- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
- Web Stories
Can Exercise Ease Parkinson’s Symptoms? 4 Ways You Can Improve Your Mental Health

Parkinson's exercise (Credit: Canva)
Mental health plays a critical role in overall well-being, yet it is often overshadowed by physical health concerns. Many individuals, particularly those dealing with chronic illnesses like Parkinson’s disease, find it challenging to maintain a positive mental state. However, emerging research highlights the profound impact of exercise in improving both physical and mental health, even for those battling conditions like Parkinson’s.
A recent study published in the Journal of Applied Physiology reveals that exercise, whether moderate- or high-intensity, can ease symptoms of Parkinson's disease, such as fatigue, and promote mental well-being. This research opens up new possibilities for those suffering from Parkinson’s and other neurological conditions, by demonstrating how physical activity can improve not only physical function but also mental resilience.
Led by Dr. Philip Millar, a team from the University of Guelph in Ontario, Canada, conducted a study to assess the benefits of exercise for individuals with Parkinson’s disease. Dr. Millar emphasized that many patients with Parkinson's often feel overwhelmed by shame, depression, or anxiety, leading them to discontinue physical activity. This withdrawal from exercise is detrimental because, as Millar notes, “If you stop physical activity, your body adapts and you lose physical function.” However, the study underscores that exercise can have significant benefits for those living with Parkinson’s, including improved oxygen capacity and reduced fatigue.
In the study, 30 individuals between the ages of 45 and 79, all at various stages of Parkinson’s disease, participated in a 10-week exercise program. The participants were divided into three groups, each performing different intensities of exercise—either moderate- or high-intensity—three times a week at the gym. Throughout the program, Millar’s team monitored several physical and mental health metrics, such as maximal oxygen consumption, fatigue levels, gait, balance, and motor symptoms.
The results were promising. Both moderate- and high-intensity exercise significantly reduced motor symptoms by about 25%, a change that could markedly improve the quality of life for Parkinson’s patients. Fatigue levels also decreased in all participants, regardless of the intensity of their exercise regimen. While some metrics, such as gait, balance, and blood pressure, remained unchanged, the overall reduction in motor symptoms was considered highly significant.
Mental Health Benefits of Exercise
One of the lesser-discussed but critical benefits of regular exercise is its positive impact on mental health. Exercise helps regulate the production of endorphins and other neurochemicals that elevate mood, ease stress, and alleviate anxiety. This is especially crucial for individuals with Parkinson’s disease, as many experience depression and a diminished sense of control over their lives.
Dr. Millar’s research indicates that physical activity, irrespective of its intensity, can make meaningful improvements in mental health by reducing fatigue, which is a common issue for those with Parkinson’s. When fatigue is managed, patients are more likely to remain physically active, contributing further to improvements in their mental and emotional health.
Exercise and Parkinson's Disease: What's the Best Intensity?
According to the findings, individuals with Parkinson's disease need not worry about whether they are engaging in the "right" intensity of exercise. Both moderate and high-intensity training showed significant benefits, suggesting that patients can choose the level of exercise they are comfortable with. This flexibility can encourage more individuals to participate in physical activity without the fear of missing out on potential benefits.
Motor symptoms, which impact movement and coordination, were reduced in all exercise groups. Dr. Millar's team discovered that high-intensity interval training might improve gait stability and confidence, although the improvements were not directly related to cardiorespiratory fitness. In other words, the improvements in motor function could be due to increased stability and confidence rather than overall physical fitness.
The results indicate that healthcare providers should recommend exercise as part of the treatment plan for Parkinson’s disease. In fact, as Millar pointed out, the significant reduction in motor symptoms "is a very significant amount that can make a meaningful change to someone’s life.” He stresses that exercise should be considered alongside medication in managing Parkinson’s disease, just as it is in managing other chronic conditions.
Exercises That Help Ease Parkinson’s Symptoms
- Activities like brisk walking, cycling, or swimming help boost oxygen capacity and reduce fatigue in Parkinson's patients, easing motor symptoms.
- Exercises involving short bursts of intense activity improve gait stability, balance, and motor function.
- Weight lifting or resistance exercises can improve muscle strength and reduce motor symptoms, enhancing physical mobility.
- These increase cardiovascular fitness and reduce fatigue, promoting overall mental well-being in patients with Parkinson’s.
