- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
World Malaria Day: What Makes Malaria Different From Other Mosquito-borne Diseases?

Credits: Canva
On the day of World Malaria Day, as we raise awareness on the dangers posed by this mosquito-borne disease, let's delve a bit deeper into how malaria is different from the other mosquito-borne diseases.
Dengue vs Malaria
Both malaria and dengue are transmitted by female mosquitoes and cause severe illness in humans. There are certain similarities between the two diseases and the mosquito species, which is why the patients and diagnoses are often confused.
As per the co-Principal Investigator, Dr Charles Guissou, for the Target Malaria, a vector control research alliance's Target Malaria Burkina Faso at the Institut de Recherche en Sciences de la Santé, "Dengue and malaria are two very different diseases caused by different pathogens and different mosquito species." “Misdiagnosis between malaria and dengue is common, and this can then contribute to inappropriate medical care.”
Every year, malaria causes 200 million cases worldwide, leading to 600,000 deaths. Many of these cases are from Africa, where children and pregnant women pay the highest price. The World Health Organization (WHO) has also reported that in 2022, Africa was home to 95% of malaria cases and 95% of malaria deaths. The global incidence of dengue has grown significantly in recent decades. Cases reported to WHO increased from 505,430 in 2000 to 6.5 million in 2023.

Dr Ajay Gupta, Head & Director - Internal Medicine, Max Super Speciality Hospital, Vaishali also points out the key differences between malaria and other mosquito-borne diseases. He says, "Malaria is caused by Plasmodium parasites, transmitted through the bite of infected Anopheles mosquitoes. In contrast, dengue, chikungunya, and Zika viruses are transmitted by Aedes mosquitoes. This distinction in the type of mosquito also reflects differences in peak biting times—Anopheles mosquitoes bite during nighttime, while Aedes mosquitoes are daytime biters."
"Another key difference lies in complications and disease progression. Malaria, especially caused by Plasmodium falciparum, can progress rapidly to severe illness with cerebral involvement, anemia, kidney failure, and even death if not promptly treated. Dengue, on the other hand, is known for a sudden drop in platelet count and risk of hemorrhage. Chikungunya commonly leads to prolonged joint pain, sometimes lasting weeks or even months after the infection clears," notes the doctor.
There is also a difference between how the mosquitoes that spread dengue and malaria.
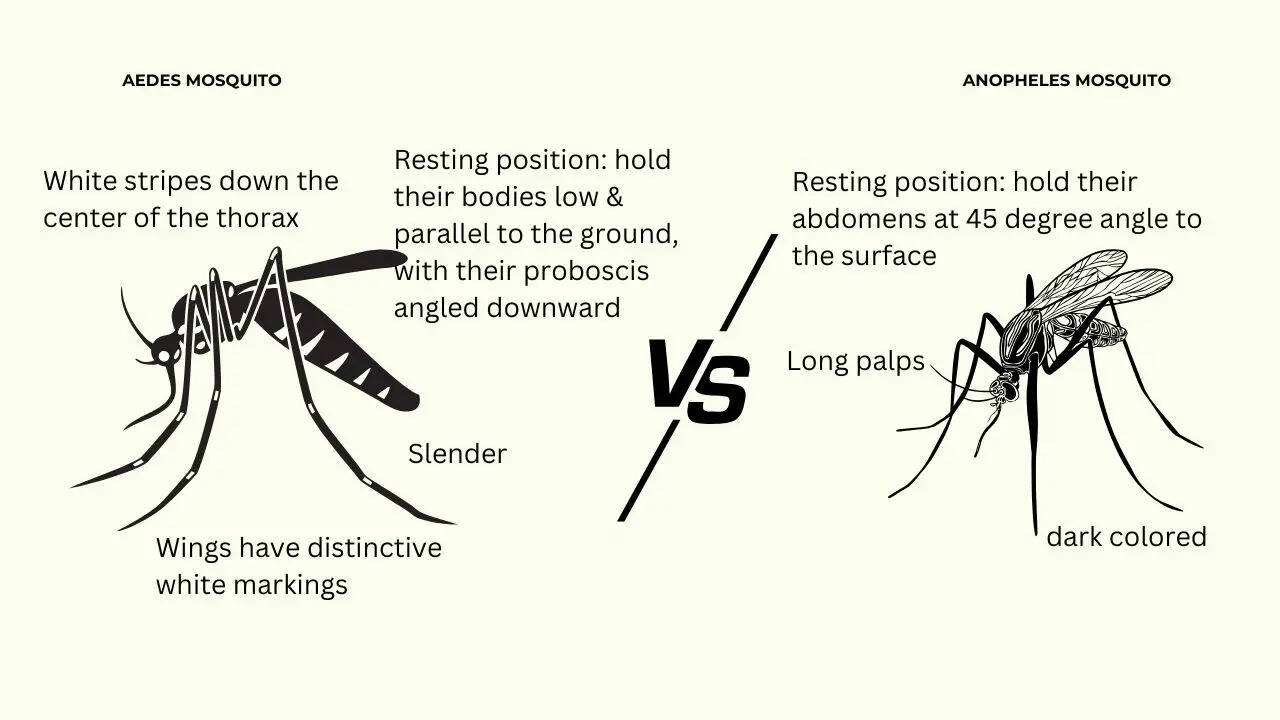
The Aedes Mosquito
It is responsible for spreading dengue and has white stripes down the center of the thorax. It also has a resting position where its body is kept low and parallel to the ground, with the proboscis angled downward. It is slender, and the wings have distinctive white markings.
