- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Belly Up Or Down? What Should Be The Correct Sleeping Position?

Belly up or belly down, does it really matter when it comes to sleeping? Well, it does. Your sleeping position could be either helping or hurting your health. It is linked with back pain, digestion and many more.
Sleeping On Your Back
There are many benefits of sleeping on your back. It is great for keeping your spine aligned and reduces pressure on your joints. It also is a go-to choice for those who struggle with back aches. If you have issues with acid reflux or heartburn, slightly raising your head can help keep stomach acid from rising up, and offers relief during the night.
However, there are cons too. Sleeping on your back can worsen snoring and it is not ideal if you have sleep apnea. Lying on your back can make it harder for air to pass through the throat and can worsen your breathing issues.
Sleeping On Your Sides
Sleeping on your sides is one of the most common positions, especially if you are sharing your bed. It also has benefits. It is helpful for reducing snoring and tends to be gentle on the spine, especially if you put a pillow between your knees and keep your hips aligned. Sleeping on your left side may also be beneficial for digestion, as it helps food move down through the stomach more easily. It can even improve circulation and reduce acid reflux.
The cons include shoulder and hip discomfort, especially if you don't switch sides now and then. Curling up too tightly in the fetal position can also put extra pressure on our neck and back and can leave you feeling stiff in the morning.
Fetal position is very common and it can help relieve back pain for some people. It is especially helpful during pregnancy as it can improve the blood flow of the baby. However, the downsides include restriction in breathing.
Sleeping On Your Stomach
This may not be very common, however, it does have some benefits, especially if you want to reduce your snoring by keeping the airway more open. This can be beneficial if you have mild breathing issues that only crop up at night.
Are there cons? Yes. This position can be rough on your body as it forces you to turn your head to one side, which can strain your neck, and it is difficult to keep your spine in a neutral position, often causing lower back pain.
Over time, this position could also lead to joint and nerve issues and can make it a long-term health.
Health Tests Every Woman Should Do Once A Year
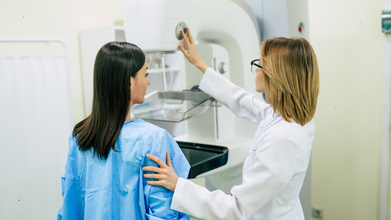
Credit: iStock
A woman’s health check-up is not about being paranoid. It's about refusing to treat your body as an afterthought.
You may not be able to control every diagnosis you ever get. But you can control how late you meet it. That's what preventive care is all about. Early detection through these screenings helps manage hormonal changes, cancer risks, and metabolic health.
From routine blood tests to specialized screenings, Dr. Supriya Bali, Director, Internal Medicine, Max Super Speciality Hospital, Saket, spoke to HealthandMe on specific tests crucial for women, right from their 20s
In Your 20s: Laying A Strong Foundation
Your 20s are all about establishing healthy habits that will carry you through life. Even if you feel great, this is a crucial time to get in the habit of seeing your doctor regularly.
Recommended screening includes:
- Blood pressure check – Every 1-2 years if normal; more often if elevated
- Pap smear – Start at age 21 (or by age 25 if you’ve never been sexually active); every three years if results are normal
- Chlamydia and gonorrhea screening – Annually for sexually active women under 25
- HPV vaccine – If not already completed by 26
- Skin check – Monitor moles and sun damage, especially if you tan easily
- Mental health screening – Don’t ignore stress, anxiety, or depression
In Your 30s: Reproductive And Preventive Health In Focus
As the body begins to undergo subtle changes in the 30s, regular screenings, hormonal health checks, and lifestyle adjustments are increasingly important.
Recommended screenings in 30s include:
- Pap + HPV co-test – Every 5 years starting at 30 (or Pap every 3 years)
- STI screening – Based on risk factors and symptoms
- Blood pressure and cholesterol check – Especially if you have a family history
- Blood sugar test – Especially if you’re planning a pregnancy or have had gestational diabetes
- Breast exam – Regular self-monitoring and breast ultrasound if you suspect a lump.