Cardiologist Warns “You Don’t Have One Heart... But 2”: How This ‘Silent’ Second Heart Could Change Your Health
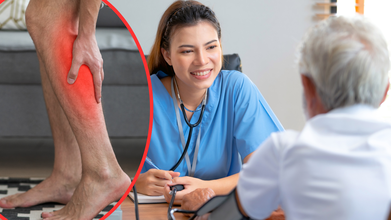
(Credit-Canva)
Our hearts works very hard to make sure we have the energy and strength to do everything we need. However, as gracious our organs are to us, most of us are not as helpful back to it. Whether it is eating junk food, not exercising, sleeping late etc. However, did you know, your heart is not the only one bearing the burden? You also have another heart in your body contributing to your health.
Heart transplant cardiologist Dr. Dmitry Yaranov calls your calf muscles your "second heart" for a very good reason. When you move your legs, these muscles squeeze and relax, which helps push blood back up toward your main heart.
This pumping action is essential for good circulation throughout your body. Without it, blood can pool in your lower legs, making it harder for your heart to work. By keeping your calf muscles strong, you help your body's entire circulatory system run smoothly, which can prevent problems like dangerous blood clots.
How Your ‘Sitting’ Lifestyle Is Killing Your Heart
Our modern lives often involve a lot of sitting, which is a big problem for our calves and our hearts. When we don't use our calf muscles, they weaken and lose their ability to pump blood effectively.
Dr. Yaranov warns that this forces your main heart to work much harder to circulate blood on its own. Over time, this extra strain can cause circulation to slow down, leading to swelling in your legs, high blood pressure, and a much higher risk of heart failure. No pill can replace the natural, powerful benefits of simply moving your body.
Simple Ways to Keep Your Calves Strong
The good news is that you can easily strengthen your calf muscles without a gym. Dr. Yaranov suggests simple changes to your daily routine. Try to walk every day to get your blood flowing.
You can also do calf raises while you're sitting at your desk or waiting in line at the grocery store. Whenever possible, choose to take the stairs instead of the elevator. These small, consistent actions will help keep your "second heart" strong and healthy for life, which in turn protects your main heart.
Calf Exercises You Can Do At Home
Calf Raises
Stand with your feet flat on the ground. Slowly lift your heels as high as you can, balancing on your toes, then lower yourself back down with control. Repeat for several repetitions to build strength.
Single Leg Calf Raise
Stand on one leg, using a chair or wall for balance. Lift your heel as high as possible, then lower it back down slowly. This variation helps improve your balance and builds strength one leg at a time.
Standing Calf Stretch
Stand a few feet from a wall and place your hands on it. Step one foot back and lean forward, keeping your back heel on the floor to feel a deep stretch in your calf. Hold for 30 seconds.
Dumbbell Calf Raise
Hold a dumbbell in each hand. Stand with your feet flat on the ground. Lift your heels and rise up onto your toes. Squeeze your calf muscles at the top before slowly lowering yourself back down.
Seated Calf Raise
Sit on a chair and place your feet flat on the floor. Place a heavy book or a dumbbell on your knees for weight. Lift your heels as high as you can, then slowly lower them for a controlled movement.
GLP-1 Alone Isn’t The Solution – Why Strength Training Is Key To Healthy Weight Loss Even With Weight Loss Injections
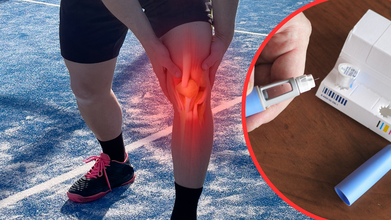
(Credit-Canva)
Weight loss injections have grown a lot in popularity as people flock to their healthcare professionals and nearby health stops to get one for themselves. Although it is rising in popularity, there are many side effects of the same. Many people find that different aspects of themselves have been altered after they took the weight loss injections along with some major bodily changes like loss of muscle mass.
Although these medications Ozempic, Wegovy, and Mounjaro—known as GLP-1 agonists—have become popular for their weight loss component, it was originally made for people with diabetes. Even though it is popular, the basic fundamentals of weight loss remain the same. A weight loss method that is devoid of exercise not only causes fat loss, but also muscle loss.
What Actually Happens When You Use GLP-1 Injection?
To understand how your body losses weight on weight loss injection, one must understand how this drug affects your body. GLP-1 agonists have three main effects on the body:
- They help the pancreas release insulin, which lowers blood sugar.
- They slow down digestion, meaning food stays in your stomach longer and releases sugar into your bloodstream more slowly.
- They affect the brain to make you feel fuller sooner and for longer.