The Anopheles Mosquito
It is responsible for causing malaria and has long palps. It is dark in color and the resting position follows it abdomen at a 45-degree angle to the surface.
Zika Virus
Zika is a viral infection also transmitted by Aedes mosquitoes, which is the first difference from malaria, in the species of mosquito that causes it. As per the WHO, those with Zika virus do not tend to experience symptoms, and if they do, it includes rash, fever, conjunctivitis, and muscle and joint pain. The symptoms are also what makes it different. They appear from 3 to 14 days after being bitten.
Chikungunya
This is also caused by Aedes mosquitoes, and the symptoms usually appear within 4 to 8 days after infection. The symptoms include fever, joint pain, headaches, and nausea.
Yellow Fever
This is caused by Aedes and haemagogus mosquitoes. People who are infected with this virus do not get sick and experience only mild symptoms. As per the Centers for Disease Control and Prevention (CDC), 12% of people who have symptoms develop serious illness, which includes organ failure and jaundice.
The key difference between all other mosquito-borne diseases and malaria is the species of the mosquito that causes it. While all the others are caused by Aedes, malaria is caused by the Anopheles.
What Else Makes Malaria Different Other Than The Type Of Mosquito That Causes It?
Drinking Beer Could Increase Chances Of Infection
According to the scientists at the University of Emory, in their 2010 study, they found that beer produces an odour in your body that is irresistible to the malaria-carrying mosquitoes.
It Could Take Four Years To Develop Symptoms
There are rare strains of this disease which could in fact take months or even years to get diagnosed. In one of the rare cases, malaria was diagnosed four years later the individuals were infected, reported UK's The Telegraph.
Malaria And Its Connection With Snow White
In 1943, Disney was tasked with creating a film to promote public health awareness. The result? The Winged Scourge — a rather unusual PSA where the Seven Dwarfs learn how to fight off malaria-spreading mosquitoes.
Malaria Has Killed Four Popes, And At Least Eight Presidents Have Suffered From It
George Washington battled malaria, and the disease is also believed to have claimed the lives of Pope Leo and Pope Sixtus—just a few of its prominent victims.
Malaria And India
The doctor also points out that diagnosis and treatment also vary. "Malaria is typically confirmed with a blood smear or rapid diagnostic test and is treated with specific antimalarial drugs. There is no antiviral treatment for dengue, chikungunya, or Zika—management is primarily supportive," he says.
In India, we often see a spike in these illnesses during and after the monsoon season, However, malaria control efforts—such as early diagnosis, insecticide-treated bed nets, and vector control—have significantly reduced the burden in recent years.
"Preventive strategies like eliminating stagnant water, using mosquito repellents, and ensuring proper sanitation are universally effective. But recognizing the distinct nature of malaria is key to prompt diagnosis and management," notes Dr Gupta.
5-Year-Old With Hearing Loss Symptoms Wasn't Deaf, Neurologist Reveals Rare Condition That Caused His Speech And Auditory Loss

(Representational Image)
In a recent post, Dr Sudhir Kumar shared the case of a five-year-old Rishi, a seemingly healthy boy, who suddenly started showing symptoms of deafness and even vision loss. However, the problem wasn’t as surface level as it seemed, as the boy’s brain health was the root cause.
Dr Sudhir Kumar, a Bangalore-based neurologist, shared the rare neurological case of Landau-Kleffner syndrome, he encountered in a five-year-old on the social media platform X.
What is Landau-Kleffner Syndrome?
