- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Why Everyone Is Suddenly Talking About Ivermectin As A Cancer Breakthrough?

A PubMed search for “ivermectin” and “cancer” yields hundreds of preclinical studies, many conducted on cell cultures or mice. In the sector of alternative cancer treatments, few drugs have generated as much buzz—and controversy—as ivermectin. Once lauded for its ability to treat parasitic infections and awarded a Nobel Prize for its contribution to global health, ivermectin has more recently been at the center of misleading narratives, first as an alleged cure for COVID-19 and now as a so-called “cancer breakthrough.”
Social media, podcasts, and even some patient communities are abuzz with stories of miraculous recoveries and scientific “breakthroughs.” But what’s driving this surge of interest, and does the science live up to the hype?
For decades, ivermectin was best known as a safe and effective treatment for parasitic diseases like river blindness and scabies. Its impact was so significant that it earned its discoverers the Nobel Prize in 2015. But after being widely discredited as a COVID-19 treatment, ivermectin found new life in online cancer forums and alternative health circles, where it’s now promoted as a cheap, accessible alternative to mainstream cancer therapies.
The renewed interest in ivermectin as a potential cancer therapy has largely been driven by non-scientific sources. On platforms like X (formerly Twitter), Substack, and YouTube, influential figures promote ivermectin as a natural, low-cost cure "suppressed by big pharma."
One viral moment came during a widely viewed episode of The Joe Rogan Experience, in which actor Mel Gibson recounted how three friends with stage IV cancer reportedly became cancer-free after taking ivermectin and fenbendazole. That snippet, viewed by nearly 20 million people, has fueled speculation—despite the anecdotal nature of the claims.
Further fanning the flames, public figures like Robert F. Kennedy Jr. have accused health authorities of deliberately suppressing ivermectin to favor profit-driven cancer treatments—a claim lacking credible evidence but resonating with those distrustful of traditional medicine.
What Is Ivermectin Approved For?
Ivermectin is a U.S. FDA-approved antiparasitic drug, used for treating river blindness (onchocerciasis), strongyloidiasis, lice, and scabies in humans. It’s also commonly used in veterinary medicine to treat parasitic infections in animals.
Its development and application in tropical medicine were so impactful that the researchers behind ivermectin received the Nobel Prize in 2015. However, its uses have always remained confined to parasitic infections—not viral illnesses like COVID-19, and certainly not cancer.
How Ivermectin Might Work Against Cancer?
Ivermectin’s anticancer effects appear to be unrelated to its anti-parasitic action. Instead, the drug disrupts cancer cell signaling, impairs mitochondrial function, induces autophagy (a process that can kill cancer cells), and inhibits cancer stem cells. It also weakens the mechanisms that allow tumors to resist chemotherapy and evade the immune system.
In the Brazilian rat study, nano-encapsulated ivermectin not only shrank tumors but also improved the health of surrounding brain tissue and reduced abnormal blood vessel growth—suggesting multiple avenues of attack against cancer.
What the Science Says About Ivermectin and Cancer?
A search of scientific literature reveals hundreds of studies linking ivermectin to cancer research. Some of these suggest that ivermectin may interfere with cancer cell metabolism, inhibit tumor growth, or boost immune response in lab-controlled environments. But—and this is critical—lab results do not equal human results.
Dr. Peter P. Lee, chair of the Department of Immuno-Oncology at the Beckman Research Institute of City of Hope, has studied ivermectin's immune-stimulating effects in mice. While findings hinted at some tumor-modulating potential, they fell far short of demonstrating therapeutic value in humans.
At the 2025 American Society of Clinical Oncology (ASCO) Annual Meeting, early results from a phase 1/2 trial combining ivermectin with immunotherapy in metastatic triple-negative breast cancer patients showed no significant benefit. Of the eight patients evaluated, six experienced disease progression, one had a partial response, and one achieved stable disease.
Risks of Using Ivermectin as a Cancer Therapy
Promoting ivermectin for cancer without evidence carries several dangers:
Neurological toxicity: High doses can lead to seizures, confusion, blurred vision, or even coma.
Drug interactions: Ivermectin can interfere with common cancer medications, such as blood thinners or immunotherapy agents.
Treatment delays: Perhaps most concerning is the risk that patients may delay or forgo evidence-based cancer treatments in favor of unproven, alternative drugs. Such delays can allow the cancer to progress unchecked.
False hope and financial exploitation: Some patients may spend time, money, and emotional energy pursuing unproven remedies, only to face worsening outcomes.
Why the Sudden Surge in Popularity?
Several factors have converged to make ivermectin a hot topic in cancer circles. Social media amplification has played a major role, with influencers and alternative health advocates promoting ivermectin as a cheap, “natural” alternative to mainstream cancer treatments. These promotions often rely on cherry-picked studies or anecdotal stories of success, rather than clinical evidence. Distrust in conventional oncology also fuels interest—many patients, disillusioned by the side effects, financial burden, or perceived limitations of standard therapies, are increasingly drawn to off-label or experimental alternatives like ivermectin.
