- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
This Year, Doctor's Day Reminded That Doctors Too Are Humans And Can Get Emotionally Exhausted
Credits: Canva
This year's Doctor's Day was a reminder to all that doctor's too are human. The theme specifically focused on healing the healers, emphasizing on the need for people to recognize doctor's struggle and treat them with empathy and sympathy.
No Lines Between Personal And Professional Life
Health and Me had earlier reported on how doctors, even when they are not at work receive work questions all the time. In a previous interview with Health and Me, Dr Guru N Reddy, a senior gastroenterologist, shared, “I didn’t spend time with my family when my kids were growing up. My work always came first and then came my family.” He also shared that how whenever he is gone for a gathering, it turns into an unofficial consultation desk. “Can I quickly show you this report?” “There’s this pain that won’t go, can you suggest something?” These are the questions he is faced with even at family events.
All such scenarios will undoubtedly make a doctor feel overwhelmed. In fact, a survey conducted by Medtalks, a doctor engagement platform, revealed that doctors are burdened by growing mental and emotional burden.
Also Read: Healthier Popcorn Alternatives You Can Try For Your July 4 Movie Nights
The survey, though small scale, conducted among 200 doctors across public and private health care, revealed an important issue. It found that 74% of respondents felt emotionally exhausted on a weekly or even on a daily basis. This survey also highlighted the depth of burnout and chronic stress in the medical profession.
Many doctors also agreed that even after their work hours, they were still entertained with questions related to their patients health through WhatsApp. The data revealed that over 83% of doctors felt that they were under constant stress as their patients continued to contact them through WhatsApp, phone calls, and digital messages, with many asking them for urgent queries. This round-the-check communication has blurred personal and professional boundaries, which has disassociated doctors from their own families.
Also Read: Measles Outbreak Update: Kentucky Confirms Its First Case
Looming Fear Of Threat And Violence On Doctors
The survey also found that threat and violence against doctors were a major source of stress and concern. Indian Medical Association (IMA) President, Dr Dilip Bhanushali, in an earlier interview with Health and Me had said, "Violence against doctors is not rare—it’s routine."
He further added: “We’ve seen mobs arrive with kerosene, petrol, even swords, burning down hospitals. There was a law during COVID promising seven years imprisonment and non-bailable warrants for attacks on doctors, but it hasn’t been enforced. Most states still have weak three-year, bailable punishments.”
He also pointed towards the RG Kar Medical College’s case where a female postgraduate trainee doctor was raped and murdered and her body was found in a seminar room on campus. Doctors across the nation went on a strike, demanding justice. “But we cannot go to the roads and do strikes every time. Despite it all, we uphold our Hippocratic oath.”
The survey too echoed the same feelings, where many respondents admitted that this fear has directly influenced their approach to diagnosis, communication, and decision-making. Doctors are now acting more defensively.
The strain on doctors is intensified by mounting administrative duties, fear of legal action, limited institutional support, and rising expectations to deliver flawless outcomes.
Over one-third of doctors reported working more than 60 hours a week, while only 17 percent are able to take a full, uninterrupted day off on a regular basis. Most respondents said they receive minimal support in coping with these demands. Strikingly, just 14 percent felt the current healthcare system allows them to prioritise their own wellbeing, whereas 52 percent said it does not.
Why India’s Cardiac Protocols Are Built Around Male Bodies — And What That Means for Women
Credit: iStock
Heart diseases are viewed as a universal health concern, and advancements in cardiology have hugely improved diagnosis and treatment outcomes around the world. At the same time, emerging research is shedding more light on how cardiovascular disease affects women.
In India, this perspective is especially important. Of the more than 10 million deaths recorded annually in the country, nearly two million are attributed to diseases of the circulatory system, with women accounting for about 40% of these cases. Significantly, more than half of the nearly 800,000 cardiovascular deaths among Indian women each year occur prematurely, underscoring the importance of greater awareness, early detection, and timely medical care.
How Cardiac Research Has Evolved
It is evident that modern cardiology has been shaped by the findings from large, well-characterized populations of patients. The frameworks that have been established from such findings are the ones that guide the approaches that are currently used in the diagnosis and treatment of various forms of heart disease.
