- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Watch: What Really Happens When You Skip The Measles Vaccination?
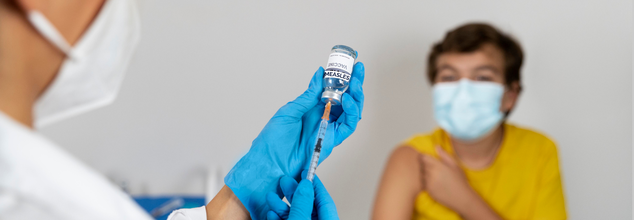
Credits: Freepik
Measles, a virus that was once officially eradicated in the United States in 2000, is making a shocking comeback — this time with more sinister layers than ever before. More than 1,000 measles cases have been confirmed across the United States in 2025, a saddening milestone of the nation's struggle with a disease it was officially announced as eliminated as far back as the year 2000. State and regional health agencies along with the Centers for Disease Control and Prevention report at least 1,002 cases so far this year—an astonishing number putting 2025 on pace to equal 2019, which was the century's worst measles year to date.
In a hard to watch medical video released by neurologists in India of a once-healthy 4-year-old boy lies on a hospital bed, eyes darting wildly, limbs convulsing, and lips foaming as his tiny body fights a losing battle against a preventable disease. The footage—published in JAMA Neurology offers more than a glimpse into one family’s nightmare. It is a sobering wake-up call for the world: measles is not just a childhood illness with a fever and rash. Left unchecked, it can be a silent predator that devastates the brain and kills with merciless precision.
The child in the video suffers from Subacute Sclerosing Panencephalitis (SSPE), a rare but invariably fatal neurological complication that follows a measles infection. His case serves as a dire warning about the consequences of skipping the measles, mumps, and rubella (MMR) vaccine—a message particularly urgent amid falling vaccination rates and surging outbreaks globally.
What is SSPE?
SSPE is a progressive, degenerative brain disorder caused by a persistent infection with a mutated measles virus. What makes SSPE especially cruel is its latency. The virus often lurks undetected in the brain for years after a seemingly mild infection before it begins destroying neurons, causing inflammation, and forming lethal lesions.
In this child’s case, his decline started with subtle symptoms—jerky limb movements, unsteadiness, and cognitive changes over six months. His parents, unaware of a previous measles infection and unable to recall any characteristic rash or fever, never had him vaccinated. It was only after his condition worsened—marked by erratic, swirling eye movements known as opsoclonus—that neurologists diagnosed SSPE.
Despite aggressive treatment with antivirals and anticonvulsants, his fate is tragically sealed. SSPE is almost always fatal, and no curative therapy exists.
What is Measles and Why Is It A Dangerous Condition?
Measles is often underestimated, dismissed by many as a benign childhood disease. But data tells a far more troubling story. A typical measles infection causes high fever, cough, runny nose, and a characteristic red rash. However, about 20% of infected children in the U.S. will be hospitalized, with complications ranging from pneumonia to diarrhea and severe ear infections that can cause permanent hearing loss.
One in 1,000 will develop encephalitis (brain inflammation), and up to three in 1,000 will die due to respiratory or neurological complications. Long after the acute phase ends, measles continues to sabotage the immune system through "immune amnesia"—a condition where the body forgets how to defend against other pathogens, leaving children vulnerable to secondary infections for up to three years.
And then there's SSPE. Though rare—with 11 cases per 100,000 measles infections on average—the risk significantly increases in children infected before age five. For them, the rate is 18 per 100,000, with symptoms surfacing seven to ten years post-infection.
The boy’s case stood out for an unusual symptom: opsoclonus—rapid, multidirectional eye movements typically associated with paraneoplastic brain syndromes or severe brain inflammation. This is believed to be the first case of SSPE captured on video with this specific presentation. Medical experts believe these movements may result from the destruction of specialized neurons like Purkinje and omnipause cells, which are critical for coordinated eye and body movement.
The presence of opsoclonus in SSPE not only expands clinical understanding of the condition but also underlines its neurological complexity—and the helplessness of medical interventions once the disease takes hold.
Is this Measles Outbreak Exacerbated by Misinformation and Complacency?
Globally, measles cases are climbing again. After decades of progress, the COVID-19 pandemic disrupted routine immunizations, and anti-vaccine rhetoric has flourished in its wake. In the United States, measles outbreaks are at their highest in over 25 years, and several communities have immunization rates far below the 95% threshold needed for herd immunity.
The situation is compounded by influential figures like Robert F. Kennedy Jr., who continue to promote vaccine skepticism, undermining public health messaging and placing children at direct risk.
Public health experts warn that if these trends continue, measles could once again become endemic in the United States—a devastating reversal of years of progress.
Why Measles Vaccination is the Only Defence?
The MMR vaccine is one of the most rigorously tested and safest vaccines available. Two doses provide 97% protection against measles. Side effects are typically mild—such as fever or a sore arm—and serious adverse effects are extremely rare.
Before the vaccine’s introduction in 1963, measles caused hundreds of deaths annually in the U.S. Now, thanks to widespread immunization, those numbers have dropped dramatically. However, as vaccination rates fall, we risk reliving the past—one preventable death at a time.
