- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
This Deadly Liver Disease Is Affecting People In Their 20s And This One Symptom Is The Red Flag
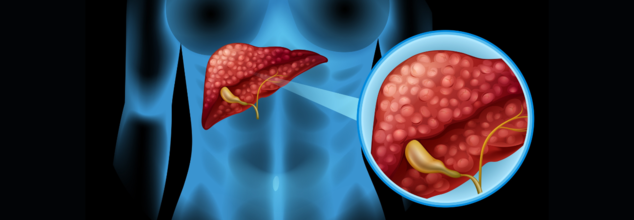
Credits: Canva
A silent epidemic is sweeping across the globe, affecting millions—many of them young adults in their 20s—without their knowledge. Non-alcoholic fatty liver disease (NAFLD), now also referred to as metabolic dysfunction-associated steatotic liver disease (MASLD), is emerging as one of the most deadly and underdiagnosed health threats of our time. Recent research published in The Lancet Regional Health Europe reveals that nearly 20 million people across the US, UK, Germany, and France are living with this condition, yet only a fraction have been formally diagnosed. Even more concerning: three-quarters of those affected have no idea they are at risk.
Once thought to be a disease of the middle-aged and overweight, NAFLD is now increasingly seen in young, seemingly healthy individuals, many of whom are asymptomatic. New research reveals that nearly 20 million people across the U.S., UK, Germany, and France are living with NAFLD—with only 2.5 million actually diagnosed. That means three out of four people have no idea they’re living with a condition that, left untreated, could progress to cirrhosis or even liver cancer.
NAFLD is often called a “silent” disease for good reason. It develops quietly, often without any symptoms, and can go undetected for years. In many cases, it is only discovered incidentally—when a patient undergoes imaging studies for unrelated health issues. This stealthy progression is what makes NAFLD so dangerous. According to experts, it is now estimated that nearly one in three adults worldwide may have some form of fatty liver disease, and the numbers are rising among younger populations.
In MASH, the liver becomes inflamed due to fat deposits. Inflammation and scarring (fibrosis) may eventually lead to cirrhosis, liver failure, or liver cancer. What makes NAFLD particularly concerning is how quietly it progresses. In many cases, it is only discovered incidentally—through imaging tests done for unrelated health issues.
Dr. Joseph Salhab, a leading gastroenterologist, describes NAFLD as “the most deadly yet underdiagnosed condition.” He stresses that most people with fatty liver have no signs or symptoms, and up to 50% may even have normal lab tests. This makes routine screening and awareness all the more critical.
What Is Non-Alcoholic Fatty Liver Disease?
NAFLD occurs when more than 5% of the liver’s weight is made up of fat, in individuals who consume little to no alcohol. This distinguishes it from alcohol-related fatty liver disease. The condition is closely linked to metabolic dysfunction, including obesity, type 2 diabetes, high cholesterol, and high blood pressure, but it can also affect people who have none of these risk factors.
NAFLD exists on a spectrum. The earliest and least severe stage is “simple fatty liver,” where fat builds up in the liver cells but there is little or no inflammation or damage. However, the disease can progress to a more serious form called metabolic dysfunction-associated steatohepatitis (MASH). In MASH, the liver becomes inflamed due to fat accumulation, which can lead to scarring (fibrosis), cirrhosis, liver failure, and even liver cancer.
Red Flag Symptom You Shouldn’t Ignore
According to Dr. Joseph Salhab, a gastroenterologist who has observed hundreds of patients with fatty liver disease, there is one symptom that often stands out—fatigue.
“Fatigue is probably one of the most commonly reported symptoms in people with fatty livers,” says Dr. Salhab. “We think it’s linked to metabolic dysfunction in the liver and poor sleep regulation.”
He also notes that pain in the upper right quadrant of the abdomen—especially discomfort after eating—is another early sign of liver inflammation. But the most troubling symptom of all may be no symptom at all.
“NAFLD is a sneaky disease,” he emphasizes. “Around 50% of people with fatty liver can even have normal lab results. You can’t rely on symptoms alone.”
Why Young Adults Are Now at Risk?
What’s particularly alarming is the growing number of younger adults—even those in their 20s—being diagnosed with NAFLD. This trend aligns with the global rise in obesity, sedentary lifestyles, and diets high in processed foods, all of which are risk factors.
Historically, NAFLD was seen primarily in middle-aged or older adults. However, the rise in obesity, sedentary lifestyles, and poor dietary habits has led to an alarming increase in cases among people in their 20s and even teenagers. The modern diet—high in processed foods, sugars, and unhealthy fats—combined with decreased physical activity, is fueling this trend.
