- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
After 27 Years In A Coma, This Woman Opened Her Eyes And Shocked Everyone- How People Wake Up From Comas?

Image Credit: Canva
Comas continue to be among the most mysterious illnesses of modern medicine, holding patients between life and death for weeks, months, or even years. Certain patients mysteriously wake up, while others do not. Coma-waking mechanisms continue not to be well understood and thus remain an active area of medical research.
One such astounding instance is the case of Munira Abdulla, who fell into a coma after a road accident in 1991. For 27 years, the doctors thought that she would never fully wake up. Then, in 2018, she stunned everyone by displaying signs of recovery, even shouting out her son's name.
Her tale mesmerized the world, raising deep questions about consciousness, medical potential, and the morality of prolonged life support. Did she know what was happening around her the entire time? How will she fit into a world that has altered so profoundly? And what does this imply for families struggling with tough end-of-life choices? As science continues to investigate the secrets of the human brain, cases such as Abdulla's provide promise and challenge our conception of coma recovery.
Coma is a long-term state of unconsciousness where an individual fails to respond to the environment. It results from multiple causes, such as traumatic brain injury, intoxication, metabolic derangement, stroke, and neurological disorders. Comas are sometimes medically induced to safeguard the brain from further injury.
Every case of coma is different, and the length can be incredibly varied. Some patients come out of their comas in a matter of days, while others are comatose for decades, such as Munira Abdulla, who awoke 27 years after a vehicle accident left her in a vegetative state.
For an individual to wake up from a coma, their brain has to heal a great deal. The healing process is either through the regeneration of lost neurons or reorienting existing brain pathways to replace lost function. Yet, brain functioning in a coma is greatly retarded, and this process is highly unpredictable. Scientists have speculated that the brain needs a "jump start" to reestablish normal communication among neural networks, but the trigger factor remains elusive.
What are the Potential Triggers for Waking Up from Coma
Although there is no surefire way to wake an individual from coma, scientists have picked out a number of possible triggers that could help in recovery of consciousness:
1. Dopamine-Boosting Medications
The most encouraging strategy involves boosting dopamine levels in the brain. Dopamine is a neurotransmitter that plays an important role in movement control and motivated behavior. Research has established that patients in coma have decreased dopamine activity.
One drug, amantadine, which is generally prescribed for Parkinson's disease, has been promising in the recovery of coma. A 2012 New England Journal of Medicine study discovered that amantadine enhanced awareness in patients who were in coma due to traumatic brain injury. Although the drug seems to hasten awakening, there is no definite proof that it enhances long-term recovery.
2. Deep Brain Stimulation (DBS)
Deep brain stimulation is another experimental method under investigation. The procedure involves the surgical implantation of electrodes deep within the brain, focusing on the thalamus—a part critical to attention and arousal. Electrical stimulation can potentially awaken dormant neural circuits and promote consciousness recovery.
A 2018 review in Neurosurgical Focus noted instances where DBS restored awareness among coma patients. The method, however, remains experimental, and its success rate differs from one patient to another.
3. Non-Invasive Brain Stimulation
Other non-surgical methods, including transcranial magnetic stimulation (TMS) and focused ultrasound, seek to stimulate brain activity with non-invasive means. These treatments apply magnetic fields or ultrasonic vibrations to activate deep-brain neurons, which could help restore consciousness.
Although initial studies are promising, they need additional clinical trials to determine their efficacy in coma recovery.
Why Do Some Patients Never Wake Up from a Coma?
Even with advances in medicine, most coma patients never wake up. It is estimated that 20% to 40% of coma patients never wake up. In a study done in the U.S. and the UK, it was discovered that 54% of coma patients died, 15% survived with severe disability, and only 31% had good outcomes.
One of the chief determining factors is the degree of brain damage. If the vital areas of the brain, e.g., brainstem or cortex, are damaged severely, then the chances of recovery of consciousness become very less. Also, unconsciousness of a long duration can result in muscle wasting, organ failure, and other secondary complications that may impede recovery.
The mystery of how patients emerge from comas is still one of the biggest medical enigmas. Some patients awaken spontaneously, but others need treatment, and others never wake up at all. The study of dopamine-boosting medications, deep brain stimulation, and non-surgical therapies brings hope to coma recovery. As technology progresses, we can soon have the potential to induce more patients to awaken sooner and lead their lives back.
Until then, coma patients' families have to live in uncertainty, hoping that science will keep on unraveling the mysteries of the brain and consciousness.
1 In 4 Diabetic Patients in India Suffer from Liver Fibrosis, Finds Lancet Study
Credit: iStock
One in four or 25 percent of adults with type-2 diabetes in India also suffer from liver fibrosis, according to an alarming study published in The Lancet Regional Health Southeast Asia journal today.