Preclinical breakthroughs, such as the much-publicized Brazilian nano-ivermectin study in animals, add to the intrigue by generating hopeful headlines, despite lacking human trial data. Finally, political and cultural overtones stemming from ivermectin’s controversial use during the COVID-19 pandemic have transformed the drug into a rallying point for individuals skeptical of established medical authorities, further complicating the public narrative around its potential role in cancer treatment.
Where Does This Leave Patients and Doctors?
While the science around ivermectin and cancer is evolving, the consensus among oncologists and researchers is clear: There is no solid evidence that ivermectin can cure or significantly treat cancer in humans. The most promising findings are still limited to laboratory and animal studies, and ongoing clinical trials have yet to show meaningful benefit in people.
That said, the safety profile in small studies is reassuring, and the innovative use of nanotechnology to deliver ivermectin to brain tumors is a genuine scientific advance—one that warrants further research but not premature celebration.
Curiosity Is Good—But Let's Stick to the Science
The buzz around ivermectin as a cancer cure is based more on anecdotes and viral claims than on real science. While early lab data may inspire future studies, there is currently no evidence that ivermectin can treat or cure cancer in humans. Ivermectin’s journey from Nobel-winning anti-parasitic to cancer “miracle drug” is a testament to both the power of scientific curiosity and the dangers of viral misinformation.
Patients facing cancer deserve hope—but not false hope. Turning away from proven therapies in favor of unproven ones could have devastating consequences.
From Vaping to Worm Attack: 5 Unimaginable Ways to Contract Meningitis

The meningococcus bacteria can harmlessly live in the throat without showing any symptoms, but in order to cause damage, it must cross the nasopharyngeal barrier. (Photo credit: iStock)
New Delhi: Meningitis may not have been the talk of the town, but it is now making headlines after an outbreak in the UK wreaked havoc on students—the outbreak recently resulted in the death of two students, and 11 others have been hospitalised. The outbreak is being linked to a nightclub event in Canterbury, Kent. Following this, the UK Health Security Agency contacted 30,000 students, staff, and their family members, along with anyone who visited the club from March 5 to March 7. This was a precautionary measure, they said, and a new report by UK health officials suggests that meningitis B has caused the outbreak. But what is most shocking is how this infection makes its way into your body.
What is meningitis?
Meningitis is an infection of the protective membranes around the spinal cord and the brain. It can become very serious if not treated or diagnosed in time. It is a consequence of bacterial or viral infection. Despite being a rare occurrence, the infection can spread through coughs, sneezes, a cold, or physical contact in the form of kissing.
Uncommon ways of contracting meningitis
Some of your daily habits may seem normal, but in turn, they can be among the worst ways to catch meningitis. Some of the most obscure ways are:
Vaping: Reminder—vaping might be common now, but that does not make it a safe practice. It is associated with respiratory disorders and even lung collapse in some cases. When it comes to meningitis, vaping can be a means of passing germs on to another person—for instance, by sharing a contaminated vape. The meningococcus bacteria can harmlessly live in the throat without showing any symptoms, but in order to cause damage, it must cross the nasopharyngeal barrier.
Second-hand smoke: Second-hand smoke may not just cause cancer, but also meningitis. This risk is particularly prevalent in children, as it may increase their chances of developing invasive meningococcal disease, a serious form of meningitis. Experts from the University of Nottingham have noted that breathing in smoke from someone else's cigarette can make one more vulnerable to infection. This makes people more likely to harbour meningitis-related bacteria in the throat and nose, thus leading to infection.
Worm infection: Some types of parasites, such as tapeworms, can cause a rare type of meningitis known as eosinophilic meningitis. These worms take residence in the gut and feed on nutrients that the body needs to stay healthy. This can result in diarrhoea, nausea, and tiredness. If the infection spreads to the brain, it can cause meningitis. Despite being rare, it is still a possibility.
Sharing cutlery: Meningitis can spread through close contact, and sharing cutlery can be one of the most overlooked ways. This can also include sharing toothbrushes. The infection can spread through droplets and saliva.
Unwashed hands: An act of laziness can cost you in the long run; therefore, using a sanitiser or regularly washing hands is a must. Experts say that particles from faeces can linger on the hands, and ingesting them in any way can lead to infections such as meningitis. The infection can also spread through coughing and sneezing.
COVID-like Nasal Swab Test May Help Spot Early Alzheimer's Signs
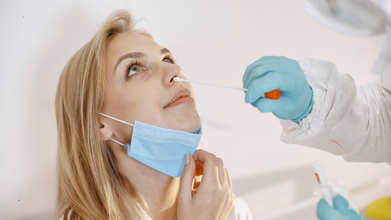
Credit: Canva
A team of US researchers has developed a novel nasal swab test, akin to those used to detect COVID-19 infections, which can spot early signs of Alzheimer's Disease -- affecting over 55 million people worldwide.
The condition is treatable in early stages to manage symptoms and slow cognitive decline. However, it remains the hardest to detect, affecting treatment outcomes. The brain changes can begin 10 to 20 years before symptoms become apparent.
