- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Is It Hair Fall Or Hair Loss? Here’s How to Tell And When to Seek Professional Help

Credits: iStock
Noticing more strands on your pillow, in the shower drain, or tangled in your brush can feel alarming. But this is the surprise: not all shed hairs are a sign of lasting damage. Occasionally it's just temporary shedding, sometimes it's real hair loss that requires intervention. Knowing and understanding the difference will save you from unnecessary panic and prevent you from acting too late.
Hair loss tends to creep up gradually, leaving individuals confused about what's actually going on. Losing a strand or two is normal in the natural cycle, but when clumps show up in your brush or your scalp begins showing through, it's tempting to freak out. Knowing the distinction between normal shedding and ongoing loss is the starting point for safeguarding your hair health. That's where professional advice can come into play. Dr. Deepak Choudhary, Senior Master Surgeon and Trainer of DHI International, states that the difference is based on both the pattern and the permanence.
"We shed 50 to 100 hairs a day, which is a natural hair cycle. But if you begin to notice clumps of hair falling out, heavy shedding, or unusual thinning, it is referred to as hair loss. Hair loss tends to be patchy with apparent thinning, but hair fall tends to be even all over the scalp," says Dr. Choudhary.
Understanding the difference is important, not only for peace of mind, but also to decide when to consult a professional.
What Is Hair Fall?
Hair will go through three natural cycles, which are anagen (growth), catagen (transitional stage), and telogen (resting stage). The hair falls out at the end of the telogen phase to give way to new growth. This telogen effluvium is what dermatologists refer to as a condition that causes excessive shedding because of a break in this cycle. Physical or emotional stressors usually cause excessive shedding. Some of the stressors include:
- Sudden loss of 20 pounds or more
- Childbirth
- Excessive stress, e.g., illness in the family, divorce, or loss of a job
- Severe fever or serious illness
- Surgery
- Stopping birth control pills
Usually, this shedding happens several months following the precipitating incident. For instance, new moms tend to notice extreme shedding two months after giving birth, and then it tends to peak at four months before tapering off. In the majority of instances, regular fullness resumes between six and nine months as the body gets back into balance.
Yet, if stressors are prolonged, shedding will last longer.
What Is Hair Loss?
Losing hair differs from shedding. Medically referred to as anagen effluvium, it is when something prevents hair from growing in the first place. In contrast to telogen effluvium, where hair will grow back, losing hair tends to need attention. The usual causes of hair loss are:
Genetic hair loss: The most common form, commonly referred to as male or female pattern baldness.
Immune system disorder: Disorders such as alopecia areata, wherein the body mistakenly attacks its own follicles.
Medications and treatments: Chemotherapy and radiation are traditional culprits.
Hairstyles and products: Severe braiding, ponytails, and harsh chemicals can harm follicles.
Trichotillomania: An urge to pull out one's own hair.
In most instances, hair grows back only once the underlying cause has been treated. Some forms of inherited hair loss, for instance, persist untreated and might need long-term measures.
Hair Fall vs Hair Loss: Spotting the Warning Signs Early
A majority of individuals overlook initial signs of abnormal hair loss until the issue becomes evident. However, minor changes can act as red flags:
- Clumps of hair seen upon brushing or showering
- Thinning which is apparent, e.g., reducing ponytail size
- Balding at the crown or receding hairline (particularly in men)
- Patchy bald patches on the head or body
- Textural changes, with brittle or easily breakable hair
- Identifying these changes in time can be a huge improvement in treatment success.
Dr Deepak continues to say that whereas basic hair fall is easily controlled with topical medications, drugs, and proper hair care, genuine hair loss usually calls for more sophisticated interventions.
Why Are Hair Transplants on The Rise?
For chronic or progressive hair loss, minimally invasive transplant procedures are bringing new hope. One such treatment is Direct Hair Implantation (DHI), which takes individual follicles from the safest donor site—the back of the scalp—and plants them on spots where hair has thinned or is bald.
Unlike classical transplant techniques, DHI does not leave scars and offers direct control of angle, depth, and density. This provides natural-looking results that integrate well with the existing hair. Healing is quicker, too, and there's very little discomfort involved.