Recent data show that more than 15 million people in the US, UK, Germany, and France are unaware they have the most aggressive form of fatty liver disease. And while being overweight, having type 2 diabetes, or high cholesterol increases the risk, NAFLD can—and does—affect people without any of these conditions.
How Is NAFLD Diagnosed?
Because symptoms are often absent, NAFLD is frequently discovered during routine bloodwork or imaging scans, such as ultrasounds or CT scans, conducted for other reasons. In some cases, a liver biopsy may be required to assess the level of inflammation and scarring. NHS Inform and Mayo Clinic list the following signs that may warrant further investigation:
- Persistent fatigue
- Abdominal discomfort (especially upper right quadrant)
- Itchy skin
- Abdominal swelling or fluid retention
- Swelling in legs
- Spider veins, red palms, and in advanced stages, jaundice
The real danger of NAFLD lies in its potential to progress. For some, simple fatty liver remains relatively benign. But for others, the disease advances to MASH, causing inflammation and scarring. Over time, this can lead to cirrhosis (permanent liver damage), liver cancer, or even liver failure—conditions that are often fatal without a transplant.
Alarmingly, the vast majority of those with NAFLD have no idea their liver is under threat. According to the research, only 2.5 million out of 20 million people with the disease have received a diagnosis. This means millions are at risk of severe complications without knowing it.
Can NAFLD Be Reversed?
NAFLD is reversible, especially in its early stages. The primary treatment isn’t medication—it’s lifestyle modification, and the most effective step is weight loss.
According to Dr. Chris Boettcher, a physician advocating for liver health awareness, “Just losing 7–10% of your body weight can reverse fatty liver in up to 90% of patients.”
The Mayo Clinic supports this, noting that even 3–5% weight loss can significantly reduce liver fat, while 10% or more can reverse inflammation and fibrosis. Key steps to reversing NAFLD include:
- Adopting a Mediterranean-style diet rich in vegetables, whole grains, lean proteins, and healthy fats
- Exercising regularly, with a focus on both cardio and strength training
- Managing blood sugar, cholesterol, and blood pressure
- Avoiding alcohol and unnecessary medications that stress the liver
With 1 in 3 adults potentially affected, NAFLD represents a looming public health crisis. Yet the condition remains underdiagnosed, and awareness is critically low—even among healthcare providers.
Dr. Boettcher calls it “the most deadly yet underdiagnosed condition,” warning that if the current trend continues, NAFLD could soon overtake hepatitis as the leading cause of liver transplants.
The medical community is now urging health systems to incorporate early screening for at-risk groups and raise awareness of subtle symptoms.
What You Can Do Right Now To Protecting Your Liver?
Whether you’re in your 20s or your 60s, now is the time to take charge of your liver health. Here’s how to start:
- Get a routine check-up—especially if you have any metabolic risk factors.
- Ask your doctor about a liver ultrasound or fibrosis scan if you experience unexplained fatigue or abdominal discomfort.
- Track your weight, blood sugar, and cholesterol regularly.
- Eliminate excess sugar, saturated fats, and alcohol from your diet.
- Prioritize movement—even 30 minutes of walking a day makes a difference.
NAFLD is a global health crisis hiding in plain sight—affecting millions, including people in their 20s, with most unaware of their risk. Fatigue is the one symptom that should not be ignored, but the absence of symptoms does not mean the absence of disease. Routine screening, especially for those at risk, is essential.
As Dr. Chris Boettcher, a physician and advocate for NAFLD awareness, emphasizes: “Just losing 7-10% of your bodyweight reverses non-alcoholic fatty liver disease in up to 90% of people. It directly burns liver fat, lowers inflammation, and reduces insulin resistance.”
Recognizing fatigue or unexplained abdominal pain might just be the red flag you need to start asking questions and demand screening.
1 In 4 Diabetic Patients in India Suffer from Liver Fibrosis, Finds Lancet Study
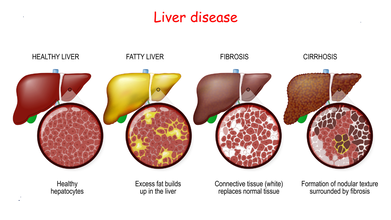
Credit: iStock
One in four or 25 percent of adults with type-2 diabetes in India also suffer from liver fibrosis, according to an alarming study published in The Lancet Regional Health Southeast Asia journal today.
