- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
- Web Stories
Could Your Child’s Upset Stomach Be A Norovirus Infection? Watch For These Red Flags

Image Credit: Canva
Norovirus infection is on the rise globally, raising concerns for parents as children are particularly susceptible to this highly infectious virus. Easily confused with ordinary stomach flu, norovirus brings sudden and severe episodes of vomiting, diarrhea, and abdominal cramps. With cases peaking in the UK and elsewhere in the world, it is important to know the signs and act fast to avoid the spread of this disease.
The most recent statistics from the UK Health Security Agency (UKHSA) show a dramatic rise in norovirus infections. During the two weeks between February 3 and 16, 2025, confirmed cases increased by 29.4% over the previous fortnight, twice the five-season average for the two-week period. Hospitals and care homes have been worst affected, with the infections being most common among the elderly. Whereas cases normally fall with better weather, the current season is being particularly unpredictable.
The spike is caused by the increase of two prevalent genotypes—GII.17 and GII.4, according to health professionals. Most cases (76%) were accounted for by GII.17 before, but its percentage decreased to 59% as GII.4 infection levels have almost doubled from 10% to 29% within three months. This indicates that people who already have norovirus this season may get reinfected with another strain.
What is Norovirus and How Does it Impact Children?
Norovirus is a contagious virus that leads to gastroenteritis, causing inflammation of the stomach and intestines. Norovirus alone infects more than 20 million people annually in the United States, which makes it the leading cause of illness related to the stomach.
Children are especially at risk because of close contact at schools, childcare facilities, and playgrounds. The virus gets transmitted easily from direct contact with an infected person, infected surface, and ingesting contaminated food or beverages. Infants and toddlers, with a habit of putting hands and objects into mouths, are additionally at risk.
Symptoms of Norovirus in Children
Early identification of norovirus symptoms will go a long way in treating the illness successfully. Some of the common symptoms include:
- Nausea and vomiting – More common in children than adults.
- Watery diarrhea – May cause dehydration if not well taken care of.
- Stomach cramps and pain – Usually intense and sudden.
- Mild fever and body aches – May be confused with flu.
- Sudden development of illness – Symptoms develop 24-48 hours after exposure and persist 1-3 days.
Notably, norovirus is still infectious for three days after the symptoms have vanished and thus isolation is very important to avoid further transmission.
What's The Biggest Concern for Young Children?
Dehydration is the most immediate threat posed by norovirus, particularly among infants and young children. As children quickly lose fluids from diarrhea and vomiting, parents must observe warning symptoms of severe dehydration such as:
- Dry mouth and tongue
- Decreased urine output (fewer wet diapers in an infant)
- Not crying tears
- Sunken soft spot on the top of a baby's head (fontanelle)
- Irritability, drowsiness, or lethargy
If your child shows these signs, get them to the doctor right away.
How to Care for a Child with Norovirus?
There is no treatment for norovirus, but supportive therapy can make symptoms more manageable and avoid complications.
1. Hydrate Your Child
Have your child drink small amounts of fluids like water, coconut water, or oral rehydration drinks like Pedialyte®. Breastfeeding infants should be kept on breast milk, but formula-fed babies can receive additional fluid support as directed by a physician.
2. Gradually Reintroduce Food
After vomiting stops, reintroduce easily digestible foods:
- Clear broths, ice pops, and gelatin to hydrate
- Plain foods such as dry cereal, toast, crackers, pasta, or pretzels
- The BRAT diet (bananas, rice, applesauce, toast) to calm the stomach
- Dairy, fatty, or highly spiced foods should be avoided until digestion returns to normal.
3. Allow Plenty of Rest
Because norovirus produces fatigue, rest is needed for recovery. Keep your child comfortable with warm blankets (not for infants), disinfected toys and games, and quiet things to do such as books or cartoons.
