- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Measles Outbreak Update: Kentucky Confirms Its First Case
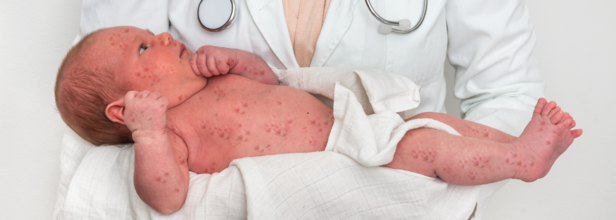
Credits: Canva
The latest state to join the measles outbreak, which has been ongoing for quite some time now in the United States, is Kentucky. It has declared the outbreak, and has been confirmed by the US Centers for Disease Control and Prevention (CDC) on Wednesday. So far, there has been a total of 1,267 confirmed cases of measles this year, nationwide.
For now, five active measles cases have been detected in Kentucky, and four of these are linked to the same outbreak.
"When there are measles outbreaks in other states and nearby countries, it is not surprising to see spread to Kentucky," Steven Stack, M.D., secretary of the Kentucky Cabinet for Health and Family Services, said in a statement. "Measles can be very serious, but it is avoidable through vaccination. We urge all parents to have their children vaccinated to ensure they are protected from preventable diseases like measles."
Also Read: This Year, Doctor's Day Reminded That Doctors Too Are Humans And Can Get Emotionally Exhausted
Measles: How Many Outbreaks And How Many Cases?
The CDC defines an outbreak as at least three related cases, and so far in 2025, 27 such outbreaks have been reported. Of them, 88% of the confirmed cases, which means 1,115 cases out of 1,267, are linked with the ongoing outbreak. In 2024, a total of 285 measles cases were reported by 33 jurisdictions, resulting in 16 outbreaks.
Since the late winter of 2024 till spring of 2025, Texas witnessed the country's largest outbreak, and three additional cases were reported this week. The case count in Texas now totals 753 since late January.
Last week, the New Mexico Department of Health reported five measles cases at the Luna County Detention Center in Deming. Officials are currently determining the vaccination status of people being held at the facility.
"The cases at Luna County Detention Center are a stark reminder that the measles outbreak in New Mexico is not over," Chad Smelser, M.D., a medical epidemiologist with the New Mexico Department of Health, said in a statement. "We urge everyone in New Mexico, especially Luna County residents, to ensure that they are fully vaccinated against measles."
So far, from the measles cases in Texas, New Mexico and Oklahoma, three deaths have been reported. Among them, two were elementary school-aged children from the West Texas epicenter, and one was an adult in New Mexico. All of them were unvaccinated.
What Vaccine Must One Take To Prevent Measles?
The CDC recommends two doses of the MMR vaccine as the "best way to protect against measles, mumps, and rubella". For children, it recommends two doses of MMRV.
The MMR vaccine is a combination of measles, mumps, and rubella vaccines, while the MMRV is a combination of measles, mumps, rubella, and varicella (chickenpox) vaccines.
In the US, two MMR vaccines are available for use, including M-M-R II, and PRIORIX. For MMRV, the vaccine is only licensed for children who are 12 months through 12 years of age. The first dose is usually administered between the ages of 12 to 15 months, while the second dose is administered between the ages of 4 to 6.
For older children, adolescents and adults, the two doses of MMR vaccines should be separated by at least 28 days.
What Is Measles?
CDC notes that it is a highly contagious virus, which means if one person has it, up to 9 out of 10 people nearby will also become infected. As per the Mayo Clinic, measles is caused by the measles virus, which can spread through an infected person's cough, sneeze, or even during conversations.
Measles: Signs And Symptoms
Measles symptoms appear 7 to 14 days after contact with the virus. Common measles symptoms include:
- High fever (may spike to more than 104° F)
- Cough
- Runny nose (coryza)
- Red, watery eyes (conjunctivitis)
- Rash
India Plans To Roll Out Universal Health Insurance By 2033, Says FM Nirmala Sitharaman

Credit: Sansad TV/X
Finance Minister Nirmala Sitharaman has announced in the Parliament that India is planning to launch universal health coverage for all by 2033.
