- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
We've Heard About Endometriosis, But What Is Adenomyosis And How Did It Become A Missed Disease?

Credits: iStock/Canva
Many women are speaking up about their delayed diagnosis for endometriosis, which affects 42 million women in India, and around 250 million women worldwide. However, what not many are talking about is adenomyosis, which affects around 1 in 5 premenopausal women.
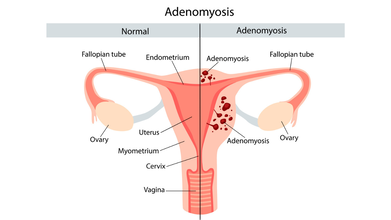
What Is Adenomyosis?
It is when a tissue similar to the lining of your uterus or the endometrium starts to grow muscle wall of your uterus. It causes the uterus to thicken and enlarge, sometimes double or even triple the usual size.
It could lead to painful and heavy period and prolonged menstrual bleeding with clotting and abdominal or pelvic pain.
To get a better understanding, Health and Me spoke to Dr Prachi Sarin Sethi, Senior Consultant, Obstetrician, Gynecologist and Laparoscopic Surgeon at Motherhood Hospitals, Gurugram, who said, “Adenomyosis is one of the most underdiagnosed causes of chronic pelvic pain, heavy periods, and infertility, often mistaken for fibroids or endometriosis.”
The worst part, like in the case of endometriosis, women are often told that their symptoms of "normal", pointed out the doctor.
"Painful periods should never be dismissed as a routine part of womanhood. Persistent symptoms deserve medical attention," she says. The doctor also explains that in this condition, the trapped tissue "behaves like normal menstrual lining, but it cannot exit the body and so it leads to ongoing pain and uterine enlargement".
While the cause is yet not known, doctor points out it is due to hormonal imbalance, especially excess estrogen. "The condition is most commonly seen in women between 30 and 45 years of age, particularly those with a history of childbirth or uterine surgery."
Read: Is Uterus Removal The Only Treatment For Endometriosis?
The diagnosis is often missed because the symptoms closely overlap with fibroids and endometriosis, which makes the accurate diagnosis challenging. “Unlike fibroids, adenomyosis causes diffuse thickening of the uterine muscle, and unlike endometriosis, it remains confined within the uterus,” explains Dr Sarin Sethi. However, with better imaging techniques and increased awareness, adenomyosis can now be diagnosed earlier and more accurately.
What Are The Common Symptoms Of Adenomyosis?
About 1 in 3 people with adenomyosis do not show any signs or symptoms, however, those who do, these could be the common symptoms:
- Painful menstrual cramps (dysmenorrhea).
- Heavy menstrual bleeding (menorrhagia).
- Abnormal menstruation.
- Pelvic pain with or without severe cramping.
- Painful intercourse (dyspareunia).
- Infertility.
- Enlarged uterus.
- Bloating or fullness in your belly (adenomyosis belly).
How Can One Diagnose Adenomyosis?
Pelvic Examination could tell whether your uterus has gotten larger, softer, or is painful to the touch.
Ultrasound can also produce images of your pelvic organs and show whether there is any thickening of the uterus wall.
Imaging scans using MRI could show uterine enlargement and thickening of certain areas of your uterus.
Dr Sarin Sethi says, “Contrary to popular belief, adenomyosis does not always require removal of the uterus, and many women can be managed with fertility-preserving treatments.”
Ozempic Burps Decoded: Diabetes Expert Reveals What Doctors Won’t
Credit: Canva
Been wondering what are Ozempic burps and how the drug works inside your body?
In a podcast episode of The Diary Of A CEO, insulin resistance expert Dr Benjamin Bikman explains how the blockbuster GLP-1 drug can alter the digestion process in your body to reduce weight.
Dr Bikman, a Professor of Cell Biology and Physiology at Brigham Young University in Utah explained: "GLP-1 is primarily a satiety hormone. It'll tell the brain that we're done eating and it will slow down the intestines significantly."
Ozempic (semaglutide) is a prescription injectable GLP-1 medication primarily approved for adults with Type 2 diabetes to manage blood sugar levels. However, the drug has gained immense popularity among those trying to lose weight as it can reduce hunger and help people feel full for longer, which forces the body to burn fat deposits to stay functional.
In clinical trials, people with obesity using semaglutide have shown to lose an average of about 15% of their body weight over 68 weeks. Most people begin to see noticeable results within 8 to 12 weeks of taking the drug.
