- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
10 Tips To Reduce Your Anxiety

Anxiety is a natural stress response that helps you keep organized, alert to potential dangers, and even calculate risks. However, if stress persists, it can lead to an anxiety disorder, which has a negative impact on mental health and well-being.
While anxiety symptoms differ from person to person, some common indicators include a racing heart, rapid breathing, restlessness, and difficulty concentrating. You may feel "butterflies" in your stomach, whilst some may experience perspiration, panic attacks, or even the desire to use the restroom. Anxiety disorders include many ailments such as generalized anxiety disorder (GAD), social anxiety disorder, and post-traumatic stress disorder (PTSD).
If you are suffering from anxiety, you may want to try natural ways for symptom management. Here are five evidence-based methods for dealing with anxiety in your daily life.
Staying Active
Exercise can effectively reduce anxiety. According to a 2021 study, people who maintain active lifestyles have a 60% lower risk of experiencing anxiety than those who live more sedentary lives. Physical activity increases brain chemicals such as serotonin, GABA, and endocannabinoids, all of which aid in anxiety reduction. Whether you favour high-intensity sports like jogging or low-impact exercises like yoga, moving can boost your mood and reduce stress.
"Staying active is the key to overall good health. The benefits of exercise for mental and physical health are enormous. However, exercising does not always entail doing intense workouts. Rather, it's critical to move your body in order to maintain your health. Engaging in enjoyable activities such as dance, gardening, hiking, and so on can help enhance your mental health. Stretching for a few minutes at work can also have a significant impact on your general mental well-being," explains Jasreen Birgi, Counselling Psychologist at LISSUN, a mental health
Limiting alcohol consumption
"According to the research, when the effects of alcohol wear off, one can experience increased anxiety. If your healthcare provider permits, occasionally drinking to relax isn't always harmful. However, you can develop a tolerance to the stress-relieving effects of alcohol once you start drinking. This may make managing stress and anxiety even more challenging," she explains.
Alcohol usage is commonly associated with anxiety, and numerous studies have shown that excessive drinking can increase symptoms. Alcohol affects neurotransmitters in the brain, causing mood swings and maybe increased anxiety. If you consume alcohol frequently, you may experience temporary anxiety increases after quitting, but these effects usually fade over time.
Reducing tobacco use
"Tobacco includes stimulants as chemicals which provide a rapid energy boost. However, the effects don't last long. After a few minutes, the chemical high from cigarettes wears off," she explains. Nicotine and other substances in cigarettes can alter stress-related brain pathways, establishing a significant relationship between smoking and anxiety. If quitting seems too difficult, try minor replacements such as gum or toothpicks, and use a support network as motivation. Research shows that stopping smoking can dramatically lower anxiety.
Additionally, you won't have to leave parties to smoke outside, which could make you feel more accepted at social occasions. Your health, happiness, and sense of self-worth can all be enhanced by these things.
Reducing Caffeine
Caffeine can trigger or worsen anxiety symptoms. According to a study, excessive coffee consumption can even lead to panic attacks in nervous people. Reduce caffeine gradually over time to avoid withdrawal symptoms, and if you're sensitive, cutting back or switching to decaf may be useful.
Prioritising sleep
Good sleep hygiene is essential for managing anxiety. The Centers for Disease Control and Prevention (CDC) advises adults to get at least seven hours of sleep every night, but many people get significantly less. Setting a consistent sleep pattern, avoiding screens before bedtime, and keeping your bedroom dark and comfortable can all help you sleep better.
How can one maintain a quality sleep? To this, Birgi explains that to maintain a quality sleep it's important to work on your nighttime routine and sleep environment. She suggests making sure to follow the same sleep schedule every day, make sure the bedroom is a de-cluttered and clean space, and avoiding caffeine in the late evening. These small movements can bring a huge change.
Practicing meditation and mindfulness
Meditation can significantly reduce anxiety by helping you to remain in the present moment. Techniques like mindfulness-based cognitive therapy (MBCT) have been demonstrated to be as beneficial as certain medications. A recent clinical trial found that an eight-week mindfulness meditation practice lowered anxiety symptoms just as effectively as the antidepressant Lexapro. "There are ample websites, videos, books, etc. available to practise mindfulness. You can also use apps like LISSUN's to start your mindfulness journey," she notes.