Essential Hygiene Practices to Prevent Norovirus
It may not be easy to completely avoid norovirus during an outbreak, but you can markedly lower the risk by taking these preventive measures:
1. Practice Frequent Handwashing
The most efficient prevention of norovirus is handwashing with warm soapy water. Sanitizers don't destroy the virus, so get kids to wash their hands:
- After toilet use
- Before meals
- After handling common surfaces or toys
2. Clean High-Touch Surfaces
Norovirus lasts on surfaces for days. Clean doorknobs, tables, toys, toilets, and diaper-changing stations frequently using bleach-based disinfectants.
3. Safe Food Handling
Norovirus is transmitted by contaminated food and beverages. Be careful as follows:
- Wash produce thoroughly.
- Cook seafood through.
- Do not prepare food if you or your child are ill.
4. Keep Sick Children Home
If your child gets norovirus, keep your child out of school and daycare until the child is symptom-free for 48 hours. This keeps others from getting infected.
When to Call a Doctor
Although most norovirus infections get better on their own, call your pediatrician if your child:
- Cannot retain liquids over 24 hours
- Vomits or has diarrhea containing blood
- Demonstrates evidence of severe dehydration
- Has an unrelenting high fever
- Acts extremely lethargic or is unresponsive
Norovirus is an uncomfortable, fast-spreading illness that can take a young child down. Although most instances will pass in a few days, dehydration is a serious concern, so rest and hydration become priorities. Recognizing the signs, following good hygiene, and avoiding exposure are good ways to protect your child during norovirus outbreaks. In the case of severe symptoms, get immediate medical care.
Ananda Lewis, Former MTV Host Who Shared Her Breast Cancer Story To The World Passes Away At 52

Credits: Getty and Instagram
Ananda Lewis, celebrated TV host known for her authenticity and warmth, passed away at 52 after a long and brave battle with breast cancer. Once a beloved face on BET’s Teen Summit and MTV’s Total Request Live, she used her platform to engage young audiences with pressing social issues and celebrity interviews that left a mark.
A Powerful Presence on Screen
Lewis first came into the spotlight through BET’s Teen Summit, where she led candid conversations on challenges facing Black youth. Her interviews with figures like Kobe Bryant, Tupac Shakur, and Hillary Clinton earned her critical acclaim, including an NAACP Image Award.
In 1997, she joined MTV, becoming a key voice on MTV Live, Hot Zone, and TRL. Though her move sparked criticism, she remained unapologetic. “Growth is necessary,” she told the Associated Press. “You’ve got to get out there and live your life.”
She later launched The Ananda Lewis Show in 2001, a daytime talk show aimed at real conversations, even if it followed a familiar format. The show lasted one season, but Lewis remained a powerful presence, later joining The Insider as a correspondent.
Breast Cancer Journey That She Shared With The World
In 2020, Lewis revealed that she had been living with stage 3 breast cancer since 2018—later advancing to stage 4. Her diagnosis came after years of ignoring persistent inflammation linked to mastitis from breastfeeding. A lump discovered in her right breast led to a biopsy, confirming it was invasive carcinoma.
Instead of following a conventional medical path, Lewis chose alternative treatments. “I wanted to understand why my body created cancer and how to change the terrain,” she explained. She focused on diet changes, stress management, detoxing, and holistic therapies like high-dose vitamin C, acupuncture, and cryoablation.
A Different Kind of Battle
Lewis moved to Arizona in 2020 for 16 weeks of intensive integrative treatment. Her cancer reduced from stage 3 to 2 and was no longer in her lymph nodes. But the journey wasn’t without hardship—financial struggles and insurance lapses made consistent treatment difficult.
In early 2023, a scan showed the tumor had grown slightly, but it had not spread. She underwent electrical ablation in Mexico, which unfortunately didn’t succeed. By October 2023, a PET scan confirmed the cancer had advanced to stage 4. Still, Lewis continued treatment and saw significant improvement by January 2024.
Lewis was candid about her journey, using her story to raise awareness about early detection and holistic health. “Stage 4 doesn’t mean the end,” she said. “It means I have to do more.”
Her message to women was clear: be proactive. Prioritize mammograms, manage stress, sleep well, and adopt a clean lifestyle. “If I had known what I know now ten years ago, perhaps I wouldn’t have ended up here,” she said.
