- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Is There A Limit To How Far Female Fertility Can Be Extended?

Credits: Canva
Over the past century, social progress has greatly altered the age at which women opt to have children. Whereas most women in the past gave birth in their early twenties or teens, the trend has since dramatically changed. Women in nations such as the U.S., South Korea, and in Europe are now delaying motherhood to well into their 30s. Indeed, the average age of first-time mothers in most OECD countries now stands at about 30.
But biology has not kept pace with society. Women's fertility is still tied to the natural aging of a woman's reproductive apparatus – something that modern medicine is always trying to get around. With career aspirations, education, and individual choice rewriting the schedules of motherhood, an urgent question presents itself: how far can we push back female fertility?
How Does The Biological Clock Work?
At the very center of female fertility is a game of numbers – one that is decided even before a girl is born. Women are born with a limited number of eggs, usually one million. By the time they reach puberty, this count drops to about 300,000. Of these, only some 300 to 400 will ever develop and get released during ovulation.
By age 37, egg stores decrease to around 25,000, and by age 51 – the average age of menopause in the United States – only 1,000 are left. Yet, ovulation and fertility do not necessarily persist up to menopause. In the majority of women, natural fertility declines sharply 7 to 10 years before, typically by the early 40s.
Though this fall has been around for some time, its raw statistics still stun: natural conception chances fall from about 25% per cycle during a woman's 20s to less than 5% per cycle by her 40s.
What Does the Egg Supply Do at Each Age?
More important than the declining egg quantity is the sharp decline in egg quality with advancing age. Each egg contains chromosomes that make up the DNA map for a new life. When egg quality falls, so does the chance for a successful pregnancy.
By age 30, nearly 25–30% of a woman’s eggs may carry chromosomal abnormalities. By 35, this rises to 40%, and after 40, it spikes dramatically. Studies show that beyond age 40, up to 75% of eggs may have abnormalities. Such eggs are less likely to fertilize, implant, or lead to a healthy baby.
The dangers posed by low quality of eggs are miscarriage, unsuccessful fertility treatment, and chromosomal abnormalities such as Down syndrome.
How Far Can Science Go in Extending Fertility?
With the help of improvements in assisted reproductive technologies (ART), the limits of biological fertility are gradually being extended. Methods like egg freezing (oocyte cryopreservation), in vitro fertilization (IVF), and the employment of donor eggs have helped many women give birth well into their 40s – and, in some instances, even their 50s.
Egg freezing, specifically, has been a game-changer. It enables women to save their younger, healthier eggs to use later in life. It's not a surefire insurance policy, though. Success is dependent on age at the time of freezing, number of eggs saved, and overall health.
Nevertheless, though technology may provide additional time, it will not halt the natural aging of the ovaries or enhance the genetic quality of aging eggs. There is still a biological limit.
Decrease in Male Fertility Level
Men, too, experience a decline in fertility – but it tends to occur more gradually. Starting around age 40 to 45, men see a drop in sperm quality and volume, but they often retain the ability to father children into their 60s and beyond. Unlike women, men continuously produce new sperm, whereas women are working from a non-renewable stockpile of eggs.
This disparity implies that while more and more couples are opting to wait to have children, the responsibility of the "biological clock" remains mostly on women.
Although most of the discussion about female reproductive aging centers on wanting to have children, it is important to note that it also marks more general changes in a woman's health – specifically the onset of menopause and its attendant risks. Perhaps one of the most important but most underappreciated is the increasing significance of regular reproductive screenings, particularly as women get older.
Among these, cervical cancer screening stands out as a powerful tool to protect women’s health beyond their childbearing years.
Pap smears and HPV testing are able to pick up on abnormal cell changes before they develop into cancer. Because the immune system shifts with age and hormonal changes impact cervical health, regular screening is even more important. Women in their 30s and 40s – the same time frame when fertility is actively shifting – need to continue to be vigilant about their yearly OB-GYN checkups.
Actually, while women are thinking of or undergoing fertility treatments or assessing their reproductive future, this is the ideal opportunity to make sure their cervical health is under surveillance. New technologies in at-home HPV testing, liquid-based cytology, and co-testing provide more convenient and precise diagnoses ever before.
So is there a boundary beyond which female fertility can be prolonged? Biologically, yes. Despite incredible scientific strides, the natural aging of eggs and of the ovaries places limits that technology can only stretch so far.
Yet reproductive health is more than fertility. By broadening the story to encompass cervical screenings and preventive care, we give women the ability to take holistic control of their reproductive path – whether they opt to become mothers at 25, 35, or older because prolonging fertility isn't merely about having the capacity to conceive, it's about maintaining a lifetime of reproductive health.
