- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
FDA Plans To Halt Animal Testing For Drug Approval, What Could Replace It?

Credits: Canva
In a significant shift, the US Food and Drug Administration (FDA) has announced its plan to reduce its reliance on animal testing for drug development. This is especially for monoclonal antibody therapies and other advanced medicines. The agency now plans to use more human-relevant technologies in order to improve safety, lower costs and also speed up the approval process.
Animal History Traces Back To Ages
Animal testing has remained the cornerstone of all experiments, whether medicine or space. Since the 1930s, when the US passed the Federal Food, Drug, and Cosmetic Act in response to the tragic consequence of untested medication, animal testing was mandated. Scientists have been using mice, rats, rabbits and other animals to test for toxicity, side effects, as well ass efficacy before any new drug could be forwarded for human trial.
Over the decades, this practice also helped introduce many life-saving treatments. However, it has also raised ethical concerns and scientific questions, especially on how accurately can animal models really predict human response.
Why Is FDA Now Moving Away From Animal Testing?
The FDA’s new initiative represents a "paradigm shift," according to its Commissioner, Dr. Martin A. Makary. There are several reasons behind this change:
Limited Predictive Value: Drugs that work safely in animals don’t always perform the same way in humans. This mismatch can lead to failed clinical trials or unexpected side effects in people.
Ethical Concerns: As public awareness and concern about animal welfare have grown, so too has the demand for more humane research methods.
Cost and Time: Animal testing is expensive and time-consuming. Each stage of testing can take months or years and cost millions of dollars.
Scientific Advancements: New technologies now offer better ways to model human biology and disease. These methods not only spare animals but also yield more accurate data.
What Can Replace Animal Testing?
The FDA is planning to incorporate innovative tools like computer modeling and AI, human organoids, and organ-on-a-chip technology, as well as real world human data.
How Will these Work? The computer modeling and AI will allow the scientists with the help of simulations to predict how a drug will behave in the human body based on its chemical structure, genetics, and existing medical data.
Furthermore, human organoids are miniature, lab-grown versions of human organs like a liver or brain which are made from stem cells. They also closely mimic how real organs function and could be used to test drug safety and effectiveness.
Organ on a chip technology involves tiny chips that simulate the activity of the entire organ systems. For instance, how the heart beats or the lungs breathe. It allows for more accurate and efficient testing.
The agency is also planning to rely more on existing human clinical data from other countries with comparable regulatory standards. If a drug has already been tested and used abroad, repeating animal testing for the same in the US should not be any longer a mandate.
The new approach will be applied immediately to investigational new drug applications—essentially, the first step in bringing a new treatment to the U.S. market. This means that pharmaceutical companies can now submit non-animal safety data as part of their applications.
Importantly, this doesn’t mean animal testing will be banned entirely. In some cases, it may still be required to answer specific safety questions. However, the goal is to make animal studies the exception, not the rule.
Heatwave In India: Govt Issues Advisory, Doctors Stress Hydration

Credit: Canva
Rising global temperatures are driving heatwave conditions in India, said the Indian government, while releasing an advisory to warn people about the increased health risks.
Taking to the social media platform X, the Ministry of Health and Family Welfare urged the public to take precautions during extreme heat.
"Heat waves are increasing due to rising global temperatures," said the Ministry in the advisory.
It shared safety measures and an informative poster explaining the impact of rising temperatures and steps to manage heat stroke.
The poster highlighted that a rise of 1 degree Celsius in global temperatures can lead to longer durations of heatwaves.
Further, it stated that insufficient hydration during heatwaves reduces the body's natural ability to cool itself, which can result in heat stroke.
The poster also detailed preventive measures to avoid heat stroke. It also advised people to avoid heavy work during mid-noon hours, drink plenty of water, avoid consuming heavily caffeinated or sugary drinks as they may cause dehydration, wear light-colored clothes, and take frequent breaks while working outdoors.
Which States Are At Risk?
The India Meteorological Department (IMD) has warned of heatwave conditions in several parts of the country.