According to John Hopkins Medicine, Landau-Kleffner Syndrome is a rare nervous system disorder that can cause the loss of ability to understand and use language.
They explain that it can happen to a child who has been developing normally and can also cause seizures. It can happen over time or even suddenly.
But what causes it and is it treatable? The condition is treatable with speech therapy and medication; however, not much is known regarding what causes it.
Researchers say it could be caused by mutation in the genes or the immune system attacking its own tissues like an autoimmune disorder.
Can A Child Stop Hearing Out Of The Blue?
While the first 3 years of Rishi’s life was on track with the development of an average child, things quickly changed.
He stopped looking up when his name was called and acted as if he couldn't hear at all. His parents took him to ear specialists, but the tests showed his ears were perfectly healthy. Over the next year, Rishi stopped speaking entirely and was eventually labeled as "deaf and mute."
Dr Sudhir explained that the timeline of his symptoms didn't match typical deafness. Most children who can't hear are born that way; they don't usually start talking and then suddenly stop.
This suggested that Rishi hadn't lost his hearing, he had lost his ability to understand sound. To solve the mystery, the doctor ordered a sleep EEG to monitor Rishi’s brain waves overnight.
What Are The Symptoms Of Landau-Kleffner Syndrome?
The symptoms of Landau-Kleffner Syndrome can be confusing because they often look like hearing loss or autism. Based on Rishi’s experience, the main signs include:
- Word deafness, which means that the child might hear a sound (like a bell) but cannot understand spoken words.
- Loss of speech is one of the main symptoms of this condition. As the child stops understanding language, they eventually stop speaking the words they once knew.
- Behavioral changes like the children may become frustrated or seem unaware of their surroundings.
- Hidden seizures could also be a symptom. While some children have physical seizures, many (like Rishi) only have abnormal brain activity during sleep.
Is Landau-Kleffner Syndrome Treatable?
The most important takeaway for Rishi’s family was that LKS is treatable. Because it is caused by abnormal electrical activity, doctors can use anti-seizure medications to "calm" the brain. Once Rishi started his treatment, the results were life-changing.
After three months, he began responding to his name again. Within six months, he was talking, playing, and laughing just like any other child. The "silence" in his home was finally gone.
Rishi’s story is a reminder that when a child suddenly loses language skills, every second counts. If LKS is caught early, the brain has a much better chance of recovering and rewiring itself.
If left untreated for too long, the loss of speech could become permanent. By understanding that the problem was in the brain and not the ears, Rishi’s doctors were able to give him his future back.
World Hearing Day: Why Ignoring Hearing Loss Can Affect a Child’s Future And an Adult’s Brain

Credits: Canva
Hearing is one of the most vital yet overlooked senses—and its impact extends far beyond the ears. It shapes how a child learns to speak, how a student performs in school, how adults stay socially connected, and even how the brain ages.
As Dr NVK Mohan, ENT and Cochlear Implant Surgeon at CK Birla Hospitals, CMRI, explains, “Hearing is one of the most vital yet overlooked senses, and its impact extends far beyond the ears.”
This World Hearing Day, the focus is clear: ignoring hearing loss doesn’t just affect sound—it affects development, confidence, learning, and long-term brain health.
What Is Hearing Loss?
Hearing loss can happen when any part of the ear is not working in the usual way. This includes:
- The outer ear
- The middle ear
- The inner ear
- The hearing (acoustic) nerve
- The auditory system in the brain
When sound cannot travel properly through these structures—or when the brain cannot process sound clearly—hearing becomes impaired. It may be partial or complete, temporary or permanent, and can occur at any stage of life, from before birth to adulthood.
In Children: The Impact Goes Beyond the Ears
In children, hearing plays a central role in speech and language development. Even mild hearing loss can cause a child to miss critical sounds needed to build vocabulary and clear speech.
Dr Mohan notes, “In children, undetected hearing loss can interfere with speech development, learning ability, and social interaction, often affecting confidence and academic performance well into adulthood.”
Many parents assume that if a child responds to loud sounds, their hearing must be normal. But hearing is more complex than that.
“Healthy hearing requires the ability to perceive sounds across all frequencies, especially those essential for speech and language development,” he explains. “Delayed identification can mean missed developmental milestones that are difficult to recover later.”
Signs of Hearing Loss in Babies
Even if a baby has previously passed a hearing screening, parents should continue to look for warning signs:
- Does not startle at loud noises
- Does not turn to the source of a sound after 6 months of age
- Does not say single words like “mama” or “dada” by 1 year
- Turns head when seeing you but not when you call their name
- Seems to hear some sounds but not others
What may look like inattention can sometimes be partial or complete hearing loss.
