- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
One Crucial Habit Every Diabetic Is Forgetting – And It Starts With Your Toothbrush
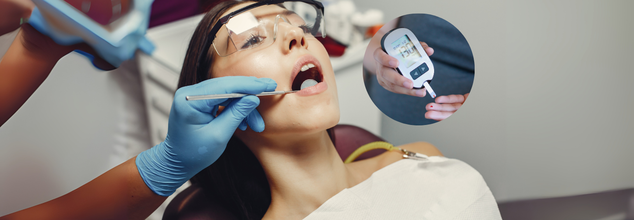
When it comes to managing diabetes, the conversation typically centers on blood sugar, insulin, and diet. However, one critical piece of the equation that usually goes unmentioned: oral health. For those who have diabetes, poor oral care can result in a chain of health issues, not only affecting teeth and gums, but possibly overall body health as well.
For millions living with diabetes, maintaining a healthy mouth is not just about preventing cavities or bad breath—it’s about safeguarding against serious complications that can affect the entire body. As diabetes rates soar globally, understanding the unique oral health challenges faced by diabetics is more important than ever.
Your mouth can reveal a lot about your health. Swollen, bleeding, or receding gums; loose teeth or missing teeth; and bad breath that won't go away are all symptoms of gum disease—something diabetes patients are particularly susceptible to. Gingivitis (mild gum disease) and periodontitis (advanced gum disease) both begin with plaque, a sticky layer of bacteria that forms on teeth. Although the bacteria themselves are not specific to diabetics, the body's inflammatory reaction to the bacteria tends to be increased in diabetics, particularly with poor blood sugar control. That enhanced inflammation may result in the loss of tissue under the teeth, ultimately leading to a loss of the teeth if not treated.
The primary distinction for individuals who have diabetes is not the bacteria involved but the increased inflammatory response of the body. Uncontrolled blood sugars enhance this inflammation, which causes wear on the tissues that hold teeth in place. This can ultimately cause teeth to fall out.
Dr. Jaineel Parekh, Orthodontist at Laxmi Dental Limited, points out, "Diabetes is a rising health issue in India, and it affects millions. Oral health is heavily linked to diabetes control, as people with diabetes are more susceptible to gum disease, which in turn can make it more difficult to control blood sugar levels."
Why Diabetics Are at Higher Risk?
Another less frequently discussed but common symptom in diabetics is dry mouth, or xerostomia. The cause can be aging, drugs, or diabetes itself. A deficiency in saliva hampers the mouth's capacity to cleanse itself naturally, and food particles, acids, and bacteria remain. This speeds up tooth decay and gum disease.
Hyperglycemia (elevated blood sugar) and hypoglycemia (low blood sugar) also cause special oral health effects. Excessive sugar levels may provide an environment conducive to fungal infections such as thrush and can retard recovery from dental procedures. Hypoglycemia management with sugar-containing substances can cause a sudden surge in mouth acidity, which can erode enamel if oral hygiene is not immediately done. Individuals with diabetes are predisposed to oral conditions for numerous reasons:
Inflammatory Response: Diabetes increases the body's inflammatory response to oral bacteria, causing gum disease to be more severe and more difficult to treat.
Dry Mouth: Medications, aging, or diabetes can all decrease saliva flow, causing dry mouth. Saliva helps to remove food particles, sugars, acids, and bacteria from the mouth. Without saliva, toxic substances remain, raising the risk of tooth decay and gum disease.
Fluctuations in Blood Sugar: Hypoglycemia (low blood sugar) and hyperglycemia (high blood sugar) episodes can both affect dental health. Hypoglycemia tends to necessitate sweetened treatments, which are mouth-acidifying and cavity-promoting, particularly if oral care isn't immediate (as at night). Hyperglycemia, by contrast, tends to dry the mouth and raise salivary sugar levels, providing a fertile ground for bacterial and fungal infection such as thrush.
