- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
James Harrison, Whose Rare Blood Saved Over 2 Million Babies, Dies At 88

Image Credit: Australian Red Cross Lifeblood
James Harrison, Australia's most successful blood and plasma donor, died at 88, leaving behind a record of saving lives that will never be equaled. Nicknamed the "Man with the Golden Arm," Harrison's blood was rare in that it had a special antibody that was instrumental in creating life-saving medication for mothers and their unborn children. His incredible efforts saved more than 2.4 million babies, making him one of the most remarkable donors in medical history.
Having been born in Australia, Harrison's blood donation experience started following a health crisis. At 14, he was subjected to open chest surgery and survived on the basis of blood transfusions. Extremely touched by the kindness of strangers, he promised to return the favor in the form of being a donor himself as soon as he could. True to his promise, at 18 he rolled up his sleeves for the first time, even though he had always been afraid of needles.
What began as a gesture of appreciation quickly evolved into a lifelong endeavor. During a span of six decades, Harrison donated blood and plasma over 1,100 times before retiring in 2018 at the age of 81. His donations became the backbone of Australia's medical breakthroughs for the treatment of a rare yet life-threatening illness called Haemolytic Disease of the Fetus and Newborn (HDFN), also referred to as Rhesus disease.
Discovery of a Rare Antibody
Medical researchers found in the mid-1960s that Harrison's blood held a rare and essential antibody called Anti-D. This antibody was instrumental in creating a revolutionary treatment to ward off HDFN, a disorder that happens when a mother's immune system strikes back at her unborn child's red blood cells because of incompatibility of blood types. If left alone, this disease might result in severe anemia, brain damage, or infant death.
Scientists suspect that Harrison’s unique blood composition may have been a result of the transfusions he received during his surgery as a teenager. Regardless of its origins, his rare antibodies became a beacon of hope for thousands of expectant mothers and their babies.
Harrison's unshakeable dedication rendered him Australia's inaugural and most committed Anti-D donor. As reported by the Australian Red Cross Lifeblood, nearly 17% of expectant mothers in the nation need Anti-D injections, and the majority of the supply is from a limited group of fewer than 200 plasma donors. Harrison's generosity formed the basis of this life-saving treatment, which continues to save nearly 45,000 infants annually.
Even with the praise and global acclaim, Harrison was humble. In 1999, he received the Medal of the Order of Australia, among the country's most distinguished civilian awards, for his remarkable service. But he most often minimized his efforts, encouraging others to donate and carry on the life-saving work.
Harrison's death on February 17 at Peninsula Village Nursing Home on the New South Wales Central Coast brought an era to a close, but his legacy lives on. Researchers at the Walter and Eliza Hall Institute of Medical Research (WEHI) in Melbourne, in partnership with Lifeblood, have been developing a project known as "James in a Jar." By using Harrison's blood and immune cell samples, scientists have been able to replicate and grow the Anti-D antibody in the laboratory. This development is promising that the vital treatment can be produced on a large scale without the need for human donors in the future.
Tracey Mellowship, Harrison's daughter, remembers her father not only as a life-saver but also as a man with a big heart and a great sense of humor. His tale is a strong reminder of what one person's dedication to a cause can do to millions of lives.
WHO's New Guidance to Accelerate Antibiotics Development for 3 Deadly Bacterial Infections
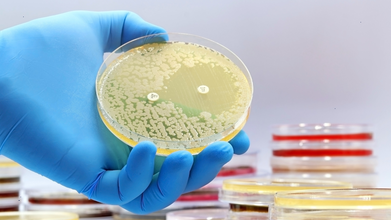
Credit: Canva
Amid a global increase in multidrug resistance, the World Health Organization (WHO) has released new guidelines that flags the lack of innovative antibiotics for vulnerable populations, as well as press the need for the rapid development of drugs to target three deadly bacterial infections.
The WHO's 2025 report on antibacterials in pipeline has highlighted that 90 new antibacterial agents are in preclinical or clinical development. Yet few are innovative antibiotic candidates with potential to target bacterial priority pathogens.
The WHO-developed Target Product Profiles (TPPs) call for accelerating the development of antibiotics to tackle the burden of drug-resistant bacteria in at-risk populations worldwide that lead to:
- Severe multidrug-resistant gram-negative infections such as bloodstream infections and hospital-acquired or ventilator-associated bacterial pneumonia. These are caused by carbapenem-resistant Enterobacterales, Acinetobacter baumannii, and Pseudomonas aeruginosa.
