- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Surprising Way To Manage Your Aviophobia

Credit: Canva
Flying was once a distant dream, but with the invention of airplanes, it has become a routine and widely accessible means of travel. According to the International Air Transport Association (IATA), nearly 100,000 flights take off around the world each day. In 2024 alone, an estimated 4.4 billion passengers flew globally. In the United States, the Bureau of Transportation Statistics (BTS) recorded a historic peak of 848 million passengers in the same year.
The popularity of air travel has not only grown in volume but also in safety. The IATA reported that the global accident rate in 2023 was just one accident per 1.26 million flights — the safest it has been in decades. Research consistently shows that air travel is statistically safer in terms of fatalities than any other common mode of transport.
Yet for some, flying remains a source of significant distress. Known as aviophobia, the fear of flying is a persistent and intense anxiety that goes far beyond typical nervousness. People with aviophobia often dread flying days or even weeks in advance, and their fear can become overwhelming.
How To Manage Aviophobia
If you suffer from a fear of flying, several techniques may help ease your discomfort.Stay Centered
Try deep breathing exercises—inhale for four counts, then exhale for six. Repeat a calming mantra, such as reminding yourself that air travel is the safest form of transportation. Reframe your focus by thinking about the excitement awaiting you upon arrival instead of dwelling on your fears.
Find A Focus
Engage in grounding techniques, such as crossing your arms and ankles while breathing deeply. Use your senses: observe five things you can see, four you can touch, three you can hear, two you can smell, and one you can taste. Hold a comforting item like a stress ball or smooth stone. Listening to calming audio, like music or meditation, and visualizing peaceful places can also help.
Reduce External Stressors
Pull down the window shade to avoid watching the scenery fly by. Use noise-canceling headphones to block out cabin noise, and wear an eye mask to minimize bright lights.Prepare For Anxiety
Practice mindfulness or meditation for a week or two before your flight. If needed, speak to a therapist before flying. If possible, visit the airport in advance or visualize the process of checking in and boarding to feel more in control.Distract Yourself
Load your device with movies or shows, bring a book, work on puzzles, journal, listen to a podcast, or play a mobile game to occupy your mind during the flight.
Avoid Added Anxiety Triggers
Steer clear of caffeine, sugary snacks, and energy drinks before flying, as these can increase feelings of anxiety.Understand Your Specific Fear
Pinpoint what aspect of flying scares you. If it's the fear of losing control, reading about aviation safety might help. For claustrophobia, consider booking an aisle seat or requesting early boarding.
Meningitis Outbreak: How to Differentiate The Symptoms From a Common Rash
Credits: Canva
Meningitis outbreak has led to authorities in the UK to urge students to get vaccines and antibiotics. Health and Me also reported on the menB vaccine that students 5,000 students in Kent University will be receiving. One of the common symptoms are rashes, however, how does one know if it is a meningitis rash?
How Do You Recognize Meningitis Rash?
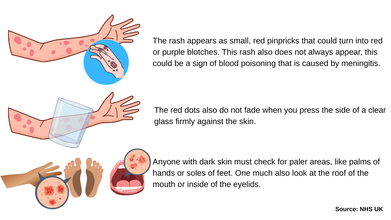
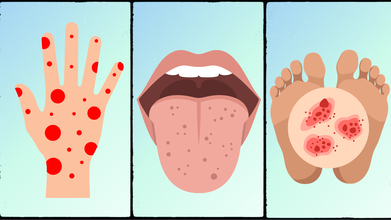
As per NHS UK, the rash appears as small, red pinpricks that could turn into red or purple blotches. This rash also does not always appear, this could be a sign of blood poisoning that is caused by meningitis.
The red dots also do not fade when you press the side of a clear glass firmly against the skin. NHS UK notes that anyone with dark skin must check for paler areas, like palms of hands or soles of feet. One much also look at the roof of the mouth or inside of the eyelids.
NHS UK notes that one must call 999, if they find such a rash.
Meningitis Outbreak UK: What Is Happening Now?
