- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
US Is 'Burdened By Disease', Reveals Study

US Is 'Burdened By Disease', Reveals Study (credits: Canva)
In a recent study, it was revealed that the US has the longest 'healthspan-lifespan gap' among more than 180 countries. Over all, the global life expectancy has seen an increase by 6.5 years, and hit an average of 72.5 among the 183 members of the World Health Organization. This data is reported in the journal JAMA Network Open. However, during the same period, the estimate for how long a person could live free of diseases or disability increased only by 5.4 years, with an average of 63.3 years among the WHO countries.
This has led to a 13% increase in the global gap between lifespan and healthspan, which is reflected by "the extent of lifespan burdened by disease". The gap is from 8.5 years in 2000 to 9.6 years in 2019, states the study.
Dr Andre Terzic, the co-author of the study and the Marriot family director of comprehensive cardiac regenerative medicine for the Mayo Clinic's Center for Regenerative Biotherapeutics, said, "On one hand we celebrate the fact that humanity lives longer. Whether you’re in North America or in the rest of the world, you look into the last century and it’s amazing how mankind lives longer and continues to live longer."
“Unfortunately, the gains in life expectancy are not matched with equivalent gains in health life expectancy," explains the doctor.
How healthy is US?
Among all the WHO countries, US had the greatest disparity between life expectancy and years lived without disease or disability.
On an average, the life expectancy in the US rose from 79.2 years to 80.7 years in women and for men, it went from 74.1 years to 76.3 years between 2000 and 2019. Which means, on an average, a person living in the US' total life expectancy would be 78.5 years, whereas the healthy life expectancy is only at 66.1 years. The gap between lifespan and healthspan has therefor increased from 10.9 years earlier to 12.4 years, now. This has led to a disparity of 29%, larger than the global average, which is at 13%.
“That’s a significant departure of what could be expected for a country with such a significant expansion of life expectancy,” Terzic says. Another point of concern is that the study also showed that women in US exhibited a 2.6-year higher healthspan-lifespan gap than men, increasing from 12.2 to 13.7 years or 32% beyond the global mean for women.
As per Terzic, the widening gap between healthspan and lifespan in the US is due to the severe burden of chronic diseases, especially musculoskeletal conditions, mental health and substance use disorders.
ALSO READ: These Are The 5 Best And Worst US States For Mental Health Care
In a different study conducted by the Commonwealth Fund that analyzed the 11 high-income nations found that the US had the highest percentage of adults who reported receiving mental health diagnosis such as anxiety or depression at 23%.
This was based on a 2016 survey data. Of the people survey, it was also found that 26% of US adults said they had experienced emotional distress, and thus it has marked it as the second-highest rate among countries.
Lupita Nyong’o Opens Up About Fibroids Returning, Doubling 12 Years After Surgery

Credit: Instagram
Kenyan-Mexican actress Lupita Nyong’o has revealed that her fibroids have returned after undergoing surgery in 2014 -- now doubling up to 50, raising awareness about the often-overlooked health condition in women.
Speaking at the Today show, the Oscar-winning star Nyong’o said that she was first diagnosed with fibroids, a noncancerous tumor -- about 30 in number -- in 2014.
The growths made of muscle and tissue were removed with myomectomy, the fibroid-removal surgery.
However, the fibroids came back after over a decade, with the largest being the size of an orange, Nyong’o said.
She noted that the doubled-up fibroids are causing her more pain, while her treatment options remain largely the same.
“The first time I got the fibroids taken out, they took out 23,” she said on the show. “And this time, I’ve been informed two years ago that I have over 50.”
“And I’m being faced with the same options,” she added. “Surgery or live with the pain.”
Even as she is contemplating her treatment options, the A Quiet Place: Day One star opened up about feeling left alone and scared for her reproductive health during the initial phase.
She is now speaking out and connecting with other women suffering like her. Nyong’o is also advocating and raising money for scientists to research less invasive and non-invasive treatment methods for fibroids.
I was told that fibroids were something women live with. In refuse to accept that. Millions of women are suffering in silence, and we deserve better answers, better care and better options," Nyong’o wrote in a post on Instagram.
What Are Fibroids
Uterine fibroids are noncancerous growths that form inside or on the uterus. They are very common, affecting an estimated 40 to 80 percent of people with a uterus between the ages of 30 and 50.
