- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
20% Americans Are Job-Hopping For Ozempic; Is It A Health Win Or A Risky Shortcut?

Credits: Freepik
As anti-obesity medications like Ozempic and Wegovy become increasingly popular, American employees are making career choices based on access to them. A recent poll found that 1 in 5 Americans would be willing to switch jobs to get insurance coverage for these in-demand medications. But as the craze for GLP-1 drugs takes hold of the workforce, the question is—are we becoming a healthier society, or merely taking a medically approved shortcut?
In a world where job benefits such as remote work, unlimited time off, and child care allowances drive the benefits discussion, there's a new player in the mix: weight loss drugs. A 2024 survey by 9amHealth found that 67% of Americans would remain at a job they disliked if it included retaining access to drugs such as Ozempic and Wegovy. And if workplaces don't pay for them? 20% of respondents would actively seek another job.
This behavior is not without purpose. Out-of-pocket expenses for GLP-1 medications such as Ozempic can run over $1,000 monthly. Confronted with this expense, some users report skimping on necessities such as food and entertainment in order to pay for their monthly supply. Coverage under employer-sponsored insurance, thus, becomes not only a benefit—but a necessity.
What is the Frenzy of GLP-1 Drugs?
Contrary to older weight loss drugs that normally achieve a 5% drop in body weight, newer GLP-1 medications provide up to 20% weight loss or more. Their impact has been so significant that Science identified GLP-1 medications as the 2023 "Breakthrough of the Year." The medications act by emulating a hormone that controls blood glucose and hunger, leading to both enhanced metabolic function and reduced hunger.
Initially approved for type 2 diabetes, Ozempic and other medications such as Mounjaro have been used extensively off-label for weight loss, driving stratospheric demand. In February 2023 alone, over 373,000 prescriptions for Ozempic were filled—a 111% increase from the year before.
Ozempic: High Demand, Higher Costs, and Potential Misuse
But with increasing demand comes increasing expense. Ozempic and Mounjaro were among 800 drugs that experienced a median list price increase of 4.5% this year, the Wall Street Journal reported. Some large institutions, such as Ascension Health and the University of Texas System, have even withdrawn coverage in light of skyrocketing prices—reporting a 233% increase in expenditures related to them.
According to the World Health Organization, over 80% of people with type 2 diabetes are overweight or obese. Chronic inflammation caused by excess fat, especially visceral fat, disrupts how insulin functions. Additionally, high levels of circulating fatty acids can impair insulin sensitivity.
Dr. Arush Sabharwal, Bariatric & Metabolic Surgeon explains, "This is where GLP-1 receptor agonists like Ozempic (semaglutide) come into the picture. Originally approved for type 2 diabetes, Ozempic also promotes weight loss by suppressing appetite and slowing gastric emptying. Clinical trials have shown significant weight reduction and improved blood sugar control in patients using it."
"Though Ozempic is not a magic solution, still it denotes a powerful association between the role of weight management and type 2 diabetes. For those who are overweight, lifestyle modifications are important, after seeking professional advice from a weight loss expert like a doctor/bariatric surgeon/certified nutritionist."
There's also an increasing worry about the abuse and stigma surrounding these medications. Although Ozempic is now a cultural buzzword and an alleged "magic bullet" for rapid weight loss, physicians warn that it's not a sustainable solution in and of itself. "Without robust support for behavior change, weight loss is generally short-term and tends to be followed by weight regain," experts in endocrinology and metabolic care stated.
In fact, 38% of respondents to the 9amHealth poll confessed to exploring black market sources prior to settling on FDA-accepted treatments—courageous behavior that reveals the desperation and lack of education about obesity management.
Why Obesity is an Expensive, Long-Term Health Problem Employers Can't Dismiss?
Over 40% of American adults qualify for the CDC's definition of obesity, a BMI of 30 or more. The disorder is a significant cause of comorbidities such as type 2 diabetes, hypertension, and cardiovascular disease—a combination frequently called "cardiodiabesity." Alone, obesity costs the U.S. healthcare system $173 billion per year and accounts for $6.38 billion in lost productivity in the workplace.
With these daunting numbers, employers are finally realizing that managing obesity up front may be cheaper in the long term. In 2023, only 25% of employers were covering GLP-1s, but this might increase to 43% in 2024, says health consulting company Accolade.
But selling prescription medications without complementing them with health support is a lost chance. Specialists recommend a combined approach—of accessible pharmaceuticals along with dietary advice, exercise routine, psychiatric help, and regular medical follow-up.
