- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Are Vitamin Deficiencies Secretly Sabotaging Your Hair Growth?

Image Credit: Canva
Hair loss can be a distressing experience, affecting both self-esteem and overall well-being. While various factors contribute to thinning hair, one of the most overlooked causes is vitamin deficiencies. And for months now, I watched my hair thin, only after a seemingly regular session with my hairdresser turned into a reality check. I unaware that my fatigue and brittle strands were signs of vitamin deficiencies and a simple blood test revealed the truth and am I on the road to restoring balance back my original hair health.
Essential nutrients play a critical role in maintaining the health of hair follicles, and when the body lacks key vitamins, the hair growth cycle is disrupted, leading to excessive shedding and weak strands.
A poor diet, hormonal fluctuations, and underlying health conditions can all contribute to nutritional deficiencies that impact hair health. Understanding the connection between vitamins and hair loss is crucial to addressing the root cause and restoring balance. Dr. Neha Khuraana, MD, dermatologist sheds light on the key vitamins responsible for healthy hair and offers expert guidance on restoring nutrient balance for optimal hair growth.
Hair follicles undergo a continuous cycle of growth, rest, and shedding. For this cycle to function optimally, the body requires an adequate supply of vitamins and minerals. Deficiencies in certain nutrients can weaken hair strands, delay regrowth, and even lead to conditions such as alopecia.
Which Vitamin Deficiency Causes Hair Loss?
Vitamins deficiencies in certain vitamins can disrupt the hair growth cycle, leading to thinning, breakage, and excessive shedding. Among the most significant culprits, two stand out:
Vitamin D Deficiency
Vitamin D is essential for hair follicle health and growth regulation. Research indicates that inadequate levels of this vitamin may contribute to hair loss by disrupting the natural hair cycle. When the body lacks sufficient vitamin D, hair strands become weaker and more prone to shedding.
Biotin (Vitamin B7) Deficiency
Biotin, also known as vitamin B7, is a key player in strengthening hair follicles and promoting new growth. When biotin levels drop, hair may become brittle, dull, and prone to breakage.
Iron Deficiency
Another key nutrient is iron, which ensures proper oxygen transport to hair follicles. When the body lacks iron, hair strands become weak, resulting in increased shedding. Vitamin B12 is also integral to red blood cell production, which helps nourish the scalp and promote strong, healthy hair growth.
Zinc Deficiency
Lastly, zinc is a vital mineral involved in the repair and maintenance of hair follicles. Deficiency in zinc can lead to excessive shedding and slower hair regrowth.
How to Identify If You Have Vitamin-Related Hair Loss?
Certain individuals are more prone to experiencing hair loss due to vitamin deficiencies. People with curly hair often struggle with dryness and breakage, which can be worsened by a lack of essential nutrients. Additionally, those with genetic hair loss conditions, such as androgenic alopecia, may notice faster hair thinning when their diets are poor in vitamins and minerals.
Hormonal imbalances, such as those seen in PCOS (polycystic ovary syndrome), pregnancy, and postpartum stages, can also contribute to nutrient depletion, leading to hair loss. Another overlooked factor is chronic stress, which has been linked to low levels of vitamin B12, folic acid, ferritin, zinc, and vitamin D. Stress can trigger hair shedding, making it essential to maintain a balanced diet and manage stress levels effectively.
How Blood Tests Can Help Detect Deficiencies
For those experiencing persistent hair loss, a blood test can provide valuable insights into vitamin deficiencies. Doctors often recommend tests for vitamin D, serum ferritin (iron storage), vitamin B12, zinc, and biotin levels to determine whether nutritional gaps are affecting hair health. Additionally, a thyroid function test can help identify hormonal imbalances that may contribute to excessive shedding.
Expert-Recommended Ways to Restore Hair Growth
According to Dr. Neha Khuraana, addressing vitamin deficiencies is key to reversing hair loss and restoring hair strength. She shares five expert-backed strategies to improve hair health naturally:
1. Prioritize a Nutrient-Rich Diet
“The first and most important step to preventing vitamin deficiency-related hair loss is consuming a wholesome diet,” says Dr. Khuraana. She emphasizes the importance of whole grains, leafy greens, fresh fruits and vegetables, lentils, and lean meat to provide essential vitamins and minerals that support hair growth.
2. Consider Supplements When Necessary
“If your diet lacks certain nutrients, supplements can help bridge the gap,” she explains. However, supplementation should always be done under the supervision of a healthcare professional to ensure the correct dosage and prevent excess intake, which can have adverse effects.
