- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Why Your Chronic Pain Might Be The Real Reason For Your Worsening Anxiety And Mood Swings

Image Credit: Canva
Pain is the body’s way of signaling that something is wrong. In most cases, pain fades once the underlying issue heals. However, for millions of people, pain becomes a constant companion, lasting for months or even years. This condition, known as chronic pain, not only affects physical health but also has a profound impact on emotional well-being.
Current studies emphasize the strong link between chronic pain and mental illness such as anxiety and depression. Individuals suffering from long-term pain tend to be stuck in a vicious cycle of fear, stress, and emotional distress. But how does chronic pain actually lead to deteriorating mental health, and how can the cycle be stopped?
For over 45 million Americans, chronic pain is a way of life. Although physical pain is the most visible symptom, its impact reaches far beyond the physical body. Chronic pain is frequently accompanied by psychological distress, as many victims experience anxiety and depression caused by their illness.
As per Dr. Ravi Kesari, a general medicine specialist, "Chronic pain and mental illness tend to exacerbate each other. Patients have disturbed sleep patterns, increased mental tension, and depression-like symptoms. This forms a vicious circle in which pain causes emotional distress, which further increases the perception of pain."
This cycle is especially seen in conditions like:
Fibromyalgia – A syndrome of widespread pain, fatigue, and cognitive difficulty.
Irritable Bowel Syndrome (IBS) – A bowel condition frequently associated with stress and tension.
Lower Back Pain – Prolonged pain in the lower back, often accompanied by decreased mobility and depression.
Migraine and Nerve Pain – Prolonged headaches and nerve pain that interfere with daily functioning.
Research indicates that two-thirds of IBS sufferers experience anxiety symptoms, and 65% of patients with depression exhibit chronic pain symptoms. This commonality indicates that mental illness not only heightens sensitivity to pain but also complicates recovery.
How Stress of Chronic Pain Can Rewires Your Brain?
When a person hurts, the body releases stress chemicals such as cortisol and adrenaline to assist in the regulation of pain. Such hormones are helpful during short-term occurrences, but once pain persists over time, continued exposure to stress hormones alters brain chemistry.
"Chronic pain leads to chronic stress, and that changes the neurochemicals in the brain that control mood, thought processes, and behavior," explains Dr. Kesari. "That's why people with chronic pain tend to be irritable, angry, or drained of emotions."
Chronic exposure to stress hormones can cause:
Heightened anxiety and fear reactions, making people excessively careful about everyday activities.
Depression, as serotonin and dopamine levels decrease—two neurotransmitters that produce happiness and motivation.
Cognitive impairment, including problems concentrating, remembering, or deciding.
Pain, Anxiety, and the Fear of Movement
Another very frequent mental impact of chronic pain is kinesiophobia, or fear of movement. Individuals with chronic pain tend to avoid movement for fear of making their pain worse. This avoidance behavior can cause stiffness in the muscles, loss of mobility, and increased pain over time.
For example, a person with chronic back pain might try to avoid exercising, which would further weaken muscles and worsen their condition. This pattern of avoidance and worsened pain begets a spiraling sense of helplessness that further fuels anxiety and mood shifts.
"Anxiety is an understandable reaction to chronic pain," says Dr. Kesari. "People become concerned about what pain will mean for their lives, so tasks that are minor—such as shopping for groceries or socializing—become overwhelming."
Daily Struggles and Self-Esteem Loss
Chronic pain does not only impact mood; it is able to significantly modify the way an individual perceives himself. Most of those who have chronic pain struggle with simple activities such as exiting bed, dressing up, or personal hygiene. Failing to do so by oneself may cause the individual to feel inadequate, frustrated, and socially withdrawn.
As Dr. Kesari describes, "Patients tend to feel ill at ease in social situations because they view their condition as a restriction. This adds to low self-esteem and exacerbates mental illness such as depression."
Considering the complex connection between chronic pain and mental well-being, both physical and emotional welfare must be treated.
Dr. Kesari stresses, "Healthcare providers need to take a whole-body approach to treating chronic pain. That involves coupling conventional pain management with mental health care to break the cycle between pain and emotional distress."
Some strategies that have been found to be effective are:
Cognitive Behavioral Therapy (CBT) – A type of psychotherapy that enables people to deal with negative thought processes and respond to pain.
Physical Therapy & Movement-Based Practices – Gentle exercise, like tai chi or yoga, decreases pain and alleviates fear of movement.
Medication Management – Painkillers can be beneficial, but only as part of a combination of holistic therapies to prevent dependency.
Stress-Reduction Techniques – Techniques such as meditation, deep breathing, and mindfulness assist in balancing stress hormones.
