- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Bjorn Borg Opens Up On His Struggle With Drug Overdose

Credits: Wikimedia Commons
In his new autobiography Heartbeats, Björn Borg strips away the icy façade that once defined him on court. The book, set for U.S. release on 23 September by Diversion Books, begins with a raw account of his 1990s hospitalization after overdosing on “alcohol, drugs, pills, my preferred ways of self-medication.” It ends with a prostate cancer diagnosis, which he now faces in remission.
“It’s good,” the 69-year-old told The Associated Press in a recent video interview from his Stockholm home, “to have a good beginning and a good ending.” The 292-page memoir is a departure from the silence he cultivated during and after his playing days, offering stories of love, regret, excess and survival.
Walking away from tennis at 25
Borg retired shockingly early, at just 25, after losing both the Wimbledon and U.S. Open finals in 1981 to his rival John McEnroe. While others saw a glittering career still ahead, Borg knew otherwise.
“My head was spinning,” he said. “And I knew I’m going to step away from tennis.”
That decision, he explains, left him unmoored. He returned briefly to the professional circuit in the early 1990s but never again at Grand Slam level. What followed was a long descent into substance abuse.
On court, Borg was famously known as “Ice-Borg”, a man of composure who never flinched. But he reveals that this restraint was a learned skill, born from shame as a 12-year-old banned by his local club for bad behavior.
Off court, that discipline dissolved. By his own account, panic attacks and depression pushed him into cocaine use starting in 1982. “The first time I tried cocaine,” Borg writes, “I got the same kind of rush I used to get from tennis.”
The rush quickly became reliance. “It really destroys you,” Borg said of drugs. “I was happy to get away from tennis, to get away from that life. But I had no plan what to do. I had no people behind me to guide me in the right direction.”
Also Read: “Day by day, year by year,” Is How Bjorn Borg Takes Life After His Prostate Cancer Diagnosis
Overdoses and shame
Borg details two overdoses that landed him in hospital, one in Holland in the early 1990s, and another in 1989 in Milan, which he insists was an accident rather than a suicide attempt. The darkest moment, he admits, came when he awoke in a hospital bed to see his father looking down at him.
“That was the worst shame of all,” he writes.
These incidents, combined with spiraling personal struggles, forced Borg to confront how far he had fallen from the grace of his early sporting stardom.
Name: drops and surreal encounters
Heartbeats is not a typical sports autobiography. Alongside harrowing stories of addiction and recovery, Borg mixes in extraordinary encounters: a water-skiing shoulder injury before the 1977 U.S. Open, receiving death threats during the 1981 U.S. Open, being robbed at gunpoint after accepting payment in cash, and facing coin-throwing spectators in Rome.
The book name-drops Donald Trump, Nelson Mandela, Tina Turner, Andy Warhol, Yasser Arafat, and even “my old friend Hugh Hefner.” These anecdotes place Borg not only in tennis history but within a swirl of 20th-century celebrity and politics.
“People will be very surprised what really happened,” Borg said. “For me to come out after all these years, all I went through, I went through some difficult times, it’s a relief for me to do this book. I feel so much better. No secrets anymore.”
A candid look at survival
The memoir also traces his strained relationships, with parents, with his children, and with his own sense of identity after leaving professional sport. By his account, retirement robbed him of purpose, and drugs filled the void.
Borg acknowledges that his descent was partly a reaction to the structure of his tennis life: “I was happy to get away from tennis … but I had no plan what to do.” Without the rhythm of tournaments and training, he spiraled.
Yet he insists he has rebuilt his life. Now, after cancer treatment, he says he is proud of where he stands: sober, reflective, and still connected to the sport he once dominated.
Looking ahead, without secrets
For Borg, writing Heartbeats is as much about catharsis as it is about record-keeping. He admits that his privacy once shielded him from scrutiny but also kept him trapped in silence about his struggles. Now, at 69, he frames his story differently: beginning with a near-death overdose, ending with cancer remission, and filling the middle with unvarnished honesty.
“I went through some difficult times,” he said, “but now I feel so much better.”