The novel outpatient nasal swab, developed by Duke University researchers, has shown promise in picking up early biological changes linked to Alzheimer's. It can spot the degenerative condition, even before problems related to thinking and memory begin to appear.
"We want to be able to confirm Alzheimer's very early, before damage has a chance to build up in the brain," said Bradley J. Goldstein, professor at Duke University's School of Medicine.
"If we can diagnose people early enough, we might be able to start therapies that prevent them from ever developing clinical Alzheimer's," Goldstein added.
How Effective Was The Nasal Swab?
In the study, published in the journal Nature Communications, the team placed a gentle swab high inside the nose of 22 participants.
The swab collected thousands of nerve and immune cells to see which genes are active.
The analysis clearly differentiated people with early or diagnosed Alzheimer's from those without the disease -- 81 percent of the time. It also included people with no symptoms.
Alzheimer’s Disease: The Leading Cause of Dementia
Alzheimer's disease is one of the most common forms of dementia and mostly affects adults over the age of 65.
About 8.8 million Indians aged 60 and above are estimated to be living with Alzheimer's disease. Over seven million people in the US, 65 and older, live with the condition, and over 100,00 die from it annually.
Alzheimer's disease is believed to be caused by the development of toxic amyloid and beta proteins in the brain, which can accumulate and damage cells responsible for memory.
While there is no clear cause of Alzheimer's disease, experts believe it can develop due to genetic mutations and lifestyle choices, such as physical inactivity
unhealthy diet
social isolation.
Early symptoms of Alzheimer's disease include forgetting recent events or conversations. Other signs include:
- losing or misplacing things
- getting lost when walking or driving
- being confused, even in familiar places
- losing track of time
- difficulties solving problems or making decisions
- difficulties performing familiar tasks
- misjudging distances to objects visually.
Over time, Alzheimer's disease leads to serious memory loss and affects a person's ability to do everyday tasks.
Currently, there is no cure for this progressive brain disorder, and in advanced stages, loss of brain function can cause dehydration, poor nutrition, or infection. These complications can result in death.
Being physically active and taking part in activities and social interactions that stimulate the brain and maintain daily function can help prevent the condition.
HPV: Why Vaccination In Adolescents Is Important?
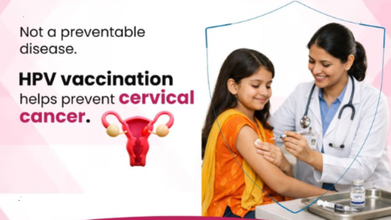
Credit: Health Ministry/X
The Human papillomavirus (HPV) vaccine is one of the most important advances in preventive healthcare, with the unique ability to prevent cancers.
Evidence consistently shows that the most appropriate age for HPV vaccination is between 9 and 14 years. At this stage, children develop a significantly stronger immune response, producing higher antibody titers than older adolescents and adults.
This enhanced immunogenicity translates into durable and highly effective protection and also allows simplified schedules, including the possibility of single-dose protection, thereby improving feasibility and coverage at a population level.
HPV Vaccine: Why Age 14 Matters The Most
The emphasis on vaccination by the age of 14 years is particularly important. Beyond this age, the immune response is relatively lower, and the number of doses required increases, making early vaccination both scientifically and programmatically more efficient.
Recognizing this, the Government of India has adopted a strategy of administering a single-dose HPV vaccine to adolescents up to 14 years of age through school- and community-based outreach programs. The program utilizes the Gardasil vaccine, which has an established track record of safety and efficacy over nearly two decades.
Equally critical is the timing of vaccination in relation to exposure. HPV is primarily transmitted through sexual contact, and vaccination before exposure ensures maximum effectiveness. Administering the vaccine in early adolescence provides protection well before any potential risk, making it a true preventive intervention with near-complete benefit.
Persistent infection with high-risk HPV types is a well-established cause of several cancers. In India, cervical cancer continues to be one of the leading causes of cancer-related illness and death among women. While HPV is also responsible for anal, penile, and oropharyngeal cancers, the burden of cervical cancer is substantially higher, which has historically led to a greater focus on vaccinating girls.
HPV: Are Boys At Risk?
However, HPV infection affects both genders. Boys are also at risk of HPV-related diseases, including anal and penile cancers, genital warts, and oropharyngeal cancers, the incidence of which is rising globally.
Vaccinating boys offers direct protection to them and also contributes to reducing transmission within the community. A broader, gender-inclusive approach has the potential to enhance population-level protection.
Public health agencies, including the World Health Organization, have emphasized HPV vaccination as a key strategy in cancer prevention and in reducing the long-term burden of non-communicable diseases.
HPV Vaccine: Part of Adolescent Health Check-ups
Integrating HPV vaccination into routine adolescent health check-ups can further normalize it as a standard preventive health measure. This approach can complement government efforts by encouraging participation from the private healthcare sector and improving overall uptake.
HPV vaccination in the 9–14 year age group is therefore not merely a recommendation; it is a time-sensitive, evidence-based intervention that can prevent cancers decades later. Strengthening awareness and ensuring timely vaccination will be critical in reducing the future burden of HPV-related cancers in India.
© 2024 Bennett, Coleman & Company Limited

