- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Is The Viral 'Quad-demic' Still Swirling? Know The Good, Bad And Ugly
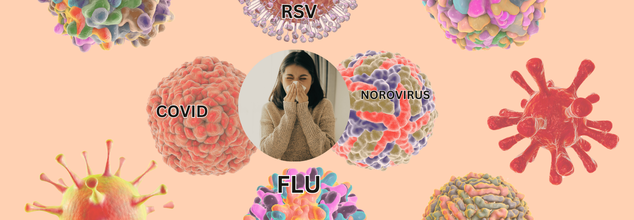
Image Credit: Health and me
There's been an alarming increase of respiratory and gastrointestinal viruses in the United States lately, causing anxiety about a so-called "quad-demic". According to surveillance reports, influenza, COVID-19, RSV and norovirus are at very high levels everywhere. While the surge aligns with patterns typical for this season, several epidemiologists view simultaneous infections of such proportions to pose risks not only to individual healthcare but public health.
The incidence of the quad-demic should vary with seasonal patterns, vaccination rates, and public health interventions. Each virus alone is relatively easy to manage; however, the effect of all together could lead to overburdening of health care facilities and increase risks for those at higher risk. Continuing surveillance, early testing, and proactive prevention measures will play an important role in the control of these infections going forward.
While the term "quad-demic" sounds daunting, it must be taken into perspective. For years, we have had all these viruses together, and we have the capabilities to mitigate some of the risk. Vaccination, proper hygiene and using common sense helps individuals get through the season unscathed. Is the quad-demic a permanent fixture or just another seasonal wave? Let's break this down.
What is the Quad-demic?
Typically, flu, COVID-19, and RSV have been the primary culprits behind seasonal respiratory infections. However, norovirus, a highly contagious stomach bug, has emerged as a fourth significant player, inducing fears of a more severe and widespread viral outbreak. According to the Centers for Disease Control and Prevention (CDC), the U.S. recorded nearly 500 norovirus outbreaks between August and December 2023, a substantial rise from the previous year’s numbers.
While the term "quad-demic" may sound ominous, the seriousness and consequences of such infections should be weighed in light of the U.S. healthcare system's experience with managing viral surges since the start of the COVID-19 pandemic.
1. Influenza (Flu)
Flu continues to be one of the most common and alarming seasonal illnesses. In the period spanning from 2023 to 2024, there were approximately 40 million cases of flu, and thousands of hospitalizations along with reported 47 deaths have been reported this season. Flu symptoms include fever, chills, cough, sore throat, muscle pain, and fatigue, with most recovering within a week or two but risky factors for severe illness effects occur in young children, elderly, and people with chronic conditions.
2. Covid-19
Despite its reduction from the first pandemic peak, COVID-19 is still rampant. The CDC estimates that alone between October and December 2023, there were between 2.7 and 5 million cases in the U.S. Hospitalization has increased by cities such as Los Angeles, Chicago, and New York. Symptoms are closely similar to the flu, fever, cough, and fatigue but uniquely presents in some cases as loss of taste and smell.
3. RSV
RSV is the most common cause of lower respiratory infections in infants, older adults, and immunocompromised individuals. While RSV peaked late in 2023 and early 2024, it continues to be a threat because it can lead to bronchiolitis and pneumonia. It is very similar to the common cold, presenting with symptoms such as congestion, runny nose, coughing, and fever, which can make it difficult to differentiate from flu or COVID-19 without testing.
4. Norovirus
Norovirus, also called the "stomach flu," is a highly contagious infection of the gastrointestinal tract, not a respiratory virus. It transmits quickly from contaminated food and water and contact with contaminated surfaces, causing such symptoms as diarrhea, vomiting, nausea, and stomach pain. Cases have shot up, the CDC said Monday, with reports of outbreaks surging compared with last year.
Is There a Challenge In Diagnosis Due to Overlapping Symptoms?
The greatest challenge during the quad-demic is how the four viruses are alike and thus make identification very hard with no testing applied. Most cases present symptoms common to all viruses: fever, tiredness, body pains, and respiratory, which includes coughing and congestions for influenza, COVID-19, and RSV; the other would be norovirus symptoms as nausea and vomiting can appear even in extreme influenza and COVID-19. This overlap increases the risk of misdiagnosis and delayed treatment, hence the need for early testing and proper medical guidance.
Also Read: Is US Preparing For A Quad- demic 2025?
