- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
How Our Ancestors Learned to Walk Upright: Scientists Trace the Genetic Steps

Credits: Canva
For centuries, the question of how humans became upright walkers has fascinated scientists and philosophers. Charles Darwin famously argued in The Descent of Man (1871) that humans evolved from apes, and one of the most striking transformations along the way was bipedalism. A new study, published in Nature, sheds light on the molecular and genetic steps that enabled this evolutionary leap.
The Pelvis: The Unsung Hero of Walking
Walking on two feet may feel ordinary today, but it required major anatomical innovations. At the heart of this transformation lies the ilium, the largest bone of the pelvis. This bowllike bone curves around the waist, anchors key leg muscles, supports the pelvic floor, and helps hold our internal organs in place when we stand upright.
The ilium is not only essential for walking, it plays a critical role in childbirth by forming much of the birth canal. Its shape is therefore central to two major evolutionary pressures: efficient locomotion and safe delivery of babies. Yet, until recently, the genetic blueprint behind its development remained poorly understood.
“It’s remarkable to me,” said Terence Capellini, a developmental geneticist at Harvard, “The ilium is essential to how we walk and how we give birth, and yet very little is known about it.”
Peering Into the Womb: A Molecular Detective Story
To unravel this mystery, Dr. Capellini and his team embarked on an ambitious project, analyzing how the ilium forms in embryos. Gayani Senevirathne, a postdoctoral researcher at Harvard, used fetal tissue samples from a University of Washington repository to build 3D models of ilium development and track which genes switched on and off at various stages.
The researchers didn’t stop with humans. They performed similar experiments on mice embryos and then expanded their investigation to primates, including chimpanzees, gibbons, and lemurs, by collaborating with museums across the U.S. and Europe.
Their efforts resulted in a treasure trove of data covering 18 different primate species, offering unprecedented insight into how this bone evolved over millions of years.
The Big Surprise: A Complete Flip
Conventional wisdom suggested that the human ilium should form like that of other mammals, starting as a rod of cartilage running parallel to the spine, which then curves forward over time. But the Harvard team’s results showed something entirely different.
In humans, the ilium starts as a rod perpendicular to the spine, one end pointing toward the belly and the other toward the back. Rather than gradually curving, it retains this perpendicular orientation as it grows into its final shape.
“That was really striking to us,” said Dr. Capellini. “Nowhere in the human body do you find a place where humans have just changed the way we grow altogether.”
Even more strikingly, the team found that humans use the same set of genes that mice do, but regulate them differently. Genes are switched on and off in a new pattern in human embryos, triggered by signals from surrounding cells. This change in genetic “timing and location” is what reoriented the ilium and made upright walking possible.
Evolution in Two Acts: Walking and Birthing
The researchers believe that this reorientation of the ilium was a turning point in human evolution, allowing our ancestors to grow a pelvis that could support strong leg muscles for bipedal locomotion.
But their work also revealed a second major shift that likely occurred millions of years later, linked to the rise of larger brains. They discovered that the human ilium is slower to transform from cartilage into bone compared to the rest of the skeleton, lagging by about 15 weeks.
This delay may have been a critical adaptation: as brain size increased, so did the risk of babies getting stuck in the birth canal. Natural selection favored rounder, more flexible pelvic shapes that made childbirth safer.
The Evolutionary Trade-Off
While these changes were crucial for survival, they may have also made humans more vulnerable to pelvic problems, including fractures, arthritis, and complications during delivery. Dr. Capellini and his team hope to continue studying the ilium to better understand these vulnerabilities, but funding cuts have placed future research in jeopardy.
“We are all wondering what would have come next had we not lost this funding,” he said.
Why This Matters
This discovery is more than an evolutionary curiosity, it offers a window into why the human body looks and functions the way it does today. It also highlights the delicate balance of adaptations: the very changes that allowed humans to walk upright and give birth to big-brained babies may have introduced new health challenges.
By mapping these genetic changes, scientists hope to not only reconstruct the story of our evolution but also find better ways to diagnose and treat conditions related to the pelvis and lower body.
World Oral Health Day: Your Mouth May Signal Disease Before You Even Know, According To Doctor
Credits: Canva
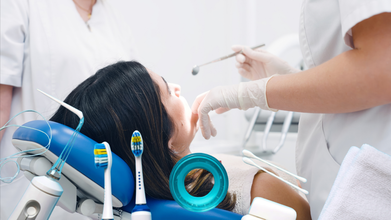
Every year on March 20, World Oral Health Day is observed to raise awareness about the importance of caring for your mouth at every stage of life. This means starting from birth through later years. However, a visit to dentist is usually the last thing anyone plans when they think of a doctor's visit. Dental visits happen only when extraction or something bigger is involved. More often than not people ignore a follow up or a regular dental checkup to maintain oral health. Why so?
