- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Medical Memoir: Comeback Of Victorian Era Diseases – Why Are We Seeing A Rise In Long-Forgotten Diseases
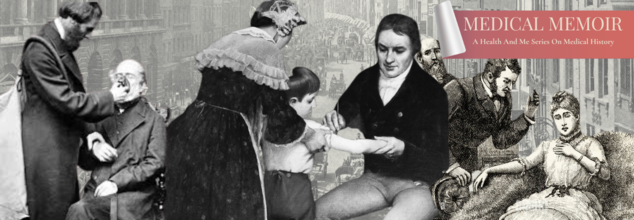
(Credit-Alamy, Victorian Era, BBC History Magazine)
Over the past few years, headlines have raised alarm bells, “Victorian diseases are making a comeback.” Measles outbreaks, scarlet fever warnings, cases of tuberculosis cropping up in urban centers all evoke a troubling echo of a time most of us believed we’d left behind but is the return of these so-called “Victorian” diseases truly a resurgence or have they simply never left us?
Many of these illnesses never disappeared entirely. Diseases like TB, measles, typhoid, and scarlet fever were dramatically reduced in prevalence due to clean water, public sanitation, improved nutrition, antibiotics, and widespread vaccination programs—but they weren’t eradicated.
In fact, public health officials have long acknowledged that these infections have remained in the background, controlled but not conquered. It is only through the combined strength of science-driven public health policy, social infrastructure, and community awareness that we’ve been able to keep them from becoming the epidemics they once were.
Vaccine hesitancy, global travel, growing antibiotic resistance, poverty, urban overcrowding, and weakened health systems in the wake of COVID-19. Measles outbreaks, for example, have surged in communities where childhood immunization rates have dropped. Tuberculosis, often associated with 19th-century slums, remains a global health threat, especially among vulnerable and marginalized populations.
Lastly, climate change and increased human-animal interaction have sort off reshaped the infectious disease landscape, allowing tick-borne and vector-borne illnesses once considered rare to move into new regions and populations.
Diseases That Have Recently Become More Prevalent
Here is a list of diseases and what you need to know about them according to the UK Health Security Agency health blog.
Typhoid
Typhoid was extremely common in the Victorian era, even affecting royalty, and it remains a problem in areas with poor sanitation globally. Caused by bacteria spread through contaminated food or water, it's estimated that 1 in 5 people with untreated typhoid worldwide die. In the UK, improved access to clean water, wholesome food, and good hygiene have drastically reduced its spread, with around 500 cases reported annually, mostly linked to international travel. It's now rarely fatal in the UK, often preventable by vaccine for travelers, and treatable with antibiotics.
Scarlet Fever
In 2018, England and Wales saw over 30,000 cases of scarlet fever, the highest since 1960, though numbers had declined significantly over the previous century due to better living conditions and antibiotics. This highly contagious childhood illness is usually mild and easily treated with antibiotics, which also reduces the risk of complications and spread. While a 1914 epidemic recorded 165,000 cases and 2,800 deaths, in 2014, fewer than 5% of patients were hospitalized, with no deaths, highlighting its much less severe consequences today. Investigations into recent case increases are ongoing.
Tuberculosis (TB)
At the start of the 19th century, TB killed at least 1 in seven people in England. Improvements like milk pasteurization (which significantly reduced TB from contaminated milk) combined with faster diagnoses and effective antibiotics became central to TB control. Today, less than 6% of those with TB in the UK die from it, with fewer than 4,672 cases reported in 2018—the lowest numbers ever. This decline is a major public health success. However, TB remains the top infectious killer globally, especially in poorer communities, emphasizing the need for continued efforts.
Cholera
Cholera, a severe diarrheal illness, can cause fatal dehydration within hours. England's last major outbreaks between 1832 and 1866 resulted in thousands of deaths. It is now very rare in the UK, with cases typically linked to international travel. A key public health breakthrough in the Victorian era was identifying cholera as waterborne, leading to major projects that provided clean water and sewage systems. While still a global concern with ongoing outbreaks in other parts of the world, cholera is easily avoided when traveling by using boiled or bottled water and practicing good hand hygiene.
