- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Experts Confirm 'Baby Brain' Is No Myth- 3 Surprising Ways It Impacts New Moms

Credits: Canva
For generations, “baby brain” has been a punchline—a casual explanation for forgetfulness, misplaced items, or that elusive word hanging just out of reach for new mothers. But what if there’s more truth to this phenomenon than we’ve ever acknowledged? Gratefully, with the aid of contemporary neuroscience and increasing scientific research, scientists are affirming what mothers have always intuited: "baby brain" isn't merely real, but is also a reflection of deep brain changes that start during pregnancy and extend after giving birth.
Science has long proven that the human brain is not fixed. By a process known as neuroplasticity, it reshapes itself constantly in response to great life events. For women, three such stages—puberty, pregnancy, and perimenopause—signal particularly dramatic episodes of brain transformation. But among all these life changes, none appears to produce more far-reaching rewiring than motherhood.
A new National Institute of Mental Health study by neuroscientist Dr. Pilyoung Kim employed MRI scans to take a close look at the brains of recently delivered mothers within days of giving birth and again several months later. In the resulting study published in Behavioral Neuroscience, measurable increases in gray matter volume in various brain regions seldom observed in adult neurodevelopment were found, including:
The hypothalamus, which is responsible for motivation in mothers.
- The amygdala and substantia nigra, which control emotion and reward processing.
- The parietal lobe, which manages sensory integration.
- The prefrontal cortex, the center of reason, decision-making, and judgment.
What's even more intriguing is that these changes were more intense in mothers who exhibited more enthusiasm and affection for their infants. Emotional bonding, in other words, may not only feel good—it could literally make a mother's brain better.
Three Unexpected Effects of "Mom Brain" on New Moms
1. Enhanced Emotional Sensitivity and Social Awareness
Forgetfulness aside, perhaps the most underestiamted phenomenon affecting "baby brain" is its possible positive side. According to new research, the shifts new mothers go through may actually increase their ability for emotional sensitivity, empathy, and social responsiveness.
Hormones such as oxytocin and prolactin—also referred to as the "bonding hormones"—increase during and following pregnancy, encouraging maternal behaviors and increasing attunement with the infant. This ensures mothers are better attuned to detecting subtleties such as a change in facial expression or voice tone—vital for caregiving and early infant maintenance.
Effectively, new mothers can potentially forgo multitasking skills in the short run in exchange for cultivating laser-sharp attention to their baby's needs. What constitutes perceived brain fog can actually be an adjustment in priorities and focus toward caregiving activities essential to a newborn's survival and emotional growth.
2. Structural Brain Development Associated with Learning and Attachment
The idea that a woman's brain "shrinks" following childbirth is a discredited and misleading concept. Actually, according to the study's implication, the maternal brain experiences beneficial structural development, specifically in gray matter—a concentrated form of brain tissue associated with learning, memory, and decision-making.
This expansion is thought to be driven not only by hormones, but by the intense sensory and emotional input of being with an infant. Each diaper change, feeding, cuddle, and lullaby provides input that remodels and strengthens maternal brain circuits.
It's also interesting to mention that all study participants were lactating mothers and none had postpartum depression. Researchers now investigate whether these two mechanisms—hormonal release and emotional management—are linked with neuroplastic modifications in the mother's brain.
3. Memory Failures Could Be Transient but Significant
Yes, "mom brain" will bring about genuine memory loss—such as tossing dirty laundry in the trash or forgetting where you parked the car—but these are fleeting and part of a greater neurological transformation. New mothers have a redirection of information prioritization, such that certain short-term memory processes are relegated to a secondary position while other cognitive processes become enhanced.
Experts believe such lapses may be a result of the brain reordering resources in order to pay attention to emotional management, caregiving actions, and heightened watchfulness over the safety of the baby. Consider it as a functional trade-off and not a decline in intellect.
Can You Prevent "Baby Brain"?
Though you can't stop the changes in your mother's brain—after all, they're engineered to accommodate the new mom role—you can do some things to cope with some of the more annoying side effects:
- Blaming self for memory lapses only creates more stress and mental haze.