Effective Prevention Strategies That Work
The best defense against these viruses is a combination of vaccines, hygiene, and lifestyle precautions. While lifestyle modifications are highlighted as part of the constant need to eat healthy, ensure daily movement and drinking adequate amount of fluids. There is a sure short two preventive strategies that are effective:
Vaccination
- Flu vaccine: Annual flu shots reduce the severity of infection, allergic flare ups and hospitalizations.
- COVID-19 vaccine: Though COVID-19 cases have declined, vaccination remains critical in preventing severe outcomes.
- RSV vaccine: Available for those aged 60 years and older, especially those with underlying conditions.
- Norovirus vaccine: No vaccine is yet available, but mRNA vaccine research is in progress.
Hygiene and Sanitation
- Washing hands frequently with soap and water for at least 20 seconds, especially after public exposure.
- Disinfect frequently touched surfaces regularly, use sanitiser when outside.
- Avoid close contact with infected people and wear masks.
Do You Need To Wear A Mask All The Time?
While debates on masked wear continue on, experts on mask-wear affirm that this does not only have a historical precedent but works towards reducing airborne viruses spreading within the environments. Hospitals, though, ensure masking in key sections of themselves. Publicized mask-wear remains a discretion, though massing indoors still goes a longer way in cases like peak flu seasons.
If you notice the symptoms of these viruses, then it's best to be confined at home and avoid having face-to-face interaction with others and seek immediate attention from your physician if your condition worsens. Quarantining for some days can decrease the spread of infection.
As we move into the first half of 2025 and beyond, staying informed and proactive is the best strategy for maintaining health and avoiding unnecessary panic. The key takeaway? Stay vigilant, but don’t be alarmed—these viruses are here, but so are the means to fight them.
Alkem Laboratories Launches Cheapest Semaglutide Injection In India
Credit: Canva
India's Alkem Laboratories is all set to launch a semaglutide injection, meant for weight-loss and diabetes patients, priced merely at weekly cost of Rs 450 - making it one of the cheapest options available in the market.
The patent for Novo Nordisk, the original maker of semaglutide, ended on March 20 and since then, numerous pharmaceutical companies have begun releasing their own versions of the blockbuster drug.
Alkem Laboratories's drug, marketed under the brand names Semasize, Obesema and Hepaglide in India, will is administered as a once-weekly subcutaneous injection and the organization has revealed a pre-filled disposable injection pen priced at Rs 1,800 for a month’s dosage.
Apart from the drug, Alkem is also offering a reusable injection pen for higher maintenance doses, allowing patients to replace only the medication cartridge instead of buying a new device each time in order to reduce long-term treatment costs and improving adherence.
The company has received approval from the Drug Controller General of India to manufacture and market semaglutide for Type 2 Diabetes Mellitus and chronic weight management, following a review of Phase 3 clinical trials conducted in India.
Other Semaglutide Injection Launches In India
Apart from this, NATCO Pharma became the first to introduce Semanat and Semafull for INR 1,290 per month and INR 1,750, about 90 per cent cheaper than Ozempic, costing INR 8,800 per month.
Eris Lifesciences also announced its plans to launch a multi-dose vial under the brand name Sundae at the same price. Dr. Reddy’s Laboratories, Sun Pharmaceutical Industries, and Glenmark Pharmaceuticals launched their generic versions of semaglutide. Dr. Reddy’s Obeda is priced at Rs 4,200 per month, available in 2 mg and 4 mg strengths.
Sun Pharmaceutical Industries will sell under the brand names Noveltreat (doses ranging from INR 900) and Sematrinity (doses ranging from INR 750). Meanwhile, Glenmark’s GLIPIQ vials range from Rs 325 to Rs 440 per week.
Zydus Lifesciences has also announced the launch of its generic version of semaglutide injection under the brand names SEMAGLYNTM, MASHEMATM, and ALTERMET. The average monthly cost of the treatment will be about Rs 2,200, the company said in a statement.
Semaglutide: Risks Vs Benefits
In people with type 2 diabetes, Harvard Health noted that the body's cells are resistant to the effects of insulin and the body does not produce enough insulin, or both. This is when GLP-1 agonists stimulate the pancreas to release insulin and suppress the release of another hormone called glucagon.
These drugs also act in the brain to reduce hunger and act on the stomach to delay emptying, so you feel full for a longer time. These effects can lead to weight loss, which can be an important part of managing diabetes.
Notably, semaglutide is not just a glucose-lowering drug, it improves weight and has proven cardiovascular, liver, and renal benefits.
