- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Why Is Snow Shoveling Risky For Your Heart?

Snow Shoveling (Credit: Canva)
Shovelling snow may seem like a routine winter task, but for many, it poses significant health risks, particularly for the heart. The cold temperatures combined with physical exertion can strain the cardiovascular system, increasing the likelihood of heart attacks. Here's what you need to know to stay safe this winter.
Why Snow Shoveling Is Risky?
Cold weather constricts blood vessels and raises blood pressure, forcing the heart to work harder to circulate blood. The physical demands of shovelling—lifting heavy snow and throwing it aside—compound this stress. Unlike leg-focused exercises, shovelling relies heavily on arm muscles, which places a greater burden on the heart.The research underscores these risks. A study by the American Heart Association linked heavy snowfall (7–8 inches) to a 16% increase in heart attack hospitalizations among men and a 34% rise in fatal heart attacks. Alarmingly, the heart rate can spike to 85% of its maximum within just two minutes of shovelling, mimicking the intensity of vigorous aerobic exercise.
You can follow these tips to protect your heart
While snow removal is unavoidable for many, there are steps you can take to reduce the risk of a heart attack:
- Time it wisely: Avoid shovelling immediately after eating or smoking, as these activities can elevate blood pressure.
- Pace yourself: Divide the task into smaller segments, taking frequent breaks to avoid prolonged exertion.
- Push, don’t lift: Pushing snow is less strenuous than lifting it. If lifting is necessary, use a smaller shovel and avoid overfilling it.
- Shovel light snow: Clear snow when it’s fresh and powdery, rather than after it has become heavy and compacted.
- Stay warm, but not overheated: Dress in layers and adjust as needed to prevent overheating.
- Shovel later in the day: If possible, wait for warmer temperatures before starting.
- For those with existing cardiovascular concerns, consulting a doctor before winter sets in is prudent. A stress test can help gauge heart health, and cardiac rehabilitation programs may improve fitness levels to reduce risk.
Besides affecting your heart, snow shovelling can also lead to brain stroke. There are multiple researches that indicate that winter months increase the risk of stroke.
Primarily, colder weather causes blood vessels to constrict because of an increase in vasoconstrictors like noradrenaline. This raises the blood pressure, a major risk factor for stroke.
Winter or colder weathers also increase the likelihood of platelet aggregation and tilts the balance of clotting and clot lysis, making it easier to clot. A blockage in a blood vessel to the brain caused by blood clots is one of the main causes of stroke.
Humidity is also known to play a major role in an increased stroke risk. High humidity in the atmosphere can cause some people to become dehydrated, increasing the risk of blood clot formation. As humidity rises, so does the stroke risk, with a two per cent increase for every five-degree rise in dew point.
Lack of sunlight exposure and a sedentary lifestyle can both increase the risk of stroke. Sunlight is the main source of Vitamin D, which is pivotal to the health of blood vessels. Meanwhile, a lack of physical activity can hamper the regular circulation of blood.
Cold weather also increases the risk of serious systemic infections in the elderly, increasing susceptibility to brain stroke.
Over 38,000 Prescriptions Of Wegovy Pill In 5th Week After Its Launch

Credits: Britannica
Five weeks after the launch of Novo Nordisk's weight loss pill, Wegovy, 38,220 US prescriptions have been reported by IQVIA for the same. The company shares too climbed up by 4% on Friday, and touched the levels last seen in October.
The oral version of the Wegovy pill became available to US patients earlier this month after the US Food and Drug Administration (FDA) approved it in December.
How Effective Is The Wegovy Pill?
After injection by Novo Nordisk, of the same name, Wegovy, which has been on the market since 2021, its popularity grew so much that it was in short supply until February 2025. The pill version has now come out, which many experts believe will expand its accessibility. As the monthly supply of pill is expected to be cheaper than the monthly supply of the weight loss injection.
A study published in the New England Journal of Medicine show that a 25 milligram Wegovy pill led to 13.6% reduction in weight on average over 64 weeks. When compared to placebo, the result was only 2.2% of weight loss. Novo Nordisk says that those who stayed on the treatment and reduced their calorie intake, it would lead to a loss of 16.6% of their weight.
How To Use The Weight Loss Pill?
The first step lies in buying the correct and safe weight loss pill. Make sure the weight loss pills are clinically proven option for people to use to reduce their weight.
