- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Spotting vs Period vs Bleeding: How To Identify
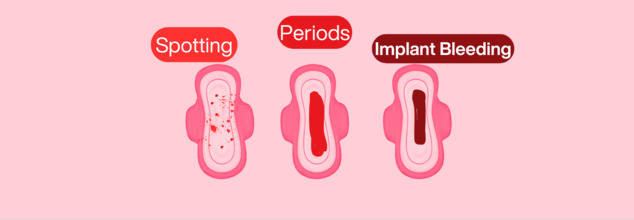
Image Credits: Health and me
A woman's health is intricately linked to her menstrual cycle, which is an important sign of her overall well-being. Throughout puberty and menopause, hormonal changes affect not only fertility but also mood, energy, and long-term health. A normal cycle usually indicates balance, whereas abnormalities may suggest problems such as PCOS, endometriosis, or thyroid disease.
Our bodies do not always work in a perfect clockwork operation and unexpected vaginal bleeding can often confused us. Is it a mere spotting? A normal period? A symptom of something more concerning? Differences between spotting, menstrual bleeding, and intermenstrual bleeding should be understood is crucial for maintaining reproduction health.
Here is a short guide to help you differentiate while you are confused.
Spotting
Spotting is vaginal bleeding that doesn't happen as part of your regular menstrual period. It commonly manifests as fine droplets or smears of blood on clothing or toilet tissue. The intensity of the blood ranges from deep red (recent blood) to pink (having cervical mucus mixed in it) or brown (older, oxidized blood). Spotting is not very much and can't be seen in a way that needs either a tampon or a pad to absorb.
Common Causes of Spotting
Spotting is caused by numerous factors, and in the majority of instances, it is nothing to worry about. Some frequent causes are:
Hormonal Birth Control Transitions: New birth control technique, for instance, birth control pills, IUDs containing hormones, or implants, results in temporary spotting as the body adapts.
Ovulation Bleeding: A few individuals get spotting light around the time of ovulation as a result of hormonal changes. It normally happens in the mid-cycle and could be followed by slight cramping.
Cervical Ectropion: A harmless condition when cells from the inside of the cervical canal migrate to the outer cervix, causing the outer cervix to become more sensitive and prone to faint bleeding on coitus or physical activity.
Early Pregnancy (Implantation Bleeding): 15–25% of pregnant women experience light spotting around 10–14 days post-conception, which is confused with an early period.
When to See a Doctor
Spotting is usually harmless, but it's best to consult a doctor if:
- It continues after a few months of initiating new birth control
- Is accompanied by pelvic pain or abnormal discharge
- Occurs after frequent intercourse
- Occurs during pregnancy and is not verified as implantation bleeding
Menstrual Bleeding
There is a time, also known as a period or menstruation, when the uterine lining sheds due to changing hormone levels. It would last for approximately 2-7 days and is heavier initially. The hue and texture of period blood shift during the menstrual cycle:
Red: New active bleeding at the start of a period
Brown or dark red: Older, slower blood in leaving the uterus
Clots: It's normal to have small clots, but bigger clots may be a sign of heavy menstrual bleeding (HMB)
Why You Have a Period Essentially?
Menstruation is a part of the reproductive cycle, and it happens around every 21–35 days. When there's no pregnancy after ovulation, hormone levels fall, causing the uterine lining to be shed.
Signs Your Period May Be Abnormal
Though periods differ in different people, there are some signs that point towards probable underlying conditions:
- Prolonged bleeding (longer than 7 days)
- Heavy flow necessitating pad/tampon changes every 1–2 hours
- Severe cramps that disrupt daily life
- Irregular periods or absent periods
If you have any of these, conditions such as polycystic ovary syndrome (PCOS), endometriosis, or thyroid disease may be involved, and a medical visit is in order.
Intermenstrual Bleeding
Unlike spotting, intermenstrual bleeding is heavier and unexpected between regular periods. It may be from bright red to dark brown and can contain blood clots.
Possible Causes of Bleeding Between Periods
Sexually Transmitted Infections (STIs): Chlamydia and gonorrhea can lead to inflammation and abnormal bleeding.
Pelvic Inflammatory Disease (PID): A bacterial infection of the reproductive organs and can lead to abnormal bleeding.
Uterine Fibroids or Polyps: Benign growths in the uterus that may cause unexpected bleeding.
Endometrial Hyperplasia or Cancer: In some instances, abnormal bleeding may be a sign of abnormal cell growth in the lining of the uterus.
