- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Not From The Brain, Scientists Trace Parkinson’s Disease To This Organ In Your Body
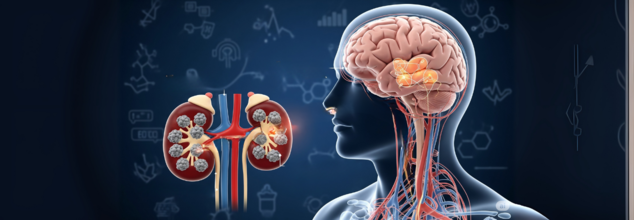
Credits: Health and me
For decades, Parkinson's disease has long been thought of as a brain disorder, characterized by the degeneration of dopamine-producing neurons in the substantia nigra — a region of the brain that regulates movement. The loss of these neurons progressively contributes to hallmark symptoms such as tremors, rigidity, and decreased movement. But groundbreaking new research appearing in the journal Nature Neuroscience is refuting that long-standing assumption. The roots of Parkinson's may not be in the brain at all, according to scientists from Wuhan University in China — they could be in the kidneys.
The new study, by a Wuhan University team in China, focuses on alpha-synuclein (α-Syn), a protein intimately associated with Parkinson's. Under normal conditions, α-Syn is involved in healthy neural function. But when it misfolds and aggregates, it becomes toxic and clumps together into Lewy bodies—Parkinson's and other related disease hallmarks.
This unexpected finding is based on an increasing amount of evidence that Parkinson's could start in peripheral organs and spread to the brain, as opposed to starting in the brain itself. The potential ramifications for early treatment, prevention, and detection are staggering.
According to the authors of the study, "We show that the kidney is a peripheral organ that is an origin of pathological α-Syn." Central to this research is a protein called alpha-synuclein (α-Syn) — already far and away with links to Parkinson's disease and other neurological disorders. In health, this protein is used in neuron function. But when it goes awry, it forms sticky clumps known as Lewy bodies, which disrupt brain function and are a hallmark of Parkinson's and dementia with Lewy bodies.
To reach their conclusion, the team performed a succession of very careful experiments. They studied kidney samples from individuals with Parkinson's and associated Lewy body dementias, as well as patients with chronic kidney disease (CKD) with no neurological symptoms. The results were dramatic: abnormal α-Syn growth was identified in the kidneys of 10 out of 11 individuals with Parkinson's or Lewy body dementia, and in 17 out of 20 CKD patients—even though these CKD patients had no evidence of disease in the brain during life.
What they discovered was astounding: Abnormal α-Syn deposits were found in 10 out of 11 Parkinson's or related disorder patients. But even more astonishing, 17 out of 20 CKD patients — with no known brain disorder — also exhibited early evidence of the same misfolded proteins in their kidneys.
This implies that protein clumping could start in the kidneys, many years before symptoms of neurological harm become evident. Traces of α-Syn pathology were also detected in regions of the brainstem and spinal cord in a few instances, again favoring the hypothesis of a kidney-to-brain route.
How Do the Kidneys Affect Parkinson's Risk?
The kidneys are not passive waste filters; they also actively remove α-Syn from the bloodstream. When kidney function is impaired, as in chronic kidney disease, this elimination process is defeated. The consequence is the accumulation of toxic proteins within the kidneys, which migrate to the brain and ultimately trigger the damage cascade causing Parkinson's.
This shift in paradigm is strengthened by epidemiological data. Massive research has revealed that individuals with compromised kidney function are at considerably greater risk of getting Parkinson's disease. The correlation is nonlinear, with increasing steepness in the risk as kidney function worsens.
Are There Multiple Triggers for Parkinson's?
This link between kidneys and brain doesn't imply the brain isn't involved in Parkinson's, but it doesn't exclude other causes either. Indeed, past studies have indicated that the gut might also be a place where α-Syn is accumulated and transmitted to the brain early on. The new research indicates Parkinson's could be a multi-system disorder, initiated by a range of causes and mechanisms—such as the kidneys, the gut, and possibly even the heart.
As the authors of the study point out, "Removal of α-Syn from the blood may hinder the progression of Parkinson's disease, providing new strategies for therapeutic management of Lewy body diseases."