Medical Experts Call for Balanced Approach
While the temptation of GLP-1 medications can be tempting, specialists advise against its use as a single solution. Pills can trigger weight loss, but long-term health is derived from behavioral modification. Fitch and others suggest addressing obesity as any chronic illness, with long-term, multidimensional management.
Dr. Arush emphasises, "There is a strong connecting link between type 2 diabetes and obesity. When there is excess deposition of abdominal fat, it makes the body insulin resistant. This is a condition wherein the body finds it hard to respond to insulin hormone and this in turn, surges the blood sugar levels. Ultimately this makes the body predisposed to type 2 diabetes."
Employers who are seriously interested in tackling obesity in the workplace need to look beyond providing coverage. They must make available comprehensive health packages that consist of individualized interventions, ongoing tracking, and lifestyle change support systems for enduring change.
For the time being, it appears GLP-1 medications are not only changing waistlines, but also workplaces. Workers are willing to make drastic life adjustments—including job-hopping—for access to these drugs. Whether this is a significant shift in corporate healthcare priorities or a troubling shortcut remains to be determined.
One thing is certain, the workplace is emerging as a central front in the battle against obesity. And as the stakes grow higher, so does the onus on employers to provide intelligent, sustainable, and equitable solutions for the long-term health of their employees.
Dr. Arush Sabharwal is a Bariatric & Metabolic Surgeon at SCOD Clinic in India
Is Chest Pain The Only Sign Of Heart Disease?

Not just chest pain, but even jaw pain can be associated with heart disease. (Photo credit: iStock)
There are many myths linked to heart health that can mislead people and prevent them from seeking timely help. This article helps to debunk the myths and keep the heart healthy. It is time to prioritize heart health. Dr Rahul Gupta, Director of Interventional Cardiology and Structural Heart Program, Gleneagles Hospital, Parel, Mumbai, spoke about the common myths about heart disease and listed the facts as well.
Heart problems are commonly seen in people of all age groups. However, heart health is often surrounded by myths and misconceptions that can lead to confusion and poor lifestyle choices in people. So, heart health depends on multiple factors, including diet, activity, stress, and overall lifestyle, and not just one or two habits. Here, the expert helps to debunk the myths associated with heart health and improve the quality of life.
Dispelling myths surrounding heart health
Myth 1: Only older people are at risk of heart problems
Fact: People commonly believe that heart problems can only happen in old age. However, currently, a large number of youngsters aged 25-35 are also struggling with heart issues such as heart attacks and heart failure because of stress, unhealthy diets, and lack of exercise. So, heart problems are not limited only to older people. Anyone, irrespective of their age, can suffer from them. Hence, there is a need of the hour to go for regular heart check-ups and to initiate timely treatment for heart problems.
Myth 2: If you are fit, your heart is SAFE
Fact: So, being physically active is important, but it does not reduce the chances of heart problems. Be attentive to the family history, genetics, and other factors such as high cholesterol or even stress. So, go for cardiac screening on a yearly basis to know the status of your heart health. Discomfort in the arms, jaw, or back and light-headedness can also mean that your heart is in danger.
Myth 3: Heart disease is only seen in men
Fact: Shockingly, heart disease also causes higher morbidity and mortality rates in women. The symptoms seen in women linked to heart disease are dizziness, palpitations, and even giddiness. Hence, women should also focus on their heart health. Stay alert, stay safe!
Your heart health matters. By understanding the facts and making informed choices, it is possible for everyone to protect their heart and overall well-being.
Beyond Medicines: How DBS Surgery Is Helping Parkinson’s Patients Reclaim Movement and Independence
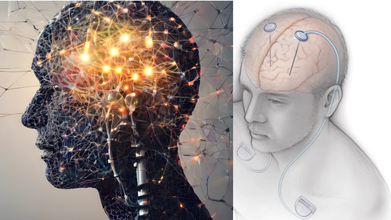
Credit: Canva/ Cleveland Clinic
Parkinson's disease is a condition that affects people with Parkinson's ability to move and do things on their own. People with Parkinson's disease will find that it gets worse over time. At first, medicines can help people with Parkinson's disease.
After a while, these medicines might not work as well as they used to for people with Parkinson's disease. Some people with Parkinson's disease might even feel bad because of the medicines they are taking for Parkinson's disease.
That is when doctors might suggest something called Deep Brain Stimulation, or DBS for short, to people with Parkinson's disease. Deep Brain Stimulation is a kind of help for people with Parkinson's disease.
What Is DBS?