"Temporary measures can improve the strength of existing hair and reduce shedding, but they won't halt progressive hair loss," explains Dr. Choudhary. "Transplantation, particularly advanced techniques like DHI, delivers a permanent, proven solution for extensive cases.
When to See a Dermatologist?
All hair changes do not need to be treated medically, but if excessive shedding or patches of balding continue, a visit to a dermatologist is a must. Dermatologists are hair, skin, and nail experts and can:
- Diagnose whether the condition is shedding hair or hair loss
- Detect underlying causes, such as hormonal, autoimmune, or drug-related issues
- Prescribe drugs or treatments specific to the condition
- Prescribe or undergo procedures such as PRP (platelet-rich plasma) therapy or transplantation
- The earlier treatment begins, the better the chances of halting progression and restoring growth.
Managing Hair Health at Home
Even if you’re not facing advanced hair loss, healthy habits can support your hair’s natural cycle:
- Eat a balanced diet rich in protein, iron, and omega-3 fatty acids.
- Manage stress with mindfulness, exercise, or therapy.
- Avoid hairstyles that pull on the scalp.
- Use gentle shampoos and conditioners, steering clear of harsh chemicals.
- Shield hair from over-exposure to heat styling and UV rays.
Hair loss and hair shedding can appear on the surface to be similar, but they result from quite different biological mechanisms. Shedding is frequently temporary and self-resolving, whereas genuine hair loss could be due to medical or surgical intervention.
If you’re losing more hair than usual, or noticing thinning patches, don’t wait until it becomes overwhelming. A consultation with a dermatologist can provide clarity and open the door to effective treatments—ranging from medications to advanced transplants like DHI.
Drinking Alcohol To Reduce Stress? Your Liver May Have To Pay The Price

If stress is making you turn to alcohol, over time it may lead to fatty liver. (Photo credit: iStock)
Many people do not realise just how closely mental health and liver health are connected—especially when alcohol becomes a go-to coping strategy for stress, anxiety, or emotional overwhelm. What may seem like temporary relief can quietly evolve into a pattern that affects both the mind and the body in significant ways. Dhara Ghuntla, Psychologist affiliated with Sujay Hospital, 7 Hills Hospital, Criticare Hospital, in an interaction with Health and Me, spoke about the impact of stress, alcohol use and emotional eating on the liver.
In today’s fast-paced, high-pressure lifestyle, it is common for individuals to turn to alcohol to unwind or escape difficult emotions. In the short term, alcohol can create a sense of relaxation or numbness. However, over time, this reliance can shift into a habitual coping mechanism and eventually into dependence. While the psychological impact is often discussed, the physical consequences—particularly on the liver—are just as important.
The liver plays a critical role in detoxifying the body. Regular alcohol consumption places it under constant strain, impairing its ability to function effectively. Over time, this can lead to conditions such as fatty liver, inflammation, and even long-term liver damage. What makes this especially concerning is that early-stage liver issues often present with little to no obvious symptoms, allowing damage to progress unnoticed.
At the same time, liver health has a direct influence on mental well-being. When the liver is compromised, it can affect energy levels, mood regulation, and cognitive function. People may experience increased fatigue, irritability, anxiety, low mood, or emotional instability. This happens because the liver plays an indirect but essential role in brain health through metabolism and toxin clearance.
The Vicious Cycle
This creates a self-perpetuating loop. A person feeling stressed, low, or anxious may turn to alcohol for relief. While it may help temporarily, it simultaneously places stress on the liver. As liver function declines, mental health symptoms—such as fatigue, irritability, anxiety, or low mood—can worsen. This often leads the individual to consume more alcohol, reinforcing the cycle.
Adding another layer, many individuals who rely on alcohol are often dealing with underlying issues such as depression, anxiety, sleep disturbances, or chronic life stressors. Alcohol is frequently used as a form of self-medication. However, instead of addressing these root concerns, it masks them temporarily while deepening both psychological and physical harm. Over time, this pattern increases dependency and makes recovery more complex.