Implications for Diagnosis and Treatment
The revelation that the kidneys could have a central role in Parkinson's offers both new hope for early detection and intervention. If α-Syn accumulation in the kidneys can be identified before neurological signs are apparent, it might be an early warning sign, enabling the possibility of preventive measures or early treatment.
In addition, treatments to enhance kidney function or facilitate clearance of α-Syn from the bloodstream may prove to be useful weapons in the battle against Parkinson's and other disorders. This strategy would complement current methods, which target preservation of the brain's dopamine-neurons.
Although the research is revolutionary, it isn't without its constraints. The human tissue sample was quite small, and though mice work well as models for human biology, they are not replicas.
Even so, the evidence is compelling enough to support more research. Subsequent studies with bigger human populations, improved imaging technology, and more comprehensive genetic analysis could replicate and build on these findings.
If confirmed, the kidney-brain link might be the missing piece of the Parkinson's puzzle — setting the stage for earlier diagnosis, tailored treatments, and even preventive medicine aimed at flushing out or blocking α-Syn in the kidneys and blood.
The kidneys could be a silent trigger for Parkinson's disease, with poisonous protein accumulation moving from the kidneys into the brain. Keeping kidneys healthy might be the key in the battle against neurodegenerative disorders.
US Woman In Active Labor Forced to Face Court Over Refusal Of C-Section
Credit: ProPublica
In a disturbing case from the US state of Florida, a pregnant woman in active labor was forced to attend a virtual court hearing via Zoom from her hospital bed for refusing a Cesarean delivery, also known as C-section — a common method of childbirth.
ProPublica reported that Cherise Doyley was in her 12th hour of contractions at the University of Florida Health facility, when she was, without her consent, made to sit in front of a host of people — a judge in a black robe and several lawyers, doctors, and hospital staff — for the Zoom proceeding.
While in active labor, a nurse came in with a bedsheet and told her to cover up, and a supervisor followed with a tablet.
“It’s a real judge in there?” Doyley asked the nurse at the beginning of what would be a three-hour hearing.
What Was The Case?
The mother of three, and a professional birthing doula, Doyley had arrived at the facility after her water broke.
While her doctors expressed concerns about the risk of uterine rupture —a potentially deadly complication for her and her baby — Doyley wanted to try for a vaginal delivery, as the risk was less than 2 percent, unless there was an emergency.
She told doctors she wouldn’t consent to a cesarean without trying to have a vaginal delivery first.
While the doctors initially relented, after several hours, she had to face a virtual court hearing, where the hospital and state attorney’s office forced Doyley to undergo a cesarean section.
Doyley has her own reasons to avoid a C-sec. She already had three prior C-sections, and one that resulted in a hemorrhage. She feared that a C-sec would lead to another serious complication and a lengthy recovery, and her kids would suffer.
However, the hospital was worried that her medical decisions may cause harm to the fetus, and that the courts may help decide which one mattered more, the report said.
Also read: Maternal Vaccination During Pregnancy Can Prevent COVID-related Hospitalization In Babies: Study
After three hours of testimony — all while Doyley lay in her hospital bed — the judge ruled that she could keep laboring unless there was an emergency. If that happened, the hospital could operate, whether she wanted it or not.
Overnight, doctors said the baby’s heart rate dropped for seven minutes. Doyley woke to her hospital bed being wheeled into surgery. The baby girl was delivered by C-section, the report said.
What Happens In A C-section?
It is a surgical procedure that is used to deliver a baby through an incision made in the abdomen and uterus.
The method is preferred, especially in cases with complications during labor or breech presentation, or multiple births.
Unlike the popular conception, it hurts. In a vaginal delivery, the pain is experienced during labor and pushing, especially if done without an epidural.
Whereas, in a C-section, a surgery is performed that numbs the body from the chest down. However, the recovery could be painful and prolonged. It is also because in a C-section, it involves healing from a major abdominal surgery, while vaginal birth recovery may be quicker, more complicated, or traumatic.
Also read: 'Husband Stitch': A Medical Necessity Or Just A Tool To Objectify Women's Bodies?