3. Use Targeted Hair Serums
For those struggling with hair thinning, Dr. Khuraana recommends serums enriched with peptides and essential oils. “These serums provide added benefits by strengthening the hair shaft and nourishing the scalp,” she adds. Regular application can improve hair texture and promote regrowth.
4. Retest Every 3-6 Months
If a deficiency is detected through blood tests, Dr. Khuraana advises regular retesting every 3-6 months to monitor progress and adjust treatment plans accordingly. “Tracking your nutrient levels can help you make necessary dietary changes and ensure long-term hair health,” she notes.
5. Maintain Overall Scalp Health
Beyond diet and supplementation, she emphasizes the importance of scalp care. “A healthy scalp is the foundation of strong hair,” she says. This includes gentle cleansing, avoiding harsh chemicals, and using nourishing hair masks to maintain hydration and prevent breakage.
Hair loss caused by vitamin deficiencies is both preventable and treatable with the right approach. A balanced diet, targeted supplementation, and proper scalp care can help restore lost nutrients and improve hair health. For individuals experiencing persistent hair thinning, consulting a healthcare professional and undergoing necessary blood tests can provide personalized solutions for regrowth.
As Dr. Khuraana highlights, "Hair health is a reflection of overall well-being. Nourishing your body from within is the key to maintaining strong, healthy hair."
Dr. Neha Khuraana MD, is a Board-certified Dermatologist and founder of House of Aesthetics, Delhi in India
Death Cap Mushroom Poisoning Claims California Resident’s Life: Symptoms And Risks Explained

Credits: Canva
A California man died last weekend after eating so-called death cap mushrooms, marking the third fatality linked to the toxic fungi in the state since November.
Health officials say California is seeing an unusually high number of mushroom poisonings this season. Between November 18 and January 4, at least 35 cases were reported statewide. In a typical year, the number is usually fewer than five.
“This year’s figures are far beyond what we normally see,” said Sheri Cardo, a communications specialist with the California Department of Public Health.
California Resident Dies After Eating Death Cap Mushrooms
At least three people have now lost their lives in California due to death cap mushroom poisoning since November. Media reports indicate a sharp rise in cases tied to foraged wild mushrooms, with more than 35 poisonings recorded over the past three months.
“The numbers we’re dealing with this year are comparatively off the charts,” Cardo told NBC News.
The most recent death occurred in Sonoma County and was the first fatal wild mushroom poisoning reported there this season, according to county health officials.
Dr. Michael Stacey, interim health officer for Sonoma County, urged residents to avoid eating wild mushrooms unless they are purchased from reliable grocery stores or licensed sellers. He warned that death cap mushrooms can look strikingly similar to safe, edible varieties.
What Is Death Cap Mushroom Poisoning?
Death cap mushrooms, scientifically known as Amanita phalloides, are among the most poisonous mushrooms in the world. They commonly grow beneath oak trees and can be found in parks, gardens, and wooded areas.
Experts say these mushrooms are often mistaken for edible types because of their appearance. Typical features include:
- A smooth cap that may appear whitish, pale yellow, light brown, or green
- White gills underneath the cap
- A white spore print
- A cup-like structure called a volva at the base of the stem
- A ring, known as an annulus, around the stem
Death Cap Mushroom Symptoms
Symptoms usually begin between six and 24 hours after ingestion. Early signs often include stomach pain, nausea, vomiting, and diarrhoea.
In many cases, symptoms ease or disappear after one or two days, which can create a false sense of recovery. By that point, however, the toxins may have already caused severe damage to the liver.
According to experts, the poison responsible, known as amatoxin, can seriously harm the liver, kidneys, and digestive system. Without prompt treatment, the damage can be fatal.
U.S. Poison Centers receive an average of about 52 calls each year related to amatoxin exposure, said Hallen-Adams, though not every case is officially reported.
Is the Risk Easing?
The danger may now be starting to decline in parts of California. Mike McCurdy, president of the Mycological Society of San Francisco, said he has noticed far fewer death cap mushrooms during recent foraging trips.
Earlier this winter, McCurdy said he spotted hundreds of death caps during a two- to three-hour walk in Sonoma County. On a recent outing near Lafayette, California, he found just one. “I think we’re getting close to the end,” he said.