Maintaining a Balanced Diet
"How we feel depends on how we eat," points out Birgi, " so we should eat the nutrient-rich food that works as a mood-booster for us like berries, bananas, whole grains, etc. "
Your nutrition has a bigger impact on your mood than you may realise. Blood sugar fluctuations, dehydration, and processed foods can all contribute to anxiety. To maintain consistent energy and mood, consume a well-balanced diet rich in complex carbs, fruits, vegetables, and lean meat.
Take deep breaths
When we are anxious, our breathing becomes shallow and quick, which can lead to dizziness and panic episodes. Deep breathing exercises with calm, even breaths may help relieve symptoms and induce relaxation. This technique is simple but effective for bringing you into a stable state.
Using aromatherapy
Aromatherapy, or plant-derived essential oils, can aid with relaxation. It also improves your mood. Popular anxiety-relieving oils include lavender, clary sage, and bergamot. These oils can be inhaled or placed in a warm bath. However, it is vital to use high-quality oils and do a patch test to rule out any possible reactions.
What does the doc say about this? Birgi notes that aromatherapy is a complementary and alternative medicine (CAM) that makes use of essential oils to improve overall health. It is a natural remedy that benefits your mind, body, and spirit as a whole. In aromatherapy, essential oils are either diluted and applied topically or inhaled. Studies have shown that essential oils increase serotonin levels that help in making one feel calm and relaxed. A few effective essential oils are: Lavender, rose, jatamansi, jasmine, etc.
Drinking Chamomile Tea
Chamomile tea is a natural cure that relieves anxiety. A 2016 research on persons with generalized anxiety disorder discovered that long-term chamomile use dramatically reduced anxiety symptoms. Chamomile includes apigenin, a flavonoid that interacts with GABA receptors, which are important targets for anti-anxiety medicines. "Regular use of chamomile tea is safe and well-tolerated by the majority of people. However, pregnant women and individuals with a history of severe allergies may not be able to drink chamomile tea," she notes.
Abdominal Obesity Greater Risk Factor For Indians, says Dr. Jitendra Singh

Credit: PIB
Abdominal, also known as central obesity, poses a greater health risk than overall obesity, especially in Indians, said Dr. Jitendra Singh, the Union Minister of State (Independent Charge) for Science and Technology.
Speaking at the release of a cardiology textbook titled “Advances in Obesity and Lipid Management in CVD,” by eminent cardiologist Dr. H.K. Chopra, Singh said that even lean and thin-looking individuals often carry significant visceral fat.
Amid a rapidly growing number of chronic conditions, such as diabetes, hypertension, and cardiovascular diseases, the Minister shared that abdominal obesity is the driving factor.
"There is sufficient evidence to show that Central obesity, even in apparently non-obese individuals, predisposes to a wide spectrum of metabolic disorders including diabetes, hypertension, cardiovascular diseases, fatty liver, dyslipidemia, etc.,” Singh, who is also a diabetologist, said.
“In other words, Abdominal or Central obesity is a greater risk factor compared to overall obesity, particularly in the Indian context where even lean and thin-looking individuals often carry significant visceral fat,” he added.
The Minister reiterated the importance of balanced health practices and emphasized the need for following a “sustained lifestyle discipline, adequate sleep, and scientifically guided preventive care”.
What Is Abdominal Obesity?
Abdominal obesity refers to an excessive accumulation of visceral fat around the stomach and internal organs, such as the liver, heart, kidneys, and the mesentery of the intestine.
Unlike subcutaneous fat, which lies beneath the skin, visceral fat is metabolically active and poses greater health risks.
It can increase your risk of heart disease, type 2 diabetes, high blood pressure, stroke, and some types of cancer.

It is because visceral fat produces hormones and other substances that can cause inflammation and insulin resistance, which can lead to these health problems.
A 2024 study from the Washington University School of Medicine in St. Louis, Missouri, showed that a higher level of visceral fat was related to increased amyloid -- accounting for 77 per cent of the effect of high BMI on amyloid accumulation.
Who Is More At Risk Of Abdominal Obesity
The Minister said that while overall obesity is rising among both men and women, the prevalence of abdominal obesity remains disproportionately high and acts as an independent determinant of cardiometabolic risk. The presence of visceral fat around the abdomen, even without generalized obesity, has significant clinical implications and requires early detection and targeted intervention.