Take the pill with a glass of water. Make sure to always have the pill prescribed and follow the instructions that you GP has told. Store the pill in a cold place, however avoid freezing the medicine. Keep the medicine out of a child's reach. In some weight loss pills, if you miss your dosage, you can take it within 1 hour, however, clarify these doubts from your GP. A pill can usually be consumed within an hour of a fat-containing meal up to three times a day., however, the Wegovy pill must be taken on an empty stomach. Patients are advised not to eat, drink, or take other medicines for at least 30 minutes afterward. Thus, one must follow what is being prescribed for the best result, as the administering of the pill could vary based on the medication.
Most importantly, a healthy balanced diet, and a regular workout routine is also important will the person is on the pill.
Read: Wegovy Starter Dose Now Available As Daily Pill, Replacing Weekly Injections
What Are The Side Effects Of Wegovy Pill?
Digestive problems such as nausea and vomiting remain the most common side effects of GLP-1 drugs. These issues were also reported in studies of the pill versions. Around 7 percent of participants taking the Wegovy pill stopped treatment because of side effects, compared with 6 percent in the placebo group. In orforglipron’s trial, up to 10 percent of patients discontinued treatment, compared with 3 percent on placebo.
One key difference lies in how the medications are used. The Wegovy pill must be taken on an empty stomach with a small amount of water. Patients are advised not to eat, drink, or take other medicines for at least 30 minutes afterward. Doctors say this requirement has limited the use of Rybelsus, the pill form of semaglutide approved for diabetes, compared with Ozempic.
Eli Lilly highlights that orforglipron was taken once daily in trials without restrictions on food or water, which may make it easier for patients to use consistently.
Women Heart Symptoms Could Differ From Men, Explains Expert

Credits: Canva
On February 13, Canadians across the country mark Wear Red Canada Day, a reminder that heart disease remains the leading cause of death for women. Yet despite the scale of the problem, many women still do not recognize their risk or their symptoms.
“We’re learning more and more each day about how heart disease uniquely affects women,” said nurse practitioner and researcher Rachel Ollivier in an interview with CTV News. She emphasized that awareness is still lagging, both among patients and within health-care systems.
According to the World Health Organization, cardiovascular disease accounts for roughly one in three deaths among women globally. In Canada, heart disease and stroke continue to be leading causes of death among women, and women are less likely than men to receive timely diagnosis or treatment.
Symptoms Can Look Different
Chest pain remains the most common heart attack symptom in both men and women. But Ollivier explained that women’s symptoms can often be subtler or feel different.
“For women, they often uniquely experience chest pain that seems like more of a discomfort or a tightness in the chest,” she said. Some women may feel pain in the left arm or jaw, unusual fatigue, nausea, vomiting, or discomfort between the shoulder blades.
Because these symptoms can be less specific, they are sometimes dismissed as stress, anxiety, indigestion, or exhaustion. Social factors also play a role. Women often juggle multiple responsibilities at home and work, and may delay seeking care. In some cases, their concerns may also be minimized within health-care settings.
Medical differences matter too. Women typically have smaller hearts and arteries, and plaque buildup behaves differently compared to men. Conditions such as spontaneous coronary artery dissection and microvascular dysfunction are seen more commonly in women, making diagnosis more complex.
Hormones and the Hidden Risk Window
Beyond symptoms, experts are urging greater recognition of the role hormones play in lifelong heart health.
“Endogenous estrogen is cardio protective,” Ollivier explained. As women enter the perimenopausal transition, estrogen levels fluctuate and gradually decline, and that protection is lost. This shift can lead to higher cholesterol levels and changes in fat distribution, increasing cardiovascular risk, particularly between the ages of 40 and 60.
Colleen Norris, a nursing professor at the University of Alberta and research lead of the CKHui LHHW Women’s Heart Health Research Collaborative who wrote on Yahoo Canada, believes the conversation needs to go even deeper.
She argues that ovaries have long been viewed only through the lens of reproduction. “The ovaries are not just reproductive organs. They are architects of women’s health across the lifespan,” she noted. Estrogen influences the heart and blood vessels, but also the brain, bones, kidneys, metabolism, and immune function.
Most women are never told that ovarian reserve and estrogen levels begin declining in their late 30s. By the time noticeable symptoms appear, biological changes may have already been underway for years.
Menopause itself is just one day, Norris explained. The larger reproductive transition surrounding it is what significantly increases vulnerability to chronic disease. Yet the health-care system often waits until disease develops before intervening.