The Gut–Liver–Brain Connection
Liver health is also closely tied to gut function and brain health. When the liver is under stress, digestion can be affected, nutrient absorption may decline, and energy levels can drop. This interconnected system—the gut, liver, and brain—plays a key role in emotional regulation and overall well-being. Disruptions in one area can ripple across the others, influencing how a person thinks, feels, and functions daily.
Breaking the Pattern
Recognising this connection is the first step towards change. Instead of turning to alcohol, healthier coping strategies can help regulate stress and support both mental and physical health. Practices such as yoga, meditation, regular exercise, journalling, and maintaining a balanced diet can significantly improve resilience and emotional stability.
Prioritising mental well-being, addressing underlying psychological concerns, and protecting liver health are not separate goals—they are deeply interconnected. Seeking timely support, whether through therapy, lifestyle changes, or medical guidance, can help break the cycle.
Reducing or eliminating alcohol use is not just about avoiding physical harm; it is about creating space to heal the underlying causes of stress and emotional distress. Supporting the liver, nurturing the gut, and caring for mental health together can lead to more sustainable and meaningful well-being.
Ordinary Movement, Extraordinary Pain: FAQs On Bursitis Answered By Expert
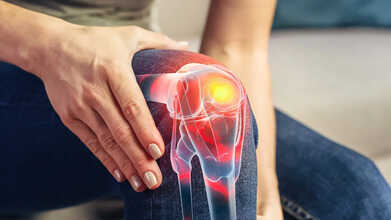
Bursitis is often linked to lifestyle. (Photo credit: iStock)
You pick up a jar on the kitchen shelf and shudder. You take a flight of stairs, and that old pain sinks into your hip. You get up in the morning, and your shoulder feels as though it has been wrung out. You attribute it to age, to a long day on your feet, to just how things are now. But what if your body is trying to tell you something very particular and you have been missing it?
Dr Apoorv Dua, Consultant, Orthopaedics, ISIC Multispeciality Hospital, in an interview with Health and Me, said that this may be a sign of bursitis—a condition that is much more widespread than most people realise, and much more treatable than most people are aware. The expert went on to answer common questions regarding extreme pain that comes with this condition.
What is bursitis?
Bursae are small, fluid-filled sacs located between your bones, muscles, and tendons. Imagine them as the natural cushioning system of the body—shock absorbers that ensure your joints move smoothly and painlessly. Under normal circumstances, you do not even think about them. However, when inflamed, due to repetitive motion, prolonged pressure, injury, or infection, they make their presence known in a very noticeable manner. This is bursitis. Although it most often appears in the shoulder, elbow, hip, and knee, it may occur in nearly any joint in the body.

Who gets bursitis—and why?
This is where the lifestyle connection cannot be overlooked. Bursitis does not discriminate, but it has definite patterns. The weekend warrior who runs ten kilometres on Saturday after sitting at a desk all week. The housewife who spends hours cleaning floors or squatting in the kitchen. The office worker who has been stooped over a computer. The gym enthusiast who does not warm up. The retired teacher who begins a walking routine too vigorously. All these individuals may be silently placing stress on their bursae, and in many cases, bursitis is the eventual outcome.
Age also plays a role—the bursae, like most of our connective tissue, grow weaker with age. Certain medical conditions such as rheumatoid arthritis, gout, and diabetes can increase the risk. However, in many instances, the cause is simply the way we move—or do not move—in our day-to-day lives.
What does bursitis feel like?
A key characteristic of bursitis is pain that is disproportionate to the activity causing it. Reaching overhead, sitting on a hard surface, pressing on your elbow, or walking downhill—these are not dramatic movements, yet with bursitis, they may trigger a sharp, deep, or burning pain that interrupts you mid-action. The affected joint is usually swollen and tender. The area may feel warm to the touch. Movement becomes guarded. Sleep, particularly in cases of shoulder bursitis, can be difficult, as lying on the affected side aggravates the pain.
The challenge with bursitis is that its symptoms can resemble other conditions—tendinitis, arthritis, a muscle strain, or even a ligament tear. Many individuals self-diagnose, self-treat with painkillers, and hope it will go away. Sometimes it does. However, chronic, untreated bursitis may persist for months and, in some cases, lead to complications.