Impaired Healing: High blood sugar compromises the immune system and slows down healing, which makes it more difficult for the mouth to heal. from infections, surgery, or trauma
Effective Oral Care for Individuals With Diabetes
The majority of these complications do not develop overnight. With regular care, diabetic patients can have great oral health. Here are evidence-supported strategies to save your smile:
1. Master the Fundamentals of Daily Care
Brush two times a day, using a soft-bristle toothbrush and fluoride toothpaste. Brushing should last two minutes, covering all surfaces—outer, inner, and chewing, according to the American Dental Association. Remember daily flossing to remove plaque between teeth and beneath the gum line. For those who dislike flossing, interdental brushes are useful substitutes.
2. Get Regular Dental Checkups
Strive for a visit to the dentist every six months. In instances of extensive gum disease, more cleaning visits (every three months) are suggested. Dentists can provide focused treatments, such as antibacterial mouthwashes or fluoride varnishes, and monitor changes in your oral health.
"A few good habits are practiced regularly," Dr. Parekh adds. "Dental flossing, brushing teeth, regular check-ups, and a good diet all help to prevent decay and gum disease."
3. Optimize Blood Sugar Control
Stable blood glucose aids in lowering dry mouth, preventing plaque formation, and enhancing immunity. Both high and low sugar levels have detrimental effects on oral health, so adhering to a well-managed diabetes care plan is essential.
4. Use Specialized Equipment for Improved Hygiene
Electric toothbrushes may be especially beneficial for individuals with dexterity issues. Sugar-free gum stimulates saliva, which mitigates dry mouth. Cheese and water at meals can also neutralize acids and aid in enamel health.
5. Drink Plenty and Stop Smoking
Dry mouth is worsened by dehydration. Drink water frequently, particularly after hypoglycemic treatment or sweets. Smoking complicates gum disease and impairs healing; stopping can significantly enhance oral and systemic well-being.
6. Brush Twice Daily
Use a fluoride toothpaste and a soft-bristle toothbrush, brushing for two minutes at least each time. Position the brush at a 45-degree angle against the gums and brush all surfaces well. Electric toothbrushes can be particularly useful for individuals with compromised dexterity.
7. Floss Once a Day
Everyday flossing eliminates plaque and food from between the teeth and along the gum line. If regular flossing is challenging, try using interdental brushes or water flossers.
Surprisingly, dentists can even identify signs of undiagnosed diabetes. According to a study published in BMJ Open Diabetes Research & Care, almost one in every five individuals who have severe gum disease are likely to have undiagnosed type 2 diabetes. This again supports the notion that dental treatment should be included in diabetes care.
Oral pathogens may enter the bloodstream, initiating inflammation that leads to cardiovascular disease such as atherosclerosis and putting them at risk for respiratory infection such as pneumonia. The connection between oral and general health is particularly important to those who have chronic illnesses such as diabetes.
"Neglecting oral hygiene is not only doing a disservice to the mouth," Dr. Parekh says. "It has the potential to affect heart health, respiratory function, and overall quality of life."
Oral care must be a foundation of diabetes treatment. With good habits and frequent professional care, diabetics can help safeguard their teeth, gums, and overall health. Summing up, as Dr. Parekh says, "Good oral hygiene is important for diabetic patients not to develop complications. Brush, floss, dental visits every six months, and a healthy diet are the keys to long-term health.".
Ozempic may reduce depression and anxiety risks in diabetics: The Lancet
Credit: iStock
While GLP-1 drugs like Ozempic are popular for weight loss, a new study published today in The Lancet Psychiatry journal showed that it can also help tackle the burden of depression, anxiety, and self-harm in high-risk diabetic patients.
The GLP-1 drugs, with ingredients such as semaglutide and liraglutide, were found to effectively reduce the risk of these mental health conditions in patients already taking the medications to manage their diabetes or obesity.
Also Read: ACC/AHA Cholesterol Guidelines 2026 Explained: Start Screening For Cardiovascular Diseases Early
The study found that these medications were linked to
- fewer psychiatric hospitalizations,
- taking sick leave due to mental illness,
- death by suicide.
The study comes as people with diabetes are known to have a higher risk of depression (2-3 times), anxiety (20 percent), and suicide than the general population.