- Severe antibiotic-resistant gram-positive infections in immune-suppressed and critically ill patients. It is caused by Enterococcus faecium
- Community-acquired and health care-associated bacterial meningitis -- a devastating and deadly disease that not only accelerates fatality rate but also causes long-term disabilities, including hearing loss, epilepsy or cognitive impairment.
“The scientific community has developed and approved new antibiotics in recent years. This is good, but unfortunately not sufficient to catch up with evolving drug-resistant bacteria, especially against those of greatest concern,” said Dr Yvan Hutin, Director of Antimicrobial Resistance at WHO.
"We need a reliable pipeline with new antibacterial agents that are innovative, affordable, and accessible to all those who need them.”
The TPPs have been developed with extensive global consultation and also define the minimum and preferred characteristics of future antibacterials against these diseases, which specifically increase the risk of immunosuppressed people and critically ill patients. The vulnerable populations are also at risk of more deaths, prolonged hospitalizations and increased demand for intensive care that in turn strains health care systems.
What The TPPs Seek
The TPPs share a blueprint which:
- prioritizes developing antibiotics for infections with high morbidity and mortality
- sets specific standards for quality, efficacy, safety, and pharmacokinetics
- includes diverse and vulnerable populations, including immunosuppressed patients, critically ill patients, neonates, and children
- promotes partnerships between public and private sector
Rising Global Antimicrobial Resistance
Antimicrobial resistance (AMR) occurs when germs develop the ability to defeat the drugs designed to kill them.
It is one of the 10 top global health threats, undermining the effectiveness of essential treatments and placing millions at risk of untreatable infections.
As per WHO data, AMR is an urgent global public health threat, killing at least 1.27 million people worldwide and associated with nearly 5 million deaths in 2019.
In the US alone, more than 2.8 million antimicrobial-resistant infections occur each year. More than 35,000 people die as a result, according to CDC's 2019 Antibiotic Resistance (AR) Threats Report.
The WHO in a 2025 report noted that one in six laboratory-confirmed bacterial infections causing common infections in people worldwide in 2023 were resistant to antibiotic treatments.
Between 2018 and 2023, antibiotic resistance rose in over 40 percent of the monitored antibiotics with an average annual increase of 5-15 percent.
Andhra milk adulteration: 13 Dead, 3 year old Among Victims

Credit: iStock
About 13 people, including a 3-year-old child, have died in East Godavari district of Andhra Pradesh in recent days, allegedly after consuming adulterated milk.
Dozens more are hospitalized and receiving treatment at hospitals in Rajamahendravaram, according to PTI news agency.
The cases first came to light on February 22, when several elderly residents were admitted to hospitals with symptoms such as anuria (absence of urine production), vomiting, abdominal pain, and kidney failure, requiring dialysis.
"The death toll in the suspected milk adulteration case in East Godavari district has reached 13, while seven persons are undergoing treatment at hospitals in Rajamahendravaram," health officials said.
Action Taken
Primary investigations indicated milk adulteration as the major reason behind the cases. High blood urea and serum creatinine levels in medical examinations of the victims also suggested possible toxic exposure.
The contaminated milk was reportedly supplied to nearly 106 families by Varalakshmi Milk Dairy in Narasapuram village of Korukonda mandal. Following the cases, the supply was immediately halted, the report said.
To curb further fatalities and hospitalization, officials have set up emergency medical camps in affected localities, with doctors and ambulances deployed round the clock.
The suspected milk vendor, Addala Ganeswararao (33), a resident of Narasapuram village, has also been taken into custody, and the associated dairy unit has been sealed.
The state Food Safety Department also plans to distribute pamphlets and booklets in educational institutions to raise awareness about identifying adulterated milk.
Recent Cases Of Contaminated Food In India
Earlier this month, the Uttar Pradesh Food Safety and Drug Administration (UPFSDA) issued 37 notices for non-compliance to sellers of substandard oil. The department also seized oil worth Rs. 6.43 crore.
Additionally, the FSSAI seized fake paneer near Noida, 1,400 kg of fake khoya in Jhansi, and 400 kg of expired ghee.
Health and Me had previously reported on FSSAI raids in Kanpur, where adulterated oil, rotten dates, and sweets were found. Bacteria were found in Amul milk packages, along with Mother Dairy and Country Delight.
Also read: FSSAI Reveals Key Tips To Keep Your Kitchen Healthy – How To Spot High Quality Vegetables?
FSSAI In Action
In February, the FSSAI launches a nationwide adulteration drive to curb adulteration in sweets, milk products, edible oils, and other festive foods.
The food regulator also led intensive inspections and on-the-spot testing through Food Safety on Wheels across States/UT.
Fisheries, Animal Husbandry, and Dairying Minister Rajiv Ranjan Singh today informed the Lok Sabha about action taken by FSSAI against the violators during 2025-26.
