- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
World Organ Transplant Day: From 3D Printing To Lab-Grown Organs, Transplant Breakthroughs Are Here
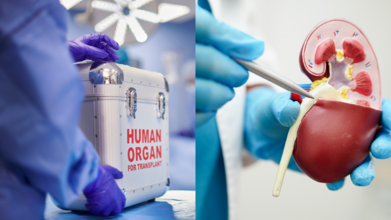
On World Organ Transplant Day, we usually hear about the urgent need for more donors, the lifesaving power of a transplant, and how one person’s decision can save up to eight lives. That is all still true and still critical but here is the twist: while the waiting lists grow, so do the technologies that might one day make them shorter or even unnecessary.
The future of organ transplantation is not just beating in donor hearts anymore; it is also whirring in lab incubators, spinning in magnetic rotors, and taking shape layer by layer on 3D bioprinters.
Despite decades of successful surgeries, the biggest roadblock in transplantation remains supply. Dr Bipin Chevale, CEO of Gleneagles Hospital Mumbai, explains, “There is still a persistent disparity between organ supply and demand. In India, thousands remain on waiting lists, and many lose their lives before a suitable organ becomes available.”
The reasons are a blend of low awareness, cultural taboos, and plain logistical hurdles. In 2023–24, nearly 50,000 Indians were waiting for organ replacement, according to the National Organ and Tissue Transplant Organisation (NOTTO). Globally, the US alone has more than 100,000 patients on transplant lists, with 13 lives lost every day while waiting.
Medical science, however, has been busy building backup plans. From 3D printing body parts to developing fully artificial organs, scientists are inching closer to a future where “no donor” does not mean “no hope”.
The Rise of 3D Bioprinting
Specialised 3D bioprinters can lay down living cells in precise patterns to create tissue that looks and behaves like the real thing.
Dr Varun Mittal, Head of Kidney Transplant at Artemis Hospitals, says researchers have “made great strides in printing living tissues and complicated networks of blood vessels”, something previously thought impossible. Techniques like Co-SWIFT create branching vessels inside heart tissue, while 3D ice printing uses water and gelatine to make smooth vessel templates.
While we are not yet popping out fully functional hearts or kidneys from printers for surgical use, these technologies are already valuable for training surgeons, testing drugs, and inching toward patient-specific implants. The idea is to design an organ to match a patient’s exact size, shape, and immune profile, dramatically lowering the risk of rejection.
Artificial Organs: Machines That Act Human
If printing an organ from scratch is the long game, artificial organs are the fast-forward button. These mechanical or bioengineered devices can take over the job of a failing organ, sometimes temporarily, sometimes for months or years.
One striking example is the BiVACOR artificial heart. It does not beat; it spins. A magnetic rotor pumps blood continuously, acting as a bridge until a donor heart is found. Dr Mittal points out that some patients have survived for months with the device, staying mobile and alert while awaiting surgery.
Similarly, researchers are developing implantable bioartificial kidneys that could filter blood and house living kidney cells without the need for dialysis or lifelong immunosuppressants. Wearable dialysis units are also in the works, aimed at freeing patients from hours tethered to clinic machines.
The Lung and Liver Challenge
Some of the boldest experiments are happening with lungs and livers, two of the trickiest organs to replace due to their complexity.
Dr Yasir Rizvi, Director of Nephrology and Kidney Transplant at Dharamshila Narayana Superspeciality Hospital, points to a landmark in lung research: a 3D-printed human-scale scaffold containing about 4,000 km of capillaries across 44 trillion voxels. In animal studies, it has already exchanged gases like a natural lung.
For the liver, bioprinting and bioengineering efforts aim to create functional tissue that can sustain patients until a full transplant is possible or even act as a permanent fix in the future.
The Benefits Are Already Here
We may still be a few years from printing a fully functional, transplant-ready heart, but artificial organ technology is already improving lives. Pacemakers, cochlear implants, and ventricular assist devices, these are all proof that machinery and biology can coexist in the human body.
Artificial organs have the potential to:
- Reduce rejection by using a patient’s own cells
- Cut waiting times dramatically
- Lower long-term medical costs by reducing hospital stays
- Give access to treatment in regions where donor organs are scarce
As Dr Chevale says, these breakthroughs are only half the story. “Their success will also depend on increasing awareness about organ donation, busting myths, and encouraging more people to pledge their organs.”
The Ethical Road Ahead
Of course, the march toward lab-grown and artificial organs comes with big ethical questions. Who gets them first? Will they be affordable or only for the wealthy? How do we ensure safety in devices meant to live inside fragile bodies?