Regions likely to face extreme heatwave conditions until April 20 include Telangana and Rayalaseema, Madhya Maharashtra and Marathwada, North Interior Karnataka, Madhya Pradesh, Chhattisgarh, Vidarbha, Odisha, Jharkhand, and West Rajasthan.
In addition, hot and humid weather conditions are expected in coastal regions such as Kerala, Tamil Nadu, Gujarat, and Coastal Andhra Pradesh.
Meanwhile, the national capital saw its hottest day of the year on Wednesday, as temperatures climbed sharply, signaling the onset of harsher summer conditions. According to IMD, the maximum temperature at Safdarjung, the city’s base station, touched 39.2 degrees Celsius, about 3 degrees above normal. This surpassed Tuesday’s 38.2 degrees Celsius, marking a noticeable upward trend.
While the mercury is expected to inch closer to 42 degrees Celsius by Friday, the weather office has ruled out heatwave conditions for at least the next week.
“A gradual rise is expected in maximum temperatures by 2-3 degrees during the next three days and fall by 1-2 degrees thereafter. The maximum temperatures are likely to be above normal to appreciably above normal during the next seven days," Times Of India quoted a Met official as saying.
As per the weather department, despite a slight chance of light rain in parts of Haryana and NCR on April 17 and 18, there is no relief expected for Delhi.
Forecasts suggest daytime temperatures will hover between 39 degrees Celsius and 41 degrees Celsius on Thursday, rising further to 40-42 degrees Celsius from Friday through Sunday.
The IMD has cautioned that such above-normal temperatures could pose moderate health risks, especially for infants, elderly individuals, and those with chronic illnesses.
Hydration Is key, Say Doctors
Dr. Anil Gomber, Director and Senior Consultant – Internal Medicine & Diabetologist, Yatharth Hospital, told HealthandMe: “It is crucial to take preventive measures to avoid heat-related illnesses".
Prolonged exposure to high temperatures can lead to dehydration, heat exhaustion, and heatstroke, which can be fatal if untreated.
Heat also places extra strain on the heart and lungs, increasing the risk of heart attacks and respiratory distress.
Heatwaves can increase the risk of deaths among the elderly and those with underlying medical conditions. It can also affect healthy and young people. Exposure to intense heat can cause headaches, dizziness, cramps, and fainting, particularly for those working outdoors or engaging in strenuous activity.
"Elderly people, kids, and those with chronic conditions like heart disease or diabetes face higher risks, so check on neighbors and family daily," Dr. Meenakshi Jain Principal Director & HOD Internal Medicine, Max Super Speciality Hospital, told HealthandMe.
She urged people to "watch for warning signs like dizziness, rapid heartbeat, nausea, or confusion, and move to a cool area immediately if they appear—seek medical help for severe symptoms. Keep homes cooler by closing curtains during the day and opening windows at night".
How To Stay Safe
To stay safe from heatwave, individuals must:- Stay well-hydrated by drinking plenty of water
- Avoid caffeine
- Avoid stepping out during peak afternoon hours
- Wear light, loose, and breathable clothing,
- Use protective gear like caps or umbrellas when outdoors
- Avoid excessive physical activity in the sun.
- Never leave children or elderly individuals in parked vehicles. Include fruits and fluids in your diet to maintain electrolyte balance.
- If you experience dizziness, headache, or fatigue, seek medical attention promptly, as early care can prevent serious complications.
Over 3 Million Eye Drops Recalled By US FDA Over Sterility Concerns: Know How To Stay Safe
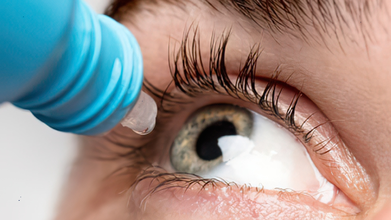
Credit: Canva
More than 3 million eye drops have been recalled by the US Food and Drug Administration (FDA) over sterility concerns.