A meningitis outbreak in Kent University is now treated as a national incident, after two people have died, one of them being the student of the university. Students have been urged to get vaccines and take antibiotics as health officials are dealing with the "unprecedented" and "explosive" outbreak.
As per the UK Health Security Agency (UKHSA), 15 cases have been reported and all of them have lead to hospital admission. Cases are also expected to rise due to the incubation period of infection to when the symptoms start to appear. The incubation period is from two to 14 days.
As per experts, many of whom are affected had attended Club Chemistry in Cantebury between 5 to 7 March. UKHSA chief executive Susan Hopkins said the outbreak "looks like a super-spreader" event with "ongoing spread" through universities' halls of residence. She added: "There will have been some parties particularly around this, so there will have been lots of social mixing. I can't yet say where the initial infection came from, how it's got into this cohort, and why it's created such an explosive amount of infections."
She further said that in her 35 years working in medicine, healthcare, and hospitals, "This is the most cases I've ever seen in a single weekend with this type of infection". She added: "It is the explosive nature that is unprecedented here - the number of cases in such a short space of time." She also remarked that this was the "quickest-growing outbreak" she has ever seen in her career.
Who Should Get MenB Vaccine?
As per the University of Oxford, MenB vaccine is given to babies at 8 weeks, 16 weeks, and one year of age.
General Practitioner surgery or clinic also send an appointment for babies to have their MenB vaccination along with their other routine vaccinations.
Read: Meningitis Outbreak: What Is MenB Vaccine?
Additional doses of the vaccine are recommended for people with some long-term health conditions who are at greater risk of more severe meningococcal disease. This includes people with:
- asplenia or splenic dysfunction (a spleen that is missing or does not work properly)
- sickle cell anaemia
- coeliac disease
- complement disorders (the complement system is an important part of the immune system, and disorders of this system can increase a person’s risk to some diseases.)
Meningitis Outbreak: What Is MenB Vaccine?
Credits: Canva
Meningitis outbreak has led to death of two people, one of them being a student of Kent University. Students have also been urged to get vaccines and take antibiotics. Health and Me also reported on the outbreak and how this has led to panic among parents who are seeking for meningitis B or menB vaccine. 5,000 students in the university halls in Kent will be offered the menB vaccine in the coming days.
What Is MenB Vaccine?
London School of Hygiene & Tropical Medicine noted that over a dozen people are seriously unwell in hospital and two people have died from an outbreak of meningitis in the UK. As per the UK Health Security Agency, illness may have spread during an event attended by students in Kent. Four cases have been confirmed to be meningitis B through laboratory testing.
As per NHS UK, menB vaccine offers protection against meningococcal group B bacteria, which is identified to be the strain that has infected people. The vaccine is recommended for babies aged 8 weeks, followed by a second dose at 12 weeks and a booster at 1 year.
Read: Kent Uni Meningitis Outbreak Caused By Less-Targeted Strain B
Who Should Get MenB Vaccine?
As per the University of Oxford, MenB vaccine is given to babies at 8 weeks, 16 weeks, and one year of age.
General Practitioner surgery or clinic also send an appointment for babies to have their MenB vaccination along with their other routine vaccinations.
Additional doses of the vaccine are recommended for people with some long-term health conditions who are at greater risk of more severe meningococcal disease. This includes people with:
- asplenia or splenic dysfunction (a spleen that is missing or does not work properly)
- sickle cell anaemia
- coeliac disease
- complement disorders (the complement system is an important part of the immune system, and disorders of this system can increase a person’s risk to some diseases.)
The University of Oxford noted that from August 2025, the MenB vaccine has been offered primarily to gay, bisexual and other men who have sex with men, in a targeted programme to prevent cases of gonorrhoea. This is because these groups of people are at higher risk of acquiring gonorrhoea.
How Does Meningitis B Spread?
Neisseria meningitidis is most commonly found living in the throat. It is spread between people through close contact with secretions from the mouth or airway and usually requires close or prolonged contact between people for the bacteria to be transmitted.
