- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
- Web Stories
Pablo Escobar And Ecuador's Most Wanted Criminal, All Had This One Disease In Common - Gastritis

Credits: Canva, Wikimedia Commons, NBC
When you hear of the drug lord Pablo Escobar, you think of someone uncatchable, beyond the law. However, it is because of such a personality that we often forget that he too has everyday problems like us, including health issues, which may have cost their lives too.
"Gastritis won't leave me alone," was one of the phrases the drug lord mentioned during the calls he had with his son and wife. One day, these were the calls that made it possible to catch him. Not just him, but also Ecuador's wanted criminal 'Fito', José Adolfo Macias Vilamar, who is the leader of Los Choneros too suffered from the same. On June 25, he was finally captured.
Drug Lords And Heart Diseases
It is Fito's medicines that gave him away. It was in the bunker of his house, or the appropriate word for it would be a hole, out of which Fito appeared. But, how did the authority know he would be in that hole, in the property? The authorities found products for heartburn and gastritis, such as Diatrol, Dexopal, and Omeprazole. This is what made them certain that Fito in fact was there. They also found medicines for treating skin conditions, such as Platsul and Itrafung, an insulin used by him to treat his diabetes.
"Fito has a serious gastritis problem and is taking some medication," said Interior Minister John Reimberg. Gastritis and heartburn was also suffered by the founder of Medellín cartel, Escobar.
After escaping from La Catedral in 1992, Escobar began hiding from authorities without the power he had during much of his criminal heyday, which prevented him from accessing the drugs he used to treat his gastritis.
What Is Gastritis?
As per John Hopkins Medicine, it is inflammation of the stomach lining. Your stomach lining is strong. In most cases, acid does not hurt it. But it can get inflamed and irritated if you drink too much alcohol, have damage from nonsteroidal anti-inflammatory drugs (called NSAIDs), or smoke.
What May Have Caused It?
For Drug lords, lavish parties, alcohol use, and extreme stress to find an escape is common. These are the exact causes of gastritis.
Lifestyle habits that can cause gastritis include:
- Drinking too much alcohol
- Smoking
- Extreme stress. This can be from serious or life-threatening health problems
- Long-term use of aspirin and NSAIDs
Health issues that too could lead to this:
- Infection caused by bacteria or viruses
- Major surgery
- Traumatic injury or burns
Diseases like autoimmune disorders, where you immune system attacks your body's healthy cells by mistake, or chronic bile reflux, where bile backs up into your stomach and food pipe (esophagus) could also cause gastritis.
Common Symptoms
- Stomach upset or pain
- Belching and hiccups
- Nausea and vomiting
- Feeling of fullness or burning in your stomach
- Loss of appetite
- Blood in your vomit or black stool. This is a sign that your stomach lining may be bleeding
Could It Lead To Complications?
Chronic gastritis hurts your stomach lining. It can raise your risk for other health problems. These include:
- Peptic ulcer disease. This causes painful sores in your upper digestive tract
- Gastric polyps. These are small masses of cells that form on the inside lining of your stomach
- Stomach tumors. These can be cancer or not cancer (benign)
- A hole (perforation) of the stomach
Ozempic, Wegovy Aren't Magic, These 5 Body Traits Predict If You’ll Actually Lose Weight
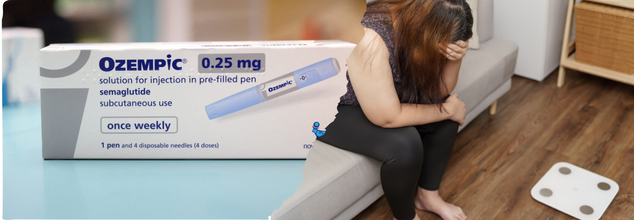
Credits: Canva/Reuters
For anyone who's been following the meteoric rise of weight-loss injections like Ozempic and Wegovy, one thing is certain: these medications are effective but not for everyone. Now, a new, in-depth study might know why.
Appearing in the journal Diabetes, Obesity and Metabolism, this new research has identified key determinants of who is most likely to thrive on GLP-1 receptor agonists (GLP-1RAs), a drug class that includes semaglutide (Ozempic/Wegovy). Ranging from use duration to body composition, and from metabolic rate to diabetic status, the results yield a finer set of directions for individualized obesity treatment—and may potentially minimize the guesswork that too often vexes patients and clinicians alike.
GLP-1RAs are drugs initially made to treat type 2 diabetes but have produced miraculous outcomes for the treatment of obesity. They function by duplicating a hormone that occurs naturally in the body, which suppresses hunger and controls the blood sugar levels. Semaglutide, the drug behind Ozempic and Wegovy, has assisted individuals in losing an average of 15–21% of their body weight when combined with diet and lifestyle modifications.