- Keep lists, write reminders, and use phone reminders to assist with day-to-day tasks.
- Talk to other moms, that way, the isolation decreases and emotional support increases.
- Lack of sleep is a major contributor that can magnify memory problems.
- Rather than bemoan what you forgot, mark the small milestones your baby achieves daily.
Scientists are now gearing up to examine adoptive mothers to see if they can differentiate changes triggered by hormones from those triggered by the mere stimulation of caregiving. The question that remains the ultimate one is: Does the brain alter behavior—or does behavior alter the brain?
What is increasingly apparent, however, is that motherhood is not an intellectual dumbing-down. It's a cognitive transformation—a restructuring of the brain's circuitry to accommodate one of life's most challenging and rewarding jobs.
Maternal Vaccination During Pregnancy Can Prevent COVID-related Hospitalization In Babies: Study

Credit: iStock/Canva
Maternal vaccination with the COVID-19 vaccine during pregnancy can be effective against severe disease and hospitalization from the SARS-CoV-2 virus in babies, according to a large study.
The study, published in the journal Pediatrics, revealed that COVID vaccination during pregnancy can protect the children against hospitalization for COVID during the first six months of life.
Also Read: COVID-19 Cicada Variant: Will It Become The Dominant Strain In The US? Know All About The Virus
Amid continuing COVID cases, babies under six months old continue to have one of the highest rates of hospitalization — one in five — due to the COVID virus in the US, as per a 2024 study.
As currently no vaccines against COVID are available for neonates and babies, the American College of Obstetricians and Gynecologists (ACOG) recommends maternal vaccination during pregnancy.
Maternal COVID Vaccination Prevented Other Infections
The retrospective study included 146,031 infants born in Norway between March 2021 and December 2023. Of these, 37, 013 (25 percent) were exposed to COVID-19 vaccination in utero.
The findings showed that babies exposed to the vaccine before birth were no more likely to visit the hospital for overall infections (of any kind) than those whose mothers did not get vaccinated in pregnancy.
However, infants whose mothers were vaccinated were about half as likely to visit the hospital specifically for COVID in their first two months of life compared to babies not exposed to the vaccine in utero.
Also Read: Olivia Munn Opens Up About Detecting No-Symptom Breast Cancer With Lifetime Risk Assessment Test
Among 3 to 5-month-old babies, the risk of a hospital visit for COVID was 24 percent lower in those exposed to the vaccine, but the vaccine's protection against COVID wore off by the time infants were older than 6 months.
Importantly, the mothers' vaccine also prevented the risk of other infections in children.
"There is often an increased risk for a subsequent infection after a viral infection, such as an increased risk of pneumonia after influenza infection, so we wanted to study whether protection against COVID-19 could influence the risk of other infections as well," said lead author Dr. Helena Niemi Eide, from the University of Oslo in Norway, the NPR reported.
"But we found that COVID vaccination in pregnancy protected the infant against COVID and had no apparent effect on other infections," Eide added.
Maternal Vaccine Recommendation in the US
Last week, the American College of Obstetricians and Gynecologists reiterated its recommendation for COVID vaccination during pregnancy.
Despite changes in federal vaccine recommendations due to the US Health Secretary Robert F. Kennedy Jr.’s anti-vaccine stance, the ACOG urged COVID vaccination for
- people who are pregnant,
- recently pregnant,
- considering pregnancy,
- lactating.
Also read: Bipolar Disorder: How Early Detection Can Help Prevent Serious Complications
"Accumulated safety data from millions of administered doses show no increased risk of adverse maternal, fetal, or neonatal outcomes associated with COVID-19 vaccination in pregnancy,” the ACOG said.
'Husband Stitch': A Medical Necessity Or Just A Tool To Objectify Women's Bodies?
Credits: AI-generated and iStock
When 36-year-old mom Angela Sanford, from Fort Mill, SC, went for an appointment for a Pap smear five years after she had her first child in 2008, her nurse midwife, who she has never seen before asked her a question she did not expect. "Who stitched you up after your first birth?"