Whooping Cough
Before routine immunization in the 1950s, whooping cough affected tens of thousands. Vaccination drastically reduced cases, though the infection hasn't disappeared and can peak every 3-4 years. Despite vaccine success, nearly 10,000 cases were confirmed in 2012, with increases also seen in other countries. These rises may be due to factors like better testing and changes in vaccine type. A vaccine program for pregnant women, introduced in response to the 2012 outbreak, has been highly effective in protecting babies until they receive their own vaccinations, making it crucial for expectant mothers to get vaccinated.
Rickets
Rickets, a deficiency disease caused by a lack of calcium or vitamin D, was widespread in poorer areas of Great Britain during the Victorian era. It wasn't until the early 1900s that researchers understood the critical role of sunlight and vitamin D in bone development. While most people get enough vitamin D from sunshine and diet in warmer months, supplements are recommended during autumn and winter, especially for those with limited sun exposure, darker skin, or for babies.
Why Are Some Age-Old Diseases Making A Comeback?
According to 2021 study published in the Lancet journal, few of the many reasons why diseases are reappearing is because sometimes, Sometimes, the germs themselves change, becoming easier to spread or more harmful. For instance, scarlet fever, once thought almost gone, has seen a global rise, including a mysterious spike in England. This might be because the bacteria causing it picked up new genes from viruses, creating "supercharged" versions that spread more easily. Also, germs are becoming more resistant to antibiotics, which means treatments that used to work are no longer as effective, allowing some diseases to re-emerge.
Is COVID-19 A Catalyst?
The study points out that human behavior is a major factor. More people living in crowded conditions and moving around (like through migration) can create new opportunities for diseases to spread. When public health systems and vaccination efforts break down, often due to conflicts, wars, or even global pandemics like COVID-19, diseases like measles can surge.
Changes to the environment caused by human activity can also upset the balance between people, animals, and germs, allowing old diseases to reappear or new ones to emerge. For example, some research suggests that climate change forced bats to move, potentially leading to new interactions between bats and viruses, and even affecting how viruses evolve and spread to other animals, like the virus that causes COVID-19.
The studies and historical significance of these diseases show that these diseases never really left. The only differences is that, now these diseases are not as fatal. These illnesses are largely preventable through good hygiene, vaccination, or proper nutrition. It remains crucial for scientists and healthcare professionals to continue investigating, managing, and informing the public about preventing diseases that could seriously affect health and well-being.
Rather than calling it a ‘comeback’, experts argue we’re witnessing a failure in vigilance. These diseases were never gone; they were simply held at bay and prevented and with weakened health safeguards or lapses in vaccination, they are ready to exploit the cracks.
Energy Drinks Are Not A Substitute For Water In Summer, Doctors Say

Credits: Canva
Water remains the most reliable and effective way to keep the body hydrated during hot weather. However, many people increasingly turn to energy drinks during long workdays or busy schedules, hoping to stay refreshed or energized.
Experts warn that relying on these drinks instead of water can create several health risks, particularly when temperatures are high.
Energy drinks are typically marketed as quick solutions for fatigue and low energy. They often contain high levels of caffeine, added sugars and stimulants that may temporarily increase alertness.
While this short term boost may seem appealing, experts say these drinks are not designed to support proper hydration. When consumed frequently, especially during summer, they can place extra strain on the body rather than helping it stay cool and hydrated.
Dr Arun Sachdeva, an Internal Medicine Specialist at Felix Healthcare in Bengaluru, explains that replacing water with energy drinks during hot weather can interfere with the body’s natural hydration balance.
According to him, excessive consumption of these beverages may contribute to both immediate and long term health concerns, particularly when the body is already losing fluids through sweating.
Higher Risk Of Dehydration
One of the main concerns with energy drinks is their caffeine content. Caffeine acts as a mild diuretic, which means it can increase urine production and lead to faster fluid loss from the body.During summer, when sweating already causes significant water loss, this effect may make it harder for the body to maintain proper hydration.
When energy drinks replace water intake, the risk of dehydration increases. Common symptoms of dehydration include fatigue, dizziness, headaches and dry mouth. In more severe cases, dehydration can also affect concentration, physical performance and overall wellbeing.
