- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Can You Safely Stop Blood Pressure Medication After Your Numbers Improve?
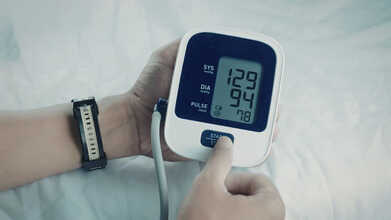
Credits: Canva
High blood pressure is a serious health issue, but it usually causes no obvious symptoms until significant harm has already occurred. This makes it difficult for many patients to stay consistent with their medication. When you do not feel any immediate change after missing a pill, it becomes easier to forget doses or stop altogether.
Many people assume it is “not a big deal” to skip a dose now and then, or even to quit the medicine completely. In reality, blood pressure medication is often meant to be taken long term, sometimes for life, though certain medicines may need to be stopped or switched during pregnancy. In some cases, people may be able to gradually reduce or fully stop their medication if major lifestyle changes lead to a clear and lasting drop in blood pressure.
How Does Blood Pressure Medicines Work?
Blood pressure medicines, also called antihypertensives, lower high blood pressure in different ways. They may relax blood vessels, lessen how hard the heart has to work, or reduce the amount of fluid in the body. These effects help lower the risk of serious problems such as heart attacks and strokes.
According to Medline Plus, these drugs work by blocking hormones that tighten blood vessels, helping the kidneys flush out excess salt and water, slowing the heart rate, or stopping calcium from tightening the arteries, which allows blood to move more freely.
What Happens When You Stop Taking Blood Pressure Medications?
If you miss a dose, it is usually best to take it as soon as you remember, unless it is close to the time for your next dose. Skipping one dose is generally less risky than taking too much. To avoid forgetting, it helps to take your medication at the same time every day and link it to a daily habit. For example, morning pills can be taken with breakfast, while evening pills can be kept near your toothbrush.
Along with choosing a regular time, your doctor may also suggest a specific time of day. One large study found that taking blood pressure medicine at bedtime significantly lowered the risk of heart attack.
Is It Safe To Stop Your Blood Pressure Medicine If Your Numbers Improve
According to Health Central, it is understandable to think about stopping your medication once your blood pressure readings improve and you feel well. However, you should never stop taking these medicines, especially all at once, without speaking to your doctor first.
Stopping blood pressure medication suddenly can lead to withdrawal effects that vary in severity, including:
- Blurry vision
- Chest pain
- Fatigue
- Headaches
- Irregular heartbeat
- Lightheadedness
- Rebound hypertension
- Rebound water retention
- Shortness of breath
When high blood pressure is no longer treated, your readings may return to previous levels or rise very quickly and dangerously, leading to what doctors call a hypertensive crisis. This is defined as a blood pressure reading above 180/120. It is a medical emergency and raises the risk of:
- Blindness
- Heart attack
- Heart failure
- Kidney damage
- Stroke
The harm caused by a hypertensive crisis is not always reversible and can sometimes be life-threatening.
When Can You Stop Taking Blood Pressure Medicine?
If you and your doctor decide that trying life without blood pressure medication is possible and something you want to explore, the safest approach is tapering. This means slowly reducing the dose over time rather than stopping suddenly.
Before doing this, you will need to regularly monitor your blood pressure at home while still on medication and share those readings with your doctor. If your numbers stay consistently at the lower end of the normal range while on treatment, such as around 115/80 mmHg or lower, your doctor may consider gradually reducing your dependence on medication.
Disclaimer: This information is meant for general awareness only and should not be treated as medical advice. Blood pressure medications affect each person differently, and stopping or changing your dose without proper medical guidance can be dangerous. Always speak to a qualified doctor or healthcare provider before starting, adjusting, or discontinuing any medication.
AI-powered Screening Tool To Boost Glaucoma care: The Lancet

Credit: Canva
An international team of researchers has developed an artificial intelligence (AI)-based tool that can significantly improve care for glaucoma -- a leading cause of irreversible blindness worldwide, according to a study published in The Lancet Primary Care journal today.
Researchers led by those from the University of Lisbon in Portugal found that the AI-based screening tool halved the number of unnecessary referrals for glaucoma.
The study, released during the Glaucoma Awareness Week, also showed an accuracy level at par with human eye doctors.
"The high accuracy at excluding people without glaucoma is especially important, as false alarms can lead to unnecessary hospital visits, patient anxiety, and added strain on healthcare services," the researchers said.
According to the researchers, AI-based screening could:
- support earlier detection,
- reduce unnecessary specialist referrals,
- prevent avoidable vision loss,
- can be integrated into routine primary care in a cost-effective way
Key Findings
The study was carried out at a single screening center in Lisbon, Portugal, in 2023.
The experts screened 671 adults aged 55-65 for glaucoma via the AI tool, analyzing images of the eyes. The images were then independently graded by six glaucoma experts.
The AI-tool:
- referred 66 people (9.8 percent) vs 118 referrals (18.0 percent) by the eye doctors,
- diagnosed glaucoma in 40 participants (6.4 percent).