Even with all the news-grabbing changes and social media hype, results are all over the place. Some patients lose weight rapidly, others plateau, and some develop side effects such as nausea that cause them to quit cold turkey. The new research, performed at Peking University People's Hospital, sheds some light on why.
Scientists monitored 679 overweight or obese patients who initiated GLP-1RA treatment between November 2022 and October 2024 at an obesity clinic in Beijing. For 12 months, they monitored a range of physical and metabolic factors to determine what characteristics were associated with improved outcomes.
Patients taking GLP-1RAs for extended periods, particularly semaglutide, had higher odds of significant weight loss. But more than how long the patient was on the drug, study authors determined that individual traits mattered substantially in effectiveness.
In particular, individuals who did not have diabetes, had a higher percentage of body fat, larger amounts of skeletal muscle, and a higher rate of basal metabolism were found to be more likely to succeed. Also, higher serum creatinine levels (a marker for muscle mass and kidney function) were associated with improved success.
Role of Muscle Mass and Metabolism
GLP-1s are effective devices, but they need to be combined with muscle-sparing measures. Most patients inadvertently lose lean muscle mass, which can lower metabolism and undermine long-term weight control.
That is, the scale may fall, but what you lose is important. Retaining muscle mass is essential to long-term health and success. Because of this, experts suggest a two-prong approach: savvy, high-protein eating and regular strength training to help maintain lean tissue throughout treatment.
5 Body Traits That Predict If You'll Actually Lose Weight on GLP-1 Drugs
New research is showing that not everyone responds the same way to GLP-1 receptor agonists—and your body’s makeup may be the key to understanding why. Here are five physical traits that strongly predict whether you’ll shed pounds successfully while on these weight-loss medications:
1. Higher Body Fat Percentage
Individuals with excess body fat at the beginning of treatment respond to GLP-1 drugs more favorably. Why? They attack hunger and fat storage, so people with more to lose are more likely to see faster and more dramatic results.
2. Increased Skeletal Muscle Mass
Muscle is not only for power—it burns calories even at rest. Individuals with greater skeletal muscle mass (particularly in the arms, legs, and abdomen) tend to have a quicker metabolism, which can strengthen the actions of weight-loss drugs.
3. Increased Basal Metabolic Rate (BMR)
A greater BMR indicates that your body expends more energy on a daily basis. Individuals with naturally quicker metabolisms are more apt to experience efficient and long-lasting weight loss when taking GLP-1RAs such as semaglutide.
4. Greater Serum Creatinine Levels
This marker is most commonly associated with muscle mass and kidney function. Individuals with slightly elevated (but normal) levels of creatinine—usually an indicator of greater lean body mass—tended to respond more favorably to these drugs.
5. No Diagnosis of Diabetes
Against expectation, individuals with no diabetes experienced more success than those with diabetes. This could be explained by improved insulin sensitivity, reduced metabolic resistance, or fewer pre-existing complications that would interfere with weight reduction.
How Your Diabetes Status Is Important?
The research demonstrated that those without diabetes had considerably higher chances of being successful with weight loss compared to those with prediabetes or diabetes. This could be because of deep-rooted metabolic distinctions or that GLP-1RAs react differently in states of insulin resistance.
Lead researcher Dr. Linong Ji described, "This study highlights the value of metabolic state-matched strategies. Individuals with diabetes can benefit from a different or more combined regimen."
Consistency is key, patients who remained on the drug for a longer period were more likely to lose weight. Those who dropped out early because of side effects, lack of response, or lifestyle interference were far less successful.
This accords with demands from doctors for improved support for adherence. Greater follow-up frequencies, tailored coaching, and symptom control can avert early dropouts.
"Adherence to medication is neglected but equally important as the medicine itself," the authors stated. "Physicians must assist patients in staying on track, especially for the first months or so."
Side Effects of GLP-1 Drugs
Side effects, particularly gastrointestinal such as nausea, constipation, or vomiting, are still the number one reasons individuals drop out of GLP-1RAs. That's where tailoring treatment comes into play even more so.
Take, for instance, individuals who have less skeletal muscle mass. These individuals are likely to be more susceptible to fatigue and muscle wasting, enhancing dropout risk. Tweaking dose schedules, incorporating physical therapy, or emphasizing diet quality can all help mitigate these problems.
The global rise of drugs like Wegovy isn’t just hype. These medications are proving to be some of the most effective tools we’ve ever had in the fight against obesity, a condition affecting over 650 million people worldwide but what this new study makes clear is that weight loss is not one-size-fits-all, even with powerful drugs. Body composition, muscle mass, metabolic health, and individual biology all play a role.
For doctors, that equates to taking a precision medicine approach—tailoring treatments based on an individual's profile, instead of simply dosing all patients the same.
And for patients? It's a reminder that medications such as Ozempic and Wegovy can be remarkably powerful but only as part of an integrated, personalized plan that values the complexity of your body.
