- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Ammonia Surge Triggers Delhi Water Crisis: How To Detect Contamination And Stay Safe

Credits: AI Generated
High ammonia levels in the Yamuna, along with reduced water supply from Haryana via the Munak Canal, have triggered a water shortage across several parts of Delhi. Seven out of the city’s nine water treatment plants have been impacted. Delhi’s largest facility at Wazirabad, which normally supplies around 140 MGD (million gallons per day), has been shut down entirely. Meanwhile, the Chandrawal plant is operating at only half its capacity and is supplying close to 100 MGD to the capital.
Delhi Water Crisis
Localities facing disruptions include IGI Airport, Dwarka, Shalimar Bagh, Sultanpuri, Raja Garden, Rajouri Garden, Karala, Bawana, Prashant Vihar, Madhu Vihar, Mangolpuri, Paschim Vihar, Mayapuri, Janakpuri, and nearby areas. In a statement, the Delhi Jal Board (DJB) said, “To make up for the diversion, Haryana is supplying water to DJB. Residents are advised to use water carefully during this period.” Officials have indicated that the water crisis could persist until February 4, 2026.
What Happens When Water Has High Ammonia Content?
Elevated ammonia levels in drinking water can pose serious health concerns, especially when concentrations cross safe limits such as 0.5 ppm (parts per million). Here’s how excess ammonia can affect the body.
1. Respiratory Issues
Ammonia can irritate the airways, leading to symptoms like coughing, a runny nose, chest discomfort, and difficulty breathing if consumed or inhaled from contaminated water. People with asthma or existing lung conditions may experience aggravated bronchitis or face a higher risk of pneumonia.
2. Neurological Effects
Ammonia acts as a neurotoxin and can enter the bloodstream, interfering with normal brain function. This may result in headaches, dizziness, confusion, or trouble concentrating. In cases of heavy exposure, it can cause nausea, vomiting, or poisoning accompanied by breathing distress.
3. Organ Damage
Long-term exposure to ammonia can strain the kidneys by increasing their workload, which may eventually impair function. It can also raise nitrite and nitrate levels in the body, increasing the risk of vascular problems, and has been linked to reproductive concerns such as infertility or low birth weight.
4. Skin and Eye Irritation
Direct contact with water containing high ammonia can irritate the skin, eyes, and mucous membranes, sometimes causing rashes or conjunctivitis. Children, pregnant women, and older adults are especially vulnerable and should be extra cautious.
How To Check For Ammonia In Water At Home?
There are a few simple ways to identify possible ammonia contamination at home without laboratory testing.
Indicators
Ammonia gives off a sharp, pungent smell often compared to fish or household cleaning agents, which can be noticeable even at low levels of 0.5–1 mg/L. The water may also taste bitter, earthy, or moldy. If you notice these signs, avoid using the water. Checking the pH can also help, as ammonia can push pH below 7, making the water more acidic. pH test strips are an easy option for this.
Chlorine Residual Test
When ammonia reacts with chlorine, it forms chloramines, which lowers free chlorine levels to below 0.4 mg/L. You can test tap water using pool test strips or chlorine kits. Low readings may point to the presence of ammonia and serve as a useful indirect indicator in treated water supplies.
Safety Tips And Precautions
If you live in an area at risk of ammonia contamination, taking precautions is essential to reduce health issues such as irritation, nausea, or neurological symptoms. Here are some practical steps to follow.
1. Use Certified Filtration
Install reverse osmosis (RO) or activated carbon filters that are certified to remove ammonia and chemical contaminants, such as those meeting NSF/ANSI 58 standards. These systems are effective at trapping ammonia ions, unlike basic filters, and make drinking water safer for daily use.
2. Avoid Boiling Alone
While boiling kills bacteria, it can cause ammonia to vaporise, concentrating it in the remaining water and steam. Avoid inhaling the vapours or relying on boiling alone. If boiling is unavoidable, combine it with proper filtration or allow the water to cool uncovered in a well-ventilated space so gases can dissipate before storage.
3. Safe Handling
Always test water if contamination is suspected. In case of exposure, rinse skin or eyes with lukewarm water for 15–30 minutes and seek medical attention if there are burns or if the water has been ingested. Keep ammonia-based cleaning products away from food preparation areas and out of children’s reach to prevent accidental mixing or exposure.
Nipah Virus Outbreak India: How Contagious Is It And Who Is Most At Risk?
Credits: Canva
Indian health authorities are moving quickly to control a Nipah virus outbreak after five confirmed cases and the quarantine of nearly 100 people in West Bengal. Officials said three fresh infections were detected earlier this week, adding to two earlier cases involving a male and a female nurse. Both nurses were employed at a private hospital in Barasat, close to Kolkata. According to Press Trust of India, the newly confirmed patients include a doctor, a nurse, and another healthcare worker.
Nipah Virus Outbreak India: What Is Nipah Virus?