“Our findings suggest that GLP-1 drugs, particularly semaglutide, might contribute to better mental health in people with diabetes and obesity,” said Jari Tiihonen, specialist physician and professor at the Centre for Psychiatry Research, Karolinska Institutet, Sweden.
Calling the results "observational", Tiihonen urged the need for controlled clinical trials to confirm the findings.
Also read: Ozempic Can Help People With Diabetes Walk Better Despite Poor Blood Flow To Legs
Key Findings
The researchers followed more than 95,000 participants diagnosed with depression or anxiety and were prescribed various antidiabetic medications through Swedish national registers between 2009 and 2022. Of the patients, 22,480 had used GLP-1 drugs.
Semaglutide, the main ingredient in Ozempic, showed the highest benefits against the mental health conditions. Semaglutide led to a:
- 42 percent reduced risk of worsening mental health
- 44 percent lower risk of worsening depression,
- 38 percent lower risk of worsening anxiety,
- 47 percent lower risk of worsening substance use disorder.
On the other hand, liraglutide, sold under the brand names Victoza (for type 2 diabetes) and Saxenda (for chronic weight management), was linked to an 18 percent lower risk of worsening mental health.
Other GLP-1 medications, including exenatide and dulaglutide, did not show the same benefit.
Also read: Oprah Winfrey Sparks Ozempic Buzz at Paris Fashion Week with Slim Figure
How Do GLP-1 Medicines Fight Against Addiction?
A recent study, published by researchers at the Washington University School of Medicine in St Louis, reported that Ozempic could prevent substance use disorder and could also treat it.
Not just the lack of will to eat food, but some people have actually reported a lack of interest in alcohol or nicotine consumption.
Previously, observational studies have also shown how it could lower the risk of alcohol and cannabis use disorders, opioid overdose, and alcohol related hospitalization.
The findings published in The BMJ showed that people taking GLP-1 drugs had a 14 percent lower risk of developing any substance use disorder.
Their substance-specific reductions:
- Alcohol use disorder risk fell by 18 percent
- Cannabis use disorder fell by 14 percent
- Cocaine and nicotine use disorders fell by 20 percent
- Opioid use disorder fell by 25 percent
Why Are Gut Problems Like Bloating, Gas, and Constipation Increasing Today?
Credit: iStock
Digestive problems like bloating, gas, acidity, and constipation have quietly become a common problem in our daily lives. It is common these days to find people experiencing discomfort after meals or feeling unusually heavy. While these problems may not be serious in nature, doctors say these problems have increased in recent times due to changes in the way people live and eat.
- The first major cause of these problems in recent times is the change in the way people eat. It is a known fact that people are now eating more of junk food and less of fiber-rich food. Fiber plays a crucial role in keeping digestion smooth and bowel movements normal. If the amount of fiber in the diet is low, digestion becomes slow, leading to bloating, gas, and constipation.
- Another major cause of these problems in recent times is the sedentary lifestyle people are leading these days. It is a known fact that a person should move around a lot in a day. Lack of physical activity may cause problems in digestion. Simple habits like eating quickly, missing meals, or drinking excessive carbonated beverages are some of the common causes of excessive gas and discomfort.
- Another cause of digestive upsets that is often overlooked is stress. The fact that the brain and digestive system are closely related means that digestive upsets can be caused by emotional stress. When a person is under a lot of stress, hormones are secreted into their system that can slow down digestion. As a result, a person may feel stomach upsets like tightness, bloating, irregular bowel movements, or even develop a medical condition like irritable bowel syndrome depending on their digestive system composition.
- In addition to that, other lifestyle habits like late-night meals, lack of proper sleep, dehydration, or excessive caffeine intake can cause digestive upsets. When a person’s body is out of sync, digestion is not as effective as it should be. As a result, food ferments in the stomach, leading to excessive gas production.
Traditional Remedies
Most people tend to use various remedies when they are feeling unwell.
Also Read: Why Regulatory Clarity Is Important for Safe Aesthetic Procedures in India
Remedies such as the consumption of warm water, fennel seeds, ginger tea, and the intake of probiotics in the form of curd may offer temporary relief. However, it is important to note that these might offer temporary relief and might not be effective if the symptoms of digestive discomfort are recurring.