Björn Borg’s memoir offers not just the tale of a tennis great, but a portrait of a man forced to confront addiction, shame, and mortality, and who, at last, seems at peace.
Obesity, Diabetes, and Kidney Disease: The Dangerous Health Triangle
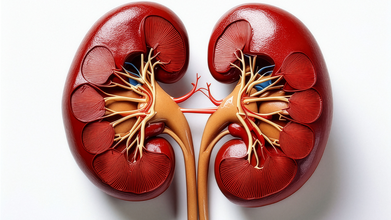
Credit: Canva
Obesity, diabetes, and kidney diseases are three serious health issues that are linked to one another. These health issues have created a dangerous health triangle that is harming millions of people across the world.
When any of these health issues appear in a person’s health profile, the chances of developing the other health issues are high. These health issues are interconnected and may have a serious impact on a person’s health.
Obesity is a serious health issue that increases the risk of developing diabetes. Obesity increases the risk of developing diabetes because the extra fat accumulated in the abdomen interferes with the production of the hormone called insulin.
The hormone insulin helps the body regulate the levels of glucose present in the blood. If the levels of glucose are not regulated in the blood, a person may develop diabetes. If diabetes is not controlled over time, it may harm the kidneys.
Obesity Affects Kidney Function
The kidneys have an important function in filtering out wastes and extra fluids from the blood. However, high blood glucose levels, which occur in diabetes, can affect the small blood vessels in the kidneys. This results in diabetic kidney disease, also referred to as diabetic nephropathy.
This disease gradually impairs the function of the kidneys. If not treated, it can lead to chronic kidney disease or even kidney failure.
Being obese can also affect kidney function. This is because being obese forces the kidneys to work harder, thus leading to impairment.
Being obese can also lead to high blood pressure, which can cause kidney disease. It has been observed that if high blood pressure and diabetes occur simultaneously, there is an increased chance of kidney damage.
How To Keep Your Kidneys Healthy
The good news is that this health triangle can be prevented or managed through a healthy lifestyle. Eating a healthy meal, exercising regularly, and keeping a healthy body weight are some of the steps that can be taken.
Monitoring blood sugar levels as well as blood pressure is important, especially for those who are overweight or have a family history of diabetes.
By taking early steps to diagnose and treat medical conditions, as well as making healthy lifestyle changes, it is possible to break the cycle of obesity, diabetes, and kidney disease.
India's Silent Crisis: Why We Must Embrace Deceased Donor Organ Transplantation
Credit: iStock
In India, around 95 percent of kidney transplants and a significant proportion of liver transplants depend on living donors—primarily family members. While live donation can be lifesaving, it transforms a medical crisis into a family ordeal.
Parents feel obligated to donate to their children, spouses face immense pressure, and siblings also navigate complex emotional stress. This decision is typically free from the weight of duty, guilt, and family expectations. I have seen young professionals delay their careers, mothers hide their own health concerns, and elderly parents risk their lives—all because we lack a robust deceased donor program.
Moreover, the real challenge lies with living donors. Donors face surgical complications, long recovery periods, and potential long-term health consequences. While we counsel families about these risks, the urgency of their loved one's condition often overshadows rational decision-making.
Why Deceased Donation Remains A Distant Dream
Despite the introduction of the Transplantation of Human Organs Act and necessary amendments in India, the decrease in organ rates continues to remain abysmal—approximately 0.8 donors per million population, compared to 20 in the UK, 36 in Spain, and 33 in the United States.
Several deeply rooted factors explain this gap:
Cultural and religious misconceptions continue to persist. Many Indians also believe that the donation of organs conflicts with the religious beliefs regarding the sanctity of the body or rebirth, even though many religious institutions have endorsed organ donation.
The concept of brain death remains poorly understood; families struggle to accept that their loved one is dead when the heart still beats, and the chest rises on ventilator support. Families fear that clinical teams may hasten death to procure organs or that the wealthy will receive preferential treatment.
These anxieties, while often unfounded and deep-rooted, reflect legitimate concerns about transparency and equity in our healthcare institutions. We lack trained transplant coordinators, efficient organ retrieval networks, and standardized protocols across states.
