- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
COVID Turns 5: Things We Have Learned And What Remains Unknown

Five years have come and gone since the world first got acquainted with the virus that would eventually be known by the name SARS-CoV-2. Originating in Wuhan, China, in late 2019, the new coronavirus had unleashed a global pandemic which had laid bare vulnerabilities in public health systems, redesigned societal norms, and left a very complex medical and emotional legacy that humanity grapples with today. The virus remains a dynamic force in the public health domain, demanding attention and adaptation from the end.
Tracing the Origins of SARS-CoV-2 and Unanswered Questions
The origin of SARS-CoV-2 is the most highly contested area of discussion for the origin of the pandemic. It is common knowledge that bats are a known reservoir for coronaviruses, and it is possible that they could have transmitted the virus to humans through intermediary species such as raccoon dogs, civet cats, or bamboo rats. This is similar to the mode by which the SARS virus was transmitted in the early 2000s.
However, other theories indicate that the virus could have leaked from a laboratory, as Wuhan is a hub for coronavirus research. Political tensions and lack of access to crucial data have further made it difficult to identify the origins of the virus. According to WHO Director Tedros Adhanom Ghebreyesus, the true origins might never be known, at least not in years to come.
Assessing the Global Human Toll and the Pandemic's Impact
The human cost due to COVID-19 has been so massive, with the World Health Organization now estimating that well over 20 million people died from the coronavirus pandemic, despite official records having reported more than 7 million deaths.
In the United States, the virus still disproportionately affects the older population. Last year, deaths averaged at around 900 per week. The majority of hospitalizations and deaths are people aged 75 years and above. Though mortality rates have reduced, the persistent presence of the virus underlines the continued public health interventions that are needed.
Also Read: New Virus Outbreak In China After COVID-19: What is HMPV? Know Symptoms And Preventive Measures
Rapid Development and Role of Vaccines
The rapid development of COVID-19 vaccines marked a watershed moment in medical science. Leveraging mRNA technology, scientists at Pfizer and Moderna achieved what was previously unimaginable: effective vaccines available within a year of the virus's identification. These vaccines have been instrumental in reducing severe disease and death, with over 13 billion doses administered globally since 2021.
Despite these success stories, vaccine limitations remain. The immunity declines gradually and requires a booster to deal with emerging variants.
Public frustration with repeated vaccination has once again necessitated a need for next-generation products including nasal vaccines which may better prevent infection.
Variants Strains and Their Challenges
As viruses replicate, genetic mutations occur, giving rise to variants. From alpha to omicron, SARS-CoV-2 has consistently adapted, posing challenges for scientists and public health officials.
Omicron, which emerged late in 2021, was on average less virulent than its predecessor, delta, partly because of increased population immunity. But its subvariants, such as XEC—now dominant in the U.S.—continue to demand attention. While existing vaccines and treatments remain effective against many of these variants, the virus's evolution underscores the importance of ongoing surveillance and vaccine updates.
Challenges of Long COVID
Long COVID represents the puzzling, often debilitating after-effect of this virus. An illness that already affects millions across the globe presents as long-standing symptoms: including fatigue, impairments to thinking and cognition--often termed "brain fog," and cardiovascular difficulties. Such manifestations can be persisting for months or even years, drastically diminishing quality of life.
Research into long COVID is in its infancy. There is some evidence that vaccination reduces the risk, but it can occur in anyone, of any age, and even without severe infection. Some emerging evidence may relate to the presence of residual virus in some, but not all, affected individuals; however, this does not explain all cases. The discovery of effective treatments should be the priority.
Lessons Learned From COVID-19 For Future Pandemics
COVID-19 has exposed the disparities in global healthcare systems, from unequal vaccine distribution to unequal access to life-saving treatments. It has also highlighted the importance of scientific collaboration and the resilience of communities in the face of unprecedented challenges.
Looking ahead, public health priorities must include the development of universal coronavirus vaccines, strengthening of global surveillance systems, and expansion of healthcare infrastructure to address future pandemics. Equally critical is combating misinformation, which has eroded public trust and hampered vaccination campaigns.
As we look back on five years since SARS-CoV-2 burst onto the world stage, it is evident that the virus has been a serious opponent. Despite vaccines and natural immunity reducing the immediate threat, an evolving virus, along with the impact of long COVID, reminds us of the problems yet to be overcome.
Two Passengers From Singapore Airlines Arrive In New Zealand With Measles
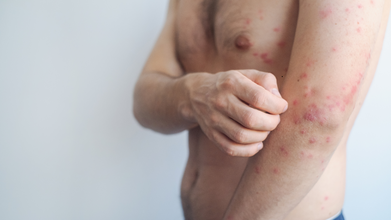
Credits: Canva
Two passengers travelling in Singapore airlines arrived in New Zealand with measles symptoms. However, reported The Strait Times, that they are not linked to any other known cases, as noted by the Communicable Disease Agency (CDA).