Do You Wear Contact Lenses? This Rare Eye Parasite Can Permanently Damage Your Vision
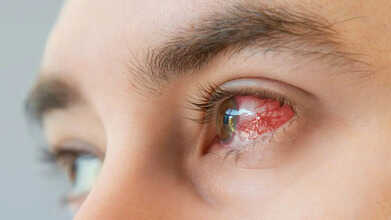
Credits: Canva
Nearly four years ago, Teresa Sanchez was in Mexico for a medical procedure when her right eye began to feel unusually dry and irritated. At first, it seemed minor. She assumed her contact lens might be torn or that the switch from daily lenses to monthly ones was causing dryness. She even wondered if her body was fighting off an infection, as per CNN.
What she did not realize at the time was that a microscopic organism was slowly attacking her cornea. Over the next three months, the parasite caused irreversible damage to her vision and triggered searing pain that spread across her head.
“I couldn’t even keep the blinds open in my room,” said Sanchez, now 33 and living in Las Vegas. “Light would cause unbearable pain. That’s when I knew something was seriously wrong.”
By then, she had already seen multiple optometrists and had been misdiagnosed. Frustrated and desperate for answers, Sanchez began researching her symptoms on her own.
What Is Acanthamoeba Keratitis?
Online searches led Sanchez to a condition she had never heard of: acanthamoeba keratitis. An eye specialist later confirmed it. Keratitis refers to inflammation of the cornea, the clear, dome-shaped layer at the front of the eye that plays a central role in focusing vision. Acanthamoeba is a microscopic, single-celled organism that cannot be seen without a microscope.
According to Dr. Jacob Lorenzo-Morales, a professor of parasitology at the University of La Laguna in Spain, acanthamoeba is commonly found in soil and water. It does not require a host to survive, which makes it especially resilient.
Once the organism comes into contact with the eye, it can attach itself to the cornea. Dr. Paul Barney, an optometric physician and director at the Pacific Cataract and Laser Institute in Alaska, explained that even tiny breaks in the corneal surface can allow the parasite to burrow deeper into the eye.
Why Contact Lens Wearers Face Higher Risk?
Acanthamoeba keratitis is considered rare. Based on data from 20 countries, including the UK, India, the US, Canada and Brazil, there are more than 23,000 cases worldwide each year. Yet a striking pattern stands out. Between 85% and 95% of people who develop the infection wear contact lenses.
Contact lenses can cause microscopic abrasions on the cornea, creating an entry point for the parasite. The organism can also cling to the lens itself or become trapped between the lens and the eye, making it easier to penetrate the corneal tissue.
“If it’s not diagnosed early and treated aggressively, the outcome can be devastating,” Barney said. “The parasite feeds on the cornea, triggering inflammation and tissue damage that can lead to permanent vision loss.”
In some cases, vision can be partially restored with treatment. Others require a corneal transplant.
A Parasite Built To Survive
Treating acanthamoeba keratitis is especially difficult because the organism has strong defense mechanisms. It can sense threats and respond by forming a cyst, allowing it to lie dormant for months or even years.
This resilience means treatment often stretches over long periods and involves intense discomfort. Because the eye is extremely sensitive, patients must work closely with specialists and strictly follow treatment instructions.
Why The Condition Is Often Missed?
Early diagnosis is one of the biggest challenges Because acanthamoeba keratitis is uncommon, many optometrists may not recognize it right away. As a result, many contact lens users only learn about the condition after they develop it or come across viral videos discussing it online.
Many patients have expressed surprise that they were never clearly warned about the risks of wearing contacts while showering or swimming.
The Contact Lens Society of America emphasized that contact lenses are medical devices and require strict hygiene. This includes avoiding water exposure during swimming, showering or sleeping. The organization also stressed the importance of patients asking questions and carefully reviewing care instructions.
Acanthamoeba Keratitis: Symptoms That Mimic Other Eye Infections
In addition to severe pain and light sensitivity, acanthamoeba keratitis can cause redness, blurred vision, dryness, excessive tearing and the sensation that something is stuck in the eye.
Because these symptoms overlap with other conditions, misdiagnosis is common. Barney said the infection is frequently mistaken for herpes simplex keratitis, a major cause of infection-related blindness. In its earliest stages, it can even resemble pink eye.
That was the case for Sanchez. Her first optometrist diagnosed pink eye. The prescribed drops blurred her vision. A second optometrist suspected a bacterial infection, and while antibiotic drops offered brief relief, she soon lost vision in the affected eye.
Acanthamoeba Keratitis: How To Reduce Your Risk?
Experts stress that contact lens hygiene is critical. Always clean and store lenses using approved contact lens solution, never water. The solution in your lens case should be replaced daily. Wash and dry your hands thoroughly before handling lenses.