Nipah virus (NiV) is a zoonotic infection, meaning it can spread from animals to humans. Fruit bats, also known as flying foxes, are the primary carriers, but the virus can also be transmitted through pigs and other animals such as goats, horses, dogs, or cats. According to the Cleveland Clinic, infection can occur when:
- People or animals come into contact with bodily fluids like blood, urine, stool, or saliva from an infected animal.
- People consume food items contaminated by infected animals.
- People have close contact with someone infected with Nipah virus, most often while providing care.
The most effective way to reduce the risk of Nipah virus is to avoid contact with sick animals, particularly bats and pigs, in regions where outbreaks have been reported. It is also advised to stay away from foods that animals could contaminate, such as raw date palm sap or partially eaten fruit. Since Nipah can spread between people through bodily fluids, caution is essential when interacting with infected individuals.
Nipah virus can lead to symptoms ranging from mild illness to severe disease, including encephalitis, which can be fatal. At present, there is no specific drug or vaccine available, and treatment focuses on managing symptoms and providing supportive care.
Preventing Nipah virus relies on strict infection control practices, including the use of protective gear, proper surface disinfection, and avoiding areas or animals linked to known outbreaks.
Nipah Virus Outbreak India: Where Is Nipah Virus Found?
Nipah virus outbreaks are reported almost every year in parts of Asia, mainly in Bangladesh and India. The virus was first identified in 1999 during an outbreak in Malaysia and Singapore that caused around 100 deaths. To stop the spread, more than one million pigs were culled, resulting in significant economic losses. Since then, roughly 20 outbreaks have been recorded.People traveling to countries prone to Nipah outbreaks, such as Bangladesh, Malaysia, Singapore, or India, are advised to take extra precautions. Other regions, including Cambodia, Indonesia, Madagascar, the Philippines, and Thailand, may also be at risk because the bat species responsible for spreading the virus are present there.
Nipah Virus Symptoms and Causes
Early signs of Nipah virus infection may include:
- Fever
- Headache
- Difficulty breathing
- Cough and sore throat
- Diarrhea
- Vomiting
- Muscle aches and extreme weakness
Symptoms usually appear within four to 14 days after exposure. Many people first experience fever or headache, followed by breathing problems such as cough or shortness of breath.
In more serious cases, the infection can progress to encephalitis, a dangerous brain inflammation. Severe symptoms may include:
- Confusion or altered mental state
- Slurred speech
- Seizures
- Coma
- Severe breathing distress
Experts do not fully understand why some people develop serious illness while others experience mild or no symptoms at all.
Nipah Virus: How Contagious Is It?
Nipah virus is infectious and can spread from animals like bats and pigs to humans through bodily fluids or contaminated food. It can also pass between people through close contact, especially in caregiving settings. While it can spread via respiratory droplets in enclosed spaces, it is not considered highly airborne and usually requires close, prolonged contact for transmission. Common routes include direct exposure to infected animals or their fluids, consuming contaminated fruits or date palm sap, and contact with bodily fluids such as saliva, urine, or blood from an infected person.
Nipah Virus Outbreak India: Who Is Most At Risk?
People most at risk of Nipah virus are those who are more likely to come into close contact with infected animals or patients. This includes:
- Healthcare workers caring for Nipah patients, especially without proper protective equipment
- Family members and caregivers who have close physical contact with infected individuals
- People living near bat habitats, particularly fruit bat roosting areas
- Those who consume contaminated food, such as raw date palm sap or fruits partially eaten by bats
- Farmers, animal handlers, and slaughterhouse workers who work with pigs or other animals that can carry the virus
- Residents of outbreak-prone regions in India and Bangladesh, where Nipah cases recur
- People with weak immunity, who may develop more severe illness after infection
- Close, prolonged contact is the biggest risk factor. Casual contact in public spaces is far less likely to spread the virus.
Double Covid Surging Across UK, Doctor Urges Immediate Vaccination

Credits: Canva
A GP has warned that people can catch Covid more than once in a short span, including while they are still unwell from a previous infection. In some cases, this may even involve picking up two strains of the virus at the same time, a situation doctors are calling “double Covid”.
Doctor Warns of ‘Double Covid’ as UK Cases Rise
New figures from the UK Health Security Agency show confirmed Covid cases have risen by 11 per cent. In the week leading up to January 9, 51 deaths were recorded and more than 500 people were in hospital with the virus.
Can You Catch Covid Twice at the Same Time?
Speaking to the BBC, GP Dr Nish Manek said it is possible to be infected again while still dealing with ongoing symptoms, including long Covid. She explained that having long Covid does not provide immunity against reinfection.
According to Dr Manek, protection from a previous infection or vaccination reduces over time. New variants are also better at evading the immune system, making repeat infections more likely.
Why Long Covid Does Not Protect You
Dr Manek said immunity can fade within months, leaving people vulnerable. New strains of the virus, including recent Omicron-related variants circulating in 2025, are able to bypass existing immune defences.As a result, someone managing long Covid symptoms may still catch Covid again. A fresh infection can trigger a relapse of symptoms or slow down recovery.