“I want to look back and say—I did that exactly how I wanted to,” Lewis reflected. Her legacy is one of resilience, wisdom, and an enduring belief in the right to choose one’s own path—even through cancer.
Smartphone Tool Can Now Detect Early Warning Signs Of Huntington’s Disease In 5 Minutes, Finds Study
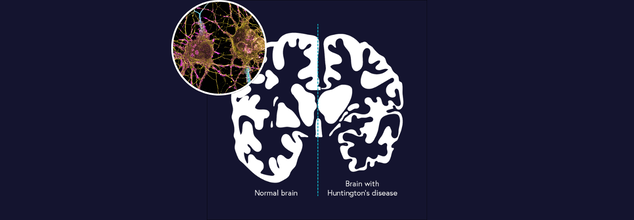
In a revolutionary medical breakthrough, scientists have identified that a five-minute phone test will soon be able to detect early onset of Huntington's disease—a rare, genetic brain disorder—long before symptoms become visibly apparent. With digital health technologies revolutionizing the future of diagnosis, the new app test offers promise of quicker, more convenient, and highly accurate tracking, all from the comfort of the patient's own home. Wondering how your phone could be part of the future of neurology? Here's what a new study says.
Scientists have created a smartphone application that can identify early signs of motor symptoms of Huntington's disease within five minutes. The research, published in the journal Brain, is presented here with the explanation of how simple devices used on a daily basis can become big medical devices to analyze a subject's neurological well-being in real time from the comfort of his or her home. This innovation is especially valuable considering the scarcity and intricacy of Huntington's disease (HD), a genetically inherited disease in which there is, as of yet, no cure.
How the Smartphone Test Works?
The test developed is composed of five smartphone tasks assessing factors like finger tapping, balance, and involuntary movements. These activities together create a Huntington's Disease Digital Motor Score (HDDMS), a sensitive measure that can identify minimal changes in motor function that could occur before more evident clinical signs. As Ed Wild, Professor of Neurology at University College London's Huntington's Disease Center, points out, the fact that motor impairment can be measured in only five minutes at home has the potential to change the way clinical trials are carried out and disease progression followed.
Huntington's disease is a genetically inherited condition that leads to progressive degeneration of nerve cells within the brain, particularly in areas responsible for movement, cognition, and emotion. The symptoms usually occur between ages 30 and 50 and gradually worsen. In the early stages, there can be involuntary jerking or contorting movements (chorea), clumsiness, imbalance, and mood swings. When the disease progresses, patients become severely disabled from a motor standpoint, develop loss of cognitive abilities, and have psychiatric disturbances.
Conventional diagnostic approaches such as neurological assessment and imaging studies can be costly, time-consuming, and not as sensitive when identifying early-stage symptoms. The HDDMS tool is a cost-friendly, easily accessible alternative that could result in improved disease management through earlier intervention.
What Sets the HDDMS Test Unique and Accurate?
In contrast to traditional clinical evaluations that entail patients visiting specialized clinics, the HDDMS may be taken on a smartphone in under five minutes. The measure was created using information from more than 1,000 participants in four independent studies and is among the most widely validated digital tests for HD to date.
The investigators discovered that the HDDMS was almost twice as effective as conventional techniques in detecting significant changes in motor function. Such accuracy is important in rare conditions such as HD, where clinical trials have often been hindered by limited sample sizes and heavy participant burden.
With a number of hopeful treatments for Huntington's disease being developed, the need to measure disease progression accurately has never been greater. Integrating the HDDMS into clinical trials could make the research process more efficient by cutting the number of participants needed and the time needed to determine the effectiveness of a drug.
Professor Wild highlighted that more sensitive equipment is essential in rare disease investigation, where the limited patient base means it is challenging to set large-scale trials. He added the HDDMS provides a "more meaningful and convenient" means of assessing motor function than standard in-clinic tests.
What is Huntington's Disease?
Huntington's disease is a hereditary, always fatal disease due to a mutation in the gene encoding a protein named huntingtin. The mutation results in an abnormal repetition of the DNA sequence CAG (cytosine, adenine, guanine), causing brain cells to degenerate over time. Every child of a parent with HD has a 50% possibility of inheriting the defective gene.