Does A C-sec Affect The Baby?
Usually, it does not harm the baby, but there could be potential risks to the baby, including:
- Surgical injury, which is very rare; however, the baby may be accidentally nicked during the incision.
- Respiratory issues: Babies born via C-section may have a higher risk of breathing, since they miss the natural compression during the vaginal birth that helps expel the amniotic fluid from their lungs
- Delayed bonding: Immediate skin-to-skin contact may take longer due to the surgical process.
- Feeding challenges: Some newborns may initially struggle with breastfeeding.
Risks Of A C-section Birth?
- Excessive blood loss
- Infection
- Blood clots in the legs, lungs, or pelvis
- Damage to nearby organs
- Adverse reactions to anesthesia
The American College of Obstetricians and Gynecologists (ACOG) advises against elective C-sections due to these potential complications.
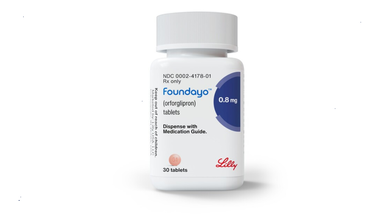
Foundayo: US FDA Approves Eli Lilly’s GLP-1 Weight Loss Pill

Credit: iStock
American drugmaker Eli Lilly’s first oral pill for weight loss, Orforglipron, marketed as Foundayo, has been given the green signal by the US Food and Drug Administration (FDA).
Lilly is also known for injectable drugs like Zepbound for obesity and Mounjaro and Trulicity for diabetes.
Foundayo’s approval comes after the US FDA in December last year approved Novo Nordisk’s Wegovy pill — the first-ever GLP-1 pill for weight loss. The Danish drugmaker rolled out the pill in January this year.
Novo Nordisk was also the first to launch oral GLP 1 Rybelsus to treat type 2 diabetes. It was approved by the US FDA in September 2019.
Also Read: World Autism Awareness Day 2026: Can Cell Therapy Be The Future Of Autism Treatment?
In a statement, the US FDA said that "Foundayo has been approved for use in combination with a reduced-calorie diet and increased physical activity. The pill is targeted to reduce excess body weight and maintain weight reduction for the long term in adults with obesity or overweight".
Lilly said that the drug will be available from April 6 through its its direct-to-consumer platform LillyDirect at a cost of $149 per month for the lowest dose for self-pay customers — on par with Novo's pill. "Shortly after” it will be available through retail pharmacies and telehealth providers in the US.
"Today, fewer than 1 in 10 people who could benefit from a GLP-1 are taking one, held back by access, stigma, perceived complexity, or the belief that their condition isn't serious enough for treatment. We believe Foundayo can help level the playing field for those living with obesity or who are overweight and living with weight-related complications," said David A. Ricks, chair and CEO of Eli Lilly and Company.
"As a convenient, once-daily oral pill that delivers meaningful weight loss, this is obesity care designed for the real world," he added.
Foundayo: A Meaningful Reduction In Body Weight
The US FDA approved Foundayo after two randomized, double-blind, placebo-controlled trials in adults with obesity or with overweight showed benefit.Also Read: Foundayo: US FDA Approves Eli Lilly’s GLP-1 Weight Loss Pill
In these trials, 72 weeks of treatment with Foundayo, in combination with a reduced-calorie diet and increased physical activity, resulted in a statistically significant and clinically meaningful reduction in body weight.
Deborah Horn, Director of the Center for Obesity Medicine at McGovern Medical School at UTHealth Houston, stated that Foundayo “delivered an average of 12.4 percent weight loss at the highest dose in clinical trials – addressing both the clinical realities of obesity and the practical challenges patients face every day."
In addition, Foundayo also led to reductions in many markers of cardiovascular risk, including waist circumference, non-HDL cholesterol, triglycerides, and systolic blood pressure across all doses, Eli Lilly said.
How Foundayo Works
Lilly licensed Orforglipron, the main ingredient in Foundayo, from a Japanese pharmaceutical company in 2018.
As with the injectable forms of GLP-1s, Foundayo is available in six doses, ranging from 0.8mg to 17.2mg.