Moving From Awareness to Action
Both experts stress that education is critical. Women with conditions such as polycystic ovary syndrome, pregnancy complications like preeclampsia or gestational diabetes, and those entering midlife should be particularly mindful of their cardiovascular risk.
Wear Red Canada Day is meant to spark awareness, but symbols alone are not enough. Experts are calling for better research funding focused on midlife women, improved medical education around ovarian aging, and more proactive screening during the reproductive transition.
Heart disease in women is not inevitable. But recognizing that symptoms can differ, and that hormonal shifts matter, could be lifesaving.
Unique Symptoms Of Chikungunya The Outbreak In Seychelles And How Long It Lasts
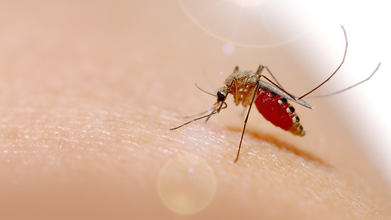
Credits: Canva
Seychelles Chikungunya Virus Outbreak: The United States warned travelers to be careful if they plan to visit the Seychelles islands anytime soon as it is currently undergoing a chikungunya outbreak. As per the Centers for Disease Control and Prevention (CDC), a 'Level 2' advisory for the island has been issued and travelers have been asked to 'practice enhanced precautions' if they do plan to visit.
Unique Symptoms Of Chikungunya: What Is The Disease?
Chikungunya is a mosquito-borne viral disease transmitted primarily by Aedes aegypti and Aedes albopictus, the same mosquitoes that spread dengue fever. Symptoms typically appear three to seven days after a bite and include sudden fever, severe joint pain, headache, nausea, fatigue, and rash in about half of cases.
However, there are certain unique symptoms of chikungunya. For instance, unlike a Dengue fever, chikungunya leaves lingering effects along with joint pain and fatigue that lasts up to weeks.
Unique Symptoms of Chikungunya: What Are They?
While common symptoms like high fever often >102 degree F is common there are other symptoms too, which includes:
- Headache
- Muscle pain
- Fatigue
- Joint Swelling
- Some unique symptoms of this disease includes neurological complications such as rare instances that could lead to encephalitis or the inflammation of the brain, meningitis, or severe nerve issues like Guillain-Barré syndrome.
- Ocular symptoms include red eyes like conjunctivitis, eye pain, or temporary vision problems.
- Unique symptoms could also include bleeding, while it is more common in Dengue, rare bleeding from gums and nose could occur in Chikungunya.
- Other unique symptoms may include chronic and persistent symptoms like joint pain that does not subside after the initial week and lasts for months or even years.
- Other symptoms include cardiovascular and respiratory issues and skin manifestation, which could go beyond the common rash. Some patients may experience vasculitis-like skin lesions.
Unique Symptoms of Chikungunya: How Long Does It Last?
Chikungunya symptoms usually occur with in 3 to 7 days after a bite. However, the symptoms could often last long. While fever could subside in a day or two, chronic symptoms especially like joint pain and muscle pain could last for months. Weakness too could persist.
Unique Symptoms Of Chikungunya: Outbreak In Seychelles Led To US Issuing Travel Advisory
A Level 2 travel advisory has been issued, which means the travelers are expected to practice enhanced precautions as compared to a Level 1 advisory that only asks travelers to practice usual precautions.
In more serious cases, Level 3 advisory is issued that asks travelers to reconsider non-essential travel, whereas a Level 4 advisory asks travelers to avoid all travel.
Read: CDC Travel Advisory Issued For These Islands Amid Chikungunya Outbreak
As CDC issues travel advisory, here is what travelers are expected to do:
- Travelers are expected to protect themselves by preventing mosquito bites, which includes using insect repellent, wearing long-sleeved shirts and pants, and staying in places where air conditioning or that have screens on the windows and doors
- The CDC also tells travelers to get vaccinated for those who are visiting the area affected by a chikungunya outbreak
- If a traveler is pregnant, they are asked to reconsider travel to affected area, especially if they are closed to delivering their baby. Mothers infected around the time of delivery can pass the virus to their baby before or during delivery. Newborns infected in this way or by a mosquito bite are at risk for severe illness, including poor long-term outcomes
- If someone has a fever, joint pain, headache, muscle pain, joint swelling, or rash during or after the travel, they must seek medical care
© 2024 Bennett, Coleman & Company Limited

