
Practice good hygiene and cover your mouth and nose with a tissue when coughing or sneezing, or use your elbow, not your hands, for it. And wash your hands properly, especially in healthcare settings.
© 2024 Bennett, Coleman & Company Limited