With data from more than 9,000 patients across the country, it is the largest ever real-world survey of liver fibrosis in type 2 diabetes from any low- or middle-income country.
While fatty liver disease has been touted as the most common liver condition among diabetes patients, the new study established liver fibrosis as the real danger among people with high blood sugar.
“Type 2 diabetes is closely linked to fatty liver disease (also known as MASLD). But how common is liver Fibrosis — the real danger — in Indian diabetics? Our answer: 1 in 4 has clinically significant liver fibrosis. One in 20 already has probable cirrhosis. Most had no symptoms. We propose liver fibrosis as the ‘4th major complication’ of diabetes,” said Ashish Kumar, from Ganga Ram Postgraduate Institute of Medical Education and Research (GRIPMER), from Sir Ganga Ram Hospital, in a post on social media platform X.
What Did The Study Find?
Fatty liver is typically the first and reversible stage of liver disease, where excess fat builds up in liver cells. Left untreated, it progresses to liver fibrosis, which is the excessive accumulation of scar tissue (collagen) in the liver resulting from chronic inflammation. The condition then progresses to the third and late stage, irreversible scarring (fibrosis) of the liver. The final stage is liver cancer.
The DiaFib-Liver Study included a total of 9,202 adults with type-2 diabetes patients who underwent FibroScan (VCTE) to assess liver fibrosis in routine diabetes care.
Of these:
- 26 percent had clinically significant fibrosis,
- 14 percent had advanced fibrosis,
- 5 percent had probable cirrhosis
- 65 percent had fatty liver disease.
- obesity
- dyslipidaemia
- kidney problems
- diabetes duration ≥10 years.
Fibrosis: The Screening Target
The study suggested the urgent need to integrate fibrosis screening into national diabetes programs.
“One in four adults with type 2 diabetes in India has clinically significant liver fibrosis and one in twenty already has probable cirrhosis, establishing advanced liver disease as a 'fourth major complication' of diabetes,” said the researchers.
“The DiaFibLiver Study calls for: Fibrosis — not steatosis — as the screening target. FibroScan integration into routine diabetes care. Moving beyond ultrasound-based referral,” Jha said.
“We hope this data from India adds to the global conversation on diabetes and liver disease,” he added.
Also read: The Silent Rise of Fatty Liver Disease: How India-Specific Guidelines Can Help
The findings highlight the urgent need to:
- move beyond steatosis
- systematically integrate fibrosis assessment into routine diabetes care,
- deploy non-invasive tools such as vibration-controlled transient elastography (VCTE) in community practice
- define screening strategies,
- evaluate therapeutic interventions.
Everyday Habits That Harm the Liver
Certain lifestyle choices can accelerate liver damage, such as:
Overeating processed or fried foods
High sugar intake (soft drinks, sweets, desserts)
Physical inactivity or prolonged sitting
Ignoring health issues like diabetes or hypertension
Crash dieting or taking unprescribed supplements.
How To Improve Liver Health?
Early screening and detection are key to prevent irreversible stages. Yet liver disease can be prevented with lifestyle changes such as:
- Eating a balanced diet with vegetables, fruits, whole grains, and lean protein
- Engaging in at least 30 minutes of exercise daily
- Staying hydrated to help the liver flush out toxins
- Avoiding alcohol and smoking
- Avoiding self-medication and unnecessary pills
- Getting routine health screenings.
Problem Of Plenty: Psychiatrist Explains How Too Many Choices Affect Mental Health

Taking too many decisions in a day can lead to mental exhaustion. (Photo credit: iStock)
New Delhi: Every day, the brain processes hundreds of choices. Most pass unnoticed: what to wear, which route to take, what to eat. But accumulated over hours and across competing demands, this constant decision-making exacts a cost. Decision fatigue is the gradual erosion of the brain’s capacity to make good choices, and over time it affects both mental functioning and physical health. Dr Shivi Kataria, Consultant – Psychiatry, CK Birla Hospitals, Jaipur, addressed the problem of plenty and said that it could take a toll on mental health in certain circumstances.
Read more: India Launches 1st Repository Of Data On Major Psychiatric Disorders
What are the signs?
The earliest signs tend to be emotional. Simple decisions start to feel disproportionately heavy. Choosing between two options takes longer than it should. Irritability surfaces. Tasks that once felt manageable begin to pile up as the mental energy required to engage with them thins. Procrastination, self-doubt, and a general withdrawal from decisions are common responses, with the brain essentially rationing what little capacity remains.