When a potential donor is identified in a district hospital, the administrative maze often ensures organs go unutilized. Finally, public awareness is minimal.
Most Indians have never discussed organ donation with their families. Death remains a taboo subject, making advance directives about organ donation exceptionally rare.
The Urgent Need For Change
Over 150,000 patients await kidney transplants; fewer than 10,000 receive them annually. Similarly, roughly 50,000 patients are listed waiting for a liver transplant nationally. For hearts and lungs, deceased donation is the only option, yet these transplants remain rare. Patients die waiting—not because medical expertise is lacking, but because organs are unavailable.
Our dependence on living donation also perpetuates inequality. Those without family networks, or
whose families cannot afford the medical evaluation and recovery costs for donors, are effectively excluded from transplantation. Deceased donation would democratize access.
Lessons From Spain And The United States
Spain has the world's highest deceased donation rate, achieving success through a "Spanish Model" of dedicated transplant coordinators in every hospital, robust training programs, and a presumed consent system where all citizens are potential donors unless they opt out. Importantly, families are still consulted, but the default position favours donation.
Their success stems not just from infrastructure but from normalizing conversations about donation through media campaigns and school education programs.
A hybrid approach suited to Indian realities—combining elements of presumed consent with robust family consultation, investing in coordinator training, and launching sustained public awareness campaigns—could transform our landscape.
The Government's Critical Role
This transformation should be led by the government through several concrete actions:
First, invest in infrastructure. Every medical college and tertiary care center must have trained transplant coordinators and clear protocols for identifying and managing potential donors. State governments must establish well-funded organ retrieval networks with 24/7 operational capacity.
Second, Public awareness campaigns should be launched. Use television, radio, social media, and community health workers to educate citizens about brain death, the donation process, and the lives saved. Do a partnership with religious leaders to dispel the myths. Make organ donation part of school curricula.
Third, ensuring transparency and equity alongside establishing clear and publicly accessible waitlist protocols. To prevent commercialization, strict oversight from the government is recommended. Transplant programs must build trust by indicating that the system works for everyone, not just the privileged.
Changing Public Perception
We must reframe organ donation from an extraordinary act to a normal, expected part of medical care at the end of life. This requires: Open family conversations and discussing their wishes regarding organ donation with the loved ones, also removing the burden of decision-making during the grief.
Celebrity and community leadership: When a pledge to donate is made by public figures, it enables a gradual shift in thought and practice.
Media responsibility: Gifts of life should be highlighted by news coverage, humanizing donors and recipients while respecting their privacy.
Medical community engagement: Doctors should initiate sensitive conversations regarding donation with families of brain-dead patients, considering it as part of compassionate end-of-life care rather than an awkward position.
With world-class transplant surgeons, excellent medical infrastructure in urban centers, and a population of over 1.4 billion. We should not have patients dying for lack of organs, and programs being heavily reliant on living organ donations.
What we lack is collective will, bold government action, and public education. As a society, we take pride in seva (service) and daan (giving), and organ donation should align perfectly with our values. Let us make it so.
Colorectal Cancer: The Preventable Tragedy
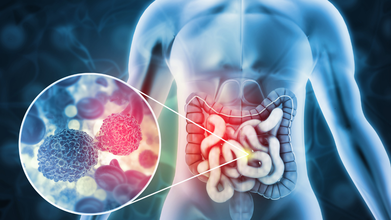
Credit: iStock
In the world of oncology, we usually speak of battling or fighting cancer. We pool in our whole life’s earnings to find a cure or solution for the advanced stages of this disease. What if cancer were not a threat?
Here is one of the most common and deadly cancers, which is also one of the most preventable ones. We are talking about Colorectal cancer, which is often described by medical professionals as a preventable tragedy. This is because, unlike many other forms of the disease, we have a clear window of opportunity to stop it before it even begins.
As we observe Colorectal Cancer Awareness Month in March, it is time to strip away the fear surrounding the tests and understand why nobody should ever have to die from a condition that gives many chances to catch it well in time.
