- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Have Belly Fat And Can't Lose Weight? These 2 Hormones Are To Blame

Image Credit: Canva
If you’re eating a healthy diet and exercising regularly but still struggling with stubborn belly fat, your hormones might be the hidden culprits. This condition, often referred to as a “hormonal belly,” results from imbalances in key hormones that regulate metabolism, stress response, and fat storage. When cortisol spikes from stress or insulin resistance develops, the body clings to fat, especially around the abdomen.
Once you understand how the hormones cause it, you might be able to devise a means of losing excessive fat and coming back into body balance. In this article we will discuss about the two major hormones which are behind your stubborn belly fat.
What is Hormonal Belly Fat?
Hormonal belly fat is the excessive fat that is stored in the abdominal area due to hormonal imbalances. This may happen as we age, suffer from chronic stress, or have metabolic disorders. The hormones of cortisol and insulin are among the most significant in controlling fat distribution. When these hormones are disrupted, they may signal the body to store more fat, especially around the midsection.
Signs You Have a Hormonal Belly
While weight gain can result from various factors like diet and inactivity, hormonal imbalances have distinct signs, including:
Chronic stress and anxiety: High cortisol levels due to stress encourage fat storage in the abdomen.
Hair loss and fatigue: Low thyroid hormones can lead to sluggish metabolism and increased fat accumulation.
Unusual food cravings: Insulin resistance can lead to intense sugar cravings and overeating, further promoting belly fat gain.
If you experience any of these symptoms, it might be the time to address your hormonal issues regarding weight gain.
The Two Hormones Behind Stubborn Belly Fat
1. Cortisol: The Stress Hormone
Cortisol, also referred to as the "stress hormone," is a hormone produced by the adrenal glands in response to stress. Although cortisol, for the most part, regulates inflammation and metabolism, persistent elevations in cortisol levels can lead to the excessive storage of fats particularly around the abdomen.
How Cortisol Causes Belly Fat
- Increases appetite: Higher cortisol levels make you desire sugary and fatty foods, promoting overeating.
- Slows metabolism: Long-term stress is a signal the body uses to conserve energy, hence hard to lose weight.
- Encourages fat storage: Cortisol guides fats to be stored in the abdominal cavity, thus promoting central obesity.
How to Reduce Cortisol Naturally
- Practice mindfulness: Meditation and deep breathing activities are practices that regulate cortisol.
- Engage in light exercise: Walking or yoga can reduce stress without causing a surge in cortisol production.
- Get enough sleep: Lack of sleep increases cortisol levels, so get 7-9 hours of quality rest.
- Reduce caffeine and sugar: Both substances can increase cortisol levels and exacerbate the stress response.
2. Insulin: The Blood Sugar Regulator
Insulin is a hormone produced by the pancreas that controls blood sugar levels through entry of glucose into cells to produce energy. In the event of excessively high insulin levels due to too much carbohydrate intake or resistance to insulin, the body tends to store more fat, especially in the abdominal area.
How Insulin Leads to Belly Fat
Raises fat deposition: the hormone signals the cells to retain excess glucose as fat.
It promotes insulin resistance: Over time, cells become resistant to insulin, leading to higher blood sugar and increased fat accumulation.
Triggers sugar cravings: When insulin levels fluctuate, it can cause sudden hunger and cravings for processed foods.
How to Improve Insulin Sensitivity
- Incorporate strength training: Lifting weights improves insulin sensitivity and helps burn fat.
- Avoid constant snacking: Frequent eating keeps insulin levels elevated. Try intermittent fasting or spacing out meals.
- Eat balanced meals: Include protein, fiber, and healthy fats to stabilize blood sugar levels.
- Cut back on refined carbohydrates: Decrease sugars and processed foods that cause a sudden insulin rise.
How Balancing Hormones for Permanent Weight Loss
Both cortisol and insulin should be balanced for less belly fat. Here's the practical guide for restoring hormone balance:
Diet for Balancing Hormones
Eat plenty of whole nutrient-rich foods like vegetables, lean proteins, and healthy fats.
Avoid processed sugars and refined carbs.
Stay hydrated and incorporate anti-inflammatory foods like turmeric and omega-3-rich fish.
Manage Stress Effectively
Engage in relaxation techniques such as deep breathing, journaling, or spending time in nature.
Maintain a Consistent Exercise Routine
Set boundaries to prevent work and life stress from overwhelming you.
Maintain a Consistent Exercise Routine
Strength training helps build muscle, which improves insulin sensitivity.
Moderate cardio, such as walking or swimming, aids fat loss without raising cortisol excessively.
Prioritize Sleep and Recovery
Establish a consistent sleep schedule to support hormonal balance.
Establish a Consistent Sleep Schedule to support hormonal balance
Limit screen time before bed to improve melatonin production and sleep quality.