- Mental health and sleep – Ongoing check-ins with your doctor
- Fertility discussions – If you're planning or delaying pregnancy
Also read: 'Husband Stitch': A Medical Necessity Or Just A Tool To Objectify Women's Bodies?
In Your 40s: Monitoring Long-Term Risk Factors
This is a time when early signs of chronic conditions may start to show up, especially if there’s a family history of heart disease, diabetes, or cancer.
You should get these screenings at certain times:
- Mammography screening: Begin at 40 years of age (earlier if you have a family history of breast cancer).
- Pap smear & HPV test: Pap and HPV every 5 years or Pap alone every 3 years.
- Cholesterol & Blood Pressure Testing: Every 1-2 years.
- Blood glucose test (diabetes screening): especially if you're overweight or at risk for diabetes.
- Thyroid function testing is optional—especially if you feel tired, cold, or have been losing weight or have changes in your bowel habits.
- Weight discussions regarding healthy nutrition and active lifestyle—assist with maintaining a healthy weight.
- Perimenopause begins in your 40's; if you experience mood swings or changes in sleep, hot flashes, or irregular cycles, please speak with your doctor.
Also read: What Your Mammogram Says About Your Heart?
In Your 50’s: Maintain Strength, Stay Ahead of Aging
Maintaining your strength, the ability to prevent illness/disease from affecting you, and remaining proactive against the challenges that arise due to aging will be your focus at this stage.
Every individual will have their own unique series of recommended screenings; however, everyone will benefit from some type of recommended screening.
Some commonly recommended screenings include:
- Mammogram screening program; every 1-2 years.
- Colorectal cancer screening, beginning at age 45 through age 75.
- Bone density scan-if at high risk.
- Hearing/Vision checks annually or as required (on an as-needed basis).
- Blood pressure, cholesterol, and diabetes screening every year.
- Lung cancer screening among those with a history of smoking.
- Vaccines--including shingles, pneumonia, flu, and COVID-19 booster.
- Cognitive screening - to discover memory concerns, changes in mental sharpness, or cognitive function.
Why Miscarriage Needs Emotional Care At Par with Medical Treatment: Doctors Explain
Credit: Canva
Conceiving after 7 years of marriage—riddled with societal shame and self-doubt and a host of tests—was a moment of immense joy to Shalini, a 30-year-old IT professional.
Shalini was cared for, pampered, and showered with gifts. But the happiness was short-lived. At 10 weeks, her doctor delivered devastating news: there was no fetal heartbeat, and the pregnancy would have to be terminated.
Shalini couldn’t process; years of taunts of not being able to deliver a child came back to her ears—a voice so profound that she was unwilling to abort, let come what may.
However, in a week, the miscarriage occurred. She woke up at 2 am with intense abdominal pain and felt her womb rolling. She rushed to the toilet and found herself in a pool of blood. Her baby was gone.
For more than an hour, she continuously pushed out huge chunks of blood clots—the flesh of her unborn baby. Shalini cried. Then she went numb.
Doctors cleaned her up, but nobody bothered to heal her emotional burden—of not being able to deliver a baby successfully.
Years passed; Shalini delivered a healthy baby girl, but deep inside her, she still cries for her lost baby.
Shalini is not alone; more than one in five pregnancies worldwide end in miscarriage. While physical recovery is often addressed, emotional care is still met with silence.
The body may heal with treatment and nourishment, but internally, many women grapple with grief, anxiety, and a profound sense of loss that often goes unrecognized and untreated, said doctors, stressing the need for addressing the emotional toll.

What Is A Miscarriage?
A miscarriage is the loss of a pregnancy or the unexpected ending of a pregnancy in the first 20 weeks of gestation.
Most of them occur in 12 weeks and are classed as early miscarriages, while far fewer happen between 13 and 24 weeks.
Symptoms include
- vaginal bleeding,
- cramping like a period pain,
- decrease in pregnancy symptoms.
These occur when the fetus stops growing before 20 weeks.
As per the World Health Organization (WHO), miscarriage is the most common reason for losing a baby during pregnancy. WHO defines a miscarriage as a baby that dies before 28 weeks.