Social Support & Therapy Groups – Sharing experiences with others who live with chronic pain has been shown to combat the sense of isolation and offer emotional support.
Chronic pain is not merely a physical condition—it has a powerful impact on mental health, causing anxiety, depression, and extreme lifestyle constraints. But knowledge of the interlinkage of pain and emotional health can encourage proactive measures toward improved general well-being.
Dr Ravi Kesari is MBBS, MD- General Medicine at Apollo Spectra Hospital, Bangalore in India
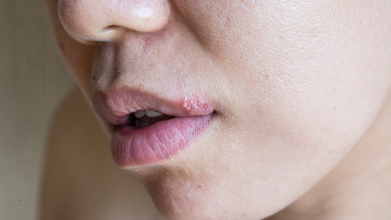
Shared Lipsticks, Makeup Items May Spread Herpes: Here’s How To Stay Safe

Credit: iStock
In a shocking incident, a woman contracted the herpes virus after using shared lipstick samples at a cosmetic store, raising concerns about makeup hygiene.
The incident highlights the risks involved in trying products that come into direct contact with the skin and are shared with a lot of people.
Also Read: World Autism Awareness Day 2026: Can Cell Therapy Be The Future Of Autism Treatment?
What Is Herpes?
The herpes simplex virus (HSV) is very common, and the infection is lifelong. But the symptoms can come and go over different periods of life. Many people never get any symptoms linked to their infection.
The common virus, carried by up to 50 to 80 percent of adults, can cause painful blisters or ulcers. It primarily spreads by skin-to-skin contact. It is treatable but not curable.
There are two types of herpes simplex virus: HSV-1 and HSV-2.
HSV- 1 is the most common and usually spreads by oral contact. It causes infections in or around the mouth (such as oral herpes or cold sores), as well as genital herpes.
Common oral herpes symptoms include
- blisters (cold sores)
- open sores (ulcers) in or around the mouth or lips.
HSV-2 generally spreads by sexual contact and causes genital herpes.
Its symptoms include painful
- bumps,
- blisters,
- open sores (ulcers) around the genitals or anus.
How Makeup Testers Can Spread Infection
Experts warned that makeup testers can become a breeding ground for germs. The repeated use of the open samples can spur their growth and can then spread by “double-dipping” — reusing an applicator after touching the skin. This can transfer viruses and bacteria between users.
“You can absolutely get a herpes infection from a makeup tester," Dr. Whitney Bowe, a dermatologist in New York City, told TODAY. "The more ‘double dipping’ that occurs, the higher the chance of spreading viruses or bacteria at a makeup counter.”
A 2010 study by researchers from Rowan University in New Jersey found that cosmetic samples harbored strep, E.coli, and staph.
For two years, the team examined makeup testers at makeup counters, specialty stores, and drug stores. They found that Saturday is the busiest day of the week, and 100 percent of the samples carried some sort of germ.
How To Stay Safe?
To reduce the risk of infection, experts recommend:
- Much like the toothbrush, personal cosmetics and cosmetic brushes must not be shared.
- Wash and dry your brushes regularly to avoid bacterial growth.
- Avoid applying testers directly to your lips or skin
- Use disposable applicators
- Test products on your hand rather than your face
- Avoid using testers if you have cuts, chapped lips, or active infections.
Why Inclusive Opportunities Matter For Individuals with Autism: Unlocking Untapped Potential

Credit: Canva
April 2 is celebrated worldwide as “Autism Awareness Day” and April as Autism month to create awareness and promote inclusivity and acceptance in society for individuals with autism.
So what exactly is Autism, and why do we need to create a culture of awareness and acceptance?
As per DSM V (Diagnostic and Statistical Manual of Mental Disorders) criteria, in simple terms, there is poor eye contact, impaired social communication skills, repetitive patterns (certain movements or fixation on certain toys, objects), difficulties with sensory processing - extreme sensitivity to sensory inputs (dislike loud noises, sensitive to touch), etc.
As a child, these individuals may not respond to name-calling, have poor eye contact/lack gestures like pointing, etc., lack imagination in play, and may not be able to relate and respond to the emotions of others. They have set routines and dislike changes to their routines. All this can cause significant disruption to their day-to-day functioning.
This year’s theme of -Autism and Humanity- Every Life has Value” reiterates the need for inclusion of autism, ensuring equitable representation of these individuals. Ensuring that society not only recognizes them but also treats them with equal respect and dignity.
Educational Support and Inclusive Workplace
Sarva Shiksha Abhiyan (SSA) was one of the Government's flagship programs, along with Action for Autism, to disseminate information in schools regarding inclusive education for autism. Education is a key foundation to ensure children with autism get suitable opportunities as adults. Special educators, with additional support in schools, can go a long way in ensuring their potential is maximized.