When to See a Doctor
If you’ve made lifestyle changes and are still struggling with belly fat, consult a healthcare provider. They can run tests to assess your hormone levels and identify underlying issues such as thyroid dysfunction, polycystic ovary syndrome (PCOS), or metabolic syndrome.
Over 40% Prostate Cancer Patients in India Diagnosed After Cancer Has Spread: ICMR study

Credit: Canva
A recent study by the Indian Council of Medical Research (ICMR) showed that more than 40 percent of prostate cancer patients in the country are diagnosed after the cancer has spread.
The 43 percent of late diagnosis cases indicates the significant burden of late detection of prostate cancer in the country. This can not only limit treatment options but also lead to poorer survival outcomes.
The study, published in the Indian Journal of Surgical Oncology, revealed that while more than 80 per cent began treatment within two months, but referral patients experienced longer delays.
Researchers from the ICMR’s National Centre for Disease Informatics and Research, in Bengaluru, stressed the need to strengthen referral pathways to ensure timely, stage-appropriate care.
“Our study indicates that over 80 percent of patients commence treatment within two months of diagnosis, but referral systems and delays in care persist,” said corresponding author Prashant Mathur, Director, ICMR-NCDIR, in the paper.
“To address these challenges, the healthcare system must prioritize improving referral efficiency, reducing administrative bottlenecks, enhancing coordination through digital health records, and multidisciplinary tumor boards,” the authors added.
Age, The Strongest Risk Factor For Prostate Cancer
The ICMR study is based on an analysis of 9,347 cases from 96 hospitals under the National Cancer Registry Program.
The researchers found that 75.6 percent of total prostate cancer cases occurred in the age group of 60–80 years, indicating that advanced age remains the biggest risk factor for the condition.
As life expectancy increases, more men reach the higher-risk age group, but awareness and screening practices have not scaled proportionately.
Adenocarcinoma was the most common pathology, constituting 77 percent of cases.
It is the most common form of prostate cancer, accounting for over 95 per cent of all cases. It develops in the gland cells that produce prostate fluid and typically grows slowly over several years.
Further, the ICMR researchers noted that about 57 percent of cases were diagnosed with localized (29.9 percent) or locoregional (27 percent) cancer.
Thirty percent underwent surgical treatment, and 22 percent received radiation therapy. Systemic therapy was the most common single modality treatment.
“Early detection and streamlined referral pathways are essential to improve prostate cancer outcomes in India,” the researchers said.
Prostate Cancer And Its Prevalence In India
Prostate cancer forms in the cells of the prostate -- a gland found only in males and a part of the male reproductive system. It lies below the urinary bladder and in front of the rectum.
Nearly all prostate cancers develop from glandular cells (adenocarcinomas).
Globally, prostate cancer is the most frequently diagnosed cancer among men in 112 countries and the leading cause of cancer death in 48 countries. In 2020, an estimated 1.4 million new cases of prostate cancer and 0.37 million deaths were reported worldwide.
In India, it is the second most common cancer among men, accounting for more than 60 percent of the prostate cancer burden in South-Central Asia. As per the ICMR data, the country reported 34,540 incidences of prostate cancer and 16,783 deaths.
Prostate cancer symptoms include urinary difficulty, a weak stream, or blood in the urine.
As prostate cancer is a slow-developing disease, it often causes no symptoms during the early-stage, leading to delayed medical consultation.
Other reasons for late detection in India include low awareness, limited routine screening -- PSA (prostate-specific antigen) programs; social stigma and hesitation due to embarrassment or cultural taboos.
Lack of access to specialist care, diagnostic facilities, and cancer centers, especially in rural populations, coupled with cost and referral gaps, also leads to delay in diagnosis.
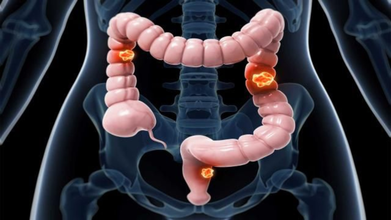
Expert Warns: Three Steps to Protect Against Colon Cancer
Credit: Unsplash
Colon cancer develops from polyps in the colon or rectum, often taking years to show symptoms. The cancer begins when small growths called polyps form on the inner lining of the colon or rectum. Over time, changes in the DNA of these cells can cause the polyps to become cancerous.
As abnormal cells multiply, they replace healthy cells and eventually form a mass known as a tumor. This process develops slowly, often taking up to ten years for a precancerous polyp to turn into cancer and begin showing symptoms.
The American Cancer Society notes that colorectal cancer impacts around 1.9 million people every year.. In India, it is the fourth most common cancer among both men and women. In 2022, there were 64,863 new cases and 38,367 deaths.
Projections suggest that incidence will continue to rise by 2026, reflecting both lifestyle changes and improved detection.
Colon cancer can be difficult to detect because it often develops without obvious symptoms. However, Dr Jordan Karlitz, MD, of Exact Sciences, shared with The American Journal of Managed Care (AJMC) the three fundamentals of CRC prevention and early detection.