Bursitis diagnosis
A thorough clinical examination is usually the first step. A skilled orthopaedic specialist can identify the affected bursa through specific physical assessments. Imaging, such as ultrasound or MRI, may be recommended depending on the case to confirm the diagnosis, rule out structural damage, or guide treatment.
If infection is suspected—indicated by increased redness, fever, and rapidly worsening pain—fluid may be aspirated from the bursa and tested. Septic bursitis is a serious condition that requires immediate medical attention and is treated differently from the more common non-infectious type.
Bursitis treatment
The encouraging fact about bursitis is that it responds well to treatment, particularly when detected early. Most cases are managed with a combination of rest, activity modification, ice application, and anti-inflammatory medication. Physiotherapy also plays an important role, helping to correct movement patterns, strengthen supporting muscles, and restore the full range of motion.
In more persistent cases, a corticosteroid injection into the bursa may provide rapid and significant relief by reducing inflammation at its source. Surgery is rare and is typically considered only in chronic, recurrent cases that do not respond to conservative treatment.
Prevention is better
In many instances, bursitis is linked to lifestyle—and that presents an opportunity for prevention. Even small changes can help: warming up before exercise, avoiding excessive strain on joints, maintaining a healthy weight to reduce pressure on hips and knees, and ensuring workstations are ergonomically designed.
Pain often becomes background noise—something we get used to, work around, and push through. However, bursitis reminds us that the body communicates with precision. That pain when you pick up a jar, that discomfort on the stairs—it is not simply ageing. It is a signal worth discussing with your doctor.
World Haemophilia Day 2026: Are Frequent Nosebleeds In Kids An Early Sign?

World Haemophilia Day 2026: Haemophilia is a genetic condition that affects the blood's ability to clot. (Photo credit: iStock)
A nosebleed that will not stop or a small cut that continues to bleed far longer than expected—these are some of the most overlooked health problems. While these symptoms are often brushed aside as minor issues, they could be early indicators of an underlying bleeding disorder such as haemophilia. Dr Gaurav Kharya, Senior Consultant and Clinical Lead – Bone Marrow Transplant, Indraprastha Apollo Hospital, Delhi, answered FAQs regarding hemophilia—whether frequent nosebleeds in children are a cause for concern or not.
Understanding haemophilia
Haemophilia is a genetic condition that affects the blood’s ability to clot properly. In its absence, even minor injuries can lead to prolonged or excessive bleeding. Despite advances in treatment, many people remain undiagnosed, often until complications start appearing. This World Haemophilia Day, Dr Kharya highlights a critical gap: most people with haemophilia do not even know they have it.
A global diagnosis gap
The World Federation of Haemophilia estimates that over three-quarters of people with bleeding disorders worldwide remain undiagnosed, leaving hundreds of thousands without access to even basic care. To appreciate the scale of this gap, the expected number of patients with haemophilia globally is 1,125,000, of whom approximately 418,000 should have severe haemophilia. Reported figures fall dramatically short of both estimates.
India’s delayed diagnosis challenge
India’s diagnostic reality is particularly sobering. The median age at diagnosis for severe haemophilia in India stands at 60 months—five full years—compared to under 12 months in high-income countries. This delay is not just a matter of time but one that poses a risk of serious clinical consequences. Late diagnosis often means repeated, unmanaged bleeding episodes during early childhood, particularly into joints, before appropriate treatment begins.
Recognising the warning signs
Recognising the early warning signs can be critical in preventing long-term complications. Symptoms such as recurrent nosebleeds, heavy menstrual bleeding in females, and prolonged bleeding after minor injuries are often overlooked or dismissed. However, these are not just minor inconveniences but potential diagnostic indicators that require timely medical consultation rather than mere dismissal.
Treatment options for haemophilia
The treatments for haemophilia have never been more effective, but they work only for patients who have been diagnosed. In a condition where every missed bleed moves a joint closer to permanent damage, the most important clinical act is also the most basic one: recognition.
© 2024 Bennett, Coleman & Company Limited

