- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
- Web Stories
Mental Health Funding Cuts: What You Need to Know

Credits: Canva
Various health agencies in the United States of America have been targeted by the Trump Administration. Thus, they are subjected to many new rules, including cost cutting. Amid all this, another key federal agency which is responsible for addiction and mental health services is facing deep staff cuts.
This is called the Substance Abuse and Mental Health Services Administration (SAMHSA). It has a $7.2 billion budget. It also looks after oversees vital services, for instance the 988 National Suicide and Crisis Lifeline, opioid addiction treatment programs and mental health grant funding.
What is SAMHSA?
It is an agency within the US Department of Health and Human Service, now being led by Robert F Kennedy Jr. It leads public health efforts to advance behavioral health of the nation. It also envisions that people with, affected by, or at risk for mental health and substance use conditions receive care, achieve well-being and thrive.
It also provides training for nonprofits and state agencies and monitors federal grant spending.
Dora Dantzler-Wright, who works with the Chicago Recovering Communities Coalition, says recent federal budget cuts have already affected operations. "We just continue to do the work without any updates from the feds at all," she said. "But we’re lost."
The cuts are part of a broader effort to lower government expenses. Last month, the Substance Abuse and Mental Health Services Administration (SAMHSA) lost about 10% of its workforce, and employees were offered $25,000 to leave voluntarily. Meanwhile, the Department of Health and Human Services (HHS) is reducing its regional offices from 10 to just four.
What Do Experts Believe?
Mental health and addiction specialists warn that reducing SAMHSA’s workforce could have serious consequences. In a letter obtained by The New York Times, U.S. Reps. Paul Tonko (New York) and Andrea Salinas (Oregon) called the cuts "extremely dangerous," especially given the ongoing behavioral health crises. Their letter was signed by 57 Democratic House members.
Overdose Deaths
SAMHSA has played a key role in combating overdose deaths, which peaked above 100,000 per year in recent years. While numbers have begun to decline, the CDC reported that 87,000 people still died from overdoses between September 2023 and September 2024.
Loss of Oversight and Accountability?
Regina LaBelle, former acting director of the Office of National Drug Control Policy, called the cuts "shortsighted." She warned that reducing staff may lower costs but also weakens oversight and accountability. Some experts worry that SAMHSA could be merged into another agency or see its funding return to 2019 levels, despite the continuing addiction and mental health crises.
The agency has not confirmed whether more layoffs are coming. However, an official told The Times that SAMHSA remains committed to working with partners across the country, despite staffing changes. For now, the future of mental health funding remains uncertain.
Ever since the Trump administration has come to power, many other health departments too have faced the cuts. This also includes USAIDS, for which the World Health Organization (WHO) has warned that it could put the vulnerable countries into risk as they would stop receiving funds to battle health crisis.
Common Heart Attack Pills May Not Be Safe For Women, New Study Shares Warning
Credits: iStock
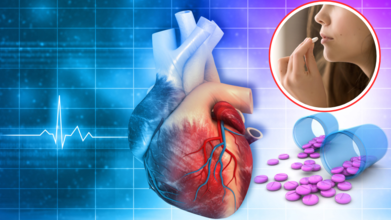
Latest research is challenging decades of established cardiac treatment, revealing that a commonly prescribed class of heart attack medications—beta-blockers—may not benefit most patients and could even pose significant risks for women. This groundbreaking finding, presented in major cardiology journals and conferences, underscores the urgent need for sex-specific approaches in cardiovascular care.
Beta-blockers have been a "heart" of heart attack management for decades, prescribed to help lower heart rate, reduce blood pressure, and decrease the heart’s oxygen demand. Their intended effect is to prevent further cardiac events and improve survival. However, new findings indicate that these benefits are not universal.
According to the REBOOT trial, women who suffered heart attacks but retained normal heart function measured by a left ventricular ejection fraction above 50%, experienced significantly higher risks when treated with beta-blockers. These women were more likely to be hospitalized for heart failure, experience another heart attack, and, alarmingly, nearly three times more likely to die than their counterparts not on the medication. The risk increased with higher doses.
“This is a pivotal moment in cardiology,” said Dr. Valentin Fuster, president of Mount Sinai Fuster Heart Hospital in New York City and director of Spain’s National Center for Cardiovascular Investigation. “These findings will reshape international clinical guidelines and emphasize the importance of sex-specific treatment strategies for cardiovascular disease.”
Why Women Respond Differently to Beta-Blockers?
The heart disease profile differs markedly between men and women, a factor long overlooked in clinical research. Men typically suffer from plaque buildup in major arteries, often presenting with classic chest pain during a heart attack. Women, on the other hand, more frequently experience issues in the smaller blood vessels of the heart and may exhibit atypical symptoms such as shortness of breath, indigestion, or back pain.