Digestive discomforts that recur frequently should not be taken lightly. Frequent occurrences of digestive discomforts such as bloating and constipation might sometimes be symptoms of an underlying condition.
Therefore, if the symptoms of digestive discomfort last for weeks and if the symptoms also include the presence of any of the aforementioned symptoms of digestive discomfort, it might be important to consult a doctor.
Gut Problems: Need For Lifestyle Modifications
The relationship between gut health and wellbeing is also well noted. Among the lifestyle modifications that may be implemented for improved digestive health is a healthy and balanced diet, exercising regularly, adequate intake of water, stress levels, and eating at regular times.
It is a normal occurrence for people to experience bloating and gas at some point in their lives. However, if discomfort in the digestive system is a frequent occurrence, it may be a wake-up call from the body that something is amiss and deserves attention. Heeding such a call and making lifestyle modifications may work wonders for the gut.
Why Regulatory Clarity Is Important for Safe Aesthetic Procedures in India
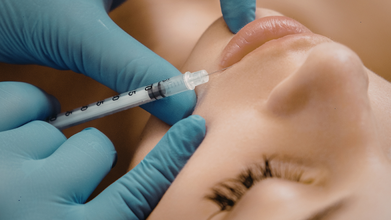
Credit: Canva
Aesthetic medicine in India has been expanding rapidly in the past decade. There is increasing demand for more minimally invasive cosmetic treatments such as injectables (botox and dermal fillers), laser treatments, and hair restoration procedures.
According to the International Society of Aesthetic Plastic Surgery (ISAPS) report, more than 1.29 million procedures have been recorded in 2024 for cosmetic treatments. India has successfully entered the top 5 countries in the world for aesthetic procedures.
Also Read: Why Are Gut Problems Like Bloating, Gas, and Constipation Increasing Today?
Although this shows the increased demand for aesthetic medicine, there is an even larger concern that there is little to no regulation to protect the consumers.
Aesthetic Services: No Regulatory Clarity
Aesthetic services and practices in India have an unclear position which has been increasing concern for stakeholders in the industry. Medical specialties like dermatology and aesthetic medicine have been recognized fields that require training, clinical judgement, and sterile environments, but cosmetology is largely non-medical. However, that is not the case. For instance, there are many beauty centers and spas that offer procedures of medical aesthetic services like chemical peels, laser treatments, and injectables.
Regulatory clarity addresses the issue by describing who can do aesthetic procedures, and the conditions required for them to do so. Absence of such descriptions could allow low-practice and trained personnel to do procedures that carry risk for infection, scarring, burning, or other dissatisfactory results and complications. There are licensing and enforcement ambiguities that are giving the ability to practitioners to call themselves "cosmetic surgeons" without any training in plastic surgery.
Need For Strong Regulatory System
A strong system of regulations is also in the interest of uniformity in clinical practices. Regulations may lay down the minimum requirements for the infrastructure of aesthetic clinics so that they can provide sterile equipment, emergency protocols, and trained medical personnel. Regulations can also mandate obtaining informed consent, so that patients know the risks, benefits, and likely results of a procedure.
A further important role for regulations is to prevent misleading advertisements, and unscrupulous behavior. The competitive field of aesthetics invites patients based on exaggerated, and unfulfilled promises. Patients can be misled if there are no regulations to relatively eliminate the occurrence.
Trust from patients stems from regulatory transparency. Accreditation of clinics and the specialties of staff performing the procedures reassure patients regarding safety, hygiene, and postoperative care. This ultimately increases the standard of the aesthetic industry for patients and ethical practitioners.
As aesthetic medicine continues to develop in India, the evolving regulatory mechanisms will be essential in continuing to promote innovation while ensuring the safety of patients. Greater regulatory documentation, transparency from governing bodies, and public education regarding evolving safety regulations will safeguard the aesthetic space from practitioners prioritizing profit over ethics.
Besides recommending patients needing aesthetic treatment to consult a licensed plastic surgeon or dermatologist, they ensure that intricate aesthetic procedures are performed in clinical environments by qualified personnel.
© 2024 Bennett, Coleman & Company Limited