What To Do if You're Exposed to Measles?
If you suspect you've been exposed to measles, especially if you or your child are unvaccinated:
- Isolate immediately and wear a mask to reduce the risk of transmission.
- Contact your healthcare provider to assess the need for post-exposure prophylaxis—either a dose of the MMR vaccine or immune globulin.
- Do not visit healthcare facilities without calling ahead to avoid exposing others.
- If you're fully vaccinated, remain vigilant for symptoms for at least 21 days post-exposure, and notify your doctor at the first sign of illness.
Vaccination isn't just a personal choice; it's a societal responsibility. The consequences of inaction are too devastating to ignore—not just for one family, but for entire communities. The heartbreaking video of the 4-year-old boy is more than a clinical case study—it’s a call to action.
Mel Schilling Dies At 54, Her Colon Cancer Spread To Her Brain

Credits: Instagram
Mel Schilling, an Australian psychologist and a dating expert died at 54. Her husband Gareth Brisbane announced the death in a social media statement.
What Happened To Mel Schilling?
Schilling was diagnosed with colon cancer in December 2023. Just two weeks ago she said that the disease had spread to her brain. "I honestly don't know how long I have left," she wrote.
Read: What Is The Correct Age To Get A Colonoscopy?
According to her husband, she died "peacefully, surrounded by love". “This is a woman who, through two years of chemotherapy, when she could barely lift her head from the pillow, never complained and never stopped showing courage, grace, compassion and empathy, and never missed a day of filming,” Brisbane wrote.
She was also an expert on 'Married at First Sight Australia' for 12 years and because of her illness she stepped down as a dating expert.
How Does Cancer Spread To Other Parts Of The Body?
Schilling said that her cancer had spread to her brain. as per the Cancer Research UK, cancer cells can spread to other parts of the body through bloodstream or lymphatic system. They can then start to grow into new tumors. The National cancer Institute notes that cancer cells spread through the body in a series of steps, which include:
- growing into, or invading, nearby normal tissue
- moving through the walls of nearby lymph nodes or blood vessels
- traveling through the lymphatic system and bloodstream to other parts of the body
- stopping in small blood vessels at a distant location, invading the blood vessel walls, and moving into the surrounding tissue
- growing in this tissue until a tiny tumor forms
- causing new blood vessels to grow, which creates a blood supply that allows the metastatic tumor to continue growing
What Is Colon Cancer?
Colon (colorectal) cancer begins when small growths called polyps form on the inner lining of the colon or rectum. Over time, changes in the DNA of these cells can cause the polyps to become cancerous.
As abnormal cells multiply, they replace healthy cells and eventually form a mass known as a tumor. This process develops slowly, often taking up to ten years for a precancerous polyp to turn into cancer and begin showing symptoms.
Colon cancer poses serious health risks because cancerous cells can invade healthy tissues. Over time, they may break away and spread to other parts of the body, making detection more difficult since the symptoms can resemble other conditions.
How Can You Get Screened For Colon Cancer?
You can get examined by a colonoscopy. A colonoscopy is a 15 to 60 minute medical procedure that is used to examine the entire inner lining of the large intestine, which includes rectum and colon for abnormalities, such as polyps, inflammation, or cancer. A doctor uses a colonoscope, which is a thin, flexible tube with a camera to take images, remove polyps, or take issue samples.
Most health experts, including federal guidelines and the American Cancer Society, recommend that people at average risk for colorectal cancer start screening at age 45. This usually means getting a colonoscopy once every 10 years, or opting for stool-based tests every one to three years. These guidelines also play a role in whether insurance companies cover the tests.
What Is The Correct Age To Get A Colonoscopy?

March is the month of colon cancer awareness and with the recent cases of colon cancer patients who are younger than 50. With the death of 48-year-old actor James Van Der Beek due to colorectal cancer, concerns are rising. While cancer death rates overall in people younger than 50may have dropped by 44% since 1990, colorectal cancer has become the leading cause of cancer death in people under 50.
Can Karlyle Morris, section chief for colorectal cancer at MD Anderson Center in Houston tells NBC News, "We anticipate that this is going to be a continued trend."
What Is Colon Cancer?
Colon (colorectal) cancer begins when small growths called polyps form on the inner lining of the colon or rectum. Over time, changes in the DNA of these cells can cause the polyps to become cancerous.
As abnormal cells multiply, they replace healthy cells and eventually form a mass known as a tumor. This process develops slowly, often taking up to ten years for a precancerous polyp to turn into cancer and begin showing symptoms.
Colon cancer poses serious health risks because cancerous cells can invade healthy tissues. Over time, they may break away and spread to other parts of the body, making detection more difficult since the symptoms can resemble other conditions.
What Is The Right Age To Get Colonoscopy?
A colonoscopy is a 15 to 60 minute medical procedure that is used to examine the entire inner lining of the large intestine, which includes rectum and colon for abnormalities, such as polyps, inflammation, or cancer. A doctor uses a colonoscope, which is a thin, flexible tube with a camera to take images, remove polyps, or take issue samples.
