- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Hundreds Of US Children Have Type 1 Diabetes, Now Their Barbie Has It Too

Credits: Mattel and Canva
Growing up, a lot of us may have played with Barbie. Back then, there was a one-size-fits-all Barbie for everyone, unlike today, where the makers have finally understood that representation matters. In this new understanding of representation, even in dolls, the latest Barbie in chic blue-polka crop top and a miniskirt with chunky heels, is not just ready for summer, but also carries an insulin pump. The Barbie also has a continuous glucose monitor on her arm, and the button is held on by a strip of heart-shaped Barbie-pink tape. Her phone also shows an app with glucose readings. She also carries a light blue purse that holds all her supplies, including snacks that can help her manage her blood sugar throughout the day.
This is the brand's first doll with type 1 diabetes.
Why Does This Barbie With Type 1 Diabetes Matter?
Dollmaker Mattel worked with Breakthrough T1D, which was earlier known as the Juvenile Diabetes Research Foundation, to design the doll and to represent the 304,000 kids and teens, as noted by the American Diabetes Association. who are living with type 1 diabetes in the United States.
The doll was launched on Tuesday with an aim to ask Congress to renew funding for the Special Diabetes Program, which had been first allocated by Congress in 1997. Currently, the program's funding will end after September.
The launch of the Barbie also focuses on the immense cuts made to federally funded projects in the past months, and thus, this launch is a way to draw people's attention on the said program that focuses on children with type 1 diabetes.
What Is Type 1 Diabetes?
As per the American Diabetes Association, Type 1 diabetes is an autoimmune disease, where your immune system mistakenly treats the beta cells in your pancreas that create insulin as foreign invaders and destroys them. When enough beta cells are destroyed, your pancreas cannot make more insulin, or makes so little that you need to take insulin to live.
What Is Insulin?
It is a hormone that helps blood glucose enter your body's cells so that it can be used as energy. If you have diabetes, blood glucose cannot enter your cells, so it builds up in your bloodstream, causing high blood glucose or hyperglycemia. Over time, high blood glucose harms your body and can lead to diabetes-related complications if not treated.
Common Symptoms of Type 1 Diabetes
- Urinating often
- Feeling very thirsty
- Feeling very hungry—even though you are eating
- Extreme fatigue
- Blurry vision
- Cuts/bruises that are slow to heal
- Weight loss—even though you are eating more
Type 1 Diabetes In Children
A 2024 study published in JAMA Network, titled: Prevalence of Type 1 Diabetes Among US Children and Adults by Age, Sex, Race, and Ethnicity, notes that nearly 4 in every 1000 youths in the US reported having type 1 diabetes from 2019 to 2022. As per the National Institute of Diabetes and Digestive and Kidney Diseases, of the 38.4 million people who had diabetes in 2021, 352,000 were children and adolescents younger than age 20, including 304,000 with type 1 diabetes.
Johns Hopkins Medicine notes that even in type 1 diabetes, there are broadly two types:
Immune-mediated diabetes: This is an autoimmune disorder in which the body's immune system damages the cells in the pancreas that make insulin. This is the most common kind of type 1 diabetes.
Idiopathic type 1: This refers to rare forms of the disease with no known cause.
In children, there could be many factors that can cause type 1 diabetes, including if a family member has a condition, if the child is White, is from Finland or Sardinia, or is aged between 4 and 6 or 10 and 14.
How Is Type 1 Diabetes Diagnosed In Children?
To diagnose type 1 diabetes, the healthcare provider will start by asking about your child’s symptoms and overall health history. They may also ask questions about your family’s medical background. A physical exam will be done, and your child may need some blood tests, such as:
Fasting plasma glucose test: This checks blood sugar levels after your child hasn’t eaten for at least 8 hours.
Random plasma glucose test: This measures blood sugar at any time, especially if your child is showing symptoms like extreme thirst, frequent urination, or increased hunger.
A1C test: This gives an average of your child’s blood sugar levels over the past 2 to 3 months. A high A1C level can help confirm a diagnosis of diabetes.
How is Type 1 Diabetes Treated in Children?
Children with type 1 diabetes need daily insulin to manage their blood sugar. Insulin can be given either through injections or an insulin pump. Your child’s healthcare team will teach you how to use whichever method is best for your child.
Treatment also involves:
Healthy eating: This includes planning meals carefully, counting carbohydrates, and eating at regular times to help control blood sugar.
Physical activity: Regular exercise helps lower blood sugar levels.
Monitoring blood sugar: This includes checking levels several times a day, often using a continuous glucose monitor (CGM).
Testing urine: To check for ketones, which can be a sign of a serious complication if blood sugar is too high.
Two Passengers From Singapore Airlines Arrive In New Zealand With Measles
Credits: Canva
Two passengers travelling in Singapore airlines arrived in New Zealand with measles symptoms. However, reported The Strait Times, that they are not linked to any other known cases, as noted by the Communicable Disease Agency (CDA).