Historically, cardiovascular studies have largely focused on male patients, delaying recognition of these sex-based differences in presentation and treatment response. The new research highlights how generalized treatment protocols may inadvertently harm women while offering minimal benefit to those with normally functioning hearts.
The REBOOT Trial and Key Findings
The REBOOT study followed 8,505 men and women across 109 hospitals in Spain and Italy for nearly four years. Patients included in the trial all had a left ventricular ejection fraction above 40%, meaning their hearts were pumping normally. The trial specifically assessed whether beta-blockers provided benefits in preventing secondary cardiac events.
While men and women with mild heart dysfunction—ejection fraction between 40% and 50%—did see some benefit from beta-blockers, women with normal heart function did not. In this subgroup, beta-blocker therapy was associated with worse outcomes, including increased hospitalization and mortality rates.
“These results underscore the need to differentiate treatment plans based on both sex and heart function,” explained lead study author Dr. Borja Ibáñez of Madrid’s National Center for Cardiovascular Investigation. “The majority of patients following a first heart attack actually fall into this normal heart function category, meaning current beta-blocker prescriptions could be largely unnecessary, and in some cases, harmful.”
Heart Attacks Among Women: Conflicting Evidence from Other Trials
Interestingly, not all recent trials agree. The BETAMI–DANBLOCK study, which included 5,574 participants in Norway and Denmark, demonstrated that beta-blockers reduced the risk of death or major adverse cardiovascular events by 15%. Differences between the studies may stem from variations in patient age, beta-blocker type, and baseline heart function, but the critical takeaway remains, treatment is not one-size-fits-all.
Dr. Dan Atar of the University of Oslo noted, “While beta-blockers remain essential for patients with significant heart damage, for those with normal function, particularly women, the risk-benefit balance is much less favorable.”
What Are The Implications for Women’s Heart Health?
These findings are a clarion call for more gender-sensitive approaches in cardiology. Women account for nearly half of all heart attack cases, yet research and treatment protocols have historically centered on male physiology. The revelation that beta-blockers may pose a serious risk for women with normal heart function challenges long-held assumptions and emphasizes the importance of personalized medicine.
Experts urge women who have experienced a heart attack to discuss their treatment options thoroughly with their cardiologist, particularly if prescribed beta-blockers. Monitoring heart function via left ventricular ejection fraction and considering alternative medications may be safer in many cases.
How Do Beta-Blockers Work?
Beta-blockers function by blocking the effects of epinephrine and norepinephrine, calming the heart and reducing its workload. While this can be lifesaving for patients with compromised heart function, the drugs may unnecessarily suppress heart activity in individuals whose hearts are already pumping normally. This over-suppression could explain the increased hospitalization and mortality rates observed in women with healthy ejection fractions.
The implications of these studies extend beyond beta-blockers. They highlight a broader need for sex-specific research and personalized medicine in cardiology. Cardiovascular disease remains the leading cause of death globally, and addressing sex-based differences in treatment is critical to improving outcomes for all patients.
“The time for generic prescriptions is over,” said Dr. Fuster. “Cardiology must recognize that men and women respond differently to medications and that clinical guidelines must reflect these differences.”
In light of these findings, international guidelines may soon be revised to limit beta-blocker use to patients with reduced heart function or those at high risk of arrhythmias. Women with normal ejection fractions should have alternative treatment strategies considered to minimize potential harm.
Pharmaceutical companies producing beta-blockers, including Pfizer, Novartis, Teva, and Sun Pharma, may also need to review dosing recommendations and safety protocols to align with emerging evidence.
The new research into beta-blockers after heart attacks challenges a decades-old assumption in cardiology and emphasizes the importance of personalized, sex-specific treatment. For women with normal heart function, these commonly prescribed medications may offer no benefit and even increase risks. As the medical community revises guidelines and treatment protocols, patients and healthcare providers alike must prioritize individualized approaches to ensure the safest and most effective care.
NHS Launches Free Chickenpox Vaccine: How Vaccinations Can Help Keep Kids In School And Reduce Absenteeism

Credits: iStock
From January 2026, NHS England will offer free chickenpox vaccinations to eligible children, a move that promises to reduce illness, prevent hospital admissions, and minimize disruption to both children’s education and parental work schedules.
This historic addition to the childhood immunisation programme will protect approximately half a million children each year, offering not only medical protection but also supporting children’s academic performance and social development by keeping them in school.
Chickenpox, caused by the varicella zoster virus, is highly contagious. While often considered a mild childhood illness, it can sometimes lead to severe complications, including bacterial infections, pneumonia, inflammation of the brain, stroke, and, in rare cases, death. Adults who have not previously had chickenpox are at higher risk of serious illness. After initial infection, the virus remains dormant and can reactivate later in life as shingles, which is why the UK has maintained a shingles vaccination programme for older adults since 2013.