The FDA, in its Enforcement Reports, stated that the products recalled “lack assurance of sterility.”
While so far, there are no reports of injuries associated with the eye drops, the FDA notice classified the action as a “Class II recall.”
Class II recalls apply to products that can cause “temporary or medically reversible” health problems.
The 3,111,072 products were manufactured by California-based K C Pharmaceuticals and were sold under names such as “Dry Eye Relief Eye Drops,” “Sterile Eye Drops,” and “Artificial Tears Sterile Lubricant Eye Drops,” according to the FDA notice.
California-based K C Pharmaceuticals made the voluntary recall of the eye drops in early March.
The eight types of eye drop products were sold at major retailers, including CVS, Walgreens, and Rite Aid. They have expiration dates ranging from April to October.
Eye Drop Recall: Implications For Patients
“The recall is very large, potentially affecting over a million people,” said C. Michael White, clinical pharmacologist and pharmacist at the University of Connecticut, in a Commentary published in The Conversation.
He added that “using nonsterile eye drops that harbor bacteria and fungus can cause eye infections, which can become severe because the immune system has a hard time accessing the eyeball and fighting the microbes”.
However, other experts stated that infections from eye drops are rare. Notably, the current voluntary recall has not reported any infections to date.
According to Jeffrey H. Ma, an ophthalmologist at the University of California-Davis Health, people with dry eyes must use preservative-free drops that come in disposable single-use vials. He advised people to dispose of any eye drops included in the recall.
“Drops that are not on the recall list should be safe to use,” said Ma. “If you have any of the drops on the list, you should immediately throw them away.”
How To Avoid Common Eye Infections
Beyond contaminated eye drops, several common eye infections can be triggered by environmental factors such as sun exposure, dust, and dirt—especially among people who work outdoors or spend long hours in front of screens.
“Conjunctivitis, known as pink eye, is the most common type of eye infection,” Ma said. Pink eye is estimated to affect about six million people every year.
“It is usually viral or bacterial, and is transmitted through direct contact, such as touching or rubbing your eyes after touching a contaminated item,” Ma added.
Contact lens wearers also have a higher risk of eye infections, particularly if they sleep in their lenses.
Symptoms of an eye infection include:
- blurry vision
- discharge
- pain or discomfort
- redness of the eyelid or eye
- feeling like there is something in the eye
- increased sensitivity to light
Experts urged investing in good sunglasses with ultraviolet protection and maintaining proper hygiene, such as washing hands before touching the lenses.
"For those who are using computers a lot, you need to blink your eyes constantly, take breaks in between, and drink a lot of water. Dehydration is also a contributing factor to dry eye," Dr Anita Sethi, who is Principal Director and HOD Ophthalmology, Max Multi Specialty Centre at Panchsheel Park.
She also recommends using zero-number protective glasses and computer glasses that can decrease strain and dry eye.
While advising people to stay away from natural remedies like turmeric or ginger put inside the eye, Dr Sethi urged people to consume more “foods rich in vitamin E, antioxidants” to maintain eye health.
Delhi HC Allows Sperm Extraction of Soldier in Coma: Doctors Call For Clearer IVF Guidelines
Credit: iStock
India needs clearer guidelines on reproductive rights, consent, and medical ethics, said doctors after the Delhi High Court, in a highly complex and sensitive case, granted permission for the extraction and cryopreservation of sperm of an Indian Army soldier in a persistent vegetative state.
As per the guidelines laid under the Assisted Reproductive Technology (ART) (Regulation) Act, 2021, it is important to have the written consent of both partners.
However, calling it “the right to reproductive autonomy,” Justice Purushaindra Kumar Kaurav allowed for sperm retrieval. The Court also cited the soldier's prior consent to undergo IVF treatment with his wife. "It constituted valid consent under the ART Act," LiveLaw reported.
What Is the Case All About?
The wife of an Indian Army soldier had approached the Court seeking directions to allow the retrieval and preservation of her husband's genetic material to enable her to undergo IVF.
