- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Malaysia Reports Record TB Outbreak With Over 3,000 Cases Amid Ramadan Celebrations
Credit: Canva
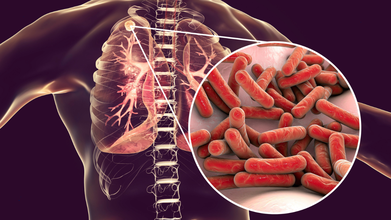
Malaysia is seeing a significant outbreak of tuberculosis (TB) -- the world’s most infectious disease -- with cases hitting more than 3,000.
As the outbreak is being reported amid ongoing Ramadan celebrations with people flocking to markets and gathering with family and friends to break their fasts, the country’s Health Ministry has urged citizens to observe precautions and maintain respiratory health, especially in crowded and enclosed spaces.
Between February 8 and 14, the ministry reported a total of 596 new tuberculosis cases nationwide, as per a statement issued on February 21. This drove the total number of TB cases to 3,161 across the country.
“It should be emphasized that Ramadan itself is not the cause of TB transmission. Nevertheless, increased social activities and gatherings during this month generally lead to greater interaction within the community,” the statement said.
Sabah reported the highest TB cases -- 755, which is nearly 24 percent of the total number of cases. It was followed by Selangor (596), Sarawak (332), and Johor (280).
A total of 2,571 cases were reported between Jan 1 and Feb 7, according to local media outlet Malay Mail.
The Health Ministry stated that “crowded, and poorly ventilated spaces” can increase the risk of transmission, “especially if there is an individual with active TB who has not yet received treatment", it said.
Thus, it advised the “public to continue practicing consistent self-care measures, including maintaining respiratory health”. These include:
- Practicing proper cough and sneeze etiquette
- Ensuring good ventilation in enclosed spaces
- Wearing a face mask if experiencing symptoms
- Seeking medical help if experiencing a prolonged cough
What Is Tuberculosis?
Tuberculosis is an airborne infectious disease that can spread when a person with active pulmonary TB coughs, speaks, or sneezes.
Common symptoms include a persistent cough lasting more than three weeks, often producing mucus or blood. These can also be accompanied by chest pain, fatigue, fever, night sweats, and unexplained weight loss.
Although highly infectious, TB does not usually spread as quickly as influenza or COVID-19 and typically requires longer and repeated exposure.
Prolonged exposure to individuals with active TB who have not yet received treatment can increase the risk of transmission.
The risk may also depend on factors like poor ventilation and immunity levels, and the presence of comorbidities like diabetes and HIV.
TB Outbreak In Malaysia: What The Experts Say?
About 85 per cent of the currently reported cases in Malaysia involve local citizens, while only 15 per cent involve foreigners, according to data from the Health Ministry.
"TB is not a new phenomenon in Malaysia’s public health landscape, as it has existed for a long time and remains an endemic disease that requires serious attention from all parties," the country’s Health Minister Dzulkefly Ahmad was quoted as saying to The Straits Times.
Health experts advised people to use a mask when in crowded places, and to seek medical help if they experience any symptoms.
"People should put on face masks while travelling and seek medical treatment early if they show symptoms," Rafdzah Ahmad Zaki, professor of epidemiology and public health at Universiti Malaya, was quoted as saying.
India to Soon Launch Free HPV Vaccine For Young Girls To Prevent Cervical Cancer
Credit: Canva
India is planning to launch a free nationwide Human Papillomavirus (HPV) vaccination program to strengthen women’s health and eliminate preventable cervical cancers in the country, official sources said today.
Human Papillomavirus is a group of common viruses, some types of which are transmitted through close skin-to-skin contact, and lead to cervical cancer.
The special vaccination program aims to protect adolescent girls against cervical cancer -- one of the most common yet preventable cancers affecting women in India.
The vaccine will be administered to adolescent girls aged 14, free of cost, at government health centers.
"The Government urges parents and guardians across the country to come forward and ensure that their 14-year-old daughters are vaccinated against HPV once the program is rolled out," the sources said.
Also Read: US FDA's New Framework Calls For Speeding Up Approvals For Rare Disease Therapies
"HPV vaccination is a powerful, preventive step that can save lives. By choosing vaccination, parents can secure a healthier, cancer-free future for their daughters," they added.