You’re Losing Muscle, Not Fat
When you lose weight, you typically lose both fat and muscle. While some studies suggest that GLP-1s don't cause more muscle loss than other weight-loss methods, it's still a concern. A study published in the 2024 Diabetes, Obesity & Metabolism, suggested that muscle loss could be a big part of the total weight lost as much as 60% in some cases, while other studies show a much smaller amount.
Losing muscle can make you weaker, increase your risk of falls, and even reduce your bone density. This is why adding strength training to your routine is so important. It helps you build and keep muscle, which is key to a healthy and strong body.
Weight Loss Injections And Strength Training: Things To Keep In Mind
Talk to Your Doctor
Before starting any new exercise plan, always get advice from your doctor. They can give you a plan that is right for your health and the medicine you're taking.
Start Slowly
Begin with simple, gentle activities like walking. As you get stronger, you can gradually do more. Finding activities you enjoy, like dancing or cycling, will help you stick with it.
Mix It Up
A good routine includes a mix of different exercises. Try for at least 150 minutes of aerobic activity (like swimming) and two days of strength training (using weights or your own body weight) each week. Add in flexibility exercises like yoga to help with movement and prevent injury.
Monitor Your Blood Sugar
If you have diabetes, check your blood sugar before and after you work out. Your doctor can help you understand if you need to adjust your food or medication.
Stay Hydrated and Nourished
Make sure you're drinking enough water and eating healthy foods. This will fuel your body and help your muscles recover.
Listen to Your Body
Pay attention to how you feel during exercise. If you feel dizzy, unusually tired, or uncomfortable, it's a sign to slow down or stop. Your body will tell you what it needs.
No Longer Need 10,000 Steps? 2,500-4,000 Are Enough To Protect Your Heart, Says Doctor

Credits: Canva
For years, 10,000 steps a day has been seen as the gold standard for fitness. However, new medical perspectives suggest that walking fewer steps, if done correctly, can still provide significant health benefits. Hyderabad-based neurologist from Apollo Hospital, Dr. Sudhir Kumar, in a detailed post on X, explained why people should not feel discouraged if they fall short of the 10,000-step benchmark.
Rethinking the 10,000-Step Target
The 10,000-step goal originated decades ago as a marketing concept rather than a scientifically backed number. While it remains a popular target, experts now stress that the quality of walking matters as much as quantity. Walking at a brisk pace and steadily increasing one’s step count over time can greatly benefit cardiovascular health, especially for individuals with high blood pressure.
Dr. Kumar noted that the UK Biobank study, a large-scale health database, revealed how every additional 1,000 steps per day lowers the risk of heart-related conditions. Missing the 10,000 mark, therefore, does not negate the benefits of walking.
Evidence From the UK Biobank Study

According to the data, each 1,000-step increase in daily activity contributed to:
- A 17% reduction in major cardiovascular events
- A 22% lower risk of heart failure
- A 9% decrease in heart attacks
- A 24% reduction in strokes
These findings underscore that even modest increases in walking can create measurable differences in long-term health outcomes.
Brisk Walking Packs an Extra Punch
One of the most striking observations was that brisk walking during the most energetic 30 minutes of the day offered unique benefits, regardless of the total daily step count. Short bursts of faster-paced walking appeared to provide added protection against heart disease. This suggests that people who cannot reach higher step counts may still safeguard their health by incorporating short, brisk walks into their routines.
Lower Threshold, Higher Impact
Dr. Kumar emphasized that as few as 2,500 to 4,000 steps per day can significantly lower illness risk when compared with a sedentary lifestyle. This is especially encouraging for individuals who may struggle to achieve higher numbers due to age, chronic illness, or busy schedules.
He also pointed out that 1.3 billion adults worldwide live with hypertension, making walking an especially important and accessible form of preventive healthcare. Even small increases in activity, such as adding 1,000 steps daily, can meaningfully reduce complications associated with high blood pressure.
How to Start Building Healthy Habits
For those looking to improve their step counts, experts recommend a gradual approach. Increasing daily activity by 500 to 1,000 steps at a time helps individuals avoid burnout and makes it easier to sustain the habit long-term. Maintaining a brisk pace is equally important, as intensity plays a key role in cardiovascular benefits.
A Simple and Accessible Strategy
Walking requires no special equipment, gym memberships, or training, making it one of the most accessible strategies for improving heart health. Dr. Kumar concluded in his X post that people should focus less on obsessing over 10,000 steps and more on moving consistently, briskly, and progressively.
Ultimately, whether someone walks 3,000 or 9,000 steps, the key message is clear: every step counts toward better heart health.
© 2024 Bennett, Coleman & Company Limited