The official price in India for a once-weekly Ozempic injection pen ranges from approximately ₹8,800 for the 0.25 mg dose to around ₹11,175 for the 1 mg dose per month. Insurance coverage is generally inconsistent for weight loss indications.
How Does Ozempic Change Your Digestion?
According to Dr Bikman, ingested food sits in the stomach and intestines for about six hours on average for digestion. However, when the body receives GLP-1 hormones from injections, the body will considerably slow down the digestion process and food can stay in the body for about 24 hours.
"If we injected ourselves with a GLP-1 drug, which puts an artificial amount of GLP-1 in our body, boom, we shoot it in. Then it would it slows down people's intestines so much that they'll have food sitting in there for 24 hours," he said during the episode.
Experts have previously noted that slowing down the digestion process on purpose using drugs is unhealthy and risky unless done under strict medical supervision to treat a specific condition (such as chronic diarrhea or dumping syndrome as it can lead to gastroparesis.
Gastroparesis is a condition that occurs when the stomach muscles become weak and slow, failing to move food into the small intestine which can reduce nutrient absorption in the body and severe constipation. It can also form a hard mass called a bezoar, which can cause blockages and may require surgery.
What Are Ozempic Burps?
As the food continues to sit in the body, it create bubbles and gas inside the stomach which leads to intense burps also know as Ozempic burps."So, one of the things people talk about is what's called Ozempic burps where they just have this kind of belching bubbling gas because the food is sitting in the stomach for way longer than it's supposed to.
"So, no surprise the people are less interested in food. GLP-1 tells the brain they don't need to eat as much and slows down the intestines," Dr Bikman noted.
READ MORE: Wegovy 7.2 mg: Higher-Dose Weight-Loss Jab Cleared For Launch In UK
Can You Regain Your Ozempic Weight?
Yes. A new BMJ study has found that people who stop using weight-loss medications can regain weight and return their original size within two years.
Researchers have found that those who lose weight using blockbuster GLP-1 drugs such as Ozempic could regain about 0.4kg every month after quitting these treatments. In contrast, those who lost weight through exercise, diet and other factors only gained 0.1kg.
UK Toddler Dies Of Rare Kawasaki Disease: What You Need To Know

Credit: Canva
A two-year-old boy from Bristol, UK has died from a rare heart disease, known to mostly affect children with only flu-like symptoms, on January 8.
Hudson Martin had been diagnosed with Kawasaki disease when he was seven months old and was placed on lifelong medication including aspirin and blood thinners to reduce the risk of clots. Since then, he had been living a normal and happy life, according to father Damien Martin.
He told Bristol Live: "You’d never know anything was wrong from pictures or videos. He bounced off everything. He loved climbing, dancing, music, he was a proper daredevil."
But days before his third birthday, he suddenly collapsed while playing at home. Despite being given CPR by paramedics for an hour, his heart did not restart and he passed away.
“They did absolutely everything they could,” Damien said. "His heart just wouldn't come back."
What Is Kawasaki Disease?
Also known as mucocutaneous lymph node syndrome, Kawasaki disease causes inflammation in the walls of small to medium-sized blood vessels that carry blood throughout the body which can damage to the heart and blood vessels, mostly in children younger than five years old.
When this happens, the heart doesn't work as well to pump blood to the body and could burst (coronary artery dilation and aneurysms). It also causes swelling in the lymph nodes and mucous membranes inside the mouth, nose, eyes and throat.
Apart from a 102.2 degrees Fahrenheit (39 degrees Celsius) fever that can last for five days, children with Kawasaki may also experience some or all of the following symptoms:
- Rash on the main part of the body or in the genital area
- Swelling and redness of their hands and feet
- Irritation and redness of the whites of their eyes
- Swollen lymph glands in the neck
- Irritation and inflammation of the mouth, lips, and throat
It remains unknown what causes Kawasaki disease in children and if it affects adults.
Diagnosis involves ruling out other diseases that cause the same symptoms which include:
- Scarlet fever
- Juvenile rheumatoid arthritis
- Stevens-Johnson syndrome (a disorder of the mucous membranes)
- Toxic shock syndrome
- Measles
- Some illnesses caused by ticks, such as Rocky Mountain spotted fever
Is It Curable?
While this non-contagious disease can be treated with a mixture of antibodies given through the veins (intravenous immunoglobulin) and aspirin, it remains uncurable. Doctors may also advice steroids if intravenous immunoglobulin is not effective.
After receiving treatment for Kawasaki disease, most children recover fully and long-term follow-up care remains unnecessary. However, children who have suffered through aneurysms or other complications related to the disease will need lifelong monitoring with a cardiologist.
