Can People With Normal Body Weight Have A Fatty Liver?
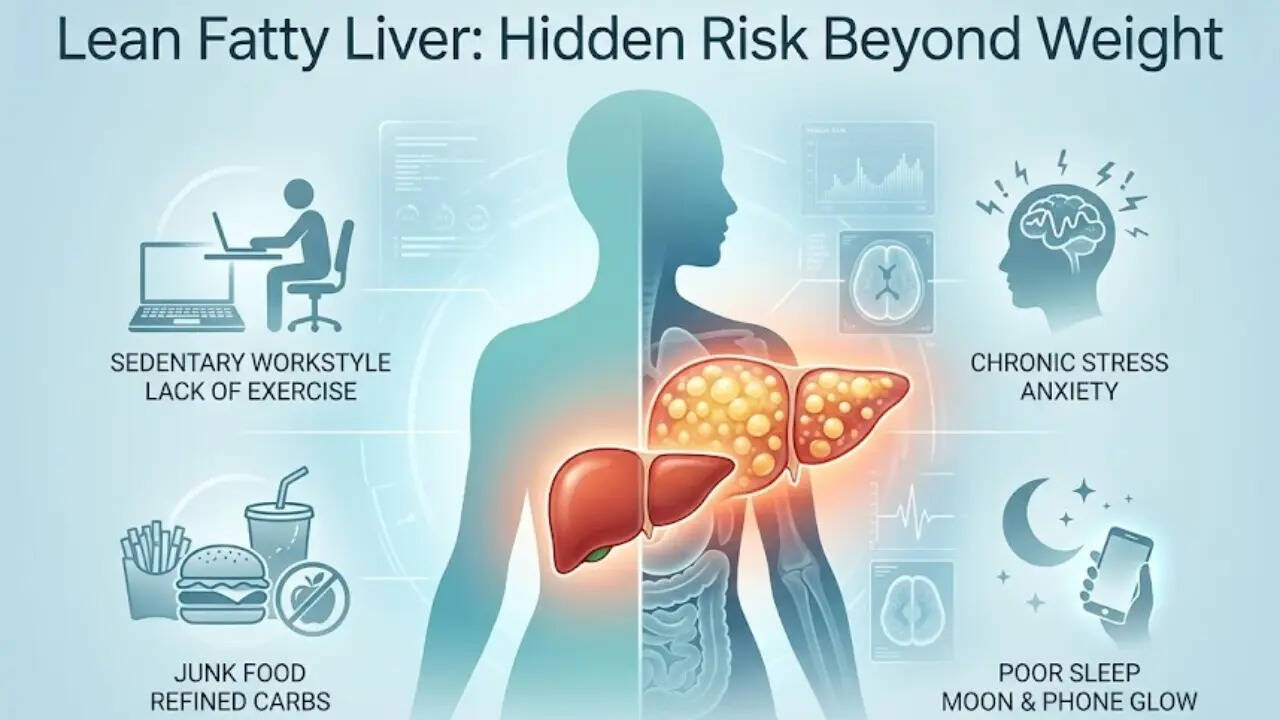
Visceral fat is one of the contributors of lean fatty liver. (Photo credit: iStock)
SummaryLean fatty liver is a clinical reality that challenges the assumption that a healthy weight means a healthy body.
End of Article