Cognitive symptoms follow. Concentration narrows. Judgement becomes less reliable. Small errors accumulate. People in this state often describe feeling mentally stuck, present in the room but unable to engage with any clarity or momentum.
The physical dimension is frequently overlooked. Headaches, low energy, disrupted sleep, and difficulty sustaining attention are all associated with sustained decision overload. These symptoms register what prolonged mental strain produces in the body and are worth taking seriously.

Who is most at risk?
Decision fatigue affects most people at some point, but the load is not evenly distributed. Professionals in high-responsibility roles, caregivers, and anyone managing multiple competing demands make a disproportionately high number of decisions each day. By the end of a long day, the quality of choices made about food, purchases, relationships, or work often reflects exhaustion more than intention.
Read more: Smartphone Overuse Linked To Rising Risk Of Eating Disorders Among Youth, Study Finds
Is there a solution?
Reducing the number of decisions that require active thought each day is the most direct intervention. Fixed routines for meals, schedules, and recurring tasks remove the need to deliberate repeatedly over the same ground. This is conservation of mental energy, and it compounds over time.
Important decisions are better made earlier in the day, when the brain is rested and cognitive resources are intact. Short breaks during sustained work periods allow partial recovery. Even brief physical activity or deliberate rest between decision-heavy tasks restores some capacity.
The brain has a finite decision-making budget each day. Spending it on low-stakes choices leaves less available for the ones that carry real consequence.
Over 30% Fever Cases In India Linked To Dengue, Typhoid: Report
Credit: iStock
While fevers are often overlooked and brushed aside or even managed with antibiotics — a dangerous trend — an alarmingly nationwide study linked it to infectious diseases with far-reaching consequences.
The report, based on data of over one lakh individuals in India with fever, between 2023 and 2025, showed that these were not vague or self-limiting, but in more than 30 percent or one-third cases had clear links to serious infections, such as dengue, and typhoid.
According to the report by healthcare diagnostics company Thyrocare, the fevers were mostly linked with
- typhoid – in over 18 percent cases
- dengue -- over 14 percent cases.
- Other diseases include malaria, chikungunya, and leptospirosis.
Presence Of Multiple Infections
Importantly, the findings highlighted the presence of co-infections in 10 per cent cases. The most common was a combination of dengue and typhoid.
Dr Preet Kaur, Chief Scientific Officer, Thyrocare, said that a significant number of patients carry serious infections, sometimes more than one at a time, revealing patterns that simple assumptions cannot capture.
"Beyond the visible rise in temperature, laboratory markers highlight hidden stress on organs, from drops in platelet counts to elevated liver enzymes, underscoring that fever is a systemic signal, not an isolated event," she added.
Also read: ‘Breakbone Fever’: US CDC Warns Of Dengue Surge Across 17 Countries
Further, the report noted that dengue positivity declined significantly over the three-year report period, malaria increased despite its lower overall base.
Typhoid and chikungunya rose in 2024 before easing in 2025 but remained present across the testing population.
Also read: Drug Resistance Driving Severe Typhoid Disease, Death Among Children Under-5s in India: Lancet Study
Fever: Men Vs Women
The report noted that more women were affected with typhoid than men. On the contrary, men reported more malaria cases.
More than 32 percent of females had fevers compared to 29 percent of men. Fevers in women was largely driven by higher typhoid detection (21 percent vs 15 percent).
Malaria affected men more than twice as often as women (1.1 percent vs 0.5 percent).
The lab reports also revealed key physiological markers such as platelet counts and liver function among people with fever, dengue, and malaria.
Low platelet levels were seen in
- 27 percent of patients with fever
- 80 percent malaria positive patients
- 37 percent dengue-positive patients
- All fever patients (56 percent) showed elevated SGOT levels and 37 percent SGPT
- Liver stress was seen across patients with dengue, malaria and leptospirosis.
Dengue cases rose throughout the year and typically peaked around October.
Typhoid positivity steadily fell from 2023 to its lowest in 2025. Despite a mild monsoon spike each year, 2025 remained consistently lower overall.
Chikungunya cases rose gradually from lower, volatile levels in 2023, peaked sharply in 2024, and moderated to a softer trend in 2025.
Malaria positivity remained relatively low overall but increased during the monsoon months, with transmission peaking between May and September.
Over the three-year period, malaria positivity rose from 0.5 percent to 1.1 percent, indicating a gradual increase despite its lower overall base.
© 2024 Bennett, Coleman & Company Limited