In a previous interview with Health and Me Lt Gen Dr Vimal Arora, the Chief Clinical officer at Clove Dental, who has 40 years of experience as a dentist and also served in the Indian Army explained how oral health is not just about a pretty smile. He explained that many do not plan a regular visit to a dentist because the problems that pertains to oral health do not seem "life threatening".
Read: Exclusive: Astronaut Rakesh Sharma Had To Get His Wisdom Tooth Extracted Before His Trip To Space
However, Dr Arora told Health and Me that oral health can in fact be the first way to know if anyone is prone to a chronic disease.
Early Signs Of Disease Your Mouth Can Reveal
“There is now scientific evidence, published in top medical journals, that shows how oral infections can significantly worsen pre-existing systemic diseases,” says Dr. Arora. This isn’t just a theory — it’s a medically established fact.
Take diabetes, for instance. People with gum infections often find it harder to control their blood sugar levels. “If you're suffering from diabetes and you have a gum infection, your diabetes will not be well controlled. In fact, it may worsen,” he adds. The same applies to heart diseases. Oral infections can increase inflammation in the body, potentially triggering or worsening cardiovascular problems.
This is concerning especially for those people who may already be managing conditions like hypertensions, arthritis, or respiratory illness. Poor oral health can actually sabotage their efforts to stay stable.
“Your tongue is a true mirror of your oral and general health,” says Dr. Arora. The correlation therefore goes beyond just gums and teeth. Dentists are trained to detect early signs of systemic disorders simply by examining the tongue's color, coating and texture.
A pale tongue might indicate iron deficiency, while a coated tongue could be a sign of digestive issues or a viral illness. “Sometimes, we ask patients if they've had their blood work done, based purely on what we see on their tongue,” he adds. In some cases, dentists can even detect undiagnosed diabetes or early signs of nutritional deficiencies.
What Mother's Oral Health Can Predict About Their Babies
Dr. Arora also highlights the overlooked risks that pregnant women face when they neglect their dental hygiene. “If you are pregnant and suffer from periodontitis or even gingivitis — essentially poor gum health — you are at risk of having a preterm or low-birth-weight baby,” he says.
This isn’t just theory; it’s a well-documented risk in obstetric dentistry. Pregnant women are encouraged to get dental check-ups not just for themselves, but for the health of their unborn child.
Despite these evidences, oral health remains one of the most neglected aspects of personal healthcare. Dr. Arora believes this is partly due to a lack of awareness and the perception that dental problems are not "serious enough."
“People often wait until they’re in pain before they see a dentist, but by then, the damage might already be affecting other parts of the body,” he says. Preventive check-ups, regular cleaning, and treating gum infections early on can go a long way in improving not just oral health, but overall wellness.
Fact Check: Sunscreen Is Only Used For Outdoors

Credits: Canva
Most people reach for sunscreen when heading to the beach or stepping out for a long day in the sun. But skincare experts say sun protection should not be limited to vacations or outdoor activities. Sunscreen is meant to be part of a daily skincare routine.
This often raises a common question. If you are staying indoors all day, do you still need sunscreen?
Dermatologists say the answer depends on your surroundings and daily habits.
Sunlight can still reach you indoors
Many people assume that staying inside completely protects their skin from sunlight. But this is not always true.
Dr Khushboo Jha, MBBS, MD, Chief Dermatologist Consultant at Metro Hospital and Founder of One Skin Clinic, explains that sunlight entering through windows can still affect the skin.
“While standard window glass blocks most UVB rays, which cause sunburn, UVA rays can still pass through. These rays penetrate deeper into the skin and are linked to long term concerns such as premature aging, uneven pigmentation and loss of skin elasticity,” she says.
These UVA rays are often overlooked because they do not cause immediate redness or burning like UVB rays. However, over time they can lead to visible signs of skin aging and pigmentation.
When sunscreen indoors becomes important
Dermatologists say sunscreen indoors is particularly useful for people who spend long hours near windows or in well lit spaces.
Dr Jha notes that individuals who work near windows, sit in sunlit rooms or spend time driving during the day may still be exposed to sunlight. “Even short periods of daily exposure to sunlight over time can contribute to cumulative skin damage,” she explains.
In such situations, applying sunscreen in the morning can offer an added layer of protection. A broad spectrum sunscreen with at least SPF 30 is generally recommended.
This approach is especially relevant for people working in offices with large windows or those who frequently commute during daylight hours.
What if you are away from windows?