Most health experts, including federal guidelines and the American Cancer Society, recommend that people at average risk for colorectal cancer start screening at age 45. This usually means getting a colonoscopy once every 10 years, or opting for stool-based tests every one to three years. These guidelines also play a role in whether insurance companies cover the tests.
Even so, most cases of colon cancer are still diagnosed in people over 50. What’s worrying, though, is the steady rise in cases among younger adults in their 20s, 30s and 40s over the past few decades.
Why Does Screening Begin At 45?
Colon cancer typically develops slowly. It often starts as small growths in the colon called polyps, which can eventually turn cancerous if not detected early.
In recent years, growing evidence has pushed experts to reconsider when screening should begin. In 2021, the U.S. Preventive Services Task Force lowered the recommended screening age from 50 to 45. The American Cancer Society had already made a similar recommendation back in 2018.
At the time, the change was not universally accepted. Some in the medical community felt 45 was still too young. Even today, there is ongoing debate.
Setting screening guidelines is not as simple as picking an age. Experts have to weigh the benefits of early detection against potential downsides, including costs, risks from procedures and even practical concerns like taking time off work.
The numbers also tell an important story. For people aged 40 to 44, the risk of colorectal cancer is about 21 cases per 100,000 individuals. That risk more than doubles to 47 per 100,000 between ages 45 and 49, which is one of the reasons screening begins at that point.
Still, younger adults account for a relatively small proportion of cases overall. According to the Mayo Clinic, about 10 percent of colorectal cancer cases occur in people under 50.
The Challenge Of Resources And Awareness
Another key factor is access. There are only so many specialists available to perform colonoscopies, and even now, people can wait months for an appointment.
On top of that, screening rates among younger eligible adults remain low. Only about one in five people aged 44 to 49 are up to date with recommended screenings.
Experts say that if the screening age were lowered further, participation might drop even more. For now, the focus remains on improving awareness and encouraging those already eligible to get screened on time.
Two Year Old Girl Diagnosed With Childhood Dementia

Credits: GoFundMe
For most parents, the toddler years are filled with first words, wobbly steps and dreams of the future. For Gus and Emily Forrester, those moments are now overshadowed by a diagnosis they describe as “every parent’s worst nightmare.”
Their two-year-old daughter, Leni, has been diagnosed with Sanfilippo Syndrome Type B, a rare genetic condition often referred to as childhood dementia. The disorder, formally known as Mucopolysaccharidosis type III, gradually robs children of their physical and cognitive abilities.
In an interview with ITV News, Leni’s parents spoke about the devastating reality of the condition, which has no approved cure or widely available treatment.
“All your dreams for your child's future are taken away,” her mother, Emily, said. “To be told that she has this condition, and there is no treatment and no cure and no support… it’s completely earth-shattering.”
What Is Childhood Dementia?

Sanfilippo Syndrome is a neurodegenerative disorder caused by the body’s inability to break down certain complex sugars. Over time, these substances build up in the brain, leading to progressive damage.
According to Cure Sanfilippo Foundation, symptoms usually begin appearing between the ages of one and six. Children may initially show mild developmental delays, but the disease gradually worsens, affecting speech, mobility and behaviour.
As the condition advances, many children lose the ability to talk, walk and recognise loved ones. Life expectancy is often limited to the early teenage years.
Emily explained the process in stark terms. Without treatment, she said, Leni’s body will slowly be overwhelmed by “toxic waste,” causing irreversible damage.
The Urgency of Early Treatment
For families like the Forresters, time is not just precious, it is critical.
“Early treatment is key for these children,” Emily said. “If she has to wait six months, that could mean she can no longer talk. If she waits 12 months, that could mean she loses the ability to walk.”
Although experimental therapies, including gene-based approaches, are being developed, access remains a major hurdle. Some clinical trials are expected to take place in the United States later this year, but Leni is not currently eligible.
Her parents are now campaigning for UK patients to be included in these trials, arguing that promising science already exists but remains out of reach for many families.
A Family's Fight For Hope
In response to the diagnosis, the Forresters have launched a fundraiser to support Leni’s care and potential treatment options. They have also pledged to donate part of the funds to Great Ormond Street Hospital, where Leni is receiving care, and to the Cure Sanfilippo Foundation, which supports affected families.
So far, donations have crossed $250,000, reflecting the growing awareness and concern around rare childhood conditions.
Leni’s father, Gus, said the emotional toll of the diagnosis is hard to put into words. “As parents, your role is to protect your children and provide every opportunity you can. Without any treatment, her future and her reality is very, very dark.”
Beyond fundraising, the couple is also raising awareness about childhood dementia and advocating for newborn screening programmes that could help detect such conditions earlier.
Experts working on experimental therapies say greater government investment is urgently needed. Without it, many children may never benefit from treatments that could slow or alter the course of the disease.
For now, Leni remains a cheerful two-year-old, full of life and affection. But for her parents, every passing day is a reminder of how quickly that could change, and how urgently answers are needed.
© 2024 Bennett, Coleman & Company Limited