When to See a Doctor
See a doctor if intermenstrual bleeding is:
- Frequent or persistent
- Associated with pelvic pain or discomfort
- Associated with abnormal discharge, fever or painful sex
Recognizing your body's rhythms can assist you in identifying normal versus abnormal bleeding. Monitoring your menstrual cycle through an app or calendar may flag changes that should be checked with a doctor. If you have any questions regarding abnormal bleeding, visiting your health care provider is the way to go.
Dhurandhar 2 Actor Mustafa Ahmed Opens Up On Growing Up With Dyslexia

Credits: Instagram
Dhurandhar 2 actor Mustafa Ahmed, who played Rizwan in the film, opened up about growing up with dyslexia. He shared that he struggled with reading and writing, but sports and dancing came naturally to him.
"I was not a bright kid. I was dyslexic and came from an Afghan background. But I was always physical, I was good at sports, and I picked up dancing naturally. Anything that involved using my body, I was good at it,” said Mustafa, who trained has Hrithik Roshan, in the Alpha Coach podcast.
What Is Dyslexia?
Dyslexia is a learning difficulty that affects reading, writing, and spelling. However, it has nothing to do with intelligence.
Common signs of dyslexia include:
- Difficulty reading or recognizing words
- Trouble with spelling and writing
- Confusing similar-looking letters (like b/d or p/q)
- Slow reading speed and poor comprehension
- Difficulty following written instructions
This means that children with dyslexia are simply wired differently and may need to focus on other learning areas.
How Did Mustafa Overcome Dyslexia?
Mustafa did exactly that. He focused on training hard and eventually worked with big stars like Hrithik Roshan. That’s when he caught the attention of Aditya Dhar, the maker of Dhurandhar. Aditya saw potential in him and encouraged him to pursue acting, helping launch his journey in the industry.
Growing up, Mustafa, who revealed in an interview, faced challenges in school due to his learning difficulties. Tasks like reading scripts or memorizing lines may not have come easily at first. However, with determination, support, and self-belief, he was able to overcome these barriers.
However, today as a rising star, his story is a reminder that with the right support, early diagnosis, and self-belief, children with dyslexia can truly thrive.
Signs and symptoms of dyslexia
Doctors say signs of dyslexia can look different at each age. It happens because your brain grows and learns in new ways as you get older. You may notice your child has:
- Has difficulty learning or recognizing letters
- Has trouble rhyming words
- Mixes up words that sound similar
- Find it difficult to read simple words after learning letter sounds
- Have trouble remembering letters, even after lots of practice
- Avoiding tasks that have to do with reading
- Feeling sick or anxious before school or homework time
- Struggling in school
Can You Treat Dyslexia?
Doctors say even though dyslexia is a lifelong condition, it can be effectively managed with the help of interventions like:
- Phonics-based reading programs
- One-on-one tutoring
- Speech and language therapy
- Use of assistive technology like audiobooks and text-to-speech tools
With these strategies, individuals with dyslexia can improve their reading skills and excel in their chosen fields.
Mel Schilling Dies At 54, Her Colon Cancer Spread To Her Brain

Credits: Instagram
Mel Schilling, an Australian psychologist and a dating expert died at 54. Her husband Gareth Brisbane announced the death in a social media statement.
What Happened To Mel Schilling?
Schilling was diagnosed with colon cancer in December 2023. Just two weeks ago she said that the disease had spread to her brain. "I honestly don't know how long I have left," she wrote.
Read: What Is The Correct Age To Get A Colonoscopy?
According to her husband, she died "peacefully, surrounded by love". “This is a woman who, through two years of chemotherapy, when she could barely lift her head from the pillow, never complained and never stopped showing courage, grace, compassion and empathy, and never missed a day of filming,” Brisbane wrote.
She was also an expert on 'Married at First Sight Australia' for 12 years and because of her illness she stepped down as a dating expert.
How Does Cancer Spread To Other Parts Of The Body?
Schilling said that her cancer had spread to her brain. as per the Cancer Research UK, cancer cells can spread to other parts of the body through bloodstream or lymphatic system. They can then start to grow into new tumors. The National cancer Institute notes that cancer cells spread through the body in a series of steps, which include:
- growing into, or invading, nearby normal tissue
- moving through the walls of nearby lymph nodes or blood vessels
- traveling through the lymphatic system and bloodstream to other parts of the body
- stopping in small blood vessels at a distant location, invading the blood vessel walls, and moving into the surrounding tissue
- growing in this tissue until a tiny tumor forms
- causing new blood vessels to grow, which creates a blood supply that allows the metastatic tumor to continue growing
What Is Colon Cancer?
