- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
How Long After a Tattoo or Piercing Can I Donate Blood?
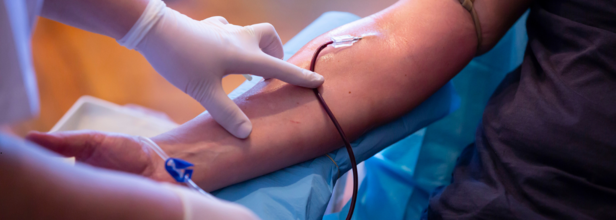
Credits: Canva
Are you that kind of person who celebrates milestones of your life with getting a tattoo? These milestones could be anything, including the things you achieved, or the things you could not achieve but taught you a lesson. If you are this person, then you must have wondered if you can donate blood with all the tattoos on your body? There are lots of rumors on how can one donate blood, or if at all they are allowed to donate blood. So let's get into its nitty gritty!
As per American Red Cross, in most states, a tattoo is acceptable if the tattoo was applied by a state-regulated entity. Which means the tattoo artist must be licensed and must practice following all the guidelines, using sterile needles and ink that is not reused. The same is the guideline for cosmetic tattoos, which includes microblading of eyebrows. If it is done by a licensed artist in a regulated state, then it is acceptable.
However, if you got your tattoo in a state that does not regulate tattoo facilities, you must wait three months after it was applied.
The states that do not regulate tattoo facilities are:
- Arizona
- District of Columbia
- Georgia
- Idaho
- Maryland
- Massachusetts
- Nevada
- New Hampshire
- New York
- Pennsylvania
- Utah
- Wyoming
Body Piercing
Similar is the case with body piercings. It has to be done following the regulation, here the key is that the instrument used has to be a single-use equipment and disposable. Which means if you are getting it by a gun, or an earring cassette, they have to be disposable. In case you got your piercing with a reusable gun or a reusable instrument, you will be required to wait for three months.
Three-Month Wait Period
The reason behind the wait time is associated with the concerns of hepatitis, which could be easily transmitted from donors to patients through transfusion. All blood donations are thus tested for hepatitis B and hepatitis C, with several tests. However, not always are these tests are perfect, thus the three-month period is given.
What Dangers Loom Over?
Donating blood after getting a tattoo can be dangerous as unclean tattoo needle could carry bloodborne viruses, which are hepatitis B, hepatitis C and HIV. In 2020, the Food and Drug Administration (FDA) updated its guideline, making the wait time shorter from one year to three months. This is because if you contract a bloodborne illness, it could be detectable within the period of 3 months.
What else makes you ineligible to donate blood?
There are other reasons why you may not be allowed to donate blood. As per the American Red Cross, you are not allowed to donate blood if you have
- hepatitis B or C
- HIV
- Chagas disease, which is a parasitic infection that kissing bugs cause
- leishmaniasis, a parasitic infection that sand flies cause
- Cruetzfeldt-Jakob Disease (CJD), a rare disorder that leads to mental deterioration
- Ebola virus
- hemochromatosis, which means extreme build up of iron
- hemophilia
- jaundice
- sickle cell disease
As per the National Institutes of Health (NIH) Blood Bank, these conditions make you permanently ineligible from donating blood.
While there are certain conditions that makes your permanently ineligible, there are other conditions that makes you temporarily ineligible from donating blood. These include:
- If you have a bleeding condition, and have issues with your blood clotting
- If you have received transfusion from a person
- If you have cancer. Here, the eligibility depend son the type of cancer you have
- If you have recently underwent a dental or oral surgery. In such a case, you would have to wait for three days
- If you had a recent heart attack, heart surgery or angina. You must wait for 6 months
- If you are pregnant, you can only donate blood after 6 months after delivering your child
How Does Your DNA Affect Your Daily Food Intake?

Credit: Canva
Your DNA, or more specifically your genes, have fascinating interactions with your diet. These interactions are often bidirectional and form the basis of personalized nutrition through genomic biohacks.
This has impressive applications in solving some of the most stubborn health related challenges, including undesirable weight gain and obesity.
Here are the five ways by which your DNA could positively shape your diet:
Nutrigenomics
Nutrigenomics is the mechanism by which your diet affects your genes, and not the other way round. The process has massive implications for your health, and especially over how you can use specific dietary components to protect yourself against serious killer diseases like cancers and issues like faster aging.
Deficiency in key nutrients like Vitamin B9 or folate, Vitamin B12, choline & methionine can cause genomic instability and increased cancer risk.