What Are The Three Tips For CRC Screening?
According to the expert, these are the three things you should do to protect yourself:
1. Timely risk screening
2. Knowing your cancer family history
3. Acting on early symptoms
"These are the 3 pillars that everybody needs to be aware of, because I think gaps in any of them could increase the risk of developing CRC and, unfortunately, lead to presenting with more advanced-stage disease," said Dr Karlitz.
Why Is Risk Screening Essential?
Timely screening for colon cancer is essential because it detects precancerous polyps early, allowing for their removal before they turn into cancer and identifies the tumors at highly treatable stages when survival rates are about 90 percent.
Screenings (like colonoscopies) can detect and remove pre-cancerous growths called polyps, preventing the development of cancer. The expert suggested that average risk screening now starts at the age of forty-five; you do not have to wait until age 50.
What Early Symptoms Should You Look Out For?
Colon cancer rarely announces its presence with dramatic symptoms. More often, it whispers — through changes in bowel habits, subtle abdominal discomfort, or unexplained weight loss.
Some of the most commonly missed early signs include:
- Persistent changes in bowel movements: Chronic constipation or diarrhea often dismissed as dietary effects.
- Blood in stool: Bright red or dark blood should not be ignored.
- Unexplained weight loss: Especially when unintentional.
- Abdominal cramps or bloating: Misinterpreted as common digestive issues.
Persistent changes in bowel habits, especially if they last more than a few days, must be taken seriously. Narrow or ribbon-shaped stools may indicate a tumor partially blocking the colon.
This Zoonotic Disease Of Himalayas Is Re-emerging But Recognition Remains Poor

Credits: iStock
A Himalayan zoonotic disease, which is transmitted by mite bites, known as Scrub typhus, is re-emerging. However, the attention and recognition to its threat remains poor. A Mongabay report noted the life of Maya Rai, 38, from Dajeeling, who works throughout the day. Her packed schedule does not allow her to stop working. When there is a febrile illness, it is "just another fever".
However, one monsoon, the fever hit her hard, while she thought it will pass too with some rest. She felt too weak to work. She received no clear diagnosis at the local Public Health Center (PHC), and was sent home with just painkillers. However, her condition did not improve. She experienced fever with cough, nausea, breathlessness and discomfort. Being a wage worker, she missed seven days, which meant no money for a week. She was finally taken to a private hospital in town, hours away from her village and the rapid test confirmed 'scrub typhus'.
This is an infectious disease caused by a bacterium Orientia tsutugamushi. Maya was prescribed antibiotics and was able to survive. However, there are many cases where this febrile fever is treated like any other fever, until it is too late. Many cases arise much later in front of a medical healthcare provider, when complications like acute respiratory distress, liver inflammation, kidney failure, and multiorgan dysfunction syndrome (MODS) have already happened.
Another case is from rural west Sikkim, where a 35-year-old Ganga Chhetri also had similar symptoms. However, by the time she was diagnosed, her organs were already critical. Ganga was also breastfeeding her two-year-old child and caring for her four-year-old.
Re-emergence of Scrub Typhus
The disease is locally known as kira le toke ko bimari, which literally translates it as a disease from an insect bite. This is re-emerging in the Dajeeling-Sikkim region of the Indian Himalayas, and is a public health concern in India. The cases have been reported across the country in India, as well as in other Southeast Asian countries. This affects one million people annually around the globe.
Scrub typhus was once confined to the Asia-Pacific’s ‘Tsutsugamushi Triangle’, a geographic stretch from northern Japan to Russia and northern Australia. Today, while this has changed, the disease still poses threat to many, including those living in the Himalayan region.
What Is Scrub Typhus And How Does It Spread?
It is an acute, potentially fatal, rickettsial infection that is caused by Orientia tsutsugamushi and transmitted by larval mites (chiggers) in rural areas.
At its core, scrub typhus in humans is associated with four interconnected elements: small mammals, particularly rats, tiny parasitic mites, the bacterium Orientia tsutsugamushi, and the environment they inhabit together. The disease is spread specifically by the larval stage of trombiculid mites, commonly known as chiggers. Only the larvae transmit the infection, passing it to humans through their bite.
These chiggers feed on the blood of small mammals such as rats, which play a key role in sustaining mite populations. Rats can also carry Orientia tsutsugamushi and pass the bacteria to mites that feed on them. In contrast, the nymph and adult stages of the mite, typically found in soil and vegetation, do not spread the disease.
Humans become infected when they enter areas infested with mites or environments with high rat populations, allowing infected chiggers to shift from rodents to people. The likelihood of such spillover events increases when rodent numbers grow, mite populations expand, or human contact with rats intensifies.
Factors such as land use changes, shifting weather patterns, natural disasters, deforestation, rapid urbanization, and increased garbage accumulation can create conditions that favor rodent and mite proliferation, thereby raising the risk of disease transmission.
© 2024 Bennett, Coleman & Company Limited