Excessive Stress On The Heart
Another concern is the combination of caffeine and other stimulants commonly found in energy drinks. These ingredients can raise heart rate and increase blood pressure. Regular consumption, especially in hot weather, may place additional strain on the cardiovascular system.For people who already have high blood pressure or existing heart conditions, excessive intake of energy drinks could increase the risk of heart palpitations or irregular heart rhythms. Experts therefore recommend limiting the consumption of these beverages, particularly during periods of intense heat.
High Sugar And Empty Calories
Many energy drinks available in the market contain large amounts of added sugar. Drinking them regularly instead of water can significantly increase daily calorie intake without providing meaningful nutritional value.Frequent spikes in blood sugar levels may gradually increase the risk of metabolic disorders. Over time, consistently high sugar consumption can contribute to health problems such as obesity and type 2 diabetes.
Therefore, doctors advise paying attention to sugar content in beverages, especially during hot weather when people tend to drink more fluids throughout the day.
Sleep Disruption And Energy Crashes
Although energy drinks are commonly used to combat tiredness, their high caffeine content can disrupt normal sleep cycles if consumed frequently. Poor sleep can lead to persistent fatigue, irritability and reduced concentration.Instead of providing sustained energy, regular consumption of energy drinks may lead to temporary stimulation followed by sudden drops in energy levels.
This cycle can leave individuals feeling even more tired later in the day, creating a pattern where they rely on more caffeinated drinks to stay alert.
Kidney Health And Hydration
Proper hydration plays an important role in maintaining kidney health. Water helps the kidneys filter waste products and maintain fluid balance within the body. Energy drinks do not provide the same hydration benefits when they replace water intake.When the body does not receive enough water, the kidneys may struggle to function efficiently. Over time, poor hydration can increase the risk of kidney related problems and may affect the body’s ability to regulate fluid levels effectively.
Why Water Remains The Best Choice
Doctors emphasize that water remains the safest and most effective drink for maintaining hydration during summer. It helps regulate body temperature, supports organ function and replaces fluids lost through sweating without introducing excess caffeine, sugar or stimulants.
Energy drinks may occasionally provide a quick boost of alertness, but they should not be used as a substitute for water. Maintaining regular water intake throughout the day remains one of the simplest and most effective ways to support overall health during hot weather.
Your Work Life Habits Can Affect Kidney Health, Doctors Say
Credits: Canva
Late nights at the office, quick dinners made from instant noodles or packaged snacks and constant deadline pressure are often treated as normal parts of professional life, but doctors say these habits may gradually affect kidney health.
Nephrologists report that routine health screenings are increasingly detecting early signs of kidney stress in people in their late 20s to 30s, even among those without traditional risk factors such as diabetes, smoking or a family history of kidney disease.
According to nephrologist Dr Kristin George, some patients show warning indicators such as elevated creatinine levels, high blood pressure or traces of protein in the urine.
Creatinine is a waste product filtered out by the kidneys and rising levels may indicate that the organs are not removing waste as efficiently as they should.
Doctors say that when lifestyle patterns are examined more closely, prolonged work stress, sedentary routines, irregular meals and frequent late-night snacking often emerge as common factors.
Kidney Disease Is A Growing Global Concern
Kidney disease is already recognized as a major global health challenge. Recent research estimates that nearly 850 million people worldwide are living with some form of kidney disease.Chronic kidney disease, or CKD, involves the gradual loss of kidney function over time and can eventually lead to kidney failure if it is not detected early.
Health experts warn that CKD could become one of the leading causes of death globally in the coming decades. Diabetes and hypertension account for a large proportion of cases and according to the International Society of Nephrology these two conditions combined contribute to nearly two-thirds of chronic kidney disease cases worldwide.
Doctors also note that prolonged stress may indirectly increase these risks because long-term elevations in stress hormones such as cortisol can raise blood pressure and disrupt metabolic balance.
Processed Foods And Late-Night Eating
Dietary habits may also contribute to kidney strain, particularly when busy schedules encourage reliance on convenient foods that are often high in sodium and low in nutritional value.Late-night meals frequently include instant noodles, chips, processed meats or packaged snacks, many of which contain significant amounts of sodium.