Many IT giants like Microsoft, Google, and SAP encourage tapping the potential of individuals with autism and their exceptional skills. In our country, organizations and NGOs, including Action for Autism, offer training for future employment opportunities.
There is a spectrum of Autistic Spectrum Disorders (ASD) known as Asperger’s syndrome, and these individuals have normal to above average intelligence and can have some exceptional skills, and the world includes some living examples of these with a higher IQ, some of whom are the most successful and famous personalities. Even on the other end of the spectrum, autistic individuals have exceptional skills, some of which include great attention to detail, creativity, problem-solving, and lateral out-of-the-box thinking.
Options for flexible working hours (part-time), understanding their need for routines, and explaining them beforehand regarding important changes to schedules can help them adapt better to an otherwise challenging workplace.
The Need For Sensitization
Understanding individuals with autism may need little extra support, being a little flexible with time deadlines, giving simple instructions, especially written/visual ones, and allowing them time to overcome their communication barriers can go a long way in ensuring they feel heard and valued like anyone else in the workplace.
Sensitization of all major organization employees to foster a culture of acceptance and awareness, and an accessible work environment, is the need of the hour. Autistic individuals do well in a variety of job profiles, including IT, technology, finance, art and creativity, and administration.
Environmental modifications like background noise cancellation with headphones help those with sensory processing issues. At the end of the day, none of us is perfect, it's recognizing our special skills and strengthening them.
Possibilities are endless if we wish to encourage and make these individuals heard. So, let’s carry the Autism Awareness Day beyond a mere day of awareness and light it up blue. Let’s value and acknowledge them being different, but also empower them to act on their special skills to earn them a dignified place in society and the workplace.
World Autism Awareness Day 2026: Origin, Theme, Significance

Credit: UN
World Autism Awareness Day is observed every year on April 2. The day is important to raise awareness about autism — a neurodevelopmental condition affecting communication, social interaction, and behavior — affecting millions of people globally.
According to the World Health Organization (WHO), one in 127 people worldwide is diagnosed with the lifelong brain health condition. It is also among the top 10 conditions contributing to health loss globally.
Also Read: Leptospirosis: US health officials flag outbreak risk after floods in Hawaii
The first child diagnosed with autistic symptoms was Donald Grey Triplett. Labelled as Case 1, he went on to become an American banker, demonstrating that, if provided with the right and inclusive support and opportunities individuals with autism be as productive as others.
“Like anyone else, autistic people should be able to shape their own lives — and help to shape our shared future,” said
António Guterres, UN Secretary-General.
World Autism Awareness Day: Date and History
April 2 was designated as World Autism Awareness Day (WAAD) by the United Nations General Assembly in 2007.
The 2007 General Assembly resolution highlighted the need to raise public awareness of autism.
It stated that "children with disabilities should enjoy a full and decent life, in conditions which ensure dignity, promote self-reliance and facilitate the child’s active participation in the community, as well as the full enjoyment of all human rights and fundamental freedoms on an equal basis with other children".
World Autism Awareness Day: Theme
This year, World Autism Awareness Day is held under the theme "Autism and Humanity - Every Life Has Value".
The 2026 theme highlights and affirms the dignity and worth of all autistic people. While there are international human rights conventions safeguarding the rights of people with autism, they continue to face stigma, discrimination, and barriers to participation.
“Access to timely, quality health care and support services remains limited, driving inequalities across the life course," the WHO said. The global health body urged "sustained action and greater investment" to address these challenges. It also called for developing inclusive policies and services that uphold the rights of autistic people.
This year's theme, thus, is a call to action to recognize the inherent dignity and equal rights of all people with autism.
Guterres highlighted the need for "equal education, fair employment, and accessible health systems" for all persons with autism and to provide inclusive opportunities to participate and thrive, along with others.
Also read: Expert Reveals Why Childhood Autism Is Going Undetected In India
What is Autism?
The National Health Service (NHS) UK defines autism as not an illness or a medical condition with treatments or a "cure", but a developmental condition that affects how people communicate, learn, behave, and interact with others.
It is a spectrum, which means "everybody with autism is different".
People with autism spectrum disorder (ASD) may have difficulty with social interaction, exhibit atypical behavior and activities, or find it hard to communicate.
Early Signs Of Autism
Studies show that symptoms of autism are usually diagnosed within the first 3 years of birth. These include:
- Limited to zero eye contact
- Delayed responses
- Repeating words or actions such as hand-flapping
- Being strong-headed about following the same routine
- Easily annoyed, throws tantrums
- Difficulty understanding and expressing emotions
- Sensitive to certain sounds, textures, lights, or smells.
© 2024 Bennett, Coleman & Company Limited