DBS is a kind of surgery where doctors put wires into the brain. These wires are connected to a device that is put under the skin in the chest. This device sends messages to the brain to help it work better. The brain can get mixed up. Cause people to shake or move slowly. The messages from the device help fix that.
One of the things about DBS is that it can help people move better when medicines are not working well. People might shake less. Feel less stiff. They might even be able to take medicine, which can be good because it can reduce the side effects.
It is very important to remember that DBS is not a cure for Parkinson's disease. It does not make the disease go away. It can help people do things on their own again. Many people who have DBS say they can eat, walk, and dress themselves better. These are things that can be very hard for people with Parkinson's disease.
DBS Promising For Parkinson's Patients
Doctors have to be very careful about whom they recommend DBS to. It is usually for people who take medicines for Parkinson's disease. The medicines do not always work well. The doctors, surgeons, and therapists all have to work to make sure everything goes well.
Exciting things are happening with DBS. Soon, there might be devices that can adjust on their own to help people more. This means that people with Parkinson's disease might have more hope for feeling better.
DBS is a step forward from just taking medicines. It helps people take control of their bodies again. It helps them feel more independent and dignified. That can make a difference in their daily lives. Parkinson's disease is a hard condition to deal with, but with DBS, people might feel like they can do things again. They might feel like they have their life back. DBS is a promising treatment for people with Parkinson's disease.
Not Diabetes or Obesity: Expert Says Chronic Stress Is The New Lifestyle Disease

Chronic stress raises cortisol levels in the body. (Photo credit: iStock)
Work, school, competition—stress appears to be inevitable these days. Across age groups, many are dealing with it in some form or the other, but unfortunately stress never stops at just headaches or fatigue. It has direct effects on an individual's health through causing disease (such as cardiovascular problems); it also has indirect effects on health by negatively influencing other health behaviors such as physical activity and sleep. It is also vital to note that stress is one of the leading health risks for people in the work environment. Healthcare professionals are advised to consider both major stressors and those that occur regularly. Further discussion about stress reduction strategies is provided.
Dr Anshuman Kaushal, Director of Robotic GI, Minimal Access & Bariatric Surgery at CK Birla Hospital, Gurugram, in an interview with Health and Me, spoke about the long-term effects of chronic stress and why it can be termed a lifestyle disorder.
Mechanisms of Chronic Stress
Exposure to certain stressors activates the HPA axis, and as a result, adrenaline and cortisol are released. While these hormones play a crucial role in survival during emergencies, they can result in serious health problems when continuously present in the body. Some of the most common consequences of stress are low immunity, insulin resistance, or inflammation. It can over time result in hypertension or heart disease.
Lifestyle as the Main Cause
With growing rates of urbanisation, competitive workplaces, financial issues, and the development of technology leading to a permanently accessible Internet, the boundaries between working time and time for rest have been blurred entirely. Moreover, an insufficient amount of sleep, poor sleeping habits, and a sedentary lifestyle cause stress as well. The young generation in India has become victims of stress-related disorders the most.
Identification of the Symptoms
One of the major challenges when identifying chronic stress cases lies in the subtlety of the condition. The list of symptoms includes constant fatigue, irritability, concentration issues, headaches, tight muscles, and insomnia. Other symptoms of the condition include gastrointestinal disorders such as acid reflux, bloating, and loss of appetite that are hardly ever associated with stress.
Long-term effects of stress
Chronic stress may appear harmless, but the truth is quite contrary. When an individual is stressed for too long without controlling it, it may result in anxiety disorders like depression. Physiological side effects of stress are:
- Poor immunity
- Inflammation
- Obesity
- Diabetes
- Weakened memory
- Mood swings
What makes chronic stress a lifestyle disease?
While most lifestyle disorders are caused by environmental factors and behavioural alterations, it can be termed a lifestyle disease. These disorders are progressive and require constant intervention in the form of medication or meditation.
Managing chronic stress
Doctors say that it takes a comprehensive strategy to reduce cortisol levels in the body and uplift mood. For instance, workouts like weight training or yoga are known to increase levels of happy hormones, thereby reducing stress. Breathing exercises and meditation, too, have a positive impact on mental health. Experts recommend combining them with nutrition, proper sleep, and socialising.
Early diagnosis matters
Chronic stress is not just a symptom of modern life but also a key health problem. Recognising it as a health issue and addressing it helps combat the long-term consequences well in time. And with continued changes in lifestyle habits and patterns, a lifestyle disease like chronic stress can also be brought under control for the better.
© 2024 Bennett, Coleman & Company Limited

