- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Women Are More Comfortable With AI-Assisted Mammography
Credits: Canva
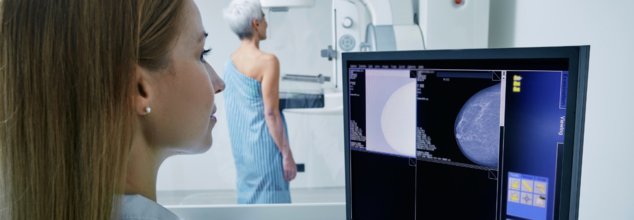
A recent study published in Radiology: Imaging Cancer, found that most women are comfortable with AI being used to support radiologists in interpreting mammograms. The study that surveyed women, found that 71% have said they are fine with AI playing a supporting role in the review process.
However, the trust in AI alone is still low. Fewer than 5% women said they would be comfortable with AI being the sole reviewer of their mammogram results. This also suggested that while women were looking forward to innovation, they still value human expertise, especially when it comes to something as sensitive as breast cancer, which could be life-altering.
What Is A Mammography?
It is a specialized medical imaging test that uses low-dose X-rays to detect any early signs of breast cancer, even before symptoms appear. It can also help identify tumors, calcifications, and other abnormalities in breast tissues. Mammograms are also a vital part of routine breast cancer screening, especially for women who are over the age of 40 or those with a family history of the disease.
During a mammogram, the breast is compressed between two plates to spread the tissue and obtain clear images. These images are then analyzed by the radiologists who then look for any suspicious signs that may indicate cancer.
How AI Plays A Role In Mammography?
With advances in technology, artificial intelligence (AI) is also being used to assist radiologists in reviewing mammogram results. AI algorithms are trained to identify patterns and flag any abnormalities. This also often spots subtle changes that could have been missed by the human eye.
In an AI-assisted mammography, the computer does not replace the radiologist, but acts as a second reader. It also offers another layer of review. This can also increase accuracy, reduce false positives or negatives, and streamline the screening process. Most importantly, AI can quickly process thousands of images, making it a valuable tool in busy healthcare setting.
How Was The Study Conducted?
The study surveyed 518 women at UT Southwestern Medical Center for seven months in 2023. The results showed that women with a higher education levels and more awareness of AI were twice as likely to accept AI in their screenings.
However, the study found that Black and Hispanic women were at a greater concern about data privacy and potential AI basis. These groups were also less likely to trust AI. They have highlighted the importance of addressing equity and transparency in AI development.
There have been previous cases where AI has been biased against African American descents. A Detroit resident Robert Williams was arrested right in front of his children and held in detention for a night after a false positive in an AI facial recognition system. He eventually found out that faulty AI had identified him as a suspect. Another Detroit resident, Michael Oliver, and in New Jersey, Nijeer Parks experienced the same, they both were victims of false positives in AI facial recognition systems.
These instances are the reason why women of color are also apprehensive about AI being used in their diagnosis, due to its perceived bias.
However, women with a family history of breast cancer showed a higher degree of trust when their results were normal, possibly due to relief and reassurance. But women who had previously experienced abnormal results were more cautious, especially when AI and radiologists offered conflicting assessments.
Dr. Basak Dogan, a co-author of the study and director of breast imaging research at UT Southwestern, emphasized the importance of gaining patient trust. “If patients are hesitant or skeptical about AI’s role in their care, this could impact screening adherence and, consequently, overall health care outcomes,” she said.
Patients need to feel confident not just in the technology but also in how it’s being used.
Unique Symptoms Of HMPV - The Virus Without A Vaccine
Credits: Canva
California made it news for a disease that has no vaccination. This is the human metapneumovirus or the HMPV. While some of the symptoms of this virus are similar to that of any common cold or influenza like cough, fever, nasal congestion or shortness of breath, there are several symptoms that are unique to the disease.
Unique Symptoms Of HMPV - The Virus Without Vaccine
Unlike mild common colds, HMPV often presents with a high-grade fever, particularly in children. Some of the other symptoms also include persistent coughing, including dry or productive and may persist for a long duration.