Colon (colorectal) cancer begins when small growths called polyps form on the inner lining of the colon or rectum. Over time, changes in the DNA of these cells can cause the polyps to become cancerous.
As abnormal cells multiply, they replace healthy cells and eventually form a mass known as a tumor. This process develops slowly, often taking up to ten years for a precancerous polyp to turn into cancer and begin showing symptoms.
Colon cancer poses serious health risks because cancerous cells can invade healthy tissues. Over time, they may break away and spread to other parts of the body, making detection more difficult since the symptoms can resemble other conditions.
How Can You Get Screened For Colon Cancer?
You can get examined by a colonoscopy. A colonoscopy is a 15 to 60 minute medical procedure that is used to examine the entire inner lining of the large intestine, which includes rectum and colon for abnormalities, such as polyps, inflammation, or cancer. A doctor uses a colonoscope, which is a thin, flexible tube with a camera to take images, remove polyps, or take issue samples.
Most health experts, including federal guidelines and the American Cancer Society, recommend that people at average risk for colorectal cancer start screening at age 45. This usually means getting a colonoscopy once every 10 years, or opting for stool-based tests every one to three years. These guidelines also play a role in whether insurance companies cover the tests.
What Is The Correct Age To Get A Colonoscopy?

March is the month of colon cancer awareness and with the recent cases of colon cancer patients who are younger than 50. With the death of 48-year-old actor James Van Der Beek due to colorectal cancer, concerns are rising. While cancer death rates overall in people younger than 50may have dropped by 44% since 1990, colorectal cancer has become the leading cause of cancer death in people under 50.
Can Karlyle Morris, section chief for colorectal cancer at MD Anderson Center in Houston tells NBC News, "We anticipate that this is going to be a continued trend."
What Is Colon Cancer?
Colon (colorectal) cancer begins when small growths called polyps form on the inner lining of the colon or rectum. Over time, changes in the DNA of these cells can cause the polyps to become cancerous.
As abnormal cells multiply, they replace healthy cells and eventually form a mass known as a tumor. This process develops slowly, often taking up to ten years for a precancerous polyp to turn into cancer and begin showing symptoms.
Colon cancer poses serious health risks because cancerous cells can invade healthy tissues. Over time, they may break away and spread to other parts of the body, making detection more difficult since the symptoms can resemble other conditions.
What Is The Right Age To Get Colonoscopy?
A colonoscopy is a 15 to 60 minute medical procedure that is used to examine the entire inner lining of the large intestine, which includes rectum and colon for abnormalities, such as polyps, inflammation, or cancer. A doctor uses a colonoscope, which is a thin, flexible tube with a camera to take images, remove polyps, or take issue samples.
Most health experts, including federal guidelines and the American Cancer Society, recommend that people at average risk for colorectal cancer start screening at age 45. This usually means getting a colonoscopy once every 10 years, or opting for stool-based tests every one to three years. These guidelines also play a role in whether insurance companies cover the tests.
Even so, most cases of colon cancer are still diagnosed in people over 50. What’s worrying, though, is the steady rise in cases among younger adults in their 20s, 30s and 40s over the past few decades.
Why Does Screening Begin At 45?
Colon cancer typically develops slowly. It often starts as small growths in the colon called polyps, which can eventually turn cancerous if not detected early.
In recent years, growing evidence has pushed experts to reconsider when screening should begin. In 2021, the U.S. Preventive Services Task Force lowered the recommended screening age from 50 to 45. The American Cancer Society had already made a similar recommendation back in 2018.
At the time, the change was not universally accepted. Some in the medical community felt 45 was still too young. Even today, there is ongoing debate.
Setting screening guidelines is not as simple as picking an age. Experts have to weigh the benefits of early detection against potential downsides, including costs, risks from procedures and even practical concerns like taking time off work.
The numbers also tell an important story. For people aged 40 to 44, the risk of colorectal cancer is about 21 cases per 100,000 individuals. That risk more than doubles to 47 per 100,000 between ages 45 and 49, which is one of the reasons screening begins at that point.
Still, younger adults account for a relatively small proportion of cases overall. According to the Mayo Clinic, about 10 percent of colorectal cancer cases occur in people under 50.
The Challenge Of Resources And Awareness
Another key factor is access. There are only so many specialists available to perform colonoscopies, and even now, people can wait months for an appointment.
On top of that, screening rates among younger eligible adults remain low. Only about one in five people aged 44 to 49 are up to date with recommended screenings.
Experts say that if the screening age were lowered further, participation might drop even more. For now, the focus remains on improving awareness and encouraging those already eligible to get screened on time.
© 2024 Bennett, Coleman & Company Limited