GLP-1 medications are revolutionizing weight control, but as this study reveals, success is not arbitrary success is individual. Understanding what influences results can enable more individuals to achieve potential through progress.
What's The Confusion! Why Most Women Don’t Know When To Start Mammogram Screenings?

Credits: Canva
Breast cancer is one of the most treatable cancers when caught early. Yet, a significant number of women remain unclear about one of the most crucial tools for early detection: the mammogram. A new survey by the Annenberg Public Policy Center (APPC) reveals just how persistent and widespread the confusion is over when women should start getting screened. Despite updated national guidelines recommending mammograms beginning at age 40, nearly half of the adults surveyed in the US are either misinformed or confused.
The US Preventive Services Task Force (USPSTF) issued a revised recommendation in April 2024, advising that women at average risk of breast cancer begin screening mammograms every other year starting at age 40. This update rolled back an earlier guideline that suggested beginning at age 50, a shift that aligns more closely with what other medical bodies have long recommended.
The American Cancer Society, for instance, has consistently recommended that women aged 40 to 44 have the option to begin annual screening, with stronger guidance to start annually from age 45. By age 55, women can shift to screenings every other year.
But with a history of back-and-forth on these guidelines, public understanding hasn’t caught up.
"Confusion can arise when medical guidance about detection or treatment changes," said Kathleen Hall Jamieson, director of the APPC. “Our data suggest that the recommendation that such screening ordinarily start at 40 years old is not yet widely enough known.”
The APPC’s April 2024 survey sampled over 1,600 U.S. adults. The results were telling:
- Only 49% correctly identified age 40 as the right age to begin biennial mammograms for women at average risk.
- A notable 10% said screenings should begin at age 20, while 21% selected age 30. 8% said 50, and 11% admitted they were unsure.
Even more telling: this level of awareness remained unchanged from a previous survey conducted before the updated guidelines were published. So while the medical advice evolved, public understanding stood still.
Is Misinformation Creating Confusion?
Women aged 40–49 were the most informed demographic in the survey—72% of them knew screenings should begin at 40. But awareness dropped significantly among younger groups. Only 37% of women aged 18–29 knew the correct age to begin mammograms and a concerning 27% of that group mistakenly thought the correct age was 30, while 16% didn’t know at all.
This gap in understanding matters because younger women especially those with family history or genetic predisposition, may need to start even earlier.
What Are Mammograms?
A mammogram is a low-dose X-ray that captures detailed images of breast tissue, capable of identifying cancers before any physical symptoms appear.
In women with a BRCA1 or BRCA2 gene mutation who are referred to as "high risk" or with a history of radiation to the chest between ages 10 and 30, screening may start as early as age 30 and include annual breast MRIs alongside mammograms.
Modern technology has made the process quicker and less painful. Better compression paddles, 3D mammograms, and AI-assisted readings now reduce both discomfort and the chance of error.
Despite technological improvements, mammograms are not infallible. Their accuracy ranges between 85–90%, and performance can dip in women with dense breast tissue.
Contrast-enhanced digital mammography (CEDM) is another newer innovation helping radiologists identify tricky cases. The integration of artificial intelligence is also streamlining diagnostic accuracy.
Does 'Abnormal' Mammogram Mean Cancer?
An abnormal mammogram result doesn’t necessarily mean breast cancer. It simply means something unusual has been spotted and warrants further testing, which could include a breast ultrasound, MRI, or even a biopsy.
In the US, follow-up care is typically swift, with guidelines in place to ensure patients are informed and supported. However, disparities in healthcare access especially for uninsured or not populations still persist.
The APPC survey’s findings highlight a deeper issue, how public health communication is struggling to keep up with shifting medical guidelines. When official recommendations change, the burden of clarity shouldn’t fall solely on the individual. It requires coordinated messaging across healthcare providers, public health agencies, insurers, and the media.
While mammograms are widely available in the U.S., access isn’t always equitable. Low-income communities and communities of color often face hurdles ranging from cost and insurance barriers to logistical challenges like transportation or time off work.
Breast cancer remains one of the leading causes of cancer death among women. Early detection significantly improves outcomes, but only if women are aware and empowered to begin screening at the appropriate time.
If you're approaching 40, talk to your doctor about when to begin screening especially if you have additional risk factors. Don’t wait for symptoms to show up.
From ADHD To Burnout: Why Modern Life Is Making You Sleepless, Anxious And Insomniac

Credits: Canva
Your struggle to fall asleep, stay asleep, or wake up rested? It’s not just on you. And it never really has been. For centuries, sleep has been a fragile and complicated process. Historically, it took place in overcrowded, uncomfortable homes, alongside families, fire smoke, bugs, animals, and the unpredictable dangers of the night. In those times, people prayed for safety more than they prayed for dreams.