From First Period to Menopause: How Your Cycle Evolves Over the Years | Women's Day Special

Considered to be a key symbol of fertility and reproductive years, a woman's menstrual cycles are an integral and natural part of her life. However, they are more than just a monthly event, but instead a reflection of their hormonal, metabolic and even emotional health.
Due to genetics and other lifestyle factors, every woman experiences their cycle differently, which leaves many second-guessing about their hormonal balance, thyroid function, metabolic health, stress levels and even sleep quality.
Dr Archana Dhawan Bajaj, Gynaecologist and IVF Expert, Nurture exclusively tells Healthandme: "Knowing these patterns would guide people to understand when the changes are normal worry and when they are upheaval of a problem. Although the cycles vary among individuals, some features of such cycles are common between individuals, including the length of the cycle, flow, symptoms, as well as consistency, which are used to determine a normal state at various ages.
Here is what you should know and keep an eye out for during each phase:
The Early Years: Finding a Rhythm
Dr Maya PL Gade, Consultant, Gynaecology & Obstetrics at Kokilaben Hospital tells Healthandme: "In the first 2–3 years after menarche i.e. your first period, irregular cycles are common. Nearly 40–50 percent of adolescents do not ovulate consistently at first. The brain–ovarian hormonal axis is still maturing, so cycles may be longer than 35 days (than their typical 28 day monthly cycle) , bleeding may be heavy and cramps can feel intense.
Dr Rohan Palshetkar, Consultant IVF Specialist, Bloom IVF also warned that bleeding for more than 7–8 days continuously, soaking pads every 1–2 hours or going more than 90 days without a period may signal hormonal imbalance, clotting disorders, or conditions like PCOS.
He told Healthandme: "It is important to note that early teen cycles often happen without ovulation. For teenage girls, developing stable cycle will take some time due to ovaries adjusting to produce hormones. It is only in their late teens and early 20s that the girls will get the cycles more regular."
Normal Menstrual Cycle: According to Dr Bajaj, a normal cycle can be between 21 and 45 days. During bleeding, flow can be light, heavy, and cramps, mood swings, or even fatigue may accompany the adaptation of the organism to the hormonal changes.
Abnormal Menstrual Cycle: The expert explained: "Extensive bleeding, which needs the replacement of sanitary items every hour to two hours, long than seven or eight days, excruciating pain, or lack of periods in several months could be a sign of hormonal imbalance, thyroid complications, or polycystic ovarian syndrome."
20s and Early 30s: The Stable Phase
Talking about the post-teenager phase, Dr Gade said: "For many women, this is when cycles become more predictable, typically every 21–35 days, with 3–7 days of bleeding. Ovulation is more regular and PMS patterns are clearer. However, this is also the stage where lifestyle has a strong impact."
"Fertility is also at its peak in the 20s and early 30s, making it easy for women in this age group to become pregnant. With childbirth and breastfeeding, the chances of cycle alteration, its flow and length are high," Dr Palshetkar added.
Dr Gade also noted that high stress, poor sleep, intense exercise, crash dieting, thyroid disorders, or PCOS can disrupt ovulation and any sudden irregularity in this decade is often the body’s early warning system. A consistently painful period is also not “normal”, it may point to endometriosis or adenomyosis, both of which are frequently underdiagnosed,"
Keeping this in mind, it is essential for girls in their 20s and early 30s to track their period for regularity and flow, Dr Palshetkar advised.
Normal Menstrual Cycle: Dr Bajaj told this publication: "The average period to undergo a cycle is 21 to 35 days at an average of three to seven days with a moderate flow. The symptoms can be mild and include bloating, cramps or breast tenderness that can be easily treated."
Abnormal Menstrual Cycle: Talking about abnormal alterations, the gynaecologist said: "Excessive menstrual bleeding, cramps that impair normal life or inter-menstrual bleeding may be some of the early signs of endometriosis, fibroids, hormonal disruption or chronic stress."
Late 30s to 40s: The Hormonal Transition
Dr Gade explained: "Fertility begins to decline gradually after 35 due to reduced ovarian reserve. Cycles may shorten initially because ovulation happens slightly earlier. As women move into perimenopause, a transition that can last 4–8 years, hormone levels fluctuate unpredictably. Estrogen doesn’t simply drop; it rises and falls unevenly.
"This explains why many women notice heavier bleeding, clotting, worsening PMS, new-onset anxiety, sleep disturbances or cycles that skip months and then return. Studies suggest that up to 90 percent of women experience noticeable cycle changes during this phase.
"Importantly, very heavy bleeding at this stage should not be ignored. It can sometimes be linked to fibroids, endometrial thickening, or other structural changes in the uterus."