With data from more than 9,000 patients across the country, it is the largest ever real-world survey of liver fibrosis in type 2 diabetes from any low- or middle-income country.
While fatty liver disease has been touted as the most common liver condition among diabetes patients, the new study established liver fibrosis as the real danger among people with high blood sugar.
“Type 2 diabetes is closely linked to fatty liver disease (also known as MASLD). But how common is liver Fibrosis — the real danger — in Indian diabetics? Our answer: 1 in 4 has clinically significant liver fibrosis. One in 20 already has probable cirrhosis. Most had no symptoms. We propose liver fibrosis as the ‘4th major complication’ of diabetes,” said Ashish Kumar, from Ganga Ram Postgraduate Institute of Medical Education and Research (GRIPMER), from Sir Ganga Ram Hospital, in a post on social media platform X.
What Did The Study Find?
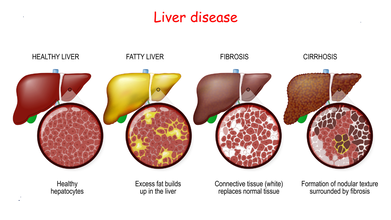
Fatty liver is typically the first and reversible stage of liver disease, where excess fat builds up in liver cells. Left untreated, it progresses to liver fibrosis, which is the excessive accumulation of scar tissue (collagen) in the liver resulting from chronic inflammation. The condition then progresses to the third and late stage, irreversible scarring (fibrosis) of the liver. The final stage is liver cancer.
The DiaFib-Liver Study included a total of 9,202 adults with type-2 diabetes patients who underwent FibroScan (VCTE) to assess liver fibrosis in routine diabetes care.
Of these:
- 26 percent had clinically significant fibrosis,
- 14 percent had advanced fibrosis,
- 5 percent had probable cirrhosis
- 65 percent had fatty liver disease.
- obesity
- dyslipidaemia
- kidney problems
- diabetes duration ≥10 years.
Fibrosis: The Screening Target
The study suggested the urgent need to integrate fibrosis screening into national diabetes programs.
“One in four adults with type 2 diabetes in India has clinically significant liver fibrosis and one in twenty already has probable cirrhosis, establishing advanced liver disease as a 'fourth major complication' of diabetes,” said the researchers.
“The DiaFibLiver Study calls for: Fibrosis — not steatosis — as the screening target. FibroScan integration into routine diabetes care. Moving beyond ultrasound-based referral,” Jha said.
“We hope this data from India adds to the global conversation on diabetes and liver disease,” he added.
Also read: The Silent Rise of Fatty Liver Disease: How India-Specific Guidelines Can Help
The findings highlight the urgent need to:
- move beyond steatosis
- systematically integrate fibrosis assessment into routine diabetes care,
- deploy non-invasive tools such as vibration-controlled transient elastography (VCTE) in community practice
- define screening strategies,
- evaluate therapeutic interventions.
Everyday Habits That Harm the Liver
Certain lifestyle choices can accelerate liver damage, such as:
Overeating processed or fried foods
High sugar intake (soft drinks, sweets, desserts)
Physical inactivity or prolonged sitting
Ignoring health issues like diabetes or hypertension
Crash dieting or taking unprescribed supplements.
How To Improve Liver Health?
Early screening and detection are key to prevent irreversible stages. Yet liver disease can be prevented with lifestyle changes such as:
- Eating a balanced diet with vegetables, fruits, whole grains, and lean protein
- Engaging in at least 30 minutes of exercise daily
- Staying hydrated to help the liver flush out toxins
- Avoiding alcohol and smoking
- Avoiding self-medication and unnecessary pills
- Getting routine health screenings.
Problem Of Plenty: Psychiatrist Explains How Too Many Choices Affect Mental Health

Taking too many decisions in a day can lead to mental exhaustion. (Photo credit: iStock)
New Delhi: Every day, the brain processes hundreds of choices. Most pass unnoticed: what to wear, which route to take, what to eat. But accumulated over hours and across competing demands, this constant decision-making exacts a cost. Decision fatigue is the gradual erosion of the brain’s capacity to make good choices, and over time it affects both mental functioning and physical health. Dr Shivi Kataria, Consultant – Psychiatry, CK Birla Hospitals, Jaipur, addressed the problem of plenty and said that it could take a toll on mental health in certain circumstances.
Read more: India Launches 1st Repository Of Data On Major Psychiatric Disorders
What are the signs?