Dr. Gayatri Amirthalingam, Deputy Director of Immunisation at the UK Health Security Agency, emphasised that while chickenpox is often viewed as a minor disease, vaccination can be life-saving for children at risk of severe complications. "This programme will have a really positive impact on children’s health and also reduce missed nursery and school days," she said.
How Vaccination Supports School Attendance and Child Development?
One of the less-discussed benefits of the chickenpox vaccine is its impact on children’s education and social growth. School absenteeism due to illness disrupts learning, affects participation in extracurricular activities, and can hinder social interactions with peers. By preventing chickenpox, the MMRV vaccine ensures children remain in school, contributing to better academic performance and stable social development.
For working parents, the benefits are equally significant. Childhood chickenpox often forces parents to take time off work, affecting productivity. Research suggests that chickenpox in the UK results in an estimated £24 million in lost income annually, with an additional £15 million spent by the NHS on treatments. Keeping children healthy and in school not only improves their educational experience but also reduces the economic burden on families and public health systems.
NHS Evidence-Based Rollout
Eligible children will receive a combined measles, mumps, rubella, and varicella (MMRV) vaccine during routine GP appointments. This approach ensures high vaccine uptake while providing protection against multiple infectious diseases. The programme is informed by the Joint Committee on Vaccination and Immunisation (JCVI), which reviewed evidence showing the impact of severe chickenpox on children’s health, hospital admissions, and associated costs.
Private varicella vaccines currently cost around £150 for two doses, but the NHS rollout will make the vaccine free for eligible children, ensuring equitable access.
Lessons in Childhood Immunisation
Countries including the United States, Canada, Germany, and Australia have already incorporated the chickenpox vaccine into their childhood immunisation schedules, seeing dramatic reductions in incidence and related hospitalisations. In the US alone, CDC data shows that over 25 years, vaccination prevented 91 million cases, 238,000 hospital admissions, and 2,000 deaths. England’s adoption of the MMRV vaccine aligns with these global best practices, offering children the safest and most effective protection.
Protecting Vulnerable Populations and Building Community Immunity
Beyond individual protection, the vaccine helps shield vulnerable populations such as pregnant women and immunocompromised patients. By reducing the circulation of the varicella virus, community immunity is strengthened, limiting outbreaks and preventing infections in children who cannot be vaccinated due to medical conditions.
Integration With Broader Health Initiatives
The chickenpox vaccine rollout is part of the government’s “Plan for Change,” aimed at raising the healthiest generation of children ever and shifting NHS focus from treatment to prevention. It complements other measures in the 10-Year Health Plan, such as free school meals, mental health services, and dental care. Additionally, the Department for Education’s Best Start Family Hubs will further support families, ensuring more children receive the healthiest possible start in life.
Moving Beyond “Chickenpox Parties”
Historically, some parents exposed children to chickenpox intentionally through “chickenpox parties” to develop natural immunity. Today, evidence-based immunisation replaces these practices with safe, effective, and preventative healthcare. Parents will be contacted by GP surgeries to schedule MMRV vaccinations, which will follow age-specific clinical guidance to ensure maximum effectiveness.
What Are The Long-Term Benefits of Free Vaccination for Children?
By preventing chickenpox, children experience fewer school absences, maintain consistent peer interactions, and avoid the stress and discomfort of illness. This creates a foundation for better academic performance, stronger social bonds, and overall well-being. The reduction in parental work disruption also contributes to family stability and societal productivity.
Amanda Doyle, NHS England’s National Director for Primary Care and Community Services, highlighted the significance of the rollout, “This is a very welcome moment for families as the NHS prepares to offer a vaccine to protect children against chickenpox for the first time. It complements other routine jabs that safeguard against serious illness and supports children in staying healthy and in school.”
The NHS chickenpox vaccination programme marks a proactive step in public health, combining disease prevention with educational and social benefits. Protecting half a million children each year, it ensures not only reduced illness and hospitalisation but also supports uninterrupted schooling, positive social development, and stronger family and community health. England’s children are poised to become the healthiest and most resilient generation yet, thanks to this strategic immunisation initiative.