- It correctly identified 78 percent of people who truly had glaucoma, vs 75 percent identified by the eye doctors
- Correctly ruled out the disease in 95 percent of people, vs 91 percent by eye doctors
While modelling studies suggest that screening could substantially reduce glaucoma-related visual impairment and blindness, barriers include the need for specialised diagnostic equipment and trained personnel, particularly in low- and middle-income countries, and the intrinsically low positive predictive value of screening tests.
In such a scenario, the new study showed that "AI may provide a more viable option than population-wide screening", which may seem impractical.
What Is Glaucoma?
Glaucoma is a chronic disease that affects an estimated 80 million individuals globally, according to the World Glaucoma Association.
It is a progressive, degenerative disorder of the optic nerve that produces characteristic visual field damage.
The disease stems from a long asymptomatic phase, resulting in substantial underdiagnosis and delayed treatment.
Even in high-income countries, up to 50 percent of individuals with glaucoma remain undiagnosed, frequently presenting moderate to advanced disease at first detection.
By the year 2040, it is estimated that there will be 22 million individuals worldwide who are blind from glaucoma.
When to see a doctor for glaucoma:
- Vision suddenly gets blurry
- Severe eye pain
- Headache
- Nausea
- Vomiting
- Rainbow-colored rings or halos around lights
Sleep Loss In Early Life May Increase Autism Risk, Researchers Say

Credits: Canva
In adults, long periods of sleep deprivation has been linked to problems such as weakened immunity, weight gain, depression, and an increased risk of dementia. However, scientists are now paying closer attention to how sleep affects the brain much earlier in life.
However, a new University of North Carolina School of Medicine study suggests that disrupted sleep during early childhood may interfere with key stages of brain development and asl well as increase the risk of developing autism.
Why Sleep Matters For The Developing Brain
From the moment babies are born, their brains are rapidly developing. During this stage, neurons form connections with one another through structures called synapses. These connections allow brain cells to communicate and are essential for learning, attention, working memory, and long term memory.Sleep plays a crucial role in helping these synapses form and strengthen. During sleep, the brain organizes and stabilizes these neural connections, shaping the foundation for future brain function. If sleep is repeatedly disrupted during this delicate stage of development, the process may be affected.
Frequent waking or sleep disturbances could interfere with how these neural connections are formed, potentially influencing behavior and cognitive abilities later in life.
The Link Between Sleep And Autism
Sean Gay, a graduate student in the laboratory of Graham Diering, PhD, assistant professor in the Department of Cell Biology and Physiology at the UNC School of Medicine and lead author said that more research was needed to determine the exact link between sleep and the development of autism.“The unique effects of sleep loss during development are largely unexplored,” Diering said. “Our data show that babies and children are more vulnerable to the negative effects of sleep disruption. We also found that sleep loss during this crucial period of time can negatively interact with underlying genetic risk for autism spectrum disorder.”
Sleep problems are already known to be common in people with autism. In fact, sleep disruption has been reported in more than 80 percent of individuals with autism spectrum disorder. However, researchers have long debated whether these sleep issues are a cause of the disorder or a consequence of it. Understanding how sleep interacts with brain development could help scientists detect autism earlier and potentially develop new treatment strategies.
Studying Sleep Disruption In Early Life
In earlier work conducted in 2022, researchers examined how sleep disruption during early life might interact with genetic factors linked to autism. Using mouse models, they disrupted sleep during the third week of life, a developmental stage roughly comparable to ages one to two in humans.
The study found that sleep disruption during this period produced long lasting behavioral changes. Male mice that were genetically vulnerable to autism showed deficits in social behavior later in life. These results suggested that sleep disruption during critical stages of development may interact with genetic risk factors in ways that shape long term behavior.
Younger Brains Respond Differently To Sleep Loss
To investigate further, researchers studied how developing and adult mice respond differently to sleep deprivation.
Using specially designed housing systems equipped with sensitive sensors, scientists tracked the animals’ breathing and movement. This allowed them to determine when the mice were awake and when they were asleep.
The researchers observed that adult mice were able to compensate for lost sleep. After experiencing sleep deprivation, the adults increased their sleep later during their normal active period. This process, known as sleep rebound, allowed them to recover some of the lost rest.
Younger mice behaved very differently. They showed no sleep rebound at all, meaning they did not compensate for the sleep they had lost. This finding suggests that younger brains may be far more vulnerable to the effects of sleep disruption.
The consequences were also visible in cognitive performance. Sleep deprived young mice performed poorly on learning and memory tasks, while adult mice were significantly more resilient after losing sleep.
Changes At The Level Of Brain Synapses
The researchers also examined what was happening inside the brain at the molecular level. Synapses are the points where neurons communicate, and they play a central role in memory formation and learning. Because sleep is closely linked to how synapses function, the team analyzed how sleep deprivation affects these structures. Using advanced protein analysis techniques, researchers mapped changes in the proteins that regulate synapses.The results showed that sleep deprivation in young mice significantly altered the formation of synapses. These changes were not seen in adult mice. “This now provides one of the largest and most comprehensive datasets to examine the molecular effects of sleep loss across the lifespan,” Diering said.