Signs of Hearing Loss in Children
As children grow, signs may include:
- Delayed speech
- Unclear speech
- Difficulty following directions
- Frequently saying “Huh?”
- Turning the TV or radio volume up too high
Babies and children are expected to reach developmental milestones in how they play, learn, communicate, and behave. A delay in these areas could indicate hearing loss or another developmental concern—and should prompt a hearing evaluation.
What Causes Hearing Loss?
Hearing loss can occur at any time during life.
Genetic Causes
About 1 in 2 cases of hearing loss in babies are due to genetic factors. Some babies may have family members with hearing loss. Around 1 in 3 babies with genetic hearing loss have a syndrome, meaning they have additional conditions such as Down syndrome or Usher syndrome.
Other Risk Factors
Around 1 in 4 cases are linked to:
- Maternal infections during pregnancy
- Complications after birth
- Spending 5 days or more in a neonatal intensive care unit (NICU)
- Severe jaundice requiring blood transfusion
- Structural differences in the head, face, or ears
- Neurological disorders
- Meningitis
- Severe head injuries requiring hospitalization
Recognizing these risks allows for closer monitoring and earlier diagnosis.
In Adults: When Hearing Loss Affects the Brain
The consequences of untreated hearing loss do not stop in childhood. In adults and older individuals, the risks shift from speech delays to brain health.
Dr Mohan highlights, “In adults and the elderly, untreated hearing loss is increasingly being linked to social withdrawal, memory problems, and cognitive decline.”
When the brain does not receive clear sound input, it must work harder to interpret speech.
“When the brain is deprived of clear sound input, it has to work harder to interpret speech, diverting cognitive resources away from memory and higher mental functions,” he explains. “Over time, this reduced auditory stimulation and social disengagement can increase the risk of accelerated cognitive ageing.”
In simple terms, when hearing decreases, conversations become exhausting. People may begin to withdraw socially. The brain receives less stimulation. Over time, this combination can affect cognitive resilience.
Hearing health, therefore, is closely linked to brain health.
Prevention: What Can Be Done?
While not all hearing loss can be prevented, certain measures reduce risk:
- Maintain a healthy pregnancy
- Ensure children receive recommended vaccinations
- Protect children from high noise levels
- Seek prompt treatment for ear infections
Noise-induced hearing loss, in particular, is preventable with awareness and protection.
Screening and Early Diagnosis: The Most Important Step
The most important message, experts say, is that hearing loss is both detectable and manageable—especially when addressed early.
“Hearing screening is easy and not painful. Babies are often asleep during the test, and it usually takes only a few minutes,” Dr Mohan says.
For Babies
- All babies should undergo hearing screening by 1 month of age.
- If a baby does not pass, a full hearing test should ideally be completed by 3 months.
For Children
- Hearing should be tested before school entry.
- Testing should also be done whenever there are concerns about speech delay, learning difficulties, or recurrent ear infections.
- Routine hearing checks are equally important for adults, particularly as they age.
Why Pap Smear Is Non-Negotiable After 30 And Why So Many Women Still Avoid It | Women's Day Special

Credit: Canva
Vaccinated for human papillomavirus (HPV)? Now, take that Pap smear test. This is the most common advice women hear to prevent the risk of cervical cancer that annually causes around 6,60,000 new cases and around 350,000 deaths worldwide.
However, it's easier said than done for most of the fairer sex.
A Pap smear is typically a gynecological examination where a speculum is inserted to collect cells from the cervix.
Although the procedure is brief and generally safe, the discomfort discourages many from getting screened. Fear of pain, anxiety of the results, form the common psychological barriers worldwide, and is followed by shame, cultural attitudes, and concerns with male clinicians.
A study in Iran, published in the BMJ Open journal in January 2024, showed that psychological stress, cultural issues, and fear, along with limited information and health services, were the biggest hindrances to getting Pap tests.
Another research published in the BMC Women's Health in December 2022, focusing on Africa, Asia, and South America, reported that many women avoided or delayed Pap smears because they are afraid the procedure will hurt. Many also reported being embarrassed about the pelvic exam or fear of having a stranger see their private areas. Some also worried that the test could damage the uterus.
A Pap Smear test, however, is proven to be safe and is recommended for every woman above the age of 21 years.
