- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
- Web Stories
Australia Sees Rise In Meningococcal Disease: What You Need To Know About Symptoms And Vaccination
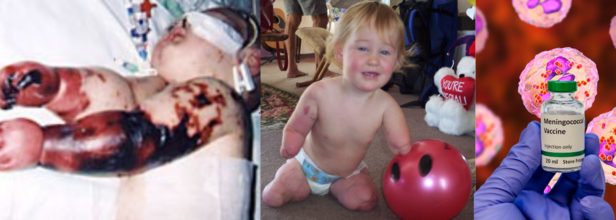
In photos: Charlotte Cleverley-Bisman, who had all four limbs partially amputated aged seven months due to meningococcal disease (Wikimedia Commons); and Canva
With the world coping with various bacterial infections, in Australia, it is the season of meningococcal disease. Last month, two Tasmanian women were hospitalized with invasive meningococcal disease, which has brought the numbers to 48.
The cases are showing an uptick, and health authorities are now urging people to watch for symptoms and to check whether they are eligible for vaccination.
What Is Meningococcal Disease?
According to the Australian Government Department of Health, Disability and Ageing, meningococcal disease is a contagious disease caused by the bacteria Neisseria meningitidis, which is also known as the meningococcal bacteria. It can develop quickly and could be fatal if not treated. Anyone with a suspected meningococcal infection needs to see their doctor immediately.
The official government website of Australia notes: "Meningococcal disease is a medical emergency. It can kill within hours, so early diagnosis and treatment are vital. Do not wait for the purple rash to appear, as that is a late stage of the disease"
However, the ray of hope is that this disease is vaccine-preventable.
What Are The Common Symptoms?
The Australian Government's Healthdirect notes that the common symptoms of this disease include:
- Fever
- Purple rash
- Meningitis
- Sepsis
- Headache
- Neck stiffness
- Light sensitivity
- Nausea and vomiting
- Loss of appetite
- Drowsiness and confusion
- Leg pain or other muscle or joint aches and pains
In babies or young children, the following can be the symptoms:
- difficulty feeding or reduced feeds
- irritability
- tiredness and floppiness
- seizures
- having a high-pitched cry
- having a bulging fontanelle (the soft spot on the top of their head)
- pale or mottled skin
The disease can live in the nose and throat of many healthy people and could spread through coughing, sneezing, sharing eating or drinking utensils, and by kissing.
Complication with the disease can also lead to:
- limb differences, or losing a limb
- skin scarring
- hearing loss
- blindness
- learning difficulties
- brain damage
Vaccination
There are different vaccines that treat the different types of this disease, including A, B, C, W, and Y. The vaccination meningococcal B and meningococcal ACWY can be taken at 6 weeks of age.
The MenACWY vaccine is a conjugate vaccine, which means it combines sugars from the outer coating of the bacteria with a protein. This helps trigger a stronger immune response, particularly in young infants.
In contrast, the MenB vaccine doesn’t use the sugar capsule. Instead, it contains four different proteins taken from the surface of the meningococcal B bacteria.
One should speak to a doctor if they have not been vaccinated at a younger age. The vaccination is recommended for:
- babies, children, teenagers and young adults
- Aboriginal and/or Torres Strait Islander people
- young adults who live in close quarters or who are current smokers
- travellers
- people who have certain medical conditions that increase their risk of meningococcal disease
- laboratory workers who work with the bacterium that causes meningococcal disease
However, as Healthdirect, an Australian Government's website notes that even with the administration of vaccine, meningococcal disease laboratory workers who work with the bacterium that causes meningococcal disease symptoms may still may linger. In such a case, go visit the hospital for further checks.
Hard-To-Manage Blood Pressure Could Now Be Treated With A Pill In Just 12-Weeks

Credits: iStock
High blood pressure, or hypertension, is one of the most common health problems worldwide yet also one of the most stubborn to control. Despite decades of new drugs and treatment combinations, millions of people remain unable to bring their blood pressure down to safe levels. Now, scientists say they may finally have an answer in the form of a pill that works in just 12 weeks.