The earliest signs tend to be emotional. Simple decisions start to feel disproportionately heavy. Choosing between two options takes longer than it should. Irritability surfaces. Tasks that once felt manageable begin to pile up as the mental energy required to engage with them thins. Procrastination, self-doubt, and a general withdrawal from decisions are common responses, with the brain essentially rationing what little capacity remains.
Cognitive symptoms follow. Concentration narrows. Judgement becomes less reliable. Small errors accumulate. People in this state often describe feeling mentally stuck, present in the room but unable to engage with any clarity or momentum.
The physical dimension is frequently overlooked. Headaches, low energy, disrupted sleep, and difficulty sustaining attention are all associated with sustained decision overload. These symptoms register what prolonged mental strain produces in the body and are worth taking seriously.

Who is most at risk?
Decision fatigue affects most people at some point, but the load is not evenly distributed. Professionals in high-responsibility roles, caregivers, and anyone managing multiple competing demands make a disproportionately high number of decisions each day. By the end of a long day, the quality of choices made about food, purchases, relationships, or work often reflects exhaustion more than intention.
Read more: Smartphone Overuse Linked To Rising Risk Of Eating Disorders Among Youth, Study Finds
Is there a solution?
Reducing the number of decisions that require active thought each day is the most direct intervention. Fixed routines for meals, schedules, and recurring tasks remove the need to deliberate repeatedly over the same ground. This is conservation of mental energy, and it compounds over time.
Important decisions are better made earlier in the day, when the brain is rested and cognitive resources are intact. Short breaks during sustained work periods allow partial recovery. Even brief physical activity or deliberate rest between decision-heavy tasks restores some capacity.
The brain has a finite decision-making budget each day. Spending it on low-stakes choices leaves less available for the ones that carry real consequence.
Over 30% Fever Cases In India Linked To Dengue, Typhoid: Report
Credit: iStock
While fevers are often overlooked and brushed aside or even managed with antibiotics — a dangerous trend — an alarmingly nationwide study linked it to infectious diseases with far-reaching consequences.
The report, based on data of over one lakh individuals in India with fever, between 2023 and 2025, showed that these were not vague or self-limiting, but in more than 30 percent or one-third cases had clear links to serious infections, such as dengue, and typhoid.
According to the report by healthcare diagnostics company Thyrocare, the fevers were mostly linked with
- typhoid – in over 18 percent cases
- dengue -- over 14 percent cases.
- Other diseases include malaria, chikungunya, and leptospirosis.
Presence Of Multiple Infections
Importantly, the findings highlighted the presence of co-infections in 10 per cent cases. The most common was a combination of dengue and typhoid.
Dr Preet Kaur, Chief Scientific Officer, Thyrocare, said that a significant number of patients carry serious infections, sometimes more than one at a time, revealing patterns that simple assumptions cannot capture.
"Beyond the visible rise in temperature, laboratory markers highlight hidden stress on organs, from drops in platelet counts to elevated liver enzymes, underscoring that fever is a systemic signal, not an isolated event," she added.
Also read: ‘Breakbone Fever’: US CDC Warns Of Dengue Surge Across 17 Countries
Further, the report noted that dengue positivity declined significantly over the three-year report period, malaria increased despite its lower overall base.
Typhoid and chikungunya rose in 2024 before easing in 2025 but remained present across the testing population.
Also read: Drug Resistance Driving Severe Typhoid Disease, Death Among Children Under-5s in India: Lancet Study
Fever: Men Vs Women
The report noted that more women were affected with typhoid than men. On the contrary, men reported more malaria cases.
More than 32 percent of females had fevers compared to 29 percent of men. Fevers in women was largely driven by higher typhoid detection (21 percent vs 15 percent).
Malaria affected men more than twice as often as women (1.1 percent vs 0.5 percent).
The lab reports also revealed key physiological markers such as platelet counts and liver function among people with fever, dengue, and malaria.
Low platelet levels were seen in
- 27 percent of patients with fever
- 80 percent malaria positive patients
- 37 percent dengue-positive patients
- All fever patients (56 percent) showed elevated SGOT levels and 37 percent SGPT
- Liver stress was seen across patients with dengue, malaria and leptospirosis.
Dengue cases rose throughout the year and typically peaked around October.
Typhoid positivity steadily fell from 2023 to its lowest in 2025. Despite a mild monsoon spike each year, 2025 remained consistently lower overall.
Chikungunya cases rose gradually from lower, volatile levels in 2023, peaked sharply in 2024, and moderated to a softer trend in 2025.
Malaria positivity remained relatively low overall but increased during the monsoon months, with transmission peaking between May and September.
Over the three-year period, malaria positivity rose from 0.5 percent to 1.1 percent, indicating a gradual increase despite its lower overall base.
© 2024 Bennett, Coleman & Company Limited