The agency told the media outlet that it was notified on February 25 that two Singapore Airlines (SIA) passengers infected with measles landed in Auckland, New Zealand. Both were from the same household and flown from Hyderabad, India. They transited in Singapore for two hours before boarding an SIA flight to Auckland.
CDA investigation also revealed that these two cases remained in the transit area at Changi Airport. Associate Professor Lim Poh Lian, group director of the CDA's Communicable Disease Programmes, as reported by The Strait Times noted that the individuals were reported to have developed symptoms only while onboard the flight from Singapore to Auckland.
New Zealand media earlier reported that the two cases were detected after the individuals arrived in Auckland on flight SQ281 on February 17. The country’s public health authority began tracing passengers seated in rows 31 to 46 on the same flight, along with people who were present in the waiting area of Waitakere Hospital’s Emergency Department on February 21.
“Based on the onset of their symptoms, they were infected before transiting through Singapore and are not linked to any other known measles cases in Singapore,” Prof Lim said.
She also clarified that their time in transit through Singapore did not coincide with that of a previously reported measles case involving a passenger who had passed through Singapore en route to Los Angeles in the United States.
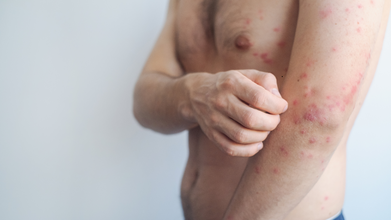
What Is Measles?
Measles has a high transmissibility, and high measles immunity levels are required to prevent sustained measles virus transmission.
This is why herd immunity for measles could be easily breached.
It easily spreads from one infected person to another through breathes, coughs or sneezes and could cause severe disease, complications, and even death.
Symptoms include:
- High fever
- Cough
- Runny Nose
- Rash all over the body
The most unique symptom or the early sign of measles in the Koplik spots. These are tiny white dots that look like grains of salt on red gums inside the cheeks that appear before the red rash starts to appear on a person's face and then the body.
Furthermore, the symptoms of measles are also characterized by the three Cs:
- Cough
- Coryza or runny nose
- Conjunctivitis or red and water eyes
Update On The Passengers Who Landed In New Zealand
The passenger on flight SQ38 arrived at Los Angeles International Airport at about 7pm on February 9, after a roughly two-and-a-half-hour transit at Changi Airport following a flight from Cambodia.
Prof Lim said the most effective protection against measles is to be fully vaccinated before travelling. She also advised travellers to practise good hygiene, such as washing hands regularly and avoiding close contact with anyone who is unwell.
Anyone who develops symptoms like fever, rash, cough, red or watery eyes, or a runny nose should wear a mask, seek medical care promptly, and inform their doctor about their recent travel and any possible exposure to measles, she added.
In response to queries, Singapore Airlines told The Straits Times that it is working closely with the authorities but cannot share specific details due to customer confidentiality.
Fact Check: Common Myths Around HPV Vaccine And How It Will Prevent Cervical Cancer
Credit: Canva
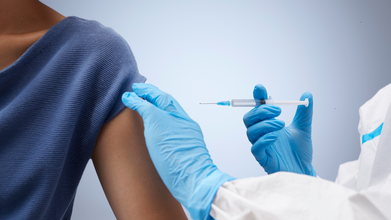
In a major push towards eliminating cervical cancer from India, Prime Minister Narendra Modi today launched the nationwide Human Papillomavirus (HPV) vaccination program for girls aged 14 years.
The new vaccination drive comes as cervical cancer remains the second most common cancer among women in India, with nearly 80,000 new cases and over 42,000 deaths reported annually. As per data from the ICMR-National Cancer Registry Program (NCRP), an estimated 78,499 new cases and 42,392 deaths were reported in 2024.
Calling it a "decisive step”, the government noted that it is aimed at “strengthening the vision of ‘swasth nari’ (healthy women) while being rooted in scientific evidence, strict regulatory oversight and global best practices”.
“India's vaccination drive reflects safety, responsibility, and long-term commitment to women’s health,” it added.
The national program will use Gardasil, a quadrivalent HPV vaccine that protects against HPV types 16 and 18, which cause cervical cancer, as well as types 6 and 11.
However, social media has been rife with concerns around the safety of the vaccine, its impact on women’s reproductive health, among others.
HPV Vaccine: The Myths And Facts
Myth: HPV vaccines can cause severe side effects and even death.
Fact: The HPV vaccines come with a “confirmed strong safety record”.
“Extensive global monitoring shows a strong safety profile supported by scientific reviews. Independent evaluations have found no causal link between vaccination and chronic harm, strengthening confidence in its continued use worldwide,” the government said.