Wider availability could therefore help reduce long-term complications such as heart disease and kidney failure. If used appropriately, this could indeed be a major step forward in total metabolic care, the experts said.
“The increasing affordability of GLP-1 receptor agonists is a double-edged development. On one hand, it significantly improves access for patients with obesity, type 2 diabetes, and high cardiovascular risk, conditions that are highly prevalent in India. These drugs have demonstrated meaningful benefits in weight reduction, glycemic control, and even cardiovascular risk reduction, which could translate into long-term public health gains,” Dr Vivek Bindal, Senior Director & Head, Bariatric and Robotic Surgery, at Max Healthcare, told HealthandMe.
A recent study published in The Lancet Psychiatry journal showed that Ozempic can also help tackle the burden of depression, anxiety, and self-harm in high-risk diabetic patients.
However, the benefits are conditional as it depends on appropriate prescribing, reliable product quality, and adequate patient monitoring, said Dr. Anoop Misra, who heads Delhi’s Fortis-C-DOC Centre for Diabetes and Endocrinology, told HealthandMe..
"These drugs should be strictly prescribed by qualified doctors and used only for therapeutic purposes, not for cosmetic weight loss,” Dr. Mohan said.
Urging for careful monitoring of side effects, the expert also called for more Indian data and strict pharmacovigilance.
“This also presents a great opportunity for India to make these drugs affordable and accessible to other developing countries across Asia and Africa,” the noted diabetologist said.
The experts also warned of “indiscriminate or unsupervised use” due to low cost.
This is particularly for cosmetic weight loss without proper medical evaluation, said Dr. Bindal.
“GLP-1 therapies are not ‘quick fixes’ -- they require careful patient selection, dose titration, and monitoring for side effects such as gastrointestinal intolerance or, rarely, pancreatitis,” he added.
However, the focus should remain on holistic obesity management, including lifestyle modification, rather than over-reliance on pharmacotherapy alone.
Fact Check: Did Keir Starmer Say UK ‘May Need To Go Into Lockdown’ If Meningitis Cases Keep Rising?
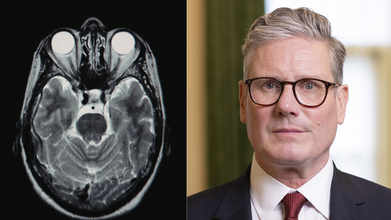
Credits: Canva and Wikimedia Commons
Meningitis cases in Kent has alerted many to take precautions. As per a BBC report, Mashaal Chugtai, 22, who studies laws in the University said that it feels like "Covid all over again". Amid this, a claim has been circulating that Prime Minister Sir Keir Starmer warned "the UK may need to go into lockdown as early as May if meningitis cases continue to escalate".
Some posts also include an additional quote, supposedly from Sir Keir, that says “I will do whatever it takes to keep the country safe over the election period, even if that means you can’t go outside”.
However, upon fact checking, it was found that Sir Keir made no such statement. Number 10 also confirmed to Full Fact that the Prime Minister did not make such claims and this appeared from a satirical Facebook page.
What Is Happening In The UK?
Meningitis outbreak in Kent University that infected a dozen of people have now further infected more people. The total number as of now is 27, as experts say that incubation period of the bacteria may lead to an increase in number of those who are sick.
The bug that causes the infection has been identified as the known strain of meningitis B and MenB vaccines will be offered to 5,000 students living in the University of Kent halls of residence in Cantebury. While several reports claim that parents are rushing to pharmacies to get their children vaccinated, due to which there is a shortage of the MenB vaccines, health secretary, Wes Streeting has denied any such claims. "There is actually plenty of stock of vaccine supply in the country," he said.
As per the UK Health Security Agency (UKHSA) official, people infected in Kent were the ones who visited a nightclub on 5,6 or 7 March. The officials, including NHS members and county council public health staff who have been tackling the outbreak believe that it has not been passed on to anyone outside the area. "All cases to date are linked to the current outbreak in Kent," said a UKHSA spokesperson, as reported by The Guardian.
Another official involved in the multi-agency response said, "We may have contained it. There are no cases popping up elsewhere that we know of – no cases that we know of outside the cluster – or not yet anyway. We are rolling out a vaccine and antibiotics and tracing contacts. So there’s nothing we’re not doing.”