Addressing the Rajya Sabha, the Finance Minister stated that health insurance has become a priority area for the government, and informed that the sector has made significant progress, covering 58 crore lives in 2024–25, news agency PTI reported.
“Health insurance is a priority for this government. In fact, we are hoping that by 2033 we will have insurance cover for all,” Sitharaman said.
Growing Insurance Market
The FM added that the total health premium collections in the country reached Rs 1,17,505 crore in 2024–25. The health premiums under
- Public sector insurers accounted -- INR 42,420 crore
- Private insurers contributed INR 37,752 crore
- Standalone health insurers INR 37,331 crore
“Health insurance is now a clear priority with GST exemption on individual premiums, expansion of coverage, and strong regulatory push driving the momentum,” she said.
Health Insurance Under AB-PMJAY
Ayushman Bharat Pradhan Mantri Jan Arogya Yojana (AB-PMJAY), the world’s largest publicly funded health insurance scheme, launched in 2018, provides health cover of Rs 5 lakh per family per year. It provides secondary and tertiary care hospitalization to about 12 crore families, representing the bottom 40 per cent of the population.
The scheme was further expanded to cover 6 crore senior citizens of age 70 years and above, belonging to 4.5 crore families, irrespective of their socio-economic status.
Union Minister of State for Health and Family Welfare, Prataprao Jadhav, stated in a written reply in the Rajya Sabha that
till February 28:
- 43.52 crore Ayushman cards created
- 1.14 crore Ayushman Vay Vandana cards created for senior citizens
- 36,229 hospitals empaneled under AB-PMJAY -- 19,483 are public, and 16,746 are private hospitals
Further, the latest national master of Health Benefit Package provides cashless healthcare services for 1,961 procedures across 27 medical specialties.
“A total of 11.69 crore hospital admissions amounting to Rs. 1.73 lakh crore have been authorized under the scheme,” Jadhav said.
He added that more than 86 crore Ayushman Bharat Health Accounts (ABHA) have been created, and more than 90 Crore health records have been linked to patients’ ABHA.
In addition, Ayushman Bharat Digital Mission (ABDM) was launched in India in September 2021 to support the development of an integrated and citizen-centric national digital health ecosystem.
Till March 11, the progress made under ABDM includes:
- 86,64,46,563 - ABHA created for citizens
- 90,70,14,529 - Health records linked to the patient’s ABHA
- 2,56,542 - Facilities using ABDM-enabled software.
HPV: 3 Lakh Girls Vaccinated in India in Just Two Weeks
Credit: iStock
India’s Human Papillomavirus (HPV) vaccination drive that began a fortnight ago has already vaccinated nearly 3 lakh girls aged 14 years, according to the Union Health Ministry.
The nationwide free HPV vaccination campaign for girls aged 14 years was launched by Prime Minister Narendra Modi from Rajasthan's Ajmer on February 28.
“Within just a fortnight of its launch, nearly 3 lakh girls aged 14 years have already been vaccinated—marking an encouraging start to this critical public health initiative,” the health ministry said.
"The enthusiastic participation seen so far reflects growing awareness among parents, schools, and communities about the importance of early protection," it added.
Further, the Ministry noted that several states, including Madhya Pradesh, Andhra Pradesh, Tamil Nadu, Gujarat, Odisha, and Mizoram, have seen a significant uptake in the nationwide HPV vaccination campaign.
The initiative marked a decisive step towards eliminating cervical cancer through timely HPV vaccination.
Cervical cancer remains the second most common cancer among women in India. Nearly 80,000 new cases and over 42,000 deaths are reported annually in the country.
The Ministry said that despite examinations currently underway in many regions, the response to the campaign has remained strong, and the momentum is expected to accelerate significantly in the coming days.
“We are leaving no stone unturned to ensure that the daughters of the country are healthy and prosperous. The objective of this initiative is the prevention of cervical cancer," the Prime Minister, earlier wrote in a post on social media platform X.