The vaccine has been licensed in India since 2008, and the new rollout follows recommendations by the World Health Organization (WHO) and approvals from the National Technical Advisory Group on Immunization (NTAGI).
“HPV vaccines have been given to hundreds of millions globally. Extensive post-marketing surveillance shows an excellent safety profile, with no causal link to serious adverse outcomes. The evidence is robust, transparent, and reassuring,” Dr. CS Pramesh, Director of the Tata Memorial Hospital, Mumbai, shared in a post on the social media platform X.
Myth: The HPV vaccine has never been used in India
Fact: The vaccine has been in use in India. It has been administered for years since 2008 with successful implementation in states like Punjab, Sikkim, and Tamil Nadu.
Myth: HPV vaccination does not prevent cervical cancer
Fact: The HPV vaccine has been proven to prevent cervical cancer
Studies show a 65 percent drop in cervical cancer cases among US women between 2012 and 2019 and an 88-89 percent reduction in precancerous lesions among Scottish women over a decade.
Countries with early HPV vaccine adoption have also shown large declines in HPV infection, high-grade cervical lesions, and cervical cancer incidence.
"Even when considering the rarest side effects, HPV vaccines are overwhelmingly safe. The protection they offer against cervical cancer far outweighs the minimal risks. Parents are encouraged to vaccinate their daughters on time," said Dr. Neena Malhotra, Professor and Head of Department, Department of Obstetrics and Gynecology, AIIMS New Delhi on X.
Myths: Are Multiple Doses Needed?
Fact: A single dose of the quadrivalent HPV vaccine is effective. It provides strong protection against HPV infection. It helps prevent cervical cancer.
“Strong global and Indian scientific evidence confirms that a single dose provides robust and durable protection when administered to girls in the recommended age group," the government said.
PM Modi Launches Nationwide Free HPV Vaccination Drive; A Landmark Step, Says WHO

Credit: Health Ministry
Prime Minister Narendra Modi today launched the nationwide Human Papillomavirus (HPV) vaccination campaign for girls aged 14 years from Rajasthan's Ajmer.
The initiative marks a decisive step towards eliminating cervical cancer through timely HPV vaccination. Cervical cancer remains the second most common cancer among women in India. Nearly 80,000 new cases and over 42,000 deaths are reported annually in the country.
"Today, I have had the opportunity to launch the HPV vaccine campaign from Ajmer. This campaign is an important step towards empowering women and daughters of this country,” PM Modi said.
“For us, this was a sensitive issue tied to the insult of our sisters and daughters, one that made them ill. That is why we resolved it at a crucial turning point in their mission,” he added.
The World Health Organization has also lauded India's mission to launch the HPV vaccine and prevent the risk of cervical cancer.
“We are leaving no stone unturned to ensure that the daughters of the country are healthy and prosperous. The objective of this initiative is the prevention of cervical cancer," the Prime Minister, earlier wrote in a post on social media platform X.
The HPV Vaccination Campaign
The nationwide program, based on expert recommendations of the National Technical Advisory Group on Immunization (NTAGI), will target girls aged 14 years.
At 14, the HPV vaccine offers maximum preventive benefit, well before potential exposure to the virus.
"By prioritizing prevention at the right age, the program is expected to provide lifelong protection and significantly reduce the future burden of cervical cancer in the country," the government said.
“The HPV vaccine works best at 9-14 years, before exposure, and when the immune response is strongest. Studies show effectiveness is highest in younger age groups and decreases with age,” Dr. Parmod Kumar, Associate Professor in Medical Oncology, AIIMS Jodhpur, shared on X.
Vaccination under the national program will be voluntary and free of cost.
The HPV vaccination will be conducted exclusively at designated government health facilities, including Ayushman Arogya Mandirs (Primary Health Centers), Community Health Centers, Sub-District and District Hospitals, and Government Medical Colleges.
Cervical Cancer Burden In South East Asia
Despite being preventable, cervical cancer continues to claim the life of a woman every two minutes globally, and the WHO South-East Asia Region bears nearly one-quarter of the global burden.
Dr. Catharina Boehme, Officer-in-Charge, WHO South-East Asia, stated that the introduction of HPV vaccination at a national scale in India "will have a far-reaching impact". It will accelerate progress not only for the country, but for the region and the world, she said.
“This landmark step, led at the highest level of government, reflects India’s strong commitment to protecting adolescent girls from cervical cancer," said Dr. Boehme.
With today’s milestone, nine of the 10 countries in the Region now include HPV vaccination in their national immunization programs.
The WHO global targets for 2030 include vaccinating 90 percent of girls by age 15, screening 70 percent of women by ages 35 and 45, and ensuring 90 percent of women with pre-cancer and invasive cancer receive appropriate treatment.
© 2024 Bennett, Coleman & Company Limited