The agency told the media outlet that it was notified on February 25 that two Singapore Airlines (SIA) passengers infected with measles landed in Auckland, New Zealand. Both were from the same household and flown from Hyderabad, India. They transited in Singapore for two hours before boarding an SIA flight to Auckland.
CDA investigation also revealed that these two cases remained in the transit area at Changi Airport. Associate Professor Lim Poh Lian, group director of the CDA's Communicable Disease Programmes, as reported by The Strait Times noted that the individuals were reported to have developed symptoms only while onboard the flight from Singapore to Auckland.
New Zealand media earlier reported that the two cases were detected after the individuals arrived in Auckland on flight SQ281 on February 17. The country’s public health authority began tracing passengers seated in rows 31 to 46 on the same flight, along with people who were present in the waiting area of Waitakere Hospital’s Emergency Department on February 21.
“Based on the onset of their symptoms, they were infected before transiting through Singapore and are not linked to any other known measles cases in Singapore,” Prof Lim said.
She also clarified that their time in transit through Singapore did not coincide with that of a previously reported measles case involving a passenger who had passed through Singapore en route to Los Angeles in the United States.
What Is Measles?
Measles has a high transmissibility, and high measles immunity levels are required to prevent sustained measles virus transmission.
This is why herd immunity for measles could be easily breached.
It easily spreads from one infected person to another through breathes, coughs or sneezes and could cause severe disease, complications, and even death.
Symptoms include:
- High fever
- Cough
- Runny Nose
- Rash all over the body
The most unique symptom or the early sign of measles in the Koplik spots. These are tiny white dots that look like grains of salt on red gums inside the cheeks that appear before the red rash starts to appear on a person's face and then the body.
Furthermore, the symptoms of measles are also characterized by the three Cs:
- Cough
- Coryza or runny nose
- Conjunctivitis or red and water eyes
Update On The Passengers Who Landed In New Zealand
The passenger on flight SQ38 arrived at Los Angeles International Airport at about 7pm on February 9, after a roughly two-and-a-half-hour transit at Changi Airport following a flight from Cambodia.
Prof Lim said the most effective protection against measles is to be fully vaccinated before travelling. She also advised travellers to practise good hygiene, such as washing hands regularly and avoiding close contact with anyone who is unwell.
Anyone who develops symptoms like fever, rash, cough, red or watery eyes, or a runny nose should wear a mask, seek medical care promptly, and inform their doctor about their recent travel and any possible exposure to measles, she added.
In response to queries, Singapore Airlines told The Straits Times that it is working closely with the authorities but cannot share specific details due to customer confidentiality.
Fact Check: Common Myths Around HPV Vaccine And How It Will Prevent Cervical Cancer
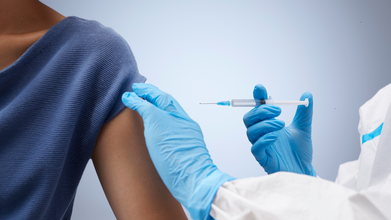
Credit: Canva
In a major push towards eliminating cervical cancer from India, Prime Minister Narendra Modi today launched the nationwide Human Papillomavirus (HPV) vaccination program for girls aged 14 years.
The new vaccination drive comes as cervical cancer remains the second most common cancer among women in India, with nearly 80,000 new cases and over 42,000 deaths reported annually. As per data from the ICMR-National Cancer Registry Program (NCRP), an estimated 78,499 new cases and 42,392 deaths were reported in 2024.
Calling it a "decisive step”, the government noted that it is aimed at “strengthening the vision of ‘swasth nari’ (healthy women) while being rooted in scientific evidence, strict regulatory oversight and global best practices”.
“India's vaccination drive reflects safety, responsibility, and long-term commitment to women’s health,” it added.
The national program will use Gardasil, a quadrivalent HPV vaccine that protects against HPV types 16 and 18, which cause cervical cancer, as well as types 6 and 11.
However, social media has been rife with concerns around the safety of the vaccine, its impact on women’s reproductive health, among others.
HPV Vaccine: The Myths And Facts
Myth: HPV vaccines can cause severe side effects and even death.
Fact: The HPV vaccines come with a “confirmed strong safety record”.
“Extensive global monitoring shows a strong safety profile supported by scientific reviews. Independent evaluations have found no causal link between vaccination and chronic harm, strengthening confidence in its continued use worldwide,” the government said.
The vaccine has been licensed in India since 2008, and the new rollout follows recommendations by the World Health Organization (WHO) and approvals from the National Technical Advisory Group on Immunization (NTAGI).