Symptoms are:
- Chorea (involuntary jerking motions)
- Cognitive impairment
- Personality and mood changes
- Trouble with walking, talking, and swallowing
- Insomnia and weight loss
With time, people with HD become unable to take care of themselves. The disease is eventually fatal, and no cure is available. Medications can be used to control chorea, depression, and anxiety, however.
Diagnosis is usually made through neurological examination, genetic testing, and imaging tests like MRIs or CT scans. Although these work well in establishing the disease, they are frequently unable to identify early signs, especially minor motor dysfunctions.
Treatment is mainly supportive. Medications like tetrabenazine and deuterabenazine are employed to manage movement disorders, and antipsychotic medications can be given for psychiatric abnormalities. Genetic counseling is highly advised for HD-affected families.
Although the HDDMS has been impressive in its accuracy in initial trials, scientists recognize that additional studies are necessary to assess its ability to forecast long-term functional decline. Additional research will also investigate how the tool can be introduced into standard clinical practice and patient follow-up.
If successful, smartphone-based HDDMS will be the cornerstone of the global battle against Huntington's disease, providing an affordable and scalable means of monitoring one of the most complicated neurological diseases in the arsenal of medicine.
Accelerated Biological Aging Could Make You At Risk For Dementia: Study

(Credit-Canva)
We have all heard people say that they are old souls trapped in a young body, however, this is a figure of speech people use. While this phrase may mean you like old school things, it can also happen literally. Sometimes your body ages faster than you do, but this is the biological age we are talking about. While chronological aging is counted as the years we have lived, biological age can be faster or slower.
Think of it as perishable food. If you leave them in unfavorable environments, they can spoil fast, becoming edible. However, when you keep them in the correct environment with even temperature, the food will stay edible for longer than it should. Our bodies are similar in that sense. If you take care of it, limiting processed food, exercising and taking care of your health, you will find that your biological age is much slower or healthier than a person who does the opposite. However, what is the connection between biological aging and our lifestyle. How do we age slower/faster depending on our choices.
A new study suggests that signs of faster aging in your body are connected to a higher chance of developing dementia and stroke. Specifically, researchers found that people with shorter telomeres in their white blood cells tend to have an increased risk of these two brain conditions. These findings were published recently in the journal Neurology.
What Are Telomeres and Why Do They Matter?
Think of telomeres as the protective caps on the ends of your chromosomes, much like the plastic tips on shoelaces. They prevent your chromosomes from unraveling and getting damaged. Every time your cells divide, these telomeres get a little shorter. This makes them a useful way to estimate a person's biological age, which is how much wear and tear your body has accumulated from stress over time, rather than just your age in years. Your biological age can be quite different from your actual age.
Lifestyle Habits Can Counter the Risk
However, there's good news: the study found that this link between shorter telomeres and brain diseases wasn't present in people who maintained healthy lifestyle habits. This suggests that even if your body shows signs of faster aging, you can still reduce your risk of age-related brain diseases. This includes things like keeping a healthy weight, limiting alcohol, getting enough sleep, and exercising regularly. These healthy choices can help delay the aging of your cells and lower your chances of developing these conditions, especially if you're already at a higher risk.
Shorter Telomeres, Higher Risk
For this study, researchers looked at genetic data from over 356,000 people. They categorized participants into three groups based on the length of their telomeres: short, medium, or long. They then compared telomere length to people's lifestyle habits and whether they had developed dementia, stroke, or depression.
Over an average of seven years, nearly 26,000 people developed at least one of these three age-related brain diseases. People with the shortest telomeres had significantly more cases of these brain diseases compared to those with the longest telomeres. Overall, after considering other risk factors, individuals with short telomeres were 11% more likely to develop one of these brain diseases. More specifically, they faced an 8% increased risk of stroke, a 19% increased risk of dementia, and a 14% increased risk of late-life dementia.
It's important to remember that this study shows a connection, not a direct cause-and-effect relationship between telomere length and brain health.
© 2024 Bennett, Coleman & Company Limited