“A Pap smear is a rapid, safe, and painless screening procedure that detects irregular cellular changes well before they become malignant. The ability to treat at this pre-cancerous stage of disease provides an excellent outcome,” Dr. Tirathram Kaushik, Senior Consultant GI, HPB, Gastrointestinal & Thoracic Oncology and Robotic Surgery, HCG Cancer Centre, Borivali, told HealthandMe.
A 2025 study, published in the Journal of Contemporary Clinical Practice, showed that pap smears are excellent at ruling out precancerous risks. It also remains a valuable screening tool where molecular testing is limited.
There are many myths about Pap smears that make people anxious or avoid screening. Let’s clear up the most common ones:
Pap Smears Are Painful
The most common myth regarding pap smear screening is that it is painful, unnecessary, or only required when symptoms are present.The Pap smear procedure, which takes only a few minutes, is often described as uncomfortable. While some feel like a quick pinch, others experience slight discomfort or spotting. Severe pain is not considered normal.
“From an oncology perspective, this myth results in a delay in diagnosis. Cervical cancer often occurs silently in its early stages, without any noticeable symptoms,” Kaushik said.
I Am Healthy, So I Don’t Need A Pap Smear
Some people believe that if they feel healthy, they don’t need a Pap smear. However, HPV can cause early cervical cell changes, which usually produce no symptoms.While individuals may feel completely well, they still have abnormal cells developing silently. As a result, regular Pap smear screening is important because it detects these changes early -- before they turn into cervical cancer.
“The HPV infection and subsequent changes that lead to cervical cancer happen slowly over many years. HPV infection is also very common, and one in two women is likely to get infected. Regular screening by a Pap smear will help to catch infection early before it can convert into cancer,” Dr. Deepak Jha, Chief - Breast Surgery & Sr. Consultant Surgical Oncology, Artemis Hospitals, told HealthandMe.
I Have Only One Partner, So I Don’t Need Screening
HPV can be transmitted even in monogamous relationships. Your partner may have been exposed to HPV before, and the virus can stay in the body for years without symptoms.“HPV doesn’t need penetrative sex for infection. It can be transferred if there is any contact of bodily fluid. It’s always safe to test and be assured rather than repent later,” Dr. Jha said.
Testing Means Cervical Cancer
Many women worry that testing automatically means cancer, which is not true. Screening is preventive, and most results are normal.“Even if HPV is detected, it usually indicates a pre-cancerous stage that is highly treatable,” Dr. Parminder Kaur, Consultant Gynecologic Oncologist at CK Birla Hospital, Delhi, told HealthandMe.
Moreover, a Pap smear only screens for cervical cancer; it can’t detect other gynecological cancers such as cervical, ovarian, uterine (endometrial), vaginal, and vulvar cancers. So, screening and appropriate tests for those will be required, irrespective of the Pap smear.
I Am Old, So I Don’t Need A Pap Smear
HPV infection happens at an early age, so merely old age is not enough to stop Pap smear. At least three consecutive negative screens (minimum three-yearly Pap smears or five-yearly HPV screens) would be needed in this situation.I Got Vaccinated, So I Do Not Need A Pap Smear
The vaccine covers the major variants of the HPV virus, but there is still a small probability of cervical cancer due to the uncommon HPV variants.Irrespective of vaccinated status, a woman should go for regular screening between the ages of 25 and 79. Also, if a woman already had HPV exposure before being vaccinated, she would not benefit, the experts said.
“Screening is not just a routine procedure - it is a preventive measure. In the treatment of cancer, early detection alters the disease course, whereas waiting for symptoms to develop means the disease is likely to be already advanced,” Dr. Kaushik said.
Dr Kaur called for more awareness and stated that open discussion are key to help more women take the important screening test.
When To Get Screened
The United States Preventive Services Task Force (USPSTF) and the American Cancer Society (ACS) recommend getting your first Pap test at age 21, followed by Pap testing every 3 years. Even if you are sexually active, you do not need a Pap test before age 21.
- Individuals must start getting Pap tests at age 21. If the result is normal, repeat the test after three years.
- For individuals aged between 30 and 65 years old, doctors are likely to recommend an HPV test along with a Pap test. If both are normal, repeat after five years.
In women older than 65, you don't need to be screened anymore if:
- You have had at least three Pap tests or two HPV tests in the past 10 years, and the test results were normal or negative, and
- You have not had a cervical precancer in the past, or
- You have had your cervix removed as part of a total hysterectomy for non-cancerous conditions, like fibroids.
© 2024 Bennett, Coleman & Company Limited