A waist circumference of more than 40 inches for men or 35 inches for women may indicate a higher risk of visceral fat accumulation.
While people with a larger waistline or pot belly are at known risk of having visceral fat, thin people too can have fat accumulation in their internal organs.
According to health experts, even people with a healthy weight can have high levels of visceral fat.
This is because visceral fat is not always visible on the outside of the body, and it can accumulate even if a person appears to be thin or in good shape.
Also read: Checking BMI For Body Weight? It Can Wrongly Mark You As Overweight or Obese, Says Study
Strategies for Successful Weight Management
To tackle obesity, one needs a holistic strategy beyond mere weight reduction. Healthy and sustainable weight reduction and improvement of health are more about body composition than mere weight. Major strategies are:
A balanced diet composed of whole foods, lean meats, and good fats in addition to physical exercise encourages sustainable weight reduction.
Resistance training helps in preserving muscle mass along with fat reduction, which improves metabolic well-being.
Prescription weight-loss medication can help manage obesity alongside lifestyle changes.
For people with severe obesity, surgeries such as gastric bypass or sleeve gastrectomy may provide significant long-term advantages.
Prioritize your metabolic health through healthy eating, portion control, and mindful eating for long-term success.
Bipolar Disorder: How Early Detection Can Help Prevent Serious Complications

Credit: iStock/Canva
Bipolar disorder is commonly misunderstood as mere mood fluctuations; however, it is a serious and complex mental health condition.
The condition presents extreme mood fluctuations — hyperactivity and impulsiveness — and depressive lows — lethargy and hopelessness.
Bipolar disorder affects over 40 million people worldwide. Yet diagnosis remains challenging, as many people remain undiagnosed or misdiagnosed for long periods. Some are treated for other mental health conditions, such as depression or ADHD, causing delays in effective treatment.
Speaking to HealthandMe, Dr. Kriti Anand, Consultant, Psychiatrist, Paras Health, Panchkula, said: “Early identification of bipolar disorder is essential for the improvement of the condition of patients. It aids in recognizing patterns early on, which helps to stabilize moods and minimize the occurrence of severe and recurring episodes”.
“With the correct identification of the condition and intervention, people can effectively maintain relationships and stay productive,” Dr. Anand added.
Importance Of Early Detection
Recognizing bipolar disorder early is critical for better outcomes. People who do not get a timely diagnosis are likely to experience more frequent and intense mood episodes, which can become harder to manage over time.
Early evaluation allows healthcare professionals to identify patterns and introduce treatments that help stabilize mood and reduce the severity of symptoms.
Notably, the experts stated that treating bipolar disorder simply as depression means that antidepressants are prescribed, which could cause a manic episode to occur.
With early diagnosis, the chances of harmful behaviors are reduced and prevent suicidal tendencies that are often a result of untreated cases of bipolar disorder.
It also enhances the quality of life, enabling patients to maintain healthy relationships, work productively, and attend to their daily responsibilities.
Early symptoms includes
- Extreme irritability, intense happiness, or sudden, uncharacteristic anger
- A sudden, unexplainable rise or decline in energy levels
- Reduced need for sleep without feeling tired or difficulty falling asleep
- Engaging in risky activities
- Racing thoughts or difficulty concentrating
It’s important to conduct a thorough evaluation to ensure an accurate diagnosis. This involves looking at the patient’s medical history and mental health history.
The symptoms are also evaluated using a structured approach. In some cases, a physical examination may also be conducted. As bipolar disorder involves long-term patterns, it’s possible to observe the patient over a long period of time.
Once diagnosed, early intervention can begin. Treatment for bipolar disorder may involve
- drugs to control mood,
- therapy to improve coping abilities,
- lifestyle habits such as sleeping and exercising regularly.
“A thorough and timely evaluation is essential for accurately diagnosing bipolar mood disorder, especially in cases where symptoms overlap with other conditions. Early intervention by mental health experts, in the form of appropriate treatment, therapy, and lifestyle adjustments, can significantly reduce complications," Surg Commodore (Dr.) Sunil Goyal (Retd), Senior Consultant - Psychiatry, Sarvodaya Hospital, Faridabad, told HealthandMe.
"This will help individuals achieve long-term stability of mood along with improved quality of life in all socio-occupational spheres," he added.