Moreover, Dr Palshetkar also warned: "For some, there is a noticeable and increasing gap between periods before menopause. Fertility decline is a reality in the age group, though it is not impossible to get pregnant.
Normal Menstrual Cycle: Dr Bajaj elaborated to Healthandme: "The hormonal shifts at this age may make the cycles a bit shorter or longer. Flow can either become thicker or thinner and premenstrual symptoms can be more pronounced as the body slowly transitions into perimenopause."
Abnormal Menstrual Cycle: Additionally, she said: "Very heavy bleeding, very prolonged intervals between the periods, bleeding following intercourse or sudden spotting between menstruation may be considered an issue, as these can be indicators of hormonal disorders, the presence of fibroids, or other gynecological problems."
Menopause: A New Baseline
Ultimately, Dr Gade detailed: "Menopause is diagnosed after 12 consecutive months without a period, with the average age globally around 50–51 years. Hormone levels stabilize at lower levels, and while periods stop, symptoms like hot flashes, vaginal dryness, bone density changes, and metabolic shifts may appear."
"Post-menopause, a woman’s reproductive health sees a significant decline of estrogen levels, fertility, and inability to produce any eggs. However, it still sees noticeable hormonal fluctuations and resultant health troubles.
"Facing PMS-like symptoms like mood swings and irritability is not uncommon. Medical attention is required when women notice severe pain or very heavy bleeding at
any age after menopause.
"The changes and evolution in the menstrual cycles are proof of her complete health during the course of the life she lives. And it impacts the way she lives or can live through her lifetime," Dr Palshetkar added.
Normal Menstrual Cycle: Lastly, Dr Bajaj said: "Prior to menopause, the cycles can become irregular since of the hormonal fluctuations and some symptoms like hot flushes, sleeping problems or mood swings can appear."
Abnormal Menstrual Cycle: While she noted that slight spotting is possible post-menopause due to fluctuations in estrogen and progesterone levels, the expert advised: "Post-menopausal vaginal bleeding is regarded as abnormal and needs to be medically examined because it may be due to underlying health conditions that must be addressed."
Hailey Bieber Revealed How A Mini Stroke At 25 Led To Her Discovering A Hole In Her Heart

(Credit - SHE MD Podcast/haileybieber/Instagram)
Hailey Bieber recently opened up about a mini stroke or Transient Ischemic Attack (TIA) she experienced when she was just 25. In an episode of the SHE MD podcast, hosted by Mary Alice Haney and Dr. Aliabadi, Hailey discussed how the mini stroke actually led her to find out an even bigger issue in her heart.
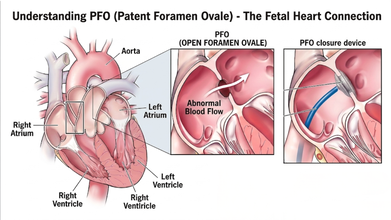
Dr. Aliabadi, a world-renowned OBGYN based in Los Angeles, who is also Hailey’s doctor, explained that this ordeal led Hailey’s medical team to discover a PFO, also known as a hole in her heart
In the interview, the founder of Rhode Beauty detailed how she had the classic stroke symptoms and said: “[My] whole right side of my arm went numb. I couldn't speak. Like my words were coming out all jumbled. The right side of my face was drooping. It was like a classic stroke symptom”
She explained that the reason why her team called it a mini stroke is because it ended within 31 minutes. By the time she reached the hospital, she didn’t need any clot busting medicine or procedure.

What Caused Hailey Bieber’s Mini Stroke?
Dr. Aliabadi explained that Patent Foramen Ovale (PFO) is extremely common phenomenon and a majority of people go through life never knowing they have it.
The Cleveland Clinic explains that the PFO is a small flap or opening between the upper chambers of your heart that everyone has. However, it usually closes up before the age of three. Most of the time, a PFO doesn’t cause symptoms and would not need treatment; however, in rare cases, it could lead to a stroke and or a TIA.
How Was Hailey’s Heart Condition Diagnosed
Hailey explained that her heart is slightly tilted in her chest and standard echocardiogram couldn't see the opening at first which led ER doctors to be unable to detect it.
As a result, she had to see a specialist for a Transcranial Doppler test. Doctors listened to the sound of blood "shunting" (moving the wrong way) through her heart to finally confirm the hole was there, which was much larger than they expected.
Also Read: Women Heart Symptoms Could Differ From Men, Explains Expert
What Is Transcranial Doppler Test?
According to the Cleveland Clinic, it is an ultrasound test that uses sound waves to detect conditions that affect blood flow to and within your brain. It can detect strokes caused by blood clots, narrowed sections of blood vessels, and numerous other heart-related issues.