In some cases, fibroids do not cause any noticeable symptoms, which means many people may not realize they have them. However, when symptoms are present, they often include:
- Heavy menstrual bleeding or painful periods
- Longer or more frequent periods
- Pelvic pressure or pain
- Frequent urination or trouble urinating
- Growing stomach area
- Constipation
- Pain in the stomach area or lower back, or pain during sex
Obesity and a higher body mass index (BMI) are the most common risk factors that can increase the chances of developing fibroids. Others include family history, not having children, early onset of menstruation (getting your period at a young age), and late age of menopause.
How To Treat Fibroids? Can They Recur?
There are several tests that can be done to confirm fibroids and determine their size and location.
These tests can include ultrasonography, magnetic resonance imaging (MRI), computed tomography (CT) scan, hysteroscopy, and laparoscopy.
Myomectomy is a commonly used surgical procedure to remove fibroids. There are several types of myomectomy, and they are used depending on the location of the fibroids, their size, and number.
The types of myomectomy procedures include hysteroscopy, laparoscopy, laparotomy, hysterectomy, uterine fibroid embolization, and radiofrequency ablation (RFA).
Even after a successful myomectomy, new fibroids can still develop. The recurrence risk is more common among young adults (under age 40) with many fibroids. The risk is less among people near menopause or with few fibroids.
Visit your doctor if you have:
- Pelvic pain that doesn't go away
- Heavy or painful periods that limit what you can do
- Spotting or bleeding between periods
- Trouble emptying your bladder
- Ongoing tiredness and weakness, which can be symptoms of anemia, meaning a low level of red blood cells.
Unique Symptoms Of Sepsis: What To Know About TIME
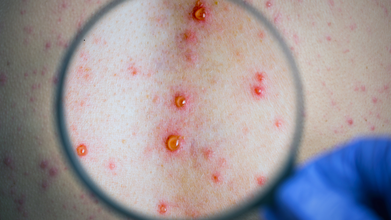
Credits: Canva
Sepsis that happened by a lick from a pet dog led to a woman losing all four of her limbs. Health and Me had previously reported that a Birmingham based woman, 56-year-old pharmacy worker Manjit Sangha caught sepsis from the lick of her pet dog. She spent her night in coma in the hospital and had to lose all her limbs. This happened because bacteria from dog's lick entered her body through a cut or a scratch. This led to sepsis, where the immune system's reaction to infection damaged the body's own tissues and organs.
This has brought a lot of attention on what sepsis is and what are the symptoms one must be aware of. As per the Sepsis Alliance, one must know about TIME to be aware of sepsis.
Unique Symptoms of Sepsis
TIME stands for temperature, infection, mental decline and extremely ill. If you notice these symptoms, rush to the hospital.
- T for Temperature: If you notice your body temperature rising or falling
- I for Infection: If you see signs or symptoms of any infection
- M for Mental Decline: If you feel confused, sleepy and difficult in rising
- E for Extremely Ill: If you feel severe pain, discomfort, shortness of breath
Unique Symptoms Of Sepsis: What To Know About Temperature
Your body temperature normally stays steady at about 98.6°F (37°C), with small changes based on activity, surroundings, and time of day. A reading of 100°F (37.7°C) or higher is considered a fever. During infection, the body often heats up to help fight germs. However, some people experience an unusual drop in temperature instead. Because of this, both a spike and a fall in temperature can be warning signs of sepsis.
Unique Symptoms of Sepsis: How To Know If You Have An Infection?
When an infection stays in one area, its symptoms usually match the site involved. A urinary tract infection may cause burning while urinating or frequent urges, pneumonia can bring cough and chest pain, and an infected cut may show redness or pus.
If the infection spreads through the body, broader symptoms like fever, tiredness, and body aches can appear. In some cases, an infection may not cause obvious symptoms at all. This is especially important to remember after surgery, medical procedures, skin injuries, or close contact with someone who is sick.
Unique Symptoms of Sepsis: What To Look Out For Mental Decline?
Sepsis can also alter how the brain functions. Some people, particularly older adults, may not develop the usual infection symptoms. Instead, they might suddenly become confused or show a sharp worsening of existing dementia. Marked drowsiness or unusual sleepiness is another common sign.