Quickest-growing Meningitis Outbreak Ever
UKHSA chief executive Susan Hopkins said the outbreak "looks like a super-spreader" event with "ongoing spread" through universities' halls of residence. She added: "There will have been some parties particularly around this, so there will have been lots of social mixing. I can't yet say where the initial infection came from, how it's got into this cohort, and why it's created such an explosive amount of infections."
She further said that in her 35 years working in medicine, healthcare, and hospitals, "This is the most cases I've ever seen in a single weekend with this type of infection". She added: "It is the explosive nature that is unprecedented here - the number of cases in such a short space of time." She also remarked that this was the "quickest-growing outbreak" she has ever seen in her career.
What Is Meningitis?
Meningitis is a serious medical condition that affects the protective membranes covering the brain and spinal cord, the meninges. While fever is not always present, it is usually considered as one of the classic symptoms of meningitis. It is important to know the varied symptoms, causes, and treatments of meningitis for early diagnosis and proper management of the disease.
Meningitis is an infectious illness that brings about inflammation in the meninges. The most common cause of such inflammation is bacterial or viral infections, though other causes are also possible including fungal, parasitic, or non-infectious causes (autoimmune disease, head injury, or brain surgery). Meningitis may be caused by bacterial meningitis, which the Centers for Disease Control and Prevention (CDC) indicates can be so severe and bring about conditions like hearing loss, vision problems, and death if not received on time.
Semaglutide Becomes Cheap In India: A Gamechanger Or Health Gamble?
Credit: iStock
The end of patent on semaglutide, the active ingredient in popular weight loss drugs like Ozempic and Wegovy, in India has ushered in the way for cheaper generic -- up to 90 per cent lower than the original drug price.
HealthandMe spoke to various experts to understand whether the cheaper versions of semaglutide will spur better health for Indians, or whether the various side effects seen in Ozempic will also be translated to the low-priced drugs.
The patent for Novo Nordisk, the original maker of semaglutide, ended on March 20. On the same day, NATCO Pharma became the first to introduce Semanat and Semafull for INR 1,290 per month and INR 1,750 -- about 90 per cent cheaper than Ozempic, costing INR 8,800 per month. Eris Lifesciences also announced its plans to launch a multi-dose vial under the brand name Sundae at the same price.
Today, Dr. Reddy’s Laboratories, Sun Pharmaceutical Industries, and Glenmark Pharmaceuticals launched their generic versions of semaglutide.
Dr. Reddy’s Obeda is priced at Rs 4,200 per month, available in 2 mg and 4 mg strengths.
Sun Pharmaceutical Industries will sell under the brand names Noveltreat (doses ranging from INR 900) and Sematrinity (doses ranging from INR 750). Meanwhile, Glenmark’s GLIPIQ vials range from Rs 325 to Rs 440 per week.
Zydus Lifesciences has also announced the launch of its generic version of semaglutide injection under the brand names SEMAGLYNTM, MASHEMATM, and ALTERMET. The average monthly cost of the treatment will be about Rs 2,200, the company said in a statement.
Dr. V. Mohan, Chairman of Dr. Mohan's Diabetes Specialities Centre, Chennai, told HealthandMe called it a “very positive development” yet stressed the need to ensure “quality”.
According to a BBC report, around 50 branded semaglutide generics will enter the Indian market within months. How will this benefit Indians? Let's take a look.
Semaglutide works as a GLP-1 receptor agonist that mimics the GLP-1 hormone to regulate appetite and blood sugar. It slows gastric emptying and makes you feel fuller longer. It also signals the brain to reduce hunger and cravings, and triggers the pancreas to release insulin when blood sugar is high.
“For a country like India, which carries a large burden of Type 2 Diabetes and Obesity (and related complications), this could translate into meaningful clinical gains,” Dr. Anoop Misra, who heads Delhi’s Fortis-C-DOC Centre for Diabetes and Endocrinology, told HealthandMe.
India is facing an alarming diabetes epidemic, ranking second globally with an estimated 101 million people living with diabetes and another 136 million with prediabetes as of 2023, according to the ICMR-INDIAB study.
Similarly, the National Family Health Survey (NFHS) 2019–21 states that 24 percent of Indian women and 23 percent of Indian men are overweight or obese.
Also read: Ozempic Will Go Generic, Weight-loss Drug Cost Could Lower By 90%
Semaglutide: Risks Vs Benefits
In people with type 2 diabetes, Harvard Health noted that the body's cells are resistant to the effects of insulin and the body does not produce enough insulin, or both. This is when GLP-1 agonists stimulate the pancreas to release insulin and suppress the release of another hormone called glucagon.