“HPV vaccines have been given to hundreds of millions globally. Extensive post-marketing surveillance shows an excellent safety profile, with no causal link to serious adverse outcomes. The evidence is robust, transparent, and reassuring,” Dr. CS Pramesh, Director of the Tata Memorial Hospital, Mumbai, shared in a post on the social media platform X.
Myth: The HPV vaccine has never been used in India
Fact: The vaccine has been in use in India. It has been administered for years since 2008 with successful implementation in states like Punjab, Sikkim, and Tamil Nadu.
Myth: HPV vaccination does not prevent cervical cancer
Fact: The HPV vaccine has been proven to prevent cervical cancer
Studies show a 65 percent drop in cervical cancer cases among US women between 2012 and 2019 and an 88-89 percent reduction in precancerous lesions among Scottish women over a decade.
Countries with early HPV vaccine adoption have also shown large declines in HPV infection, high-grade cervical lesions, and cervical cancer incidence.
"Even when considering the rarest side effects, HPV vaccines are overwhelmingly safe. The protection they offer against cervical cancer far outweighs the minimal risks. Parents are encouraged to vaccinate their daughters on time," said Dr. Neena Malhotra, Professor and Head of Department, Department of Obstetrics and Gynecology, AIIMS New Delhi on X.
Myths: Are Multiple Doses Needed?
Fact: A single dose of the quadrivalent HPV vaccine is effective. It provides strong protection against HPV infection. It helps prevent cervical cancer.
“Strong global and Indian scientific evidence confirms that a single dose provides robust and durable protection when administered to girls in the recommended age group," the government said.
PM Modi Launches Nationwide Free HPV Vaccination Drive; A Landmark Step, Says WHO

Credit: Health Ministry
Prime Minister Narendra Modi today launched the nationwide Human Papillomavirus (HPV) vaccination campaign for girls aged 14 years from Rajasthan's Ajmer.
The initiative marks a decisive step towards eliminating cervical cancer through timely HPV vaccination. Cervical cancer remains the second most common cancer among women in India. Nearly 80,000 new cases and over 42,000 deaths are reported annually in the country.
"Today, I have had the opportunity to launch the HPV vaccine campaign from Ajmer. This campaign is an important step towards empowering women and daughters of this country,” PM Modi said.
“For us, this was a sensitive issue tied to the insult of our sisters and daughters, one that made them ill. That is why we resolved it at a crucial turning point in their mission,” he added.
The World Health Organization has also lauded India's mission to launch the HPV vaccine and prevent the risk of cervical cancer.
“We are leaving no stone unturned to ensure that the daughters of the country are healthy and prosperous. The objective of this initiative is the prevention of cervical cancer," the Prime Minister, earlier wrote in a post on social media platform X.
The HPV Vaccination Campaign
The nationwide program, based on expert recommendations of the National Technical Advisory Group on Immunization (NTAGI), will target girls aged 14 years.
At 14, the HPV vaccine offers maximum preventive benefit, well before potential exposure to the virus.
"By prioritizing prevention at the right age, the program is expected to provide lifelong protection and significantly reduce the future burden of cervical cancer in the country," the government said.
“The HPV vaccine works best at 9-14 years, before exposure, and when the immune response is strongest. Studies show effectiveness is highest in younger age groups and decreases with age,” Dr. Parmod Kumar, Associate Professor in Medical Oncology, AIIMS Jodhpur, shared on X.
Vaccination under the national program will be voluntary and free of cost.
The HPV vaccination will be conducted exclusively at designated government health facilities, including Ayushman Arogya Mandirs (Primary Health Centers), Community Health Centers, Sub-District and District Hospitals, and Government Medical Colleges.
Cervical Cancer Burden In South East Asia
Despite being preventable, cervical cancer continues to claim the life of a woman every two minutes globally, and the WHO South-East Asia Region bears nearly one-quarter of the global burden.
Dr. Catharina Boehme, Officer-in-Charge, WHO South-East Asia, stated that the introduction of HPV vaccination at a national scale in India "will have a far-reaching impact". It will accelerate progress not only for the country, but for the region and the world, she said.
“This landmark step, led at the highest level of government, reflects India’s strong commitment to protecting adolescent girls from cervical cancer," said Dr. Boehme.
With today’s milestone, nine of the 10 countries in the Region now include HPV vaccination in their national immunization programs.
The WHO global targets for 2030 include vaccinating 90 percent of girls by age 15, screening 70 percent of women by ages 35 and 45, and ensuring 90 percent of women with pre-cancer and invasive cancer receive appropriate treatment.
© 2024 Bennett, Coleman & Company Limited