In consultation with their doctors, patients start with the lowest dose and gradually work up to higher doses; not everyone may need to reach the highest dose.
Also read: Eli Lilly's Experimental GLP-1 Pill Shows Promising Weight Loss
Unlike the Wegovy pill, people taking orforglipron do not need to restrict food or drink after taking the pill. Orforglipron is a small molecule that the body can absorb quickly and get into the blood, where it reaches the necessary tissues.
Foundayo: Side Effects
Foundayo is not safe for use in children and has an increased list of side effects, such as tumors in the thyroid, including thyroid cancer.
The drugmaker urged watching for possible symptoms, such as
- a lump or swelling in the neck,
- hoarseness,
- trouble swallowing
- shortness of breath.
- nausea,
- constipation,
- diarrhea,
- vomiting,
- indigestion,
- stomach (abdominal) pain,
- headache,
- swollen belly,
- feeling tired,
- belching,
- heartburn,
- gas,
- hair loss.
New Zealand Launches Surveillance After Spotting Dengue, Zika-carrying Mosquito Larvae

Credit: Canva
New Zealand has stepped up surveillance after the first detection of a dengue and Zika-carrying mosquito larvae in the country.
The larval species was confirmed as 'Aedes aegypti' — known to carry diseases including dengue fever, yellow fever, Zika, and chikungunya, across the globe.
As New Zealand does not normally have the mosquito species, the larvae detected were counted as "exotic".
The mosquito species did not cause any outbreak, but were spotted during a routine surveillance program in Auckland.
"The National Public Health Service has commenced a heightened surveillance and interception programme following mosquito larvae being collected from a routine surveillance trap at Queens Wharf, Auckland, on Monday 30 March," Health New Zealand said in a statement.
Health New Zealand reported that exotic species were occasionally found at ports and airports.
Not A Public Threat Yet
The health body noted that the larvae were not considered a public health or biosecurity threat yet because there was no indication they had become established.
But the agency aimed to continue "intensive monitoring for at least three weeks".
"The monitoring would take place within a 400m radius of the site where the larvae were identified. Health Protection Officers would place mosquito traps in the survey area," the statement said.
"These have been hidden away from plain sight so they are not disturbed, for example, in old tyres, bushes, or pools of water. We ask members of the public to avoid touching or disturbing these traps if they find them, as it may disrupt our monitoring and trapping efforts," medical officer of health Dr David Sinclair said.
Sinclair said New Zealanders were most at risk from diseases transmitted by mosquitoes when travelling overseas, including to Pacific Island countries and territories where dengue fever was known to be present.
Dengue Surging In 17 Countries
The US Centers for Disease Control and Prevention recently issued a travel alert of dengue outbreaks across 17 countries.
The CDC alert issued on March 23 identified 17 countries reporting an increased number of cases of dengue. These include: Afghanistan, Bangladesh, Bolivia, Colombia, Cook Islands, Cuba, Guyana, Maldives, Mali, Mauritania, New Caledonia, Pakistan, Samoa, Sudan, Timor-Leste, Vietnam, and the United States territories of American Samoa, Puerto Rico, and the US Virgin Islands, where local transmission is already common.
Also read: Long-term Exposure To Air Pollution Increases Fatality Rates In Dengue: Study
What Is Dengue?
Dengue is a disease caused by a virus spread through mosquito bites. It is transmitted through infected mosquitoes, primarily the species Aedes aegypti.
The breakbone fever is caused by an infection with any of four different dengue viruses. These include:
• Dengue virus type 1 (DENV-1 or DEN-1)
• Dengue virus type 2 (DENV-2 or DEN-2)
• Dengue virus type 3 (DENV-3 or DEN-3)
• Dengue virus type 4 (DENV-4 or DEN-4)
Also read: New dengue vaccine over 80% effective, prevents severe disease for up to 5 years
Common Symptoms of dengue include:
• Sudden onset of high-grade fever.
• Intense headache
• Severe muscle, joint, or bone pain.
• Skin Rash that often appears 2–5 days after the fever starts
• Nausea and Vomiting
• Minor bleeding
• Fatigue.
© 2024 Bennett, Coleman & Company Limited

