- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Brain Teasers: Can You Spot 4 Differences In This Enchanting Scene IN 7 Seconds!

Are you ready to put your eagle eyes to the test? This enchanting image, filled with vibrant colors and magical creatures, presents a fun challenge. Take a close look at the two seemingly identical pictures and try to spot the four differences that lie hidden within.
As you scan through the images, pay close attention to details that may seem insignificant at first glance – they could be key to solving this puzzle! Look out for changes in color, shape, or items that may appear or disappear from one picture to another.

Here are the four differences:
1. The dragon's missing left horn.
2. The wolf's right ear.
3. The castle's highest tower has a missing window
4. Just behind the dragon's horn, there is a missing door.
Did you manage to find all four differences? If you did, congratulations! You have a keen eye for detail. If not, don't worry, take another look and see if you can spot them now.
New gene-editing tech corrects Canada teen’s DNA, cures rare disease in world-first
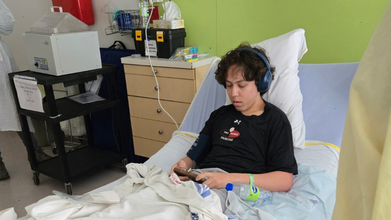
Credit: BC Children’s Hospital
In a world first, doctors have corrected the DNA of a teen from British Columbia, Canada, using new gene-editing technology under clinical trial, and cured him of his rare disease, raising hopes for scores of patients with such inherited diseases around the globe.
A new paper published recently in the New England Journal of Medicine described Ty Sperle, 19, as the first person to be cured of chronic granulomatous disease (CGD) -- a genetic condition where the body’s white blood cells do not work properly, increasing his risk of infectious disease -- by a treatment known as “prime editing”.
Ty was diagnosed with the condition at the age of five and has since been on pills, antibiotics, and antifungals. Yet, skin and soft-tissue infections, as well as an invasive bacterial infection in the lung, were quite frequent in his life.
“We have an immune system that I like to think of as a suit of armor that protects us, and because of Ty’s issue, he really had a big hole in that suit of armor,” Dr. Stuart Turvey, a pediatric immunologist at B.C. Children’s Hospital was quoted as saying in Global News.
"And so different bacterial or fungal infections could sneak in really at any time and cause serious or even life-threatening infections. So, it’s a tough disease to live with. People with this disease don’t live long, healthy lives," he added.
The Landmark Gene-Editing Technology
Ty became the first person to take part in the clinical trial, set up by US-based Prime Medicine, where doctors utilized the technology to correct an error in the DNA of patients affected by CGD.
In the trial, Ty's blood stem cells were drawn and enriched before being treated with the gene editing product.
"The product contains the necessary components to target and correct the mutation in the gene responsible for the condition, NCF1," the B.C. Children’s Hospital shared in a statement.
Ty was discharged after spending 24 days in hospital care. Follow-ups revealed that his immune system’s antimicrobial activity remained even durable six months later.
“When we got the call from Dr. Turvey, I was very excited as there were no cure options for me at that time,” Ty said.
“It was nerve-wracking for me as I was the first patient to volunteer for this procedure, and it seemed I was the only one, so it was scary," he said.
"I am thrilled with the result because I am cured of CGD and can live my life fully.”
What Is CGD?
CGD is an inherited disease that severely impacts the immune system and affects approximately one in 200,000 children.
Turvey, who treated Ty for more than a decade, said that the rare genetic disease leaves patients susceptible to infections that can turn serious, even fatal.
People with the condition have a dramatically reduced ability to fight illnesses and are extremely vulnerable to inflammatory conditions and bacterial and fungal infections.
While other treatments, such as hematopoietic stem cell transplantation, or a bone marrow transplant, can help patients with CGD, they work only in the case of an optimal healthy donor.
WHO Includes All 3 Viral Strains For Fall Flu Shot
Credits: iStock
The World Health Organization (WHO) recommended that vaccine manufacturers must change the three strains included in the vaccines for the Northern Hemisphere's next influenza season. The WHO recommended that the vaccines for the next flu season must include the new variant of the influenza virus that increased last fall too late to be included in this winter's flu shots.
As of now with the technology available, companies need at least six months time to prep for new flu shots in time for immunization campaigns beginning in the late summer or early fall.
What Is The New Strain That WHO HAs Recommended To Be Included In Vaccine Shots?
Researchers first found out about the new variant in October after this season's flu shot was already out and distributed. This was the A (H3N2) subclade K. As per Danuta Skowronski MD, a flu researcher at the British Columbia Centre for Disease Control in western Canada, this led to a mismatch in the vaccines that went into people's arms and the viruses circulating around them.
While vaccines manufactured for the Southern Hemisphere were updated as compared to those distributed in the US last year, subclade K also appeared too recently. In the Southern Hemisphere, including Australia and South Africa, flu season runs from April to October. The highest number of cases and peak activity is seen between June and September.
More About Subclade K
The A (H3N2) subclade K, also known as the "super flu" is the new version of H3N2, which has been circulated worldwide this year "acquired 7 new mutations over the summer," said Antonia Ho, a consultant in infectious disease at Scotland's University of Glasgow. As per her media statement, this "means the virus is quite different to the H3N2 strain included in this year's vaccine".
Does That Mean Earlier Flu Shots Were Useless?
Many scientists and public health experts were worried that the current flu shots in circulations used in Northern Hemisphere were useless against the subclade K. However, Skowronski says that the vaccine, in fact, worked better than imagined.
Many other experts, William Schaffner, an infectious disease expert at Vanderbilt University Medical Center, in Nashville, Tennessee, as reported by NBC, said, “Decades of data show that even when the match isn’t perfect, the flu shot continues to prevent hospitalizations, ICU admissions, and helps keep people out of the cemetery."
In an interim report released earlier this month, researchers found that the latest flu vaccine sin Canada reduced the risk of illness caused by influenza A (H3N2) viruses and severe enough to require an outpatient medical visit by 40 per cent as compared with the risk faced by unvaccinated people.
Strains Recommended For Fall Flu Shots
The WHO recommended different strains on how the latest flu shots will be manufactured. For instance, some traditional vaccines are based on viruses grown in eggs, whereas new vaccines are made in cell cultures or use recombinant or nucleic acid based technology.
The recommendation for egg-based vaccines are:
- an A/Missouri/11/2025 (H1N1)pdm09-like virus;
- an A/Darwin/1454/2025 (H3N2)-like virus; and
- a B/Tokyo/EIS13-175/2025 (B/Victoria lineage)-like virus.
The recommendation for cell culture-, recombinant protein- or nucleic acid-based vaccines are:
- an A/Missouri/11/2025 (H1N1)pdm09-like virus;
- an A/Darwin/1415/2025 (H3N2)-like virus; and
- a B/Pennsylvania/14/2025 (B/Victoria lineage)-like virus.
Over 40% Prostate Cancer Patients in India Diagnosed After Cancer Has Spread: ICMR study