How Did They Fix Hailey Bieber’s Heart?
Instead of an open-heart surgery, doctors performed a modern, minimally invasive procedure on Hailey's heart. She detailed the procedure where the doctors reached her heart through a vein in her groin. They threaded a tiny "button" made of metal and Teflon up to her heart and used it to securely plug the hole.
Hailey also learned she has some genetic factors that put her at a higher risk for blood clots and inflammation. Despite suffering a life-altering stroke, she views it as a "blessing in disguise" as it led her to find these issues early.
Now, she manages her health through a clean lifestyle, focusing on sleep, exercise and keeping her heart inflammation low.
Reducing Mother-To-Child HIV Transmission To Zero Key To End AIDS In India: Experts
Credit: iStock
Reducing mother-to-child HIV transmission, also called vertical transmission, to zero is crucial to achieve the end AIDS target by 2030 in India, in line with the UN Sustainable Development Goals, said experts.
At the 17th National Conference of the AIDS Society of India (ASICON 2026), health officials and experts together deliberated on the progress made in the country against HIV and also called for a stronger last-mile effort to eliminate AIDS from the country.
While India has made a major reduction in vertical HIV transmission, with just 0.7 percent of infant diagnoses. But the experts stressed the need to further reduce it to zero.
From 25 percent in 2020, the vertical transmission of HIV has come down to 11.75 percent in 2023, according to Dr. Glory Alexander, President of AIDS Society of India (ASI).
“Before treatments were available to prevent vertical transmission, the risk of a newborn acquiring HIV in India ranged from 15 percent to 45 percent. The risk was nearly 45 percent among infants who were breastfed,” Dr. Alexander said.
She attributed the reduction to the introduction of antiretroviral therapy (ART) and implementation of HIV prevention and treatment guidelines.
"The government has successfully reduced the rate of infant HIV diagnosis (risk of a child getting infected with HIV due to vertical transmission) to 0.71 percent. We need to further reduce it to zero to eliminate vertical transmission of HIV,” Dr. Alexander added.
Intensifying Last-Mile Approach
India reportedly has 27-29 million pregnancies every year.
As per the latest National AIDS Control Organization (NACO) report, 83 percent of all pregnant women are tested for HIV, and 78 percent of all pregnant women are tested for syphilis in India.
“Out of an estimated 19,000 pregnant women who might be living with HIV in India, over 16,000 were reached by the government-run program and linked to services -- half of them were newly diagnosed with HIV,” Dr. Alexander said.
NACO runs 794 antiretroviral therapy centers across the country and provides free HIV treatment to 18 lakhs people with HIV.
NACO's over 700 “Suraksha Sewa Kendras” also provide preventive services for people who are at risk of acquiring HIV.
Dr. Ishwar Gilada, Emeritus President of AIDS Society of India (ASI), called India's progress "commendable."
"But to end AIDS, the last mile approach has to be accelerated and intensified manifold,” the expert said.
Increase HIV Testing Manifold
Dr. Gilada stressed the need to "ensure that all key populations know their status, and those with HIV are linked to treatment, care, and support services and remain virally suppressed".
If a person with HIV is virally suppressed, then there is zero risk of any further HIV transmission, as per the WHO, he added.
Indian data shows 9-43 times higher HIV rates (as compared to the general population) among key populations, such as men who have sex with men, transgender people, sex workers, people who inject drugs, among others.
These key populations are hard to reach, which warrants community-led and science-backed approaches, said Dr. Gilada.
Reducing Advanced HIV Disease
Despite commendable progress in India’s HIV response, there is a huge number of cases of advanced HIV disease (AHD) -- about one third of all people living with HIV in the country, the experts said.
The World Health Organization (WHO) defines AHD as a CD4 count less than 200 cells per cubic millimeter/ or WHO stage 3/4 in adults/adolescents, and all children less than 5 years old.
It indicates a severely weakened immune system, high mortality risk, and vulnerability to infections like TB and cryptococcal meningitis.
AHD cases in India are majorly among those who are HIV infected but are not on lifesaving antiretroviral treatment.
"This could be because HIV infection is undiagnosed in people until they present with opportunistic infections to healthcare centers, or they were not able to adhere to the treatment for a range of reasons,” said Dr Trupti Gilada, Joint Secretary, AIDS Society of India (ASI).
TB, which is preventable and treatable, is the most common opportunistic infection among people with HIV.
Another concern is the rising antimicrobial resistance in HIV patients. Studies show that people with HIV are 2-3 times more likely to get drug-resistant forms of TB.
© 2024 Bennett, Coleman & Company Limited