Her husband, an Indian Army soldier, suffered a severe traumatic brain injury during deployment in Jammu and Kashmir in July last year and has since remained in a persistent vegetative state.
Before the incident, the couple had already opted for IVF and initiated procedures. However, the process was halted due to the husband's inability to provide fresh written consent as required under Section 22 of the ART Act, Live Law reported.
“While ...as on date there is no express indication of consent from the petitioner's husband, however, under the facts and circumstances of the present case, it is found to be fair, reasonable, and just for the respondents to undertake the necessary procedure/steps which are required to take the IVF treatment to its logical conclusion. But for this, the original consent given by the petitioner's husband shall stand vitiated, and the very purpose for acceding to the IVF treatment shall be rendered otiose,” said Justice Kaurav, in the Court's ruling.
“It is further directed that the petitioner's consent be considered as valid consent for her husband for the purposes of IVF procedure, if the same is required for any other step/procedure. The respondents shall not disentitle the petitioner on the sole ground that the petitioner's husband's written consent is absent,” the Court said.
HealthandMe spoke to IVF specialists to understand the procedure and implications around reproductive rights, consent, and medical ethics.
How Is Sperm Retrieval Performed in a Comatose Patient?
Dr Rachita Munjal, Director and Senior Consultant - Department of Fertility at Cloudnine Group of Hospitals, Gurugram, said that sperm retrieval and cryopreservation are possible in coma/vegetative patients, but success depends on timing and medical condition.
Also read: Explained: What Is Posthumous Reproduction?
In such conditions, sperm quality may be compromised, but assisted reproductive techniques can still make conception possible.
"Cryopreservation of sperm in men who are in a vegetative state or coma is medically complex but technically feasible in many cases, depending on the underlying condition and timing," the doctor told HealthandMe.
How sperm is retrieved
Since the person cannot ejaculate voluntarily, doctors use assisted techniques, such as
- Penile vibratory stimulation (PVS): Non-invasive; works if spinal reflexes are intact
- Electroejaculation (EEJ): Electrical stimulation under anesthesia to induce ejaculation
- Surgical sperm retrieval: If the above fail. Testicular sperm aspiration (TESA), Testicular sperm extraction (TESE)
- Percutaneous epididymal sperm aspiration (PESA)
These are typically performed by urologists or fertility specialists with consent from legal guardians or prior consent of the patient. Once sperm is obtained:
- Sperm is analyzed (count, motility, morphology)
- Mixed with a cryoprotectant to prevent cell damage
- Gradually cooled and stored in liquid nitrogen at –196°C
- Can be preserved for years without significant degradation
- Cause of coma (trauma vs neurological disease)
- Time since coma onset (earlier is better)
- Baseline fertility health
- prolonged immobility
- infections
- medications (sedatives, antibiotics)
- hormonal disruption
Are There Any Ethical Considerations
There are many ethical considerations in such cases, said Dr Munjal, noting that this requires explicit prior consent or legal authorization.
“Ethical concerns include reproductive rights and future child welfare,” she added.
Dr. Sabine Kapasi, IVF Specialist & Public Health Strategist, called it “an emotionally sensitive case where law, ethics, and reproductive rights intersect”.
“While prior IVF consent may indicate shared intent to build a family, it does not always automatically equal consent for gamete retrieval during permanent incapacity. Such decisions should ideally involve explicit consent, ethics review, and psychological counseling for the family,” the expert said.
This is not the first time that sperm have been retrieved from a comatose patient.
In 2024, a Kerala High Court permitted the extraction of the sperm of a childless couple where the husband was in a brain-dead condition and kept alive with ventilator support. The Court allowed the extraction and cryopreservation of the gametes, without the written consent of the husband.
"India now needs clearer ART guidelines for coma, posthumous, and incapacity-related reproduction to avoid future disputes. Compassion is important, but medical ethics and long-term child welfare must remain central,” Dr Kapasi noted.
© 2024 Bennett, Coleman & Company Limited