HPV Vaccine: Who Can Take It, Where To Get It From
The nationwide program, based on expert recommendations of the National Technical Advisory Group on Immunization (NTAGI), will target girls aged 14 years.
At 14, the HPV vaccine offers maximum preventive benefit, well before potential exposure to the virus.
"By prioritising prevention at the right age, the program is expected to provide lifelong protection and significantly reduce the future burden of cervical cancer in the country," the sources said.
Vaccination under the national program will be voluntary and free of cost.
The HPV vaccination will be conducted exclusively at designated government health facilities, including Ayushman Arogya Mandirs (Primary Health Centres), Community Health Centres, Sub-District and District Hospitals, and Government Medical Colleges.
The vaccine to be used is non-live and does not cause HPV infection. It is supported by more than 500 million doses administered globally since its introduction in 2006.
"India’s national program will use Gardasil, a quadrivalent HPV vaccine that protects against HPV types 16 and 18, which cause cervical cancer, as well as types 6 and 11. Strong global and Indian scientific evidence confirms that a single dose provides robust and durable protection when administered to girls in the recommended age group," the sources said.
Also Read: Fact Check: Should You Change Your Underwear In Every 6 Months?
The new program also aligns with the recommendations of the World Health Organization, which identifies HPV vaccination as a central pillar of the Global Strategy to Eliminate Cervical Cancer.
More than 90 countries worldwide are implementing single-dose HPV vaccination schedules. And about 160 countries worldwide have already introduced HPV vaccination into their national immunization schedules.
"Several countries have already demonstrated substantial reductions in HPV infection, precancerous lesions, and cervical cancer incidence following widespread vaccinations," the sources said.
Cervical Cancer: A Public Health Challenge in India
Cervical cancer remains the second most common cancer among women in India, with nearly 80,000 new cases and over 42,000 deaths reported annually.
According to scientific evidence, almost all cases of cervical cancer are caused by persistent infection with high-risk types of Human Papillomavirus (HPV), particularly HPV types 16 and 18.
In India, HPV types 16 and 18 together account for more than 80 percent of cervical cancer cases.
Although cervical cancer is preventable with vaccination and early screening, it continues to impose a heavy burden on women and families.
The impending vaccination program will help prevent the risk of HPV infection before it can progress to cancer.
US FDA's New Framework Calls For Speeding Up Approvals For Rare Disease Therapies

Credit: Canva
The US Food and Drug Administration (FDA) today recommended a new framework for accelerating approvals for the development of individualized therapies for rare and ultra-rare diseases.
The Plausible Mechanism Framework, issued by the FDA's Center for Biologics Evaluation and Research and Center for Drug Evaluation and Research, is the first such framework by the regulator in 25 years.
The draft guidance can help drugmakers with cutting-edge personalized treatments for patients with ultra-rare diseases to be used as a basis for FDA approval.
Also Read: Zepbound Outperforms Other Weight Loss Drugs, More Details Inside
The move is expected to drive innovation among drugmakers to develop life-saving treatments for patients with ultra-rare diseases, that are not only safe but also low-cost.
Importantly, with the new framework drugmakers can depend on small, well-controlled studies in cases where traditional randomized controlled trials are not possible due to small patient populations.
“President Donald Trump promised to accelerate cures for American families -- and we are delivering, especially for children with ultra-rare diseases who cannot afford to wait,” said Health and Human Services Secretary Robert F. Kennedy, Jr.
“We are cutting unnecessary red tape, aligning regulation with modern biology, and clearing a path for breakthrough treatments to reach the patients who need them most,” he added.
What Does The Framework Propose
The draft guidance focuses on genome editing and RNA-based therapies such as antisense oligonucleotides.
The therapies must target a specific genetic, cellular, or molecular abnormality.
They must also be designed to correct or modify the underlying cause of the disease. The key criteria for therapies include:
- Finding the disease-causing abnormality
- Demonstrating that the therapy targets the root cause or proximate biological pathway
- Relying on well-characterized natural history data in untreated patients
- Confirming successful target drugging or editing
“This guidance is a critical step the FDA is taking to tailor our regulatory approach to patients with ultra-rare conditions,” said FDA Commissioner Marty Makary.
“It is our priority to remove barriers and exercise regulatory flexibility to encourage scientific advances and deliver more cures and meaningful treatments for patients suffering from rare diseases,” Makary added.