More than 1.3 billion people globally are living with hypertension. For about half of them, blood pressure remains uncontrolled, and in roughly one in ten, it’s resistant even to multiple medications. That group faces the highest risk of stroke, heart attack, kidney disease, dementia, and premature death.
In the United States alone, nearly half of adults have elevated blood pressure, according to the CDC. For millions of these patients, lifestyle changes like reducing salt intake, exercising more, or losing weight help — but for many, even combining several prescription drugs is not enough. Resistant hypertension has long been a frustrating challenge for both patients and doctors.
Enter baxdrostat, a new pill developed by AstraZeneca. Early data suggest it may finally offer hope to patients with hard-to-control blood pressure. In a large clinical trial known as BaxHTN, which included 796 patients from 214 clinics worldwide, baxdrostat demonstrated significant blood pressure reductions over just 12 weeks.
Patients who took either 1 mg or 2 mg of the drug daily saw their systolic blood pressure drop by about 9–10 mmHg more than those who received a placebo. For context, cardiologists say that even a 5 mmHg reduction can lower cardiovascular risk significantly. Nearly four in ten patients on baxdrostat reached healthy blood pressure targets — compared with fewer than two in ten on placebo.
Professor Bryan Williams, chair of medicine at University College London and principal investigator of the trial, called the findings “a gamechanger.” He explained, “I’ve never seen blood pressure reductions of this magnitude with a drug in such a challenging patient group. This has the potential to help up to half a billion people worldwide.”
Why Existing High Blood Pressure Treatments Fall Short?
To understand why baxdrostat is making headlines, it’s important to look at how blood pressure medications currently work. Most existing drugs target the symptoms of hypertension:
- Diuretics help the body eliminate excess fluid and salt.
- Vasodilators relax arteries to reduce resistance.
- ACE inhibitors and ARBs block hormones that constrict blood vessels.
- Calcium channel blockers ease the workload of the heart by limiting calcium uptake.
While effective for many, these medications often fail in resistant hypertension. Patients may cycle through multiple classes of drugs, often taking three or more at once, and still see little improvement. Side effects like dizziness, fatigue, and swelling can make adherence harder.
How Does The Pill Tackle the Root Cause of Aldosterone?
Baxdrostat takes a different approach. Instead of targeting blood vessels or fluid directly, it blocks an enzyme critical to producing aldosterone, a hormone made in the adrenal glands.
Aldosterone regulates salt and water balance in the body, but some people produce too much of it. Excess aldosterone pushes the body to retain salt and fluid, raising blood pressure and making it unusually hard to control. Scientists have long known that aldosterone plays a central role in resistant hypertension, but attempts to block its production selectively have fallen short — until now.
Williams called baxdrostat “a triumph of scientific discovery,” noting that the drug’s precision in targeting aldosterone could explain why it worked so effectively in patients who had failed multiple treatments.
Could These Results Shift Hypertension Guidelines?
The results of the BaxHTN trial were presented at the European Society of Cardiology Congress in Madrid and published in the New England Journal of Medicine. Cardiologists at the meeting emphasized the potential impact on global treatment guidelines if baxdrostat wins regulatory approval.
Dr. Stacey E. Rosen, volunteer president of the American Heart Association, who was not involved in the trial, noted: “Resistant hypertension is incredibly difficult to manage. Having another option, especially one that directly addresses aldosterone, could be transformative.”
The safety profile of baxdrostat was also encouraging. The most common side effect observed was mild abnormalities in sodium and potassium levels, but these were rare. Unlike some older treatments, baxdrostat did not show widespread adverse effects.
Hypertension is often called the “silent killer” because it produces no obvious symptoms while quietly damaging arteries, the brain, kidneys, and heart. Globally, it contributes to more than 10 million deaths each year, making it the single most important modifiable risk factor for heart disease, the world’s leading cause of death.
Lowering blood pressure is the most effective way to reduce this burden. Studies show that every 10 mmHg reduction in systolic blood pressure cuts the risk of stroke by about 40 percent and heart disease by about 25 percent.