Credit: Canva
A recent study by the Indian Council of Medical Research (ICMR) showed that more than 40 percent of prostate cancer patients in the country are diagnosed after the cancer has spread.
The 43 percent of late diagnosis cases indicates the significant burden of late detection of prostate cancer in the country. This can not only limit treatment options but also lead to poorer survival outcomes.
The study, published in the Indian Journal of Surgical Oncology, revealed that while more than 80 per cent began treatment within two months, but referral patients experienced longer delays.
Researchers from the ICMR’s National Centre for Disease Informatics and Research, in Bengaluru, stressed the need to strengthen referral pathways to ensure timely, stage-appropriate care.
“Our study indicates that over 80 percent of patients commence treatment within two months of diagnosis, but referral systems and delays in care persist,” said corresponding author Prashant Mathur, Director, ICMR-NCDIR, in the paper.
“To address these challenges, the healthcare system must prioritize improving referral efficiency, reducing administrative bottlenecks, enhancing coordination through digital health records, and multidisciplinary tumor boards,” the authors added.
Age, The Strongest Risk Factor For Prostate Cancer
The ICMR study is based on an analysis of 9,347 cases from 96 hospitals under the National Cancer Registry Program.
The researchers found that 75.6 percent of total prostate cancer cases occurred in the age group of 60–80 years, indicating that advanced age remains the biggest risk factor for the condition.
As life expectancy increases, more men reach the higher-risk age group, but awareness and screening practices have not scaled proportionately.
Adenocarcinoma was the most common pathology, constituting 77 percent of cases.
It is the most common form of prostate cancer, accounting for over 95 per cent of all cases. It develops in the gland cells that produce prostate fluid and typically grows slowly over several years.
Further, the ICMR researchers noted that about 57 percent of cases were diagnosed with localized (29.9 percent) or locoregional (27 percent) cancer.
Thirty percent underwent surgical treatment, and 22 percent received radiation therapy. Systemic therapy was the most common single modality treatment.
“Early detection and streamlined referral pathways are essential to improve prostate cancer outcomes in India,” the researchers said.
Prostate Cancer And Its Prevalence In India
Prostate cancer forms in the cells of the prostate -- a gland found only in males and a part of the male reproductive system. It lies below the urinary bladder and in front of the rectum.
Nearly all prostate cancers develop from glandular cells (adenocarcinomas).
Globally, prostate cancer is the most frequently diagnosed cancer among men in 112 countries and the leading cause of cancer death in 48 countries. In 2020, an estimated 1.4 million new cases of prostate cancer and 0.37 million deaths were reported worldwide.
In India, it is the second most common cancer among men, accounting for more than 60 percent of the prostate cancer burden in South-Central Asia. As per the ICMR data, the country reported 34,540 incidences of prostate cancer and 16,783 deaths.
Prostate cancer symptoms include urinary difficulty, a weak stream, or blood in the urine.
As prostate cancer is a slow-developing disease, it often causes no symptoms during the early-stage, leading to delayed medical consultation.
Other reasons for late detection in India include low awareness, limited routine screening -- PSA (prostate-specific antigen) programs; social stigma and hesitation due to embarrassment or cultural taboos.
Lack of access to specialist care, diagnostic facilities, and cancer centers, especially in rural populations, coupled with cost and referral gaps, also leads to delay in diagnosis.
© 2024 Bennett, Coleman & Company Limited