Sleeping in contact lenses should be avoided, as it increases dryness, irritation and the risk of corneal damage. Daily disposable lenses may lower infection risk compared to monthly lenses.
For water-based activities, glasses or prescription goggles are safer options. Some people may also consider vision correction surgery after discussing risks and suitability with a doctor.
Taking NSAIDs For Osteoarthritis? NHS Shares An Important Warning
Credits: Canva
More than 10 million adults, young people, and children in the UK are currently living with arthritis, according to a 2025 report by Arthritis UK. The NHS says osteoarthritis is the most common form of the condition across the country.
NHS Issues Warning For People Taking NSAIDs For Osteoarthritis
Osteoarthritis develops when joints become stiff and painful over time. Symptoms vary widely depending on the joint involved and the severity of damage. While medication is often used to manage pain and inflammation, the NHS warns that some commonly used treatments can carry risks if not taken correctly.
One of the most widely used options for pain relief is NSAIDs, a group of medicines many people rely on daily.
What Are NSAIDs And Why Are They Prescribed?
NSAIDs, or non-steroidal anti-inflammatory drugs, are commonly prescribed by GPs to relieve pain, swelling, and inflammation. They are available in several forms, including tablets, capsules, suppositories, creams, gels, and injections. Some NSAIDs can be bought over the counter, while stronger versions require a prescription.
Common types of NSAIDs
The most commonly used NSAIDs include:
- ibuprofen
- naproxen
- diclofenac
- celecoxib
- mefenamic acid
- etoricoxib
- indomethacin
- aspirin for pain relief (low-dose aspirin is not usually classed as an NSAID)
Doctors usually advise which NSAID is suitable and explain the potential benefits and risks. However, the NHS stresses that patients should also understand possible side effects and when to seek medical help.
NHS Warning On Who Should Be Cautious With NSAIDs
The NHS advises that NSAIDs may not be suitable for everyone. Extra caution is needed if you have asthma, stomach ulcers, angina, or if you have previously had a heart attack or stroke. People taking low-dose aspirin should always speak to their GP before using an NSAID.
Who Should Avoid Or Seek Advice Before Taking NSAIDs?
You should consult a pharmacist or doctor before using NSAIDs if you:
- are over the age of 65
- are pregnant or trying to conceive
- are breastfeeding
- have asthma
- have had an allergic reaction to NSAIDs in the past
- have a history of stomach ulcers
- have heart, liver, kidney, blood pressure, circulation, or bowel problems
- are taking other medicines
- are buying medicine for a child under 16 (aspirin should never be given to children under 16)
The NHS explains that NSAIDs are not always completely avoided in these cases, but they should only be used with medical advice, as the risk of side effects may be higher.
If NSAIDs are unsuitable, doctors or pharmacists may recommend alternatives such as paracetamol.
Possible Side Effects Of NSAIDs
Over-the-counter NSAIDs generally cause fewer side effects than prescription-strength versions. However, risks increase when they are taken at high doses, used for long periods, or taken by older adults or people with underlying health conditions.
Possible side effects include:
- indigestion, stomach pain, nausea, and diarrhoea
- stomach ulcers, which can lead to internal bleeding and anaemia
- headaches
- drowsiness
- dizziness
- allergic reactions
In rare cases, NSAIDs can affect the liver, kidneys, heart, or circulation, and may increase the risk of heart failure, heart attacks, or strokes.
Taking NSAIDs Alongside Other Medicines
It is essential to seek medical advice before taking NSAIDs if you are already using:
- another NSAID
- low-dose aspirin or warfarin
- ciclosporin
- diuretics for high blood pressure
- lithium
- methotrexate
- selective serotonin reuptake inhibitors (SSRIs) such as citalopram or fluoxetine
Signs And Symptoms Of Osteoarthritis
Common symptoms of osteoarthritis include joint pain, stiffness, and difficulty moving the affected joints. Some people may also experience:
- swelling
- joint tenderness
- a grating or crackling sensation when moving joints
- pain and stiffness after periods of inactivity
- enlarged or knobbly joints
- reduced range of movement
- muscle weakness or muscle loss
The NHS notes that osteoarthritis can affect almost any joint but most commonly involves the knees, hips, and small joints of the hands. Anyone with persistent symptoms should see their GP for diagnosis and treatment advice.
Even people who do not fall into higher-risk groups should only use NSAIDs as directed by a healthcare professional. Side effects can still occur, especially with long-term use. If NSAIDs are not appropriate, safer alternatives may be suggested to manage pain effectively.
© 2024 Bennett, Coleman & Company Limited