Potential Future Treatments
The research team hopes their findings may eventually help guide the development of new treatments for autism and other neurodevelopmental conditions. One goal is to create sleep based therapies for children that work differently from traditional sleep medications. Instead of acting as sedatives, these treatments would target the biological mechanisms that regulate synapses and sleep function.“Development is not something that one can go back and do again,” Diering said. “Sleep is important for the entire life and especially during development. Understanding what we know now will place greater emphasis on understanding sleep issues in ASD and could lead to an important therapeutic avenue to treat ASD and other developmental conditions.”
The findings highlight an important message for parents and caregivers. During early childhood, healthy sleep patterns may play a critical role in shaping the brain for years to come.
Recreational Drugs Increase Brain Stroke Risk In Young Adults, Study Finds

Credits: Canva
Using amphetamines, cocaine and cannabis can significantly increase your risk of having a brain stroke particularly among younger adults, according to a new University of Cambridge analysis
The findings highlight how recreational drug use may contribute to a preventable health risk, especially among people under the age of 55.
Megan Ritson, a stroke genetics researcher at the University of Cambridge and lead author said the results provide strong evidence linking certain drugs to stroke risk.
“These findings provide compelling evidence that drugs like cocaine, amphetamines, and cannabis are causal risk factors for stroke,” Ritson noted.
A stroke occurs when blood flow to part of the brain is interrupted. This can happen when a blood vessel becomes blocked by a clot, known as an ischemic stroke, or when a blood vessel bursts and causes bleeding in the brain, known as a hemorrhagic stroke. Both types can lead to serious brain damage and can be life threatening.
Amphetamines Associated With The Highest Risk
Among the substances examined, amphetamines were linked to the largest increase in stroke risk. Amphetamines are powerful stimulants that affect the central nervous system and can significantly increase heart rate and blood pressure. In illegal forms, they are often sold under street names such as meth or ice.When researchers combined data from eight previous studies, they found that recreational amphetamine use was associated with more than double the risk of stroke across all adult age groups. For individuals under the age of 55, the increase was even greater. In this group, amphetamine use was linked to nearly triple the risk of stroke compared with people who do not use the drug.
Across all age groups, the analysis found that amphetamine use increased the risk of ischemic stroke by 137 percent and hemorrhagic stroke by 183 percent. These figures reflect relative risk, meaning the probability of stroke is higher among users compared with non users.
Cocaine Shows A Similar Pattern
The researchers also found a strong association between cocaine use and stroke. Cocaine is another central nervous system stimulant that can raise blood pressure and constrict blood vessels. These effects may increase strain on the brain’s blood vessels and raise the likelihood of both clot formation and vessel rupture.The analysis showed that cocaine use nearly doubled the risk of stroke of any kind and more than doubled the risk of hemorrhagic stroke. Additional genetic investigations were conducted alongside the main analysis to better understand whether the relationship might be causal rather than simply linked to other lifestyle factors.
Eric Harshfield, a genetic epidemiologist at the University of Cambridge, said the findings suggest the drugs themselves may play a direct role. “Our analysis suggests that it is these drugs themselves that increase the risk of stroke, not just other lifestyle factors among users,” Harshfield said.
Cannabis Linked To Smaller But Significant Risk
Compared with amphetamines and cocaine, the association between cannabis use and stroke was smaller but still statistically significant. Researchers reviewed 19 previous studies investigating cannabis use and stroke outcomes. The analysis found that recreational cannabis use was associated with a 16 percent increase in the risk of any stroke and a 39 percent increase in the risk of ischemic stroke.Among people under the age of 55, cannabis use was linked to a 14 percent increase in stroke risk. Although the increase is lower than that associated with stimulant drugs, researchers say it remains important because cannabis is widely used.
Opioids Showed No Clear Association
The analysis did not find evidence linking opioid use to an increased risk of stroke. However, researchers caution that stroke risk can be influenced by many factors. These include how long a person has used a drug, how much they use, their overall health, diet, genetics, and socioeconomic environment. Heavy alcohol use is also known to increase the risk of stroke and may worsen the effects of other substances.A Preventable Health Risk
Experts say the findings highlight the need for greater awareness about how recreational drugs can affect long term health, particularly among younger people who may not associate stroke with their age group. “Illicit drug use is a preventable stroke risk,” Ritson explained. “I don’t know if young people are aware how high the risk is.”The researchers also note that many of the studies included in the analysis relied on participants reporting their own drug use. Because of this, other lifestyle factors could potentially influence the results. Further research will be needed to better understand the biological mechanisms involved and how different patterns of drug use may affect stroke risk. Still, scientists say the evidence now available provides an important foundation for future public health strategies.
“These findings give us stronger evidence to guide future research and public health strategies,” Ritson said.
© 2024 Bennett, Coleman & Company Limited