She added that a positive test may reflect either the same strain or a new variant. In both cases, it is still Covid and should be taken seriously.
Vaccines Still Reduce Severe Illness
Dr Manek stressed that vaccination remains important. While vaccines may not fully prevent infection, they significantly reduce the risk of severe illness and hospitalisation.
She said Covid continues to change and remains present in the community. Simple protective steps still matter, including testing when unwell, wearing masks in crowded indoor settings, and staying up to date with vaccinations.
Which Covid Variants Are Circulating Now
As of January 2026, Covid continues to evolve in the UK. One of the most common strains currently in circulation is NB.1.8.1, often referred to as the Nimbus variant.Latest Covid Symptoms to Watch For
Doctors say symptoms linked to current variants often affect the upper respiratory tract and can feel similar to a bad cold or flu.
Commonly reported symptoms include a very painful sore throat described as feeling like razor blades, a hoarse voice with swollen glands, blocked or runny nose, sneezing, and extreme tiredness. Fever, a persistent cough, and body aches are still widely seen.
Loss of taste or smell is now reported far less often than during the early stages of the pandemic.
Who Is Eligible for a Covid Vaccine in the UK
The UK has moved to a targeted vaccination approach, focusing on those most at risk of serious illness.
The current winter vaccination programme is coming to an end. The final date to receive this dose is January 31, 2026. You are eligible if you are aged 75 or over, live in a care home for older adults, or are aged six months or older and immunosuppressed due to medical treatment or long-term conditions.
A spring booster programme has been confirmed for 2026. Appointments are expected to open in late March, with vaccinations starting from April 13. Eligibility criteria remain the same as the winter programme.
How To Book Your Covid Vaccine?
Eligible individuals do not need to wait for an invitation. Vaccinations can be booked online through the NHS website, via the NHS App, by calling 119 for free, or by visiting a walk-in pharmacy or clinic.Doctors continue to urge those eligible to get vaccinated while doses are still available.
Doctors Warn: This Skin Pattern Could Signal Blocked Arteries
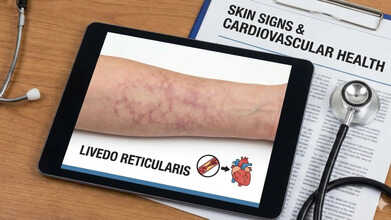
Credits: AI Generated
A lace-like pattern appearing on the skin may sometimes point to blocked arteries. Health experts warn that this netted discoloration can, in certain cases, be linked to damage in tissues and organs.
Heart and circulatory diseases remain the leading cause of death worldwide, claiming close to 18 million lives every year. This group includes serious conditions such as stroke, coronary artery disease, and heart failure.
An Unusual Skin Pattern That Could Signal Artery Blockage
In the UK, cardiovascular disease is responsible for around one quarter of all deaths. Because of its scale and severity, recognising warning signs early can save lives.
Most people are familiar with common symptoms like chest pain. What is less widely known is that heart-related problems do not always announce themselves clearly. Some signs are subtle and can appear in unexpected places, including the skin.
What Is Livedo Reticularis?
The American Academy of Dermatology highlights one particular skin pattern that may be linked to heart and blood vessel problems. A blue or purple, net-like discoloration on the skin can sometimes indicate reduced blood flow or a blocked artery.
This condition is known as livedo reticularis. It is believed to occur when small blood vessels near the skin tighten suddenly or when circulation close to the skin becomes uneven.
When the Pattern Is Usually Harmless
In many cases, livedo reticularis is not a cause for concern. Cold temperatures are a common trigger, and the pattern often fades once the skin warms up. Certain medications can also produce this effect without posing a serious health risk.
According to the dermatology body, some people notice the pattern when they feel cold, only for it to disappear as their skin warms. When medication is responsible, it is generally considered harmless.
When It May Point to a Serious Condition
In some situations, the same skin pattern can be linked to a condition known as cholesterol embolisation syndrome. This happens when tiny arteries become blocked by cholesterol particles.
Such blockages can interfere with blood supply and lead to damage in tissues and organs. For this reason, experts stress the importance of medical evaluation to rule out any underlying or undiagnosed disease.
When to See a Doctor
The Mayo Clinic advises seeking medical advice if the mottled skin does not fade with warmth or if it appears alongside other worrying symptoms. You should also consult a doctor if painful lumps or sores develop in the affected area, if you already have a condition that affects blood flow to your limbs, or if you have a connective tissue disorder and notice new skin changes.
Doctors also caution that a similar-looking condition, called livedo racemosa, is more often linked to serious underlying illnesses.
Other Warning Signs of Heart Disease
Skin changes are only one possible clue. Other symptoms linked to heart disease include chest discomfort, pain or weakness in the arms or legs, shortness of breath, irregular heartbeats, dizziness, unusual tiredness, and swelling in the limbs.
If any of these symptoms feel concerning or persistent, it is important to speak to your GP for further advice.
© 2024 Bennett, Coleman & Company Limited