What Comes Next for High Blood Pressure Patients?
For patients who have struggled for years to bring their numbers down despite medication, a once-daily pill that directly addresses a root cause could be life-changing.
Historically, hypertension was most common in Western nations. Today, thanks to changes in diet and lifestyle, low- and middle-income countries carry the heaviest burden. More than half of all people with hypertension now live in Asia, including 226 million in China and nearly 200 million in India.
That global spread makes baxdrostat’s potential even more important. If approved, the drug could not only transform care in the United States and Europe but also provide a critical tool in regions where hypertension is rising fastest and healthcare access is uneven.
AstraZeneca is expected to file for regulatory approval soon. If approved, baxdrostat would be the first new type of hypertension drug in decades. Experts caution, however, that more research is needed to understand how the drug performs over longer periods and across diverse populations.
Still, the initial results have generated rare excitement in a field where progress has been incremental for years. For doctors treating resistant hypertension, a 12-week pill that lowers blood pressure by nearly 10 mmHg represents a genuine breakthrough.
As Professor Williams summed it up, “This could change how we treat one of the most important causes of death and disability worldwide. For patients and clinicians alike, that is hugely exciting.”
Celebrity Chef Gordon Ramsay Reveals Skin Cancer Diagnosis While Sharing Photo With 'A Line Of Stitches'
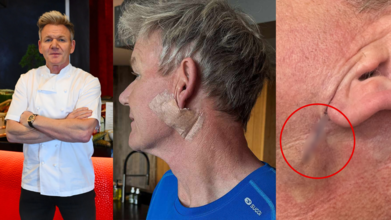
Credits: Instagram/Gordon Ramsay
Celebrity chef Gordon Ramsay, 58, has revealed he underwent surgery to remove skin cancer, using his platform to raise awareness about sun protection and early detection. In a candid Instagram post, the Michelin-starred chef thanked the medical team at The Skin Associates for their “fast reactive work” in removing a basal cell carcinoma, a common form of non-melanoma skin cancer.
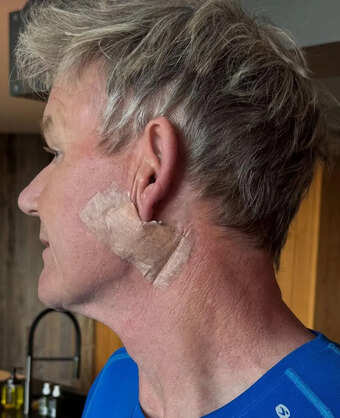
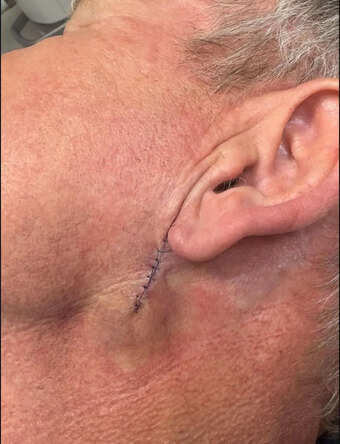
Ramsay’s post included two images, one showing a bandage below his ear and another displaying a long line of stitches stretching from his earlobe to the side of his neck. He downplayed the seriousness with humor, joking, “I promise you it’s not a facelift, I’d need a refund.” But behind the quip lies an important reminder about the dangers of prolonged sun exposure.
The diagnosis and subsequent surgery sparked widespread messages of support from fans and friends, including TV judge Robert Rinder and Ramsay’s daughter Holly, as well as a statement from Cancer Research UK applauding his openness in encouraging people to protect themselves from harmful UV rays.
In his Instagram post, Ramsay urged fans to take sun safety seriously. “Please don’t forget your sunscreen this weekend,” he wrote, highlighting a preventive measure that dermatologists stress as the most effective defense against skin cancer.
The reminder is particularly timely as skin cancer remains the most common form of cancer globally. In the United States alone, more than 3.6 million cases of basal cell carcinoma are diagnosed each year, according to the Skin Cancer Foundation. While most cases are treatable, the emotional and physical toll including scarring from surgical removal can be profound.