Fast forward to today — temperature-controlled bedrooms, memory foam mattresses, sleep masks, blackout curtains — and yet, millions are still wide awake at 3 AM, staring at the ceiling, wondering what’s broken.
It’s not just about your mattress or screen time. Your body isn’t failing you. It’s that the world you live in is making rest harder than it should be.
In 2020, over 14% of adults in the US reported struggling to fall asleep on most days, according to the National Health Interview Survey. About 12% have been diagnosed with chronic insomnia.
A third of American adults don’t get the recommended seven hours of sleep per night. And that lack of rest isn’t distributed equally: Native Hawaiian, Pacific Islander, and Black adults, along with those earning under $15,000 a year, are the most sleep-deprived.
What this really means is: sleep loss isn’t just a personal health issue. It’s a socioeconomic one.
You’re Not Lazy — The System Isn’t Built for Rest
We live in a society that glorifies hustle, devalues downtime, and equates sleep with laziness. We’re constantly connected, bombarded with notifications, and working longer hours — even when we're off the clock.
And then there's revenge bedtime procrastination — the habit of staying up late because it’s the only time you have for yourself. We scroll through emotionally charged or overstimulating content on our phones, even though we know it's sabotaging our sleep. We drink coffee too late. We binge-watch one more episode. We use alcohol to unwind, which only fragments sleep more.
Ironically, even the wellness-obsessed are losing sleep trying to perfect it — tracking every breath, wearing sleep rings, taping their mouths shut, and obsessing over micro-wakeups. Experts say this hyper-focus on sleep performance can actually heighten anxiety and worsen insomnia.
The truth is, many factors that destroy your sleep are beyond your control.
Shift workers — who make up 20% of the US labor force — have sleep cycles dictated by employers, not biology. Irregular schedules disrupt circadian rhythms and increase the risk of sleep disorders. Studies show that people of color are more likely to work alternating shifts, compounding their sleep challenges.
Lack of basic sleep-friendly infrastructure is another major barrier. People living in noisy, polluted, or unsafe neighborhoods — often low-income communities — face chronic sleep disruptions. Bright street lights, traffic noise, subpar housing, no access to air conditioning or heating — these all add up.
And then there’s the toll of racism and discrimination. Research shows that the stress from daily microaggressions and systemic injustice has a measurable impact on sleep quality and duration.
For many, sleep is not just elusive — it’s systematically denied.
Is Parenting and Caregiving Fuelling The Quiet Sleep Crisis?
Caregivers are among the most sleep-deprived populations. Babies, toddlers, aging parents — their needs don’t clock out at night. Sleep training might work for infants, but there's no such system for grown-up responsibilities.
If you're a new parent or a caregiver running on fumes, advice like “just wind down before bed” rings hollow. For people in this group, it’s not about willpower or habits — it's about survival.
Now add neurodivergence to the mix. A new study in BMJ Mental Health finds that adults with higher ADHD traits are significantly more likely to report insomnia, low sleep quality, and — unsurprisingly — a lower quality of life.
The research suggests that insomnia may be the link between ADHD symptoms and reduced life satisfaction. And while ADHD and insomnia both independently affect mood and functioning, their overlap is a major red flag.
The traditional treatment for one often ignores the other. Experts now advocate for targeted sleep therapies like Cognitive Behavioral Therapy for Insomnia (CBT-I) or Sleep Restriction Therapy to improve both sleep and daily functioning in adults with ADHD traits.
How Can You Sleep Better?
First, stop blaming yourself. Instead of focusing solely on sleep hygiene tips like cool rooms and no screens, try identifying what’s really keeping you up. Is it your work schedule? Your housing situation? Noise? Anxiety? All of the above?
If possible, consult a sleep medicine specialist to rule out disorders like insomnia, apnea, or circadian rhythm disruptions. If therapy is an option, CBT-I has proven effective for many.
For those dealing with unavoidable stressors — think shift work, noisy neighborhoods, caring for kids — small tools may help. White noise machines, blackout curtains, cooling fans, sleep earplugs. They’re not perfect, but they can create small windows of peace.
The goal isn’t eight perfect hours. It’s about carving out enough restorative rest — wherever and however possible — to function and feel human.
Sleep isn’t optional. It’s biological. Your body wants to rest. Your brain needs it. And even though society isn’t built to support that, the rhythm is still there — pulsing under the noise, waiting to be reclaimed.
So, maybe tonight, instead of battling the night like an enemy, trust your body. Dim the lights, breathe and let sleep come — if not easily, then at least without shame because the struggle to sleep isn’t yours alone.
Disclaimer: This article may include interpretations of research, and commentary that reflect individual or editorial perspectives. It is intended for informational purposes only and should not be considered a substitute for professional medical advice
© 2024 Bennett, Coleman & Company Limited

