Can Fertility Be Preserved In Men After Chemotherapy?
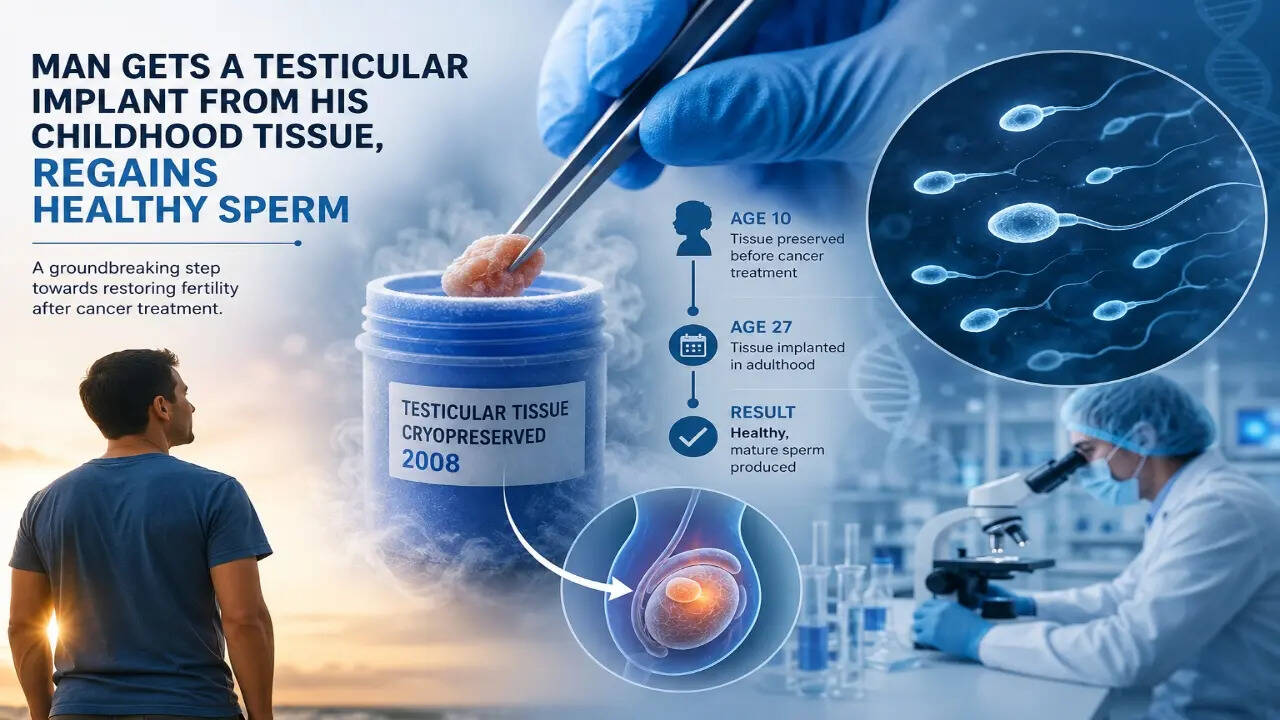
A case of testicular implant may change the way infertility is managed. (Photo credit: AI generated)
SummaryEgg freezing helped many women plan pregnancies later—but this testicular implant helped a sickle cell disease patient regain fertility.
End of Article