Miscarriage: Mental Health Implications
Also read:UK Women Who Suffer From Miscarriage May Get Two Weeks Paid Leave
Miscarriage often causes sadness, disinterest, sleeplessness, and depression. Many times, women experience low self-esteem and guilt.
There can also be marital issues, differences in psychological reaction of the spouse, and self-blame. There is also a sense of deep personal loss and trauma. It can lead to symptoms such as
- PTSD,
- feelings of yearning,
- emptiness,
- emotional numbing.
HealthandMe spoke to some mental health experts to understand what women who face the unexplained loss suffer.
“Miscarriage in women leads to many adverse consequences in psychological, social, marital, and physical domains. Most immediate effect is an acute feeling of loss, grief, and bereavement,” Dr. Savita Malhotra, President of the Indian Psychiatric Society, told HealthandMe.
She added that women who faced miscarriage can also feel anxiety over future pregnancies.
“About 20-30 percent of women after miscarriage show clear depression and anxiety. A similar number may show PTSD. Women who have an earlier history of miscarriage, trauma, or mental illness are more prone to mental ill health,” Dr Malhotra said.
Also read: Why Many Older Men Struggle to Conceive Despite ‘Good Health’
So why do women face these emotional turmoil?
"The lack of open conversation can intensify isolation, making women feel their pain is invisible or minimized. Social stigma and well-meaning but dismissive comments further deepen the wound," Dr. Chetna Jain Director Dept of Obstetrics & gynecology Cloudnine Group of hospitals, Gurugram, told HealthandMe.
Dr Deepak Raheja, a New Delhi-based psychiatrist, said that miscarriage is not just a medical event; for many women, it represents the loss of a deeply hoped-for future.
"Hormonal changes, lack of open conversations around pregnancy loss, and a tendency to internalize blame can make the emotional impact even heavier," the doctor told HealthandMe.
The experts urged the need for better familial support and good marital relationships that can prevent mental health issues in women.
Recognizing miscarriage as both a medical and emotional event is essential. Compassionate care, counselling, and supportive communities play a critical role in healing and long-term wellbeing.
Also read: Planning A Pregnancy In The 30s: Expert Answers FAQs On Women's Fertility in 30s
Dr Malhotra said, "There's a need for clear mental health intervention and psychiatric treatment."
"It is important to recognize miscarriage as a legitimate form of bereavement," added Dr Raheja.
Compassionate care from families and healthcare professionals, along with timely psychological support, can help women process the loss more healthily and gradually rebuild emotional resilience.
Silent Deficiency, Rising Risk: Why Protein May Be The Missing Link In Diabetes Care

Credit: Canva
On most clinic days, I meet patients who are doing what they believe is “everything right” for their diabetes—avoiding sweets, switching to brown rice, walking regularly. Yet their blood sugar remains stubbornly high, and complications quietly advance. When we look closer, the problem is often not just what they are cutting out, but what they are missing.
This is where the story changes. In the larger conversation on diabetes, protein rarely takes center stage. But it should.
India’s Diabetes Burden: Looking Beyond Sugar
India continues to carry one of the world’s largest burdens of Type 2 diabetes. Urban lifestyles, reduced physical activity, and easy access to refined carbohydrates have all played their role. Public messaging has, understandably, focused on reducing sugar intake.
But diets are not built on sugar alone. In countless Indian homes, especially those of vegetarians and people with limited means, the bulk of the diet revolves around cereals. Rice, wheat, or millets dominate the plate.
Protein, on the other hand, tends to be an afterthought. This creates a subtle but important imbalance: a high intake of carbohydrates coupled with insufficient protein. It's a problem that seldom gets much attention, yet it has a profound impact on metabolic health.
Understanding the Real Culprit: Insulin Spikes
To grasp the significance, let's break down the post-meal process. Eating foods high in carbohydrates, particularly those that are refined, causes a swift influx of glucose into the bloodstream. The body's response is to release insulin, a hormone that facilitates the transport of glucose into cells. While occasional spikes are perfectly normal, frequent and repeated ones put a strain on the system.