Scabies UK: Can Ivermectin Help Treat Scabies In Children Safely?
Credits: AI Generated
Cases of scabies, a highly contagious skin condition caused by microscopic mites, continue to remain higher than normal across England this winter, according to the latest surveillance data. Recent findings from the Royal College of General Practitioners’ Research and Surveillance Centre indicate that scabies has been spreading more widely than expected over the past few months, with infections steadily increasing through autumn and winter.
Overall, reported cases have stayed above the usual five-year average, with the sharpest rise recorded during the final four months of last year, particularly across northern regions of the country. With scabies infections continuing to climb, concerns are growing around which treatments are safe to use, especially when it comes to children.
What Is Scabies?
Scabies is caused by a microscopic parasite known as Sarcoptes scabiei. This mite burrows into the top layer of the skin to lay its eggs, triggering severe itching and a red, spotty rash that often becomes more intense at night. Although the mites are too small to be seen easily, measuring less than half a millimetre, the body reacts to their saliva, eggs, and waste, leading to an allergic response.
Scabies spreads through prolonged skin-to-skin contact and can affect people of all ages. According to the NHS, it is most commonly transmitted through close household contact, including between partners, family members, people living together, and during sexual activity.
How Is Scabies Spreading In The UK?
UK Health Security Agency surveillance data shows that scabies cases reported through sexual health services remained relatively stable before the COVID-19 pandemic, but numbers began rising sharply from 2022 onwards. Diagnoses increased from 3,393 cases in 2023 to 4,872 cases in 2024, marking a 44 per cent rise.
- London accounted for roughly one-third of all cases recorded in 2024.
- The steepest percentage increase was seen in the North East, where reported cases nearly doubled.
- Young adults aged 20 to 24 made up 41 per cent of diagnoses, while those aged 25 to 34 accounted for 31 per cent.
Scabies UK: What's Behind The Surge In Cases?
Both the UKHSA and the British Association for Sexual Health and HIV (BASHH) suggest several reasons could be driving the surge:
- Increased social interaction and physical contact following the pandemic, after years of reduced mixing.
- Greater awareness of scabies and more testing taking place at sexual health clinics.
- Overcrowded housing and the ongoing cost of living crisis, which may delay access to prompt treatment.
Experts also caution that the actual number of cases is likely much higher, as the available data only reflects diagnoses made in sexual health settings.
Scabies UK: Can Ivermectin Treat Scabies In Children Safely?
Ivermectin is an oral antiparasitic medicine used to treat scabies by paralysing the mites. It offers a systemic alternative to topical creams and is often considered in cases that are widespread, severe, or involve institutional outbreaks. Because the drug does not kill scabies eggs, a second dose is usually required after seven to fourteen days to target newly hatched mites.
According to the Centres for Disease Control and Prevention, ivermectin is generally well tolerated, improves treatment compliance compared to creams, and has been widely used in mass drug administration programmes, though repeat dosing is important due to its limited effect on mite eggs.
Despite its broad use in programmes targeting conditions such as river blindness, intestinal worms, and scabies, ivermectin has traditionally not been recommended for children weighing under 15 kilograms, largely due to limited safety data. However, researchers revisited this concern following a systematic review and meta-analysis that suggested the drug could be safe even in children weighing as little as 11 pounds.
In a double-blind clinical trial, researchers assessed the safety, effectiveness, and pharmacokinetics of ivermectin in young children with scabies. A total of 240 children weighing between 11 pounds and under 33 pounds in The Gambia, Kenya, and Brazil were randomly assigned to receive ivermectin at doses of 200, 400, or 800 micrograms per kilogram alongside a placebo cream, or placebo tablets alongside permethrin cream. Blood samples were collected on days 0, 3, 7, 10, and 14 to monitor biochemical markers, drug levels, and blood health.
Ivermectin: Only One Serious Adverse Event
The findings showed that ivermectin was effective in treating scabies, with just one serious adverse event reported. This involved a temporary increase in liver enzymes, which returned to normal levels within 32 days. All other side effects possibly linked to the treatment were mild, resolved on their own, and were similar to those seen in children weighing more than 33 pounds.
“Outcomes from the Ivermectin Safety in Small Children trial will hopefully provide greater reassurance that ivermectin can be safely used in children weighing less than 15 kilograms,” said lead study author Kevin Kobylinski, PhD, an honorary visiting research fellow at the University of Oxford with the Mahidol Oxford Tropical Medicine Research Unit in Bangkok, in an ASTMH press release.
© 2024 Bennett, Coleman & Company Limited