Such frameworks have been instrumental in the advancement of the management of various forms of cardiovascular diseases worldwide. As the research expands to include larger populations, there is an increased understanding that the manifestation of cardiovascular diseases differs from one group to another, particularly in females.
Recognizing Differences In Symptoms
This growing awareness is particularly useful in recognizing symptoms. Although women, like men, may experience chest pain as a symptom of a heart attack, there are other, less common symptoms that women may also experience.
These include fatigue, shortness of breath, nausea, dizziness, as well as neck, jaw, or back discomfort. The awareness of these symptoms will allow women to seek treatment sooner, as well as help healthcare providers better understand their symptoms.
The Role of Life Stages in Women’s Heart Health
Women’s heart health is influenced by various life stages and the hormonal changes that accompany them. For instance, after menopause, estrogen levels decline, and since this hormone offers some protective benefits for the heart, the risk of developing heart disease may gradually rise.
Certain pregnancy-related conditions, including gestational diabetes, preeclampsia, and high blood pressure during pregnancy, may also indicate a greater likelihood of cardiovascular disease later in life. Recognising these factors allows doctors to monitor heart health more closely and recommend preventive measures that support long-term wellbeing.
Strengthening Prevention And Early Detection
Prevention continues to be one of the most effective strategies for reducing heart disease. Regular health check-ups, along with monitoring blood pressure, cholesterol, and blood sugar, are essential for lowering cardiovascular risk. Adopting healthy lifestyle habits further supports long-term heart health. Awareness is equally important.
Symptoms such as fatigue or breathlessness are not always immediately linked to heart disease, particularly among women. Raising awareness about heart health can help people recognize early warning signs sooner and seek timely care.
Moving Toward More Inclusive Cardiac Care
Encouragingly, the field of cardiology is constantly evolving with the help of emerging research that is further enlightening us about the health of the heart in both men and women. With more women being included in research and better developments in diagnostic procedures, healthcare professionals are refining their strategies to deal with heart health.
Thus, by adopting the best strategies and emerging research about the health of women’s hearts, awareness and early intervention are the keys to better outcomes and reduced risks among women in India.
Physical Inactivity Due To Climate Change To Lead To 700,000 Additional Deaths By 2050: The Lancet

Credit: iStock
Physical activity is a known factor for better physical and mental well-being. However, imagine severe heat forcing you to remain indoors and not being able to just walk around your neighborhood.
The new study published in the journal The Lancet Global Health predicts that by 2050, the rising temperatures are likely to stop people from being active.
It showed that lack of physical activity, especially for people unable to access gyms, will lead to an estimated 700,000 additional premature deaths.
It is also projected to cause $2.59 billion in annual productivity losses.
“Rising temperatures are projected to increase the prevalence of physical inactivity, translating into additional premature deaths and productivity losses, especially in tropical regions,” said a team of Latin American researchers, led by Pontifical Catholic University of Argentina.
The latest report comes amid climate scientists from the UN Intergovernmental Panel on Climate Change warning of a warmer climate -- between 2.7 and 3.1 degrees Celsius by 2100.
In addition, physical inactivity is already a major global health problem, with about one in three adults failing to meet World Health Organization guidelines for weekly exercise.
Deaths Due To Climate Change
The study models how rising temperatures may affect physical activity globally up to the year 2050 based on an analysis of data from 156 countries between 2000 and 2022.
It suggests that by 2050, an average temperature above 27.8°C per month would increase physical inactivity by
- 1.5 percentage points globally
- 1.85 percentage points in low- and middle-income countries
- No clear impact in high-income countries
“This translates to a predicted 0.47–0.70 million additional premature deaths annually and $2.40–3.68 billion in productivity losses,” the researchers said.
The biggest increase in inactivity will be in hotter regions such as
- Central America,
- the Caribbean,
- Eastern Sub-Saharan Africa,
- Equatorial Southeast Asia
Heat can discourage the most common exercise regimen – walks, lead author Christian Garcia-Witulski, Professor at the Pontifical Catholic University, was quoted as saying to The Washington Post.
“The real-world picture is usually not that people suddenly stop moving altogether. It is that heat that gradually erodes the safe, comfortable, and practical opportunities people have to stay active in everyday life,” Garcia-Witulski said.