Furthermore, it could cause wheezing, difficulty in breathing, which could also lead to severe lower respiratory tract illness like bronchiolitis or pneumonia. In children and older adults, it could also cause severe or often fatal bronchiolitis or rapid-onset pneumonia.
In infants, it could also exhibit irritability, poor feeding, or dehydration.
Other symptoms, which could resemble common cold like symptoms are:
- cough
- fever
- sore throat
- runny or stuffy nose
- body ache
- headache
What Is Happening In California?
As per the public database WasterwaterScan Dashboard, high levels of HMPV were detected across Northern California cities. The highest levels were reported in Redwood City, whereas elevated levels were found in San Francisco Bay Area and Napa's Wine Country. What's more dangerous is that this virus is without a vaccine.
The good news is that in other parts of country HMPV remains lower. However, the Centers for Disease Control and Prevention (CDC) noted that data from October 2025 shows the cases are trending up, especially during winter and spring.
Read: Virus Without Vaccine Hits California; No Need To Worry, Say Public Health Officials
Dr. Matthew Binnicker, director of the Clinical Virology Laboratory at Mayo Clinic, as reported by The Independent said, "In the late winter, early spring, it can account for five percent to 10 percent of all the respiratory infections that we diagnose in the United States. So it's definitely out there." Experts explain that other viruses like HMPV or influenza get a chance when COVID is quieter.
What Is HMPV - The Virus Without Vaccine?
HMPV was first discovered in 2001 and is part of the Pneumoviridae family along with the Respiratory syncytial virus (RSV).
HMPV most likely spreads from an infected person to others through:
- the air by coughing and sneezing
- close personal contact, such as touching or shaking hands
- touching objects or surfaces that have the viruses on them, then touching the mouth, nose, or eyes
In the US, HMPV circulates in predictable patterns each year, typically beginning in winter and lasting through spring.
Who Are At Risk Of HMPV?
People at risk include:
- elderly people
- children
- people with comorbidities
"The HMPV is not deadly, and there is no evidence of mortality or a severe transmission rate," former Indian Council of Medical Research (ICMR) scientist, Dr. Raman Gangakhedkar, told IANS, during the virus's outbreak in India in 2025.
“The virus may cause pneumonitis-like illness, but the mortality rates are almost unknown so far. HMPV has a global prevalence of about 4 per cent,” he added.
US Heart Surgeon Reveals The Worst Habit That Damages The Entire Body

(Credit Canva/Drjeremylondon)
Smoking has been long recognized as one of the worst habits a person can have, and Dr Jeremy London agrees with this statement. Dr. London, a cardiovascular surgeon, in a recent interview with Mel Robbins revealed that his number one advice as a heart doctor is to avoid smoking.
“I cannot come up with one single thing that does as much damage to every organ in the body as smoking cigarettes. And look, it's incredibly addictive and I know that and I pass no judgment because I know how difficult it is.”
He explained that in his practice he has dealt with chronic smokers for years and still believed that it is the single most dangerous thing one can do to themselves.
Also Read: Why Is It Harder For Women To Quit Smoking?
How Does Smoking Affect Other Organs?
Emphasizing how this one habit affects all organs in our body, Dr London mentioned the well-known link between lung cancer and smoking.
However, there are many more chronic diseases associated with the rest of the body that can develop due to smoking apart from lung conditions, according to the American Lung Association.
Here is what you should keep an eye out for:
Heart Disease
Smoking damages your heart and narrows your arteries, restricting vital oxygen flow. While heart disease rates dropped as smoking decreased, it remains a top killer. Stopping tobacco use helps clear your blood vessels and protects your body’s most important organ.Also Read: 3 Science-Backed Methods To Quit Smoking For Good
Asthma
Asthma makes moving air in and out of your lungs a constant struggle. Cigarette smoke irritates these airways, triggering sudden and dangerous attacks. For the millions of people living with asthma, smoking makes the condition much harder to manage daily.Reproductive Health
For women, smoking reduces fertility and makes it much harder to get pregnant. It also increases the risk of life-threatening ectopic pregnancies. Protecting your reproductive health starts with avoiding tobacco to ensure a safer environment for a potential future pregnancy.Vision Loss
Smoking can actually lead to permanent blindness by damaging the internal structures of your eyes. It is the primary cause of age-related macular degeneration in older adults. Quitting helps preserve your sight and prevents cataracts from forming as you age.Lung Cancer
Smoking is the leading cause of lung cancer, accounting for nearly 90 percent of all cases. Although medical treatments have improved, the five-year survival rate remains low. Quitting is the most effective way to lower your risk of this deadly disease.