In contrast, specific foods like curcumin, resveratrol, green tea, broccoli, Brussels sprouts etc can help with genomic stability and help fight inflammation, oxidative stress and cancers.
Nutrigenetics
These are the processes by which your genes affect your diet or consumed food and hence central to our theme here. At times, nutrigenetics is referred to by the wider umbrella term nutrigenomics.
Your gene variants determine how you process specific nutrients, which explains why the same diet works differently for different people. Genetic tests like Eplimo can easily find this out.
For instance, presence of certain variants of the SGK1 gene make those individuals more prone to high blood pressure from salt intake.
Similarly, variants in the FTO gene are strongly linked to obesity risk. Other very common examples are variants in the CYP1A2 gene that determine how fast you metabolize caffeine and mutations in the LCT gene that determines whether you are at risk of lactose intolerance.
Hunger & Satiety Hormones
Ghrelin, the hunger hormone, is produced mainly in the stomach and stimulates appetite, increases food intake as well as promotes fat storage.
The production of ghrelin hormone is governed by the GHRL gene, and a common variant in this gene called RS696217 is associated with unnecessary hunger and higher obesity risk.
Similarly, leptin is a hormone produced by the body’s fat tissues and regulates satiety or the feeling of fullness with regard to food.
Production of leptin is governed by the LEP gene, while its utilization is controlled by the LEPR (leptin receptor) gene. Variants in either, especially LEP, can cause severe, early-onset obesity.
Metabolic Pace
Genes play a significant role in determining your metabolic pace. Studies show that genes account for up to 60 percent of the variations seen in the Resting Metabolic Rate between individuals.
RMR is basically a measure of how much calories are burnt while you are sitting or doing light activities.
It is different from Basal Metabolic Rate (BMR) that requires fasting and bed rest. Hundreds of genetic variants work together to set your RMR.
These include variants in the UCP1 gene governing thermogenesis or heat production, the MC4R gene that influences how the body burns nutrients for energy, and genes governing mitochondrial efficiency.
Building more muscles is a proven way to counter the negative impact of such variants and boost RMR.
Gut Microbiome
Does your gut microbiome impact your genes more, or does your genes impact your gut microbes more? Definitely, it is the former, which is also a better known mechanism due to that greater impact.
But that doesn’t mean that the reverse impact, from your DNA to your microbiome which accounts for around 10 percent of its composition, is insignificant in any way.
For instance, your specific gene variants determine which bacteria thrive by influencing immune responses, metabolism, and food preferences.
Specific genes, such as the LCT gene, directly correlate with the abundance of beneficial bacteria like Bifidobacterium. Genetics also influence how you digest food and your dietary preferences, which in turn feeds specific bacterial species.
Other genetic factors too have been identified as having strong links to microbial diversity, which is a great marker for not only gut health, but overall health, performance and longevity.
World Happiness Report 2026 Flags Social Media Harms On Adolescents' Mental Well-being

Credit: iStock
The impact of social media on adolescents’ well-being is significant, said the World Happiness Report 2026 today, warning that the scale of harm is significant enough to affect entire populations.
The annual report, published by the Wellbeing Research Centre at the University of Oxford, points to overwhelming evidence of both direct and indirect harm.
Direct harms include exposing them to videos of graphic pornography and real-life violence, facilitating cyberbullying and deepfakes, promoting dangerous “challenges”, connecting them with sexual predators, and facilitating the purchase of illegal drugs.
The indirect harms involve rising levels of depression, anxiety, and reduced life satisfaction.
“The harms and risks to individual users are so diverse and vast in scope that they justify the view that social media is causing harm at a population level,” the report said.
The harmful "experiences are so common that they should also count as ordinary use,” it added.
Notably, the report called the major social media platforms such as Facebook, Instagram, Snapchat, TikTok, and X, "dangerous consumer products that harm adolescents at a massive scale”.
“The evidence of harm – both direct and indirect – is so strong and comes from so many sources in so many countries that we believe policymakers around the world now have enough evidence to justify action to protect children and adolescents,” the report said.
In line with this, countries such as Australia and Indonesia recently introduced legislative restrictions on social media use among young people. In India, states including Karnataka and Andhra Pradesh have announced bans, while Bihar is considering similar measures.
The report pointed out that social media is causing direct harms to millions of people globally. This includes:
- Addiction and problematic use
- Sleep deprivation
- Sextortion
- Sexual harassment
Impact on Youth Well-being
Research cited in the report shows a clear link between heavy social media use and lower life satisfaction among adolescents. Youth and teens who spent more time on social platforms reported poorer mental well-being compared to those who used less.