These drugs also act in the brain to reduce hunger and act on the stomach to delay emptying, so you feel full for a longer time. These effects can lead to weight loss, which can be an important part of managing diabetes.
Notably, semaglutide is not just a glucose-lowering drug -- it improves weight and has proven cardiovascular, liver, and renal benefits.
Wider availability could therefore help reduce long-term complications such as heart disease and kidney failure. If used appropriately, this could indeed be a major step forward in total metabolic care, the experts said.
“The increasing affordability of GLP-1 receptor agonists is a double-edged development. On one hand, it significantly improves access for patients with obesity, type 2 diabetes, and high cardiovascular risk -- conditions that are highly prevalent in India. These drugs have demonstrated meaningful benefits in weight reduction, glycemic control, and even cardiovascular risk reduction, which could translate into long-term public health gains,” Dr Vivek Bindal, Senior Director & Head, Bariatric and Robotic Surgery, at Max Healthcare, told HealthandMe.
A recent study published in The Lancet Psychiatry journal showed that Ozempic can also help tackle the burden of depression, anxiety, and self-harm in high-risk diabetic patients.
However, the benefits are conditional -- it depends on appropriate prescribing, reliable product quality, and adequate patient monitoring, said Dr. Misra.
"These drugs should be strictly prescribed by qualified doctors and used only for therapeutic purposes, not for cosmetic weight loss,” Dr. Mohan said.
Urging for careful monitoring of side effects, the expert also called for more Indian data and strict pharmacovigilance.
“This also presents a great opportunity for India to make these drugs affordable and accessible to other developing countries across Asia and Africa,” the noted diabetologist said.
The experts also warned of “indiscriminate or unsupervised use” due to low cost.
This is particularly for cosmetic weight loss without proper medical evaluation, said Dr. Bindal.
“GLP-1 therapies are not ‘quick fixes’ -- they require careful patient selection, dose titration, and monitoring for side effects such as gastrointestinal intolerance or, rarely, pancreatitis,” he added.
However, the focus should remain on holistic obesity management, including lifestyle modification, rather than over-reliance on pharmacotherapy alone.
Also read: Semaglutide: Wegovy Can Spur Sudden Sight Loss By 5x; Men More At Risk, Finds Study
The major concerns around semaglutide include:
- Quality and manufacturing variability
Semaglutide is a complex peptide, unlike conventional small-molecule drugs. Variations in manufacturing, storage, or delivery devices may affect efficacy and safety.
- Cold-chain and storage issues
Maintaining 2-8°C across India’s diverse healthcare settings is challenging. Breaks in the cold chain could reduce drug effectiveness without being immediately apparent.
- Regulatory burden
With 40+ companies entering the market, ensuring uniform quality, batch consistency, and device reliability will stretch regulatory systems.
- Inadequate physician training
Many prescribers may lack experience with GLP-1 receptor agonists—particularly regarding dose titration, side-effect management, and patient selection.
- Pharmaceutical promotion vs. scientific education
- Indiscriminate or cosmetic use
There is a real risk of semaglutide being used for “quick weight loss” without proper medical supervision.
- Adverse effects and monitoring gaps
Gastrointestinal side effects, gallbladder disease, and rare pancreatitis require counselling and follow-up—often lacking in routine practice.
The greatest benefit will be seen in:
- Patients with Type 2 diabetes and overweight/obesity
- Individuals with poor glycemic control despite standard therapy
- Patients with high cardiovascular risk, or who have suffered heart attacks and strokes
- Those with metabolic syndrome or abdominal obesity
- Selected patients with chronic kidney disease
- People with obstructive sleep apnea (disordered breathing at night)
- People with severe fatty liver and consequent damage to the liver
"In these groups, semaglutide provides multidimensional benefit -- glucose lowering, weight reduction, and cardiometabolic protection," Dr. Misra said.
Who Should Avoid Semaglutide?
Semaglutide should be avoided or used with extreme caution in:
- Patients with a history of medullary thyroid carcinoma
- Individuals with a history of pancreatitis
- Those with severe gastrointestinal disease (e.g., gastroparesis)
- Pregnant or breastfeeding women
- Patients with Type 1 diabetes
- Patients with severe eye problems due to diabetes (can be taken with care)
- Individuals seeking purely cosmetic weight loss without a medical indication.
© 2024 Bennett, Coleman & Company Limited