"A total of 1,65,747 samples were analyzed by the FSSAI between 2025-26. Of these, 28,450 were found non-conforming, with 6492 unsafe and 19,073 in the sub-standard category," Singh told the Parliament.
During the period, a total of 2,493 samples were analyzed in Andhra Pradesh. Of these, 216 were found non-conforming, with 101 in the 'unsafe' and 114 'sub-standard' category.
Travel Vaccine Update: CDC Issues Travel Advisory Against 32 Countries For Poliovirus

Credits: Canva
On March 9, the United States issues a travel advisory against global polio and listed 32 countries, including some European countries. The International travel often comes with vaccine reminder and health checks to stay safe. The Centers for Disease Control and Prevention (CDC) issued a Level 2 travel advisory for certain international destinations with circulating poliovirus. The CDC has asked travelers to ensure they are up to date on their polio vaccines.
Also Read: Harish Rana Case Brings Spotlight On How Passive Euthanasia Has Evolved Over The Years
The Destination list for global polio travel Advisory notice includes:
- Afghanistan
- Algeria
- Angola
- Benin
- Burkina Faso
- Cameroon
- Central African Republic
- Chad
- Côte d'Ivoire
- Democratic Republic of the Congo
- Djibouti
- Ethiopia
- Gaza
- Germany
- Guinea
- Israel
- Laos
- Namibia
- Niger
- Nigeria
- Pakistan
- Papua New Guinea
- Poland
- Senegal
- Somalia
- South Sudan
- Sudan
- Tanzania
- United Kingdom
- Yemen
The CDC issued a 'Level 2' advisory, which means to 'practice enhanced precautions'.
The advisory suggests that children and adults should be up to date on their routine polio vaccines. Travelers are also asked to get an inactivated polio vaccine booster if they are going to the destination that has circulating poliovirus, or have completed their routine polio vaccine series; and have not already received one adult booster dose.
Also Read: Colon Cancer Is The Leading Cause Of Death In US For People Under 50
If Polio Has Been Eliminated In The US, Then Why Do Travelers Need Advisory?
Dr Leana Wen, CNN wellness expert, who is an emergency physician and adjunct associate professor at the George Washington University said that while the US eliminated continuous transmission of polio in 1979, eradication within the country does not eliminate the risk when people travel to places where the virus is still circulating.
Speaking to CNN, Wen said that the risk for any individual traveler is usually low if they are fully vaccinated, however, from a population health perspective, it is important to take the precautionary steps. "Even a single imported case could lead to local spread in communities where vaccination coverage is low."
Types Of Notices Issued By CDC
The CDC issues four different types of notices based on the gravity of the disease spread.
Level 1 : Practice Usual Precautions
Practice usual precautions for this destination, as described in the Travel Health Notice and/or on the destination page.
Level 2: Practice Enhanced Precautions
Practice enhanced precautions for this destination. The Travel Health Notice describes additional precautions or defines a specific population at risk.
Level 3: Reconsider Nonessential Travel
Reconsider nonessential travel to this destination. The outbreak or event poses risk to travelers because limited precautions are available.
Level 4: Avoid All Travel
Avoid travel to this destination unless traveling for humanitarian aid or emergency response; there is an extreme health risk for travelers and no available precautions.
What Is Polio?
The World Health Organization (WHO) notes that it is a highly infectious disease caused by a virus that invades the nervous system and can cause total paralysis in matter of hours. The virus is transmitted by person to person spread mainly through the fecal-oral route, or less frequently, by a common vehicle, which could be either from contaminated food or water. The virus also multiplies in the intestine.
The National Institute of Health (NIH), US, notes that the virus responsible for causing Polio belongs to the Picornaviridae family.
As per the WHO, the common Polio symptoms are:
- Fever
- Fatigue
- Headache
- Vomiting
- Stiffness of the neck a
- Pain in the limbs
How Does Polio Spread?
Polio is mainly transmitted through the fecal-oral route, meaning it spreads when a person consumes food or water contaminated with the virus. It can also spread through close contact with an infected individual. The poliovirus lives in the throat and intestines of those infected, and poor sanitation, unsafe water, and inadequate hygiene greatly increase the risk of transmission, especially in communities with limited access to clean facilities.
In severe cases, polio can lead to acute flaccid paralysis, which may affect the diaphragm and throat muscles, making it difficult to breathe or swallow. Since there is no cure for polio, prevention remains the only line of defense. Raising awareness about polio vaccination is therefore essential to protect individuals, especially children, from this potentially life-threatening disease.
© 2024 Bennett, Coleman & Company Limited