Experts also say sunscreen use indoors is not always equally necessary for everyone.
If you spend most of the day inside a room with minimal natural light and away from windows, your exposure to ultraviolet radiation becomes much lower.
Dr Jha says that in such cases the urgency of frequent sunscreen reapplication becomes less important. The risk of sun related skin damage is significantly reduced when there is little to no direct daylight entering the space.
This means sunscreen indoors should not be treated as a strict rule but rather as a flexible part of skincare based on lifestyle and environment.
What about blue light from screens?
Another topic that often comes up is blue light exposure from digital devices such as phones, laptops and tablets.
Some studies suggest that prolonged exposure to visible light may contribute to pigmentation, especially in individuals with deeper skin tones. However, dermatologists point out that the amount of blue light from electronic screens is much lower than what we receive from natural sunlight.
Dr Jha says the effect of digital screens on the skin is still being studied, but compared to sun exposure, the impact remains minimal.
A practical approach to daily skincare
Dermatologists suggest viewing sunscreen as a preventive skincare habit rather than a rigid rule.
Dr Jha recommends incorporating sunscreen into your morning routine, particularly if your day includes stepping outdoors or spending time in naturally lit environments.
In simple terms, if daylight reaches your workspace or you plan to go outside later in the day, applying sunscreen in the morning is a small step that can help protect your skin over time.
Woman Left Medically Infertile After Seven Surgeries For Endometriosis That She Did Not Have
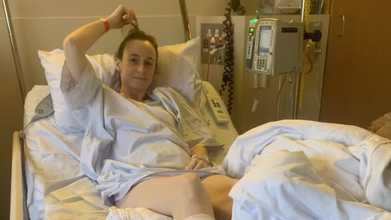
Credits: ABC News' Four Corners
At the age of 28, Courtney Paton realized she could never have children. She was medically infertile. This was after years of repeated surgeries, a total of seven, for 'suspected' endometriosis, due to which Dr Simon Gordon, Melbourne-based gynecologist removed both her ovaries and eventually her uterus.
Also Read: Menopause Can Raise Alzheimer Risk In Women, Neurologist Warns
Her story came to light through an investigation by the Australian Broadcasting Company or ABC's Four Corners, an investigation that looked at the treatment she received from Dr Gordon.
Courtney says she trusted the doctor completely. Now she says that trust has been shattered. “I feel completely betrayed by not only Simon Gordon, but by Epworth, by the healthcare system,” she told the program.
A Wrong Diagnosis That Led to Repeated Surgeries
Courtney first had laparoscopic surgery in 2018 with another surgeon, which confirmed she had endometriosis. The condition affects about one in seven Australian women and can cause severe pelvic pain and fertility problems.
Still struggling with pain, she began seeing Gordon in 2019 when she was 21.
Over the next several years she underwent seven surgeries with him. Gordon told her the procedures were necessary to treat severe endometriosis. Courtney and her family paid more than 32,000 Australian dollars for these surgeries alone.
But when investigators asked her to obtain her pathology reports, the results told a very different story. The tissue tests from most of her surgeries showed no evidence of endometriosis.
Despite this, operation reports written by Gordon continued to describe findings consistent with the disease.
Read: A Woman Lost Her Ovary To Endometriosis Surgery After Receiving An Ultimatum From Gynecologist
Removal of Both Ovaries
In 2021 Gordon removed one of Courtney’s ovaries, saying it was stuck to the pelvic wall. Later he removed the second ovary as well.
Independent specialists who reviewed the pathology for the investigation said the ovary appeared normal and there was no clear justification for removing it. One expert described the treatment as “unbelievable” after reviewing the medical records.
Medical guidelines generally advise caution when removing ovaries from young women who may want children in the future.
A Hysterectomy At 25
Despite losing both ovaries, Courtney continued to experience pelvic pain. Gordon later advised that she should undergo a hysterectomy.
Concerned, she sought a second opinion from another gynecologist who said the procedure was unnecessary and suggested non surgical treatments.
But after years of pain and repeated surgeries, Courtney says she felt desperate for relief and trusted the doctor who had treated her for so long. Her uterus was removed in 2023 when she was just 25.
Again, pathology results found no evidence of endometriosis.
Investigation and Legal Action
Courtney is now pursuing legal action through a medical negligence claim. The case has also drawn attention from regulators, with investigations underway into Gordon’s conduct.
Australia’s federal health minister Mark Butler described the allegations as “physically sickening”.
For Courtney, the emotional impact remains overwhelming.
“No woman should ever have to endure what I’ve endured,” she said. “I’ve had the opportunity to have a family taken away from me.”
© 2024 Bennett, Coleman & Company Limited