Left untreated, bipolar disorder can lead to serious problems that affect every area of your life, including:
- Problems related to drug and alcohol misuse
- Suicide or suicide attempts
- Legal or financial problems
- Trouble getting along with others
- Poor work or school performance
The experts noted that early detection of bipolar disorder is not just about diagnosis; it is about improving lives.
Identifying the condition early helps in reducing the chance of developing serious complications, decreasing the possibility of being misdiagnosed, and also allows for treatment to be delivered in a timely and appropriate manner.
Olivia Munn Opens Up About Detecting No-Symptom Breast Cancer With Lifetime Risk Assessment Test
Credit: Instagram
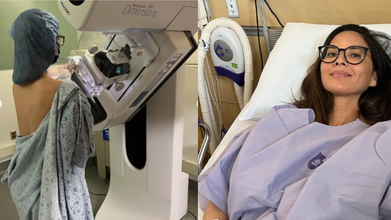
American actress Olivia Munn has opened up about her journey with deadly breast cancer, which came with no typical symptoms.
In her latest interview on CBS News Sunday Morning, the 45-year-old actress recalled being “faced with the possibility of death” in April 2023, when she was diagnosed with Stage 1 breast cancer.
Importantly, the actress had no symptoms, and even tests like a mammogram and ultrasound gave her a clean chit.
"No symptoms. And I had a clear mammogram and a clear ultrasound," Olivia was quoted as saying.
However, the condition was detected after taking the Lifetime Risk Assessment test -- a free online Q&A that gave her a high score estimating the risk of developing breast cancer in a lifetime. The test marked any score above 20 percent as a high risk. Munn's risk score was 37.3 percent.
The online test — Tyrer-Cuzick Risk Model — is publicly accessible and widely recommended by experts, and it calculates a woman’s five-year and lifetime risk of developing breast cancer using a combination of factors like age, family history, genetics, reproductive history, and more.
Post the assessment, she took "an MRI, which led to an ultrasound, which then led to a biopsy," she explained.
The biopsy showed that she had what she described as "an aggressive, fast-moving cancer" in both of her breasts.
Once she learned the diagnosis, she fought back with everything she had. She got a double mastectomy, an ovariectomy, and a partial hysterectomy. Now her risk score is zero.
Instead of recovering quietly, Olivia made it her mission to raise awareness about the condition — posting about her cancer on social media and telling the world about the risk assessment test.
In the years since Munn started sharing her story, the number of women taking the test has increased by 4,000 percent, the report said.
"Knowing that it's really changed so many people's lives. It's been the most amazing thing. There's no way I could have ever predicted it," she said.
In 2025, Olivia’s mother, Kim, was also diagnosed with breast cancer after taking the same risk assessment test.
In an Instagram post, Munn said her mother was diagnosed with Stage 1 HER2-positive breast cancer, a fast-growing but often treatable type of the disease. Her diagnosis came after Munn encouraged her mom and sister to take a free online breast cancer risk assessment.
Also read: Amanda Peet Opens Up About Breast Cancer Battle, Shares Toughest Moment
What Is A Lifetime Risk Assessment Test?
The MagView Tyrer-Cuzick Risk Assessment Calculator is an online tool that helps one calculate their lifetime risk of developing breast cancer.
The tool urges people to reach out to their healthcare professional in case they have any questions about their risk of developing breast cancer and what the best options are for breast cancer screenings or genetic counseling they may have.
Olivia stressed that any woman over 30 should take the test, and if their risk is above 20 percent, they should ask their doctor for a breast MRI.
Also read: Christy Carlson Romano’s Cancer Test Result Shows Why Regular Screening Is Important
Who Should Get Breast Cancer Screening Done?
According to the American Cancer Society, you are considered to be at average risk if you do not have a personal history of breast cancer, a strong family history of it, or a known genetic mutation (like in the BRCA gene) that increases your risk.
This also applies if you have not had chest radiation before the age of 30. These are the breast cancer screening recommendations for women who are at average risk.
Ages 40-44: You have the choice to start getting a mammogram every year.
Ages 45-54: You should get a mammogram every year.
Ages 55 and older: You can switch to getting a mammogram every other year, or you can choose to continue getting one every year.
You should continue to get screened as long as you are in good health and are expected to live at least 10 more years.
© 2024 Bennett, Coleman & Company Limited