Physical Inactivity - A Silent Global Crisis
Regular physical activity promotes both mental and physical health in people of all ages. The WHO advises at least 150 minutes of moderate or 75 minutes of vigorous exercise weekly, alongside regular muscle-strengthening activities.
As per the Global Status Report on Physical Activity 2022, more than 80 percent of adolescents and 27 percent of adults do not meet the WHO’s recommended levels of physical activity.
The UN health body also aims to achieve the global target of a 15 percent relative reduction in the prevalence of physical inactivity by 2030.
The WHO recommends that countries increase levels of physical activitywithin their populations by developing and implementing dedicated comprehensive national policies to ensure safer roads for cycling and walking, accessible opportunities for active recreation where people live, work, and play, and promoting physical activity.
The Lancet researchers called for
- action to protect the public from rising heat,
- design cooler cities,
- provide affordable air-conditioned places to exercise,
- clear advice on how to stay safe in extreme heat,
- reduce greenhouse gas emissions.
Meningitis Outbreak: How to Differentiate The Symptoms From a Common Rash
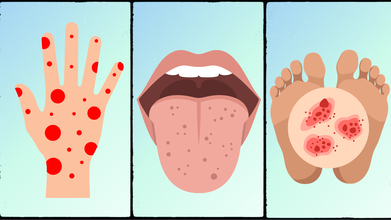
Credits: Canva
Meningitis outbreak has led to authorities in the UK to urge students to get vaccines and antibiotics. Health and Me also reported on the menB vaccine that students 5,000 students in Kent University will be receiving. One of the common symptoms are rashes, however, how does one know if it is a meningitis rash?
How Do You Recognize Meningitis Rash?
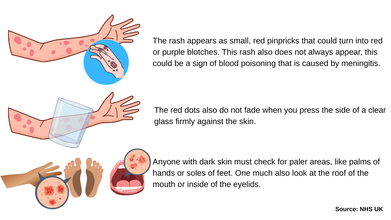
As per NHS UK, the rash appears as small, red pinpricks that could turn into red or purple blotches. This rash also does not always appear, this could be a sign of blood poisoning that is caused by meningitis.
The red dots also do not fade when you press the side of a clear glass firmly against the skin. NHS UK notes that anyone with dark skin must check for paler areas, like palms of hands or soles of feet. One much also look at the roof of the mouth or inside of the eyelids.
NHS UK notes that one must call 999, if they find such a rash.
Meningitis Outbreak UK: What Is Happening Now?
A meningitis outbreak in Kent University is now treated as a national incident, after two people have died, one of them being the student of the university. Students have been urged to get vaccines and take antibiotics as health officials are dealing with the "unprecedented" and "explosive" outbreak.
As per the UK Health Security Agency (UKHSA), 15 cases have been reported and all of them have lead to hospital admission. Cases are also expected to rise due to the incubation period of infection to when the symptoms start to appear. The incubation period is from two to 14 days.
As per experts, many of whom are affected had attended Club Chemistry in Cantebury between 5 to 7 March. UKHSA chief executive Susan Hopkins said the outbreak "looks like a super-spreader" event with "ongoing spread" through universities' halls of residence. She added: "There will have been some parties particularly around this, so there will have been lots of social mixing. I can't yet say where the initial infection came from, how it's got into this cohort, and why it's created such an explosive amount of infections."
She further said that in her 35 years working in medicine, healthcare, and hospitals, "This is the most cases I've ever seen in a single weekend with this type of infection". She added: "It is the explosive nature that is unprecedented here - the number of cases in such a short space of time." She also remarked that this was the "quickest-growing outbreak" she has ever seen in her career.
Who Should Get MenB Vaccine?
As per the University of Oxford, MenB vaccine is given to babies at 8 weeks, 16 weeks, and one year of age.
General Practitioner surgery or clinic also send an appointment for babies to have their MenB vaccination along with their other routine vaccinations.
Read: Meningitis Outbreak: What Is MenB Vaccine?
Additional doses of the vaccine are recommended for people with some long-term health conditions who are at greater risk of more severe meningococcal disease. This includes people with:
- asplenia or splenic dysfunction (a spleen that is missing or does not work properly)
- sickle cell anaemia
- coeliac disease
- complement disorders (the complement system is an important part of the immune system, and disorders of this system can increase a person’s risk to some diseases.)
© 2024 Bennett, Coleman & Company Limited