Common Symptoms Of Meningitis
- Headaches
- Neck stiffness
- Fever
- Drowsiness
- Nausea or vomiting
- Increased sensitivity to light
Some meningitis infections can also cause a rash that does not disappear with pressure. However they may not be always visible in the early stages.
No Refrigeration Needed: New Vaccine May Expand Immunization Worldwide
Credits: Canva
Vaccines are among the most powerful tools in modern medicine, preventing millions of deaths each year. Yet getting those vaccines safely from laboratories to people who need them is far more complicated than many realise. Most vaccines must be kept within a strict temperature range between 2°C and 8°C from the moment they are produced until they are administered.
This temperature controlled system, known as the cold chain, depends on refrigerators, insulated transport boxes and a steady supply of electricity at every step of the journey. Any disruption can damage the vaccine and make it ineffective. Now, scientists are testing a new technology that could remove this challenge altogether.
A vaccine designed to remain stable even at room temperature has shown encouraging results in an early human trial. Researchers believe this could change how vaccines are distributed, especially in regions where refrigeration is difficult to maintain.
The Challenge Of Keeping Vaccines Cold
Vaccines are sensitive biological products. Exposure to excessive heat or freezing temperatures can damage their active ingredients and reduce their ability to trigger an immune response.
To avoid this, countries rely on a carefully managed cold chain that transports vaccines from manufacturing facilities to warehouses, regional storage centers and finally to clinics. This process requires specialised equipment, trained staff and constant monitoring of temperatures.
However, maintaining this system is both expensive and complex. Equipment failures, power outages and transport delays can disrupt the cold chain at any stage. In rural or remote regions where electricity supply is unreliable, these challenges become even more serious.
Global health experts estimate that a large number of vaccines are lost every year because of temperature control failures during storage and transport. This leads to wasted doses, increased costs and gaps in vaccination coverage.
Because of these difficulties, scientists have long been searching for ways to develop vaccines that can remain effective without strict refrigeration.
A Vaccine That Can Survive At Room Temperature
One promising development is a vaccine candidate called SPVX02, which targets tetanus and diphtheria. It has been developed by the biotechnology company Stablepharma with support from the UK Health Security Agency.
What makes this vaccine different is the technology used to stabilize its active ingredients. The formulation allows the vaccine to tolerate higher temperatures without losing potency.
Early findings from a Phase I clinical trial suggest the vaccine can remain stable at around 30°C for as long as two years. The study was carried out at the Vaccine Development and Evaluation Centre in the United Kingdom and involved healthy volunteers.
Phase I trials are the earliest stage of human testing. At this stage, researchers focus mainly on safety, possible side effects and the body’s immune response.
If further trials confirm these findings, the same stabilization technology could potentially be applied to other vaccines as well.
Why This Could Matter For India
A fridge free vaccine could have major implications for countries such as India, which runs one of the largest immunization programmes in the world.
India’s Universal Immunisation Programme delivers vaccines to millions of children every year. To reach remote villages and urban settlements, the programme depends on a vast cold chain network that includes refrigerated storage facilities, specialized transport and vaccine carriers.
Maintaining this infrastructure across a country with varied climates and uneven electricity supply can be difficult. Heat exposure during transport or power failures can lead to spoilage and wastage.
A thermostable vaccine that remains effective at room temperature could simplify this process significantly. It would reduce dependence on refrigeration, lower costs and make it easier to deliver vaccines in remote or resource limited areas.
What Happens Next
Although the early results are encouraging, the vaccine still needs to go through larger clinical trials before it can be approved for widespread use.
Future studies will involve more participants and compare the new formulation with existing refrigerated vaccines to confirm its effectiveness.
If the technology proves successful, researchers believe it could be adapted for many other vaccines in the future. That possibility could reshape how immunization programmes operate worldwide and help bring life saving vaccines to communities that have long struggled to access them.
© 2024 Bennett, Coleman & Company Limited