Cancer Research UK echoed Ramsay’s warning in a reply to his post: “Seek shade, cover up and apply sunscreen regularly and generously.”
What is Basal Cell Carcinoma?
Basal cell carcinoma (BCC) is the most common type of skin cancer, accounting for nearly 80% of non-melanoma cases. It begins in the basal cells of the epidermis, the outermost layer of skin, which are responsible for generating new skin cells.
Unlike melanoma, which is more aggressive and deadly, BCC is usually slow-growing and rarely spreads to other parts of the body. However, if left untreated, it can cause significant damage to surrounding skin, nerves, and bone. According to the Mayo Clinic, the most frequent cause of BCC is long-term exposure to ultraviolet (UV) radiation from the sun or tanning beds.
The cancer is most likely to appear on areas of the body that receive regular sun exposure—such as the face, neck, ears, scalp, shoulders, and arms.
What Are The Symptoms of Basal Cell Carcinoma?
Symptoms of basal cell carcinoma can vary in appearance, making it easy to overlook in its early stages. Common warning signs include:
- A shiny, translucent bump that may look like a pimple but doesn’t heal
- A flat, scaly patch of skin that slowly enlarges
- A sore that bleeds or oozes and keeps returning
- A scar-like area that feels firm or waxy in texture
While Ramsay did not disclose how long his lesion had been present before diagnosis, health experts emphasize that noticing these subtle changes early can make a critical difference in treatment outcomes.
Why Early Detection and Surgery Can Save Your Life?
Although basal cell carcinoma has a high treatment success rate when caught early, delayed diagnosis increases the risk of disfigurement and more complex surgical procedures. In advanced cases, BCC can grow locally invasive, disfiguring tissue and necessitating reconstructive surgery.
Early diagnosis is possible with less extensive treatments, such as excisional surgery or curettage and electrodesiccation, which destroy cancerous lesions without significantly affecting surrounding skin. More established or recurrent cases can necessitate Mohs surgery, a highly accurate procedure in which cancer cells are excised layer by layer with a microscope until only normal tissue is left.
Early treatment of BCC has an outstanding prognosis, with more than 95% cure, according to the American Cancer Society.
Ramsay's story also serves to point up the global challenge of climbing skin cancer rates. Dermatologists say the surge can be put down to more outdoor activities, tanning culture, and climatic changes that amplify sun exposure. His revelation is a flashback to cricketer Michael Clarke's ordeal when he too had to undergo surgery for skin cancer on his face after years of exposure to sun as he played cricket. Both these public figures are now calling for people to take their health seriously, emphasizing that regular skin checks can save lives.
Although individuals with light skin are at increased risk, skin cancer may occur in all races and ethnicities. In dark skin, BCC is less detectable and therefore takes longer to diagnose, presenting later in the course of disease.
International health agencies emphasize three prevention pillars: avoiding sun exposure during the midday sun, wearing protective clothes and a hat, and using a broad-spectrum sunscreen with a Sun Protection Factor of at least 30.
For Gordon Ramsay, things after his skin cancer operation appear set to go on as normal at his hectic rate of filming, flying, and maintaining an empire of restaurants and television programs. With 17 Michelin stars throughout his career and over 80 restaurants globally—including more than 20 in the US, the chef is still one of food entertainment's most influential figures.
New York City Declares Harlem Legionnaire’s Disease Outbreak Over: Here's What Killed 7 People

Credits: Canva
New York City health officials have confirmed that the Legionnaires’ disease outbreak that struck central Harlem this summer is officially over. The announcement came on August 29, 2025, three weeks after the last new case was reported.
In total, 114 people were infected, 90 were hospitalized, and seven lives were lost. Six patients remain in hospital care. City leaders say while residents can breathe easier now, the tragedy highlights urgent lessons about how New York manages its water systems.
“This is an unfortunate tragedy for New York City and the people of central Harlem,” said Mayor Eric Adams. “Our job here is not done. We must learn from this and improve our detection and response to future clusters.”