As the years pass, our cells start to ignore insulin's signals. This phenomenon, insulin resistance, is the primary problem in Type 2 diabetes. In response, the pancreas kicks into overdrive, cranking out extra insulin to try to keep up. However, this increased demand takes its toll. This slow decline in pancreatic function is what fuels the disease's advancement and opens the door to further health issues.
Also read: Diabetes Diet Plan: South Indian Breads That Are Better Than Roti
Protein: The Quiet Regulator
Now, where does protein fit into this? Protein does not cause sharp rises in blood sugar. In fact, when included in meals, it acts as a natural regulator. It slows down how quickly the stomach empties, meaning glucose enters the bloodstream more gradually. It also promotes a sense of fullness, reducing the tendency to overeat.
More importantly, protein helps maintain muscle mass—and muscle is one of the body’s largest sites for glucose utilization. Simply put, healthier muscles mean better sugar control.
A meal that includes adequate protein alongside carbohydrates behaves very differently from one that is carb-heavy and protein-poor.
The Invisible Problem: Hidden Protein Deficiency
Protein deficiency is not always obvious. Many individuals appear well-fed, even overweight, yet lack adequate protein at a cellular level. This is often referred to as “hidden malnutrition.”
In people living with diabetes, this becomes particularly concerning.
Low protein intake contributes to gradual muscle loss, especially with ageing. This loss—known as sarcopenia—reduces metabolic efficiency and worsens insulin resistance. Recovery from illness slows down. Wound healing becomes less effective. The body, in a sense, loses its resilience.
Also read: Shift to Plant-Based Proteins, Low-Fat Dairy To Boost Heart Health: American Heart Association
When Deficiency Meets Disease: A Compounding Risk
Diabetes is not just about blood sugar numbers; it is about long-term impact.
When protein intake is inadequate, the risks multiply. Nerve damage becomes more likely. Kidney health may deteriorate faster. Physical strength declines, increasing frailty and reducing quality of life.
There is also a vicious cycle at play. Reduced muscle mass leads to poorer glucose control, which in turn accelerates further muscle breakdown. Breaking this cycle requires more than medication—it requires nutritional correction.
Also read: 1 In 4 Diabetic Patients in India Suffer from Liver Fibrosis, Finds Lancet Study
How Much Protein Do We Really Need?
For most healthy adults, daily protein needs are modest but essential—roughly 0.8 grams per kilogram of body weight.
In individuals with diabetes, requirements are often slightly higher, around 1.0 to 1.2 grams per kilogram per day. However, this must always be individualized, especially in those with kidney disease or other medical conditions.
The key message is not excess, but adequacy—and consistency.
Making It Practical: The Indian Plate Reimagined
The good news is that improving protein intake does not require expensive supplements or drastic dietary changes.
For vegetarians, traditional foods offer excellent options: dals, chickpeas, kidney beans, paneer, curd, soy products, nuts, and seeds. For those who consume non-vegetarian foods, eggs, fish, and lean meats provide high-quality protein.
The simplest strategy is also the most effective: ensure that every meal contains a meaningful source of protein.
A bowl of dal with lunch, a serving of curd with dinner, or an egg at breakfast—these small additions can create a measurable difference over time.
Also read: What Is The Viral ‘Boy Kibble’ Trend?
Beyond Diet: Completing the Picture
Nutrition does not work in isolation. Regular physical activity—particularly resistance exercises—helps preserve and build muscle mass, enhancing insulin sensitivity. Adequate sleep supports hormonal balance. Stress management prevents metabolic disruptions that worsen glycemic control.
Diabetes care is not a single intervention; it is a continuum of daily choices.
Conclusion: Rethinking What We Prioritize
For too long, diabetes management has been framed as a battle against sugar alone. While reducing excess carbohydrates remains important, it is only half the story.
The other half lies in restoring balance. Addressing the protein gap offers a simple, accessible, and powerful tool to stabilize blood sugar, protect muscle health, and reduce long-term complications.
Protein is not just another nutrient on the plate. In the context of diabetes, it is part of the treatment itself.
© 2024 Bennett, Coleman & Company Limited