Chronic Obstructive Pulmonary Disease
Chronic Obstructive Pulmonary Disease (COPD) is a severe lung condition that makes breathing difficult and exhausting. It often starts with mild shortness of breath but can eventually leave people housebound. Smoking causes up to 90 percent of cases, significantly limiting your physical activity and independence.Other Cancers
Apart from lung, smoking also causes at least twelve different types of cancer, including liver, stomach and colon cancer. For survivors, continuing to smoke greatly increases the chance of a second cancer developing. Avoiding tobacco is the best way to improve overall survival rates.A Three-Hour Dinner Gap May Protect Your Heart, Study Finds

Credit: Canva
Fasting for three hours before bed can significantly improve heart health and reduce the risk of coronary artery disease (CAD) as well as other chronic conditions, an Arteriosclerosis, Thrombosis, and Vascular Biology study suggests.
While many believe that diet plans such as intermittent fasting or time-restricted eating can help reduce their weight, researchers at Northwestern University have found that not eating three hours before going to sleep can reduce overnight blood pressure by nearly four percent, heart rate by five percent and strengthen overall heart rhythms.
This can help reduce overall strain on the heart which lowers risks for conditions like hypertension and CAD. Additionally, the scientists also discovered a drop in blood sugar levels, improved glucose tolerance and insulin sensitivity.
Participants who underwent glucose tests also showed better insulin release which tend to stabilize during the day. Additionally, an improved heart rate also lowered nighttime cortisol, which helped in metabolic balance.
Dr. Phyllis Zee, director of the Center for Circadian and Sleep Medicine and chief of sleep medicine in the department of neurology at Feinberg and corresponding author said of the results: "It's not only how much and what you eat, but also when you eat relative to sleep that is important for the physiological benefits of time-restricted eating."
The study authors also noted: "Extending overnight fasting duration by three hours in alignment with sleep improved cardiometabolic health in middle-aged/older adults by strengthening coordination between circadian- and sleep-regulated autonomic and metabolic activity.
"This sleep-aligned time-restricted eating approach represents a novel, accessible lifestyle intervention with promising potential for improving cardiometabolic function."
Coronary Artery Disease: The Silent Killer
Despite being as a common heart disease, coronary artery disease (CAD) develops over years and has no clear signs and symptoms apart from a heart attack. The illness begins due to a buildup of fats, cholesterol and other substances known as plaque in and on the artery walls.
Over time, this can cause narrowing or blockage of the coronary arteries and block the supply of oxygen-rich blood to heart which can lead chest pain (angina), shortness of breath and ultimately, heart attacks.
Typically, those above the age of 45, having a biological family member with heart disease, lack of sleep, smoking, consuming saturated fats along with other autoimmune diseases such as lupus and rheumatoid arthritis can increase the risk of developing CAD.
Treatment options may include medicines and surgery. Eating a nutritious diet, getting regular exercise and not smoking can help also prevent CAD and the conditions that can cause it.
Nearly one in 10 Indian adults suffer from CAD and about two million people die from the disease annually. Apart from this, about 18 to 20 million American adults aged 20 and older are also affected about the disease.
Strokes: A Rising Crisis In India
Additionally, heart strokes are also one of the leading global health burdens, causing significant deaths and disability worldwide, including in India. Compared to Western countries, stroke also tends to occur at a younger age and is associated with a higher case fatality rate in the country.One in seven stroke patients in India are young adults aged below 45 years, with hypertension leading as the major risk factor, according to a study by the Indian Council of Medical Research (ICMR).
The Global Burden of Disease Study 2021 identified hypertension, air pollution, tobacco smoking, high cholesterol, increased salt intake, and diabetes as the leading risk factors of stroke.
Incidence of stroke is increasing significantly in low- and middle-income countries (LMICs), especially in India, due to population growth, aging, and greater exposure to risk factors.
© 2024 Bennett, Coleman & Company Limited