'Act Now To Protect Yourself ', Warns AMA As Whooping Cases Hit Decades-High, Calls For Vaccinations
Credits: iStock
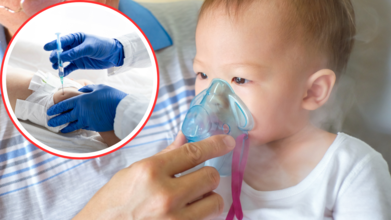
Australia is facing its largest whooping cough outbreak in more than three decades, with medical leaders sounding an urgent alarm: vaccination is the only reliable shield. Whooping cough, or pertussis, is not a new disease, but it is making a dramatic comeback. In 2024, more than 57,000 cases were reported across Australia the highest number since 1991. And the wave has not slowed. In South Australia, early 2025 data show over 1,000 infections — more than ten times higher than the same period last year.
The national disease surveillance dashboard reports nearly 19,000 cases already in 2025, with hotspots including Queensland, South Australia, and Western Australia’s Kimberley region. Doctors say this is now Australia’s most significant and long-lasting pertussis outbreak in decades.
Pertussis is caused by the bacterium Bordetella pertussis. It spreads easily through coughs and sneezes, thriving in close-contact settings such as households and schools. For most adults, it causes weeks of relentless coughing that disrupts sleep, work, and quality of life. But for infants — especially those too young to be vaccinated it can be life-threatening.
Newborns can develop severe respiratory distress, pneumonia, and even brain damage from prolonged oxygen deprivation during coughing fits. Globally, the World Health Organization estimates that pertussis kills tens of thousands of children every year, most of them under six months old.
AMA’s Urgent Call
The Australian Medical Association (AMA) has issued a clear warning: complacency is dangerous. AMA President Dr. Danielle McMullen described the outbreak as “extremely concerning,” citing both the sheer scale of cases and the drop in vaccination coverage.
“We can’t afford to be complacent,” Dr. McMullen said. “Each year, thousands of lives are lost to respiratory diseases like whooping cough — and we all have a role to play in preventing their spread. Vaccination remains our most powerful defence.”
Why Pregnancy Vaccination is Crucial?
One of the AMA’s strongest messages is directed at expectant mothers. A pertussis-containing vaccine is recommended during every pregnancy, ideally between 20 and 32 weeks. This approach allows protective antibodies to pass from mother to baby through the placenta, shielding the newborn during the critical first weeks of life.
“Maternal vaccination creates antibodies which are passed to the unborn baby and protect them in their first days and weeks of life,” Dr. McMullen explained. “But it doesn’t stop there — ensuring family members and other caregivers are also vaccinated helps create a protective cocoon around infants.”
This cocooning strategy reduces the risk that parents, grandparents, siblings, or caregivers will transmit the infection to newborns who are too young to complete their first immunization schedule.
Vaccines Are Free and Accessible
In Australia, whooping cough vaccines are free for all pregnant women under the National Immunisation Program. Parents are also encouraged to keep their children’s vaccines up to date, particularly during the first six months, when infants are most vulnerable.
For adults, boosters are recommended every 10 years, especially for anyone living with or caring for babies. General practitioners and pharmacies can check vaccination records and provide catch-up doses when needed.
Falling Vaccination Rates and Rising Cases
Part of what makes this outbreak alarming is its timing. Australia has not met its childhood vaccination targets in several regions, and vaccine hesitancy has crept upward in recent years. This leaves pockets of communities vulnerable, creating fertile ground for pertussis to spread.
The AMA warns that failing to address this could undo decades of progress in reducing serious childhood diseases. “Getting vaccinated is one of the simplest and most effective ways you can protect your loved ones and your community,” Dr. McMullen said.
Learning From History
Australia has seen waves of whooping cough before. The last major epidemic peaked in 2011 with over 38,000 cases. But today’s surge is different in scale, surpassing even that crisis and persisting longer. Globally, other countries have also seen cyclical rises in pertussis, underscoring that this is not just an Australian problem.
The key difference between a contained outbreak and a devastating one is vaccination coverage. Experts point to herd immunity thresholds: when enough people are vaccinated, the chain of transmission breaks, protecting those who cannot be immunized.
Though the latest figures come from Australia, health experts stress that this is a global concern. Travel and migration mean outbreaks do not remain confined to national borders. Declining vaccination rates in parts of the United States and Europe could set the stage for similar resurgences.
For families worldwide, the lessons are clear: stay up to date on vaccinations, encourage maternal immunization, and understand that diseases once considered “childhood illnesses of the past” can and do return if immunity gaps open.
Australia’s pertussis outbreak is a wake-up call for all of us. With more than 57,000 cases in a single year and rates still climbing, whooping cough has proven it can resurge when vaccination rates slip.
The AMA’s message is urgent but simple: act now. Pregnant women, parents, and caregivers should prioritize immunization to protect both themselves and those too young to be vaccinated. Free vaccines are available, and the science is clear immunization saves lives. As Dr. McMullen put it, “We must not lose sight of the fact that immunisation saves lives.”
© 2024 Bennett, Coleman & Company Limited