Speaking to Healthline, Sanford shared that she just started crying when the nurse said, "This is not right." Sanford said that this was the first time she ever heard the term 'husband stitch'. Sanford was told that her stich was "too tight" by the hospitalist who managed her after her first delivery.
Also Read: US CDC Warns Of New Immune-Evasive COVID Variant In 23 Countries
“He gave you what some people call a husband stitch,” Sanford recalled the midwife telling her.
“I couldn’t connect in my mind why it would be called that. My midwife said, ‘They think that some men find it more pleasurable,’” she recalled. “My husband has been worried about me and fearful of hurting me. He would never have asked for this.”
A 'Husband Stich' - What Is It?
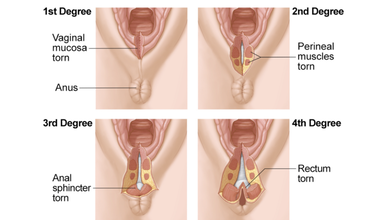
During vaginal delivery, a woman undergoes perineal tears or vaginal lacerations which means tears between the vaginal opening and anus. This causes pain, and requires stitches for grades two and higher. It also takes 4 to 6 weeks to heal. Women can experience from first to fourth degree tears.
Sometimes, a surgical incision is made in the perineum during childbirth to enlarge the vaginal opening, this is called an episiotomy. However, it is not medically necessary or a routine procedure, unless it is a case of emergency.
Stiches are required in such cases that dissolves on its own. However, a 'husband stitch', also known as "daddy stitch" is an unethical practice where an extra stitch is given during the repair process that 'tightens the vagina' to increase sexual pleasure for a male partner. While it is considered a medical malpractice, it is still done to women after vaginal delivery.
Many women face difficulty after the extra stich is given to them. In Sanford's case, she felt "excruciating" pain during sex afterwards.
Read: Romanticization And The Silent Dismissal Of Women’s Pain
When Objectifying Women's Bodies Is Made A Medical Practice
Stephanie Tillman, CNM, a certified nurse midwife at the University of Illinois at Chicago and blogger at The Feminist Midwife told Healthline: “The fact that there is even a practice called the husband stitch is a perfect example of the intersection of the objectification of women’s bodies and healthcare. As much as we try to remove the sexualization of women from appropriate obstetric care, of course the patriarchy is going to find its way in there."
Harkins, 37, said that she "kind of" laughed it off when an "old, crusty Army doctor" overstitched her so she could give her husband more pleasure. In many cases, doctors do it as a routine practice without even being told by anyone. “I couldn’t even process [it], but I kind of laughed, like what else do you do when someone says that? I had just had a baby. I didn’t think much about it because the whole birth experience was so traumatizing, but now that I think about it differently, the implications of that are just crazy.”
Episiotomy Is An Excuse For 'Husband Stitch'
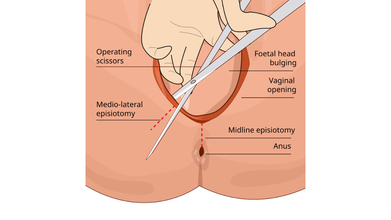
Dr Robert Barbieri, chair of obstetrics and gynecology and reproductive biology at Brigham and Women’s Hospital in Boston, told the Huffington Post that doctors were taught in the 50s and 60s that "routine episiotomy was good for women".
“What they thought is that if they did a routine episiotomy, they’d have a chance to repair it and that during the repair, they could actually create a better perineum than if they hadn’t done it. The idea [was] that we could ‘tighten things up,’” explains doctor.
However, a 2005 systematic review in the Journal of the American Medical Association found no benefit to routine episiotomy use. A 2017 Cochrane review “could not identify any benefits of routine episiotomy for the baby or the mother.” In 2016, the American College of Obstetricians and Gynecologists (ACOG) recommended that clinicians “prevent and manage” delivery lacerations through strategies like massage and warm compresses rather than making cuts on the perineum. Yet, this practice still continues inside the labor rooms.
© 2024 Bennett, Coleman & Company Limited