Overall, internet use was linked with negative effects, particularly among girls and in countries such as the UK and Ireland. Yet, among those who used the internet for communication, learning, news consumption, and content creation, higher life satisfaction was reported.
The report noted that negative emotions are becoming more common across all regions. Worry increased among young people, while the frequency of anger declined across both younger and older populations.
Despite these trends, positive emotions still occur about twice as often as negative ones globally.
Global Happiness Rankings
Finland has been ranked the world’s happiest country for the ninth consecutive year, followed by Iceland, Denmark, and Costa Rica. Other countries in the top 10 include Sweden, Norway, the Netherlands, Israel, Luxembourg, and Switzerland.
In contrast, when measuring changes in happiness among people under 25, countries in the NANZ region -- the United States, Canada, Australia, and New Zealand -- rank much lower, placing between 122 and 133 out of 136 countries.
Menopause Can Raise Alzheimer Risk In Women, Neurologist Warns

Hormonal changes during menopause can significantly increase Alzheimer's disease (AD) risk in women, according to Dr Lisa Mosconi, a neuroscientist and women’s brain health specialist.
In a new The Journal of Clinical Investigation review, the renowned AD expert noted that menopause can change brain biology and metabolism and may contribute to amyloid plaques and tau tangles, which are key biological markers of AD.
Alzheimer disease is the most common cause of dementia, affecting over 55 million individuals worldwide, with projections exceeding 150 million by 2050 . Out of the reported cases, nearly two-third are made up of women, with the majority being postmenopausal women
Estrogen protects the brain by lowering inflammation, increasing neuronal survivals supporting non-amyloidogenic processing, and reducing amyloid-beta-related neurotoxicity, all of which are factors contributing to the development of AD.
However, when estrogen levels drop during menopause and follicle-stimulating hormone (FSH) and luteinizing hormone (LH) rise, the brain becomes more likely to develop AD-related damage.
Previous research has also shown that early menopause, especially before age 45, is linked with increased risk of dementia and the removing the ovaries before natural menopause could increase long-term dementia risk, with the greatest excess risk seen at younger ages, especially before 45.
READ MORE: Simple Blood Test Can Predict Dementia Risk in Women 25 Years Before Symptoms
What Is Alzheimer’s Disease?
Alzheimer's disease is one of the most common forms of dementia and mostly affects adults over the age of 65.
About 8.8 million Indians aged 60 and above are estimated to be living with Alzheimer's disease. Over seven million people in the US 65 and older live with the condition and over 100,00 die from it annually.
Alzheimer's disease is believed to be caused by the development of toxic amyloid and beta proteins in the brain, which can accumulate in the brain and damage cells responsible for memory.
Amyloid protein molecules stick together in brain cells, forming clumps called plaques. At the same time, tau proteins twist together in fiber-like strands called tangles. The plaques and tangles block the brain's neurons from sending electrical and chemical signals back and forth.
Over time, this disruption causes permanent damage in the brain that leads to Alzheimer's disease and dementia, causing patients to lose their ability to speak, care for themselves or even respond to the world around them.
While there is no clear cause of Alzheimer's disease, experts believe it can develop due to genetic mutations and lifestyle choices, such as physical inactivity, unhealthy diet and social isolation.
Early symptoms of Alzheimer's disease include forgetting recent events or conversations. Over time, Alzheimer's disease leads to serious memory loss and affects a person's ability to do everyday tasks.
There is no cure for this progressive brain disorder and in advanced stages, loss of brain function can cause dehydration, poor nutrition or infection. These complications can result in death.
Can You Detect Alzheimer's Early On?
The US Food and Drug Administration has approved the use of a blood test which can help diagnose Alzheimer’s disease in adults aged 55 and above.
The blood test, known as Lumipulse, can detect amyloid plaques associated with Alzheimer’s disease and has proven to be a “less invasive option” that “reduces reliance on PET scans and increases diagnosis accessibility.”
FDA Commissioner Martin A. Makary said of the landmark decision, "Alzheimer’s disease impacts too many people, more than breast cancer and prostate cancer combined.
"Knowing that 10 percent of people aged 65 and older have Alzheimer's, and that by 2050 that number is expected to double, I am hopeful that new medical products such as this one will help patients."
It remains unclear when this test will be available for commercial use across the world.
© 2024 Bennett, Coleman & Company Limited