How It All Begins
To understand why colorectal cancer is preventable, we have to look at how it develops. As with most cancers, this too doesn’t appear overnight. Almost always, these cancers start as small growths called polyps or precancerous lesions on the inner lining of the colon or rectum.
These polyps are like seeds; they are mostly benign. But there is one type of polyp that can gradually turn into cancer over a period of time. This is where the advantage lies. There is a long interval of time before polyps develop into cancer.
During this time, they can be removed if they are identified. If a doctor removes a precancerous polyp during a routine screening, they would not only have nipped the cancer in the bud, but would have also prevented it from occurring.
The statistics are encouraging when detected early, with figures showing that over 90 per cent of cases of colorectal cancer are fully curable. However, people do not seek medical attention until they experience some symptoms, at which point the seed-like polyps have already grown into a deep-rooted cancer.
Screening – The Main Defense
In Western countries, the death rate from colorectal cancer has been declining at a visible rate due to the presence of strong and well-supported screening programs from their governments.
Although some countries have not yet introduced a formal national program, the consensus among medical experts is that if you are above 45 years of age or have high-risk factors, you need to take the initiative to be screened.
There are two primary ways we do this:
1. The FIT (Fecal Immunochemical Test) – This is a simple, non-invasive stool test that has become a staple in most general health check-up packages. It works by detecting tiny amounts of human hemoglobin (blood) that aren’t visible to the naked eye.
The advantage of getting a Fecal Immunochemical Test done is that it is very easy, and it can be done at home, and requires no special preparations. It acts as an early warning system. If a FIT result comes back high, it signals that something is happening in the bowel that requires a closer look via colonoscopy. It is recommended that everyone over 45 undergoes this test annually. While not as definitive as a colonoscopy, it is a vital first line of defence.
2. The Colonoscopy – This is the gold standard. Despite all the fear and misinformation that can be spread on the Internet, a colonoscopy is a routine and safe procedure. It allows a doctor to visually inspect the inside of the colon. It is a procedure that has dual benefits – to see what is wrong, and to make things right. Should the doctor find a polyp, it can be safely removed at the time of the procedure.
Many people avoid this procedure because of embarrassment and fear of discomfort. However, with the sedation, most people find it to be completely painless.
Recognizing The Red Flags
While screening is for people with no symptoms, you must be alert to signs that require an immediate expert opinion, regardless of your age. Also, never ignore these symptoms or assume that they are due to bad food choices:
- If you feel changes in bowel habits frequently, then this is not just a one-off upset stomach. Pay attention to persistent change, such as recurrent diarrhea or a sudden onset of constipation that doesn’t resolve.
- Blood in the stool is perhaps the most critical sign. Many people write off rectal bleeding as piles (hemorrhoids). But bleeding that persists despite treatment must be checked by an expert.
- Losing weight without trying is often a sign that the body is under significant stress. Not all unexpected weight loss is a happy occurrence.
- Anemia and fatigue are visible proof. If a blood test shows low hemoglobin or iron-deficiency anemia – especially in men or in post-menopausal women – a colonoscopy is often mandatory to rule out internal bleeding from a tumor.
- Persistent abdominal pains, which are chronic, severe, or are accompanied by unexplained cramping and pain in the lower tummy area, must be evaluated by a doctor.
Breaking The Stigma
The aim of Colorectal Cancer Awareness Month is not just to create awareness about the disease; it is also about providing support as we pay tribute to cancer warriors who have completed the painful journey from surgery and chemotherapy to rehabilitation. Shared stories can help remove the fear in others’ minds.
There is no such thing as too much information in the doctor’s office. Our bowels are part of our body, and we must overcome the shame or embarrassment associated with talking about them. A simple dialogue about bathroom habits or asking for a FIT test can save a life.
By promoting early detection leading to the removal of precancerous polyps, we can build a world where no one ever has to die from colorectal cancer. If you are aged 45 years or older, make this the month you arrange for a screening. If you have symptoms, do not wait; the right time is now.
In the case of colorectal cancer, prevention is not just the best medicine, it IS the cure.
© 2024 Bennett, Coleman & Company Limited