Unique Symptoms of Sepsis: Signs That You Are Extremely Ill
Many sepsis survivors recall feeling sicker than ever before. They describe overwhelming symptoms such as the most severe sore throat or abdominal pain they had experienced, along with a frightening sense that they might not survive.
Unique Symptoms Of Sepsis In Children
| A Child Who | Child under 5 (Infant) Who |
| Feels abnormally cold to touch | Is not eating |
| Looks mottled, bluish or has very pale skin | Is vomiting repeatedly |
| Has a rash that does not fade when you press it | Has not urinated in 12 hours |
| Is breathing very fast | |
| Has a convulsion | |
| Is very lethargic or is facing difficulty in waking up |
Unique Symptoms Of Sepsis In Adults
- High blood cell count
- Immature white blood cells in circulation
- Elevated plasma C-reactive protein
- Elevated procalctonin (PCT)
- Low blood pressue
- Low central venous or mixed venous oxygen saturation
- High cardiac index
- Low oxygen level
- Low urine output
- High creatinine in the blood
- Coagulation or clotting abnormalities
- Absent bowel sounds
- Low platelets in blood
- High bilirubin levels
- High lactate in blood
- Decreased capillary filling or mottling
Woman Lost Weight On Mounjaro But Her Breasts Didn't Stop Growing, This Is Why...

Credits: SWNS (Tianna Moon)
Mounjaro, a popular weight loss drug that helped many lose weight, however, in this one case, a woman, who was on the same drug noticed something different. While she lost weight, she noticed that her breasts continued to grow. The 30-year-old Tianna Moon of East Anglia, a region in eastern England first realized something was not normal with her chest in 2024. This was when she started to use Mounjaro.
She was losing weight, but her breasts continued to grow. This is when Moon's doctor diagnosed her with a rare disease call gigantomastia, which causes breast tissue to grow rapidly and in excess.
Also Read: 15 States Sue Trump Administration Over Revised Vaccine Schedule
Woman Lost Weight On Mounjaro But Her Breasts Didn't Stop Growing: What Happened To Her?
Moon said that the doctors had thought that she had macromastia, a less severe, however, a similar condition. "But when I broke down medical history, the weight loss on Mounjaro and the increased growth and side effects, he was point-blank like, 'This is gigantomastia'," she said.
Moon also told that her breasts currently weight 39 lbs, which is approximately 20 per cent of her overall body weight.
Moon also said that while her large breasts are "normal" at this point in her life, she said the rare condition still comes with challenges.
"The side effects are having numb arms quite a lot and having quite severe indentations on my shoulders. I have some light scarring under my breasts where bras have rubbed and ripped the skin open."
She also said that laying on her back is something she cannot do for a long time, as it restricts the amount of airflow she can get in. She also said that when she goes out she tries to make her breasts look smaller than they are and strap them up. "I [still] get stares and double takes."
Also Read: Wegovy And Ozempic Will Cost Less In 2027, Novo Nordisk Slashes Weight Loss Drugs Prices By Half
Woman Lost Weight On Mounjaro But Her Breasts Didn't Stop Growing: What Is Gigantomastia?
As per Cleveland Clinic, it is a rare condition where your breasts become excessively large. It can also cause pain, infection, discomfort and issues with body image. It is also known as breast hypertrophy where one experiences rapid and disproportionate breast growth. The speed with which the breasts grow could vary depending on the person. It could take a few weeks to over several years. The tissue is almost never benign.
Gigantomastia is characterized by:
- Breasts that have an excess of at least 5 pounds of breast tissue.
- Extra breast tissue that equals more than 3% of your total body weight.
There are different types of gigastomastia:
- Juvenile gigantomastia: This type happens during puberty.
- Gestational gigantomastia: This is when gigantomastia occurs during pregnancy.
- Drug-induced gigantomastia (or medication-induced): This happens after taking certain drugs.
- Idiopathic gigantomastia: This is when the cause of gigantomastia is unknown or can't be determined. Idiopathic gigantomastia is the most common type.
Moon is now considering a breast reduction surgery. She has for now set up an account on OnlyFans. “I might as well try and reap the benefits of my medical condition rather than the negatives," she said.
© 2024 Bennett, Coleman & Company Limited