What Is A Rare Disease
The World Health Organization (WHO) defines a rare disease as an often debilitating, chronic, or degenerative condition affecting 1 or fewer per 1,000 population.
Rare diseases lack of epidemiological data, are at high risk of misdiagnosis, and often also lack of effective treatments.
According to the WHO ICD-11 (International Classification of Diseases), there are over 5,500 rare diseases. It also assigns unique identifiers (URIs) to them for better tracking.
There are estimated to be over 7,000 distinct rare diseases affecting more than 300 million people globally.
Rare Disease Day 2026
The FDA hosted Rare Disease Day, a virtual public meeting, on February 23, in global observance of Rare Disease Week.
The theme “Moving Forward. Looking Ahead. An Event for Patients" explored ways to engage and collaborate with patients and their communities to support and accelerate the development of medical products for rare diseases.
Globally the day is observed on February 28 (February 29 in case of a leap year).
Zepbound Outperforms Other Weight Loss Drugs, More Details Inside

Credits: Canva
The weight loss drug competition has gotten more serious as a late-stage clinical trial compared two next generation obesity drugs and found Eli Lilly's Zepbound to produce greater result in weight loss than Novo Nordisk's much-anticipated CargiSema. The new Novo Nordisk drug was once projected to redefine the treatment landscape.
As a result, Novo Nordisk's shares have dropped by 16 per cent. However, the outcome is not just significant because of market reaction, but also because these medicines are now shaping how doctors treat obesity, a chronic disease affecting more than one billion people worldwide. The results suggest the next phase of weight-loss therapy will be decided less by hype and more by real world effectiveness.
Zepbound Outperforms Other Weight Loss Drugs: What Did The Comparison Reveal?
In the head-to-head study, patients taking CagriSema lost an average of 23 per cent of their body weight after 84 weeks. Participants treated with tirzepatide, sold as Zepbound for obesity and Mounjaro for type 2 diabetes, lost 25.5 per cent.
The gap may appear small but in clinical medicine it matters. The trial’s primary goal was to prove the new Novo Nordisk therapy was at least not inferior to tirzepatide. It failed to meet that benchmark.
Earlier trials had suggested CagriSema might rival or even surpass existing GLP-1 based drugs. However, those studies did not directly compare the medicines against each other. This time the comparison was unavoidable.
Zepbound Outperforms: Why These Drugs Matter Beyond Weight Loss
Modern anti-obesity medicines do more than reduce body fat. Doctors increasingly prescribe them to lower the risk of heart disease, diabetes complications, sleep apnea and fatty liver disease.
Zepbound belongs to a newer class of dual-action hormone therapies. It mimics both GLP-1 and GIP hormones, which regulate appetite, insulin response and metabolism.
CagriSema uses a different strategy. It combines semaglutide, the active ingredient behind earlier blockbuster treatments, with an experimental molecule called cagrilintide that targets hunger signals from another pathway.
Researchers hoped attacking appetite through multiple mechanisms would produce stronger results. The trial showed improvement but not enough to surpass tirzepatide.
Zepbound Outperforms Other Weight Loss Drugs: Did The Trial Design Effect The Outcome?
Novo Nordisk executives said the study’s open label design may have influenced results. Participants knew which drug they were receiving, which could lead to behavioral bias.
Doctors often see adherence improve when patients believe they are taking a proven therapy rather than an experimental one. The company suggested familiarity with tirzepatide may have worked in its favor.
Still, clinical researchers generally consider head-to-head trials the most reliable way to evaluate competing treatments. Even accounting for bias, the data indicates tirzepatide currently delivers slightly greater sustained weight reduction.
Zepbound Outperforms Other Weight Loss Drugs: What Does This Mean For Obesity Treatment Race?
The study highlights a shift happening in obesity care. The first generation of GLP-1 drugs proved weight loss medications could achieve double digit body weight reduction. Now companies are competing over incremental but clinically meaningful gains.
For patients, even a two to three percent difference can affect blood sugar control, blood pressure and long term cardiovascular risk. It can also influence insurance coverage decisions and treatment guidelines.
Novo Nordisk still plans to bring CagriSema to market and has filed for regulatory approval, with a decision expected by late 2026. The company is also studying higher doses and alternative dosing strategies to maximize effectiveness.
© 2024 Bennett, Coleman & Company Limited