How the Outbreak Unfolded?
The outbreak began in late July, with patients reporting pneumonia-like symptoms. Over the next three weeks, dozens of people—many of them older adults or those with existing health conditions—were admitted to hospitals across Harlem.
On August 9, the last new case was identified. Since then, no additional infections have been recorded. The outbreak was declared over only after health authorities completed an extensive investigation tracing the bacteria to cooling towers on multiple buildings, including Harlem Hospital and a nearby city-run construction site.
Twelve cooling towers across ten buildings tested positive for Legionella bacteria, according to the city health department. All towers underwent emergency cleaning and disinfection.
What Is Legionnaires’ Disease?
Legionnaires’ disease is a severe form of pneumonia caused by Legionella bacteria, which thrive in warm water. Unlike the flu or COVID-19, it does not spread person-to-person. Instead, people become sick after inhaling mist or vapor from contaminated water systems. According to the U.S. Centers for Disease Control and Prevention (CDC), the bacteria can be found in:
- Cooling towers used for air conditioning in large buildings
- Hot tubs and spas
- Showers and faucets
- Decorative fountains and humidifiers
- Large plumbing systems
Under certain conditions, even supermarket misters used to keep produce fresh have been linked to infections. Mist carrying the bacteria can drift up to a mile, meaning people don’t necessarily need to enter a building to be exposed.
NYC Legionnaires’ Disease Outbreak: Why Harlem Was Hit Hard?
Investigators determined that Harlem’s outbreak likely stemmed from untreated rainwater in cooling towers at both the hospital and construction site. The bacteria multiplied in these systems, and when mist was released into the air, nearby residents and workers inhaled it.
Lawyers for two construction workers have already filed lawsuits, claiming their clients contracted the disease while working at the affected site. They allege improper maintenance allowed the bacteria to spread. The city health department has declined to comment on pending litigation.
The symptoms typically appear two to 14 days after exposure. They include cough, fever, muscle aches, headaches, and shortness of breath. Some patients also experience nausea, diarrhea, or confusion.
Of the Harlem cases, most hospitalized patients fell into high-risk categories, which explains why the outbreak had such a high hospitalization rate.
This is not the first time New York City has battled Legionnaires’ disease. A 2015 outbreak in the Bronx killed 16 people and sickened over 120. That crisis prompted new regulations requiring cooling towers to be registered, tested, and disinfected regularly.
But the Harlem outbreak revealed gaps in compliance and enforcement. Despite existing rules, city officials discovered multiple cooling towers with Legionella contamination.
New York City’s Response and New Rules
The Adams administration has announced several proposals to strengthen protections:
- Requiring building owners to test cooling towers every 30 days during operating months, instead of every 90 days
- Expanding the health department’s ability to proactively sample cooling towers across the city
- Increasing penalties for violations of cooling tower regulations
- Contracting additional labs to boost testing capacity during outbreaks
While the city moves forward, survivors and the families of those who died are left grappling with loss. Several lawsuits have already been filed, and more are expected in the coming months.
Some survivors are still recovering from long-term complications. Legionnaires’ disease, like other severe pneumonias, can leave patients with lingering lung damage, fatigue, and cognitive difficulties. For families of the seven victims, the outbreak is a painful reminder of how vulnerable urban populations can be when basic infrastructure fails.
Harlem’s outbreak underscores a critical challenge for cities worldwide: how to manage aging infrastructure and hidden health risks in water systems. Cooling towers, fountains, and plumbing are often overlooked until tragedy strikes.
Public health experts warn that climate change could worsen these risks. Warmer, wetter summers create ideal breeding grounds for Legionella bacteria. In densely populated areas like New York, even a small lapse in maintenance can put thousands at risk.
For now, central Harlem residents can feel reassured that the outbreak has ended. But the city has committed to turning this crisis into a turning point. Mayor Adams summed it up: “Public safety is at the heart of everything we do. We owe it to the families who lost loved ones to make sure this never happens again.”
© 2024 Bennett, Coleman & Company Limited