The government has urged parents and guardians to support and encourage eligible girls to get vaccinated at the earliest.
HPV Vaccine in India
HPV vaccination is voluntary, and parental consent is mandatory before administration of the vaccine.
The single-dose Gardasil-4 vaccine is administered free of cost at government health facilities across all areas, including rural and underserved areas, and will be available even after the campaign ends.
The vaccine used is non-live and does not cause HPV infection. It is supported by more than 500 million doses administered globally since its introduction in 2006.
The vaccine is most effective when it is administered before exposure to HPV and before becoming sexually active. Young women aged 9 to 14 years show vaccine effectiveness of 74 to 93 per cent and this decreases with age.
- Girls aged 9 to 14 should get two doses of the vaccine 6 to 12 months apart
- Women aged 15 to 26 years can get three doses in 0, 2, and 6 months apart
- Adults aged 27 to 45 must get it after consultation with their healthcare provider
To avail the free HPV vaccine, visit any government health facilities including
- Ayushman Arogya Mandirs- Primary Health Centres (PHCs
Argentina Exits The World Health Organization

Credit: Reuters/iStock
Argentina has formally withdrawn from the World Health Organization (WHO), its foreign minister has announced.
The country follows the footsteps of the United States, which in January made its exit from the global health body, after President Donald Trump condemned the WHO for not properly handling the deadly COVID-19 pandemic.
Argentina, a key ally of Trump, also criticized the WHO on its role during COVID and made the formal notification of withdrawal last year. Based on the provisions of the Vienna Convention on the Law of Treaties, the withdrawal takes effect one year after a notification is made.
Taking to the social media platform X, the country's Foreign Ministry reported that Argentina has now completed the withdrawal process within the timeframe stipulated by international treaties.
"Today, Argentina's withdrawal from the World Health Organization (WHO) takes effect, marking one year since the formal notification made by our country," Foreign Minister Pablo Quirno said on X.
"Our country will continue to promote international cooperation in health through bilateral agreements and regional forums, fully safeguarding its sovereignty and its decision-making capacity in health policy matters," he added.
In 2025, Argentina declared that "the WHO's recommendations are ineffective because they are not based on science, but on political interests", the AFP reported.
Presidential spokesperson Manuel Adorni told a press conference at the time that the decision "gives the country greater flexibility to implement policies adapted to the context and interests that Argentina requires, as well as greater availability of resources, and reaffirms our path towards a country with sovereignty also in matters of health", Xinhua news agency reported.
US' Withdrawal From The WHO
While WHO's membership is nearly universal, and withdrawals are extremely uncommon, the United States, earlier in January this year, became the first country to formally withdraw from the UN health body.
It comes a year after Trump signed an executive order to exit the multinational grouping on his return to the White House.
In its statements, the United States cited as one of the reasons for its decision, “WHO failures during the COVID-19 pandemic”, including “obstructing the timely and accurate sharing of critical information” and that the WHO “concealed those failures”.
The World Health Organization (WHO) was founded on April 7, 1948, when its constitution officially came into force, making it a specialized agency of the United Nations.
The global health body has been instrumental in eradicating smallpox and tackling public health threats like polio, HIV, Ebola, and tuberculosis.
Global Health Funding Takes A Hit
In January, WHO chief Tedros Adhanom Ghebreyesus said he deeply regretted the move, saying it would make the United States and the rest of the world unsafe.
The withdrawal of the US -- accounting for nearly a fifth of the WHO’s budget -- also affected its budget. Ghebreyesus also warned of falling donor support and severe budget cuts.
The agency is facing “the greatest disruption to global health financing in memory” as contributions fall sharply across the board, the WHO chief said.
The WHO has revised its financial plans, scaling back its current spending and proposing a 21 percent cut for the 2026-2027 budget cycle.
In November 2025, the global health body announced that its workforce will shrink by nearly a quarter or over 2,000 jobs by mid 2026.
© 2024 Bennett, Coleman & Company Limited