Sodium helps regulate fluid balance, but excessive intake forces the kidneys to work harder to maintain stable blood pressure. The World Health Organization estimates that most adults consume nearly twice the recommended daily sodium intake, largely because of processed foods.
Doctors say that consistently high salt intake can gradually increase blood pressure and place additional strain on kidney function.
Sedentary Work And Poor Hydration
Hydration habits and prolonged sitting are additional concerns among office workers. Many professionals rely heavily on coffee, energy drinks or sugary beverages during long workdays, often replacing plain water as the main source of fluid intake.
While moderate caffeine consumption is generally considered safe, relying mainly on caffeinated drinks can contribute to mild dehydration, which may affect blood circulation through the kidneys and increase the likelihood of kidney stones.
At the same time, many corporate jobs require employees to remain seated for extended periods. Sedentary routines have been linked to obesity, impaired glucose metabolism and high blood pressure, all of which are major contributors to kidney disease.
Early Signs Often Go Unnoticed
Kidney disease often develops silently in its early stages, which means many people remain unaware of the problem until significant damage has occurred.
Early kidney dysfunction may progress quietly for years before symptoms appear, and by the time signs such as swelling, fatigue or changes in urination become noticeable, kidney function may already be reduced.
Doctors therefore recommend periodic screening tests, including serum creatinine measurements, estimated glomerular filtration rate (eGFR) tests and urine albumin tests, which can detect early signs of kidney damage.
Small Changes Can Make A Difference
Health experts say that protecting kidney health often begins with small lifestyle changes. Reducing processed food consumption, limiting excessive salt intake, staying adequately hydrated and maintaining regular sleep schedules can all support kidney function.
Taking short movement breaks during long work hours and managing stress through regular physical activity or relaxation techniques may also help reduce the long-term strain that modern work routines place on the body.
Doctors emphasise that kidney disease usually develops gradually, which means recognising and adjusting everyday habits early may help many young professionals protect their kidney health.
AHA Cholesterol Guidelines 2026: How Indians Can Improve Heart Health

Credit: Canva
Heart disease remains the leading cause of death in India, often affecting people nearly a decade earlier than in Western populations.
Recent cholesterol management recommendations from the American Heart Association (AHA) and related global guidelines emphasize aggressive control of LDL cholesterol — the so-called “bad cholesterol.” For Indians, these recommendations carry particular importance.
Studies consistently show that South Asians have a higher tendency for premature coronary artery disease. Even individuals who appear relatively lean may have underlying metabolic risk factors such as insulin resistance, abdominal obesity, and elevated triglycerides. Because of this inherent susceptibility, the same cholesterol levels that may appear “borderline” in Western populations can translate into a significantly higher cardiovascular risk in Indians.
What Does The New Guidelines Say
The newer guidelines shift the focus away from merely treating cholesterol numbers to assessing an individual’s overall cardiovascular risk.
Factors such as diabetes, smoking, blood pressure, family history of early heart disease, and age are considered together. If a person falls into a higher-risk category, doctors now recommend lowering LDL cholesterol more aggressively than before.
For people who already have established heart disease, the goal is particularly strict. LDL cholesterol is ideally reduced to levels below 55 mg/dL. Achieving such targets often requires not only lifestyle changes but also medications such as statins, and in some cases, newer therapies that further lower cholesterol levels.
How Indians Can Prevent Heart Disease
For Indians without diagnosed heart disease, prevention becomes the key message. Regular screening after the age of 30–35 years is increasingly advisable, especially if there is a family history of heart disease or diabetes. Diet also plays a central role: reducing trans fats, limiting refined carbohydrates, increasing fibre intake, and maintaining a healthy body weight can significantly influence cholesterol levels.
Equally important is regular physical activity. Even 30 minutes of brisk walking most days of the week can improve lipid profiles and reduce cardiovascular risk.
The key takeaway is simple: Indians develop heart disease earlier and often at lower cholesterol levels.
The newer AHA recommendations reinforce the need for earlier screening, individualized risk assessment, and more proactive cholesterol management to prevent future heart attacks.
© 2024 Bennett, Coleman & Company Limited