Dr Rizvi believes that with “careful regulation, transparent trials and patient-centred design, these innovations can turn prototypes into standard care”. In India, collaborations between AIIMS, IITs, and bio-technical start-ups are already laying the groundwork, with the hope of producing affordable devices for both domestic and global use within a decade.
A Future Worth Donating To
Even if the day comes when a printer can make you a brand-new kidney, organ donation will still matter. Research organs, temporary implants, and hybrid solutions will always benefit from donated tissue to validate safety and function.
The future of transplantation is no longer just a race against the clock for a donor organ, it is also a race to develop, print, and perfect replacements that can save lives anywhere, anytime.
German Study Shows Squirrels May Be Harboring Mpox Virus
Credit: Canva
Squirrels could be natural hosts of the mpox virus (MPXV) -- that causes monkeypox disease -- according to a recent study by German researchers.
The team from the Helmholtz Institute for One Health (HIOH) identified the fire-footed rope squirrel (Funisciurus pyrropus) as a likely natural reservoir of the MPXV.
The study published in the journal Nature revealed that sooty mangabeys – a primate found in West Africa -- can contract mpox by eating infected squirrels. The disease may present mild lesions, but it can also cause more severe skin lesions or even be fatal.
"Identifying the animal sources of the virus and the exposure routes that lead to inter-species transmission are key steps towards understanding spillover mechanisms and developing effective prevention measures to mitigate the risk of transmission to humans," said Livia V. Patrono, one of the senior authors at HIOH.
Squirrels Suspected MPXV Hosts
While squirrels have long been suspected as potential reservoirs for MPXV, their role was confirmed after an investigation of an mpox outbreak among wild sooty mangabeys (Cercocebus atys) in Côte d'Ivoire.
During the outbreak, reported in early 2023, nearly one-third of the primates showed clinical signs of disease, and four infants died.
The team conducted viral genome sequencing and found that the infected monkeys carried a virus that was nearly identical to an MPXV strain identified in a fire-footed rope squirrel found dead 12 weeks earlier nearby.
Further, the team analyzed fecal samples from the mangabeys. A sample collected eight weeks before the outbreak's onset contained DNA from both the virus and the rope squirrel. This provided strong evidence of interspecies transmission at that moment.
Sooty mangabeys have been previously observed catching and eating fire-footed rope squirrels, which provide a direct route for the transmission of viruses.
Mpox Continues To Spread Globally
Although mpox is no longer a public health emergency, outbreaks of clade I and clade II strains of the mpox virus are continuing in many countries around the world, especially in Africa.
Last week, Madagascar announced the country's first death from mpox, a 3-year-old girl from the island nation’s eastern city of Toamasina.
The WHO has also confirmed that two cases of the recombinant strain – combining genomic elements of clades Ib and IIb of the monkeypox virus (MPXV) – have been identified to date: one in the United Kingdom and one in India.
Mpox is an infectious disease caused by the monkeypox virus (MPXV), part of the Orthopoxvirus genus, which also includes the virus that causes smallpox.
It spreads through close physical contact, including sexual contact, and in some cases through contaminated materials or respiratory droplets.
Symptoms typically include fever, swollen lymph nodes, rash, and/or lesions.
The global health body has also urged all countries to “remain alert to the possibility of MPXV genetic recombination.” It has also urged for continued epidemiological surveillance, sequencing, vaccination of at-risk groups, and infection prevention and control measures.
This AI Tool Predicts Women’s Breast Cancer Risk Up to Four Years
Credit: Canva
An international group of scientists has created an artificial intelligence tool that can estimate a woman’s likelihood of developing breast cancer within the next four years.
The AI tool, known as the BRAIx risk score, analyzes mammogram images to generate an individualized risk assessment and flag women who may face a higher chance of developing the disease.
It may not only show the current risk but also predict the future risk, enabling early detection and treatments for a better outcome.
According to the findings published in The Lancet Digital Health journal, nearly one in 10 women ranked in the top 2 percent of risk by the AI tool were diagnosed with breast cancer within four years. This was despite previously receiving a clear screening result.
“These risk scores enable future development of personalized screening pathways to transform population breast cancer screening and save lives,” said corresponding author Helen M. L. Frazer of the University of Melbourne.
Frazer noted that identifying women who appear cancer-free but carry very high risk -- comparable to those with inherited BRCA1 or BRCA2 mutations -- will unravel both hereditary and non-hereditary causes of breast cancer.
From one-size-fits-all screening to personalization
Breast cancer screening programs have significantly lowered mortality rates -- by roughly 40-50 percent among women aged 50 to 74. However, most screening systems still apply the same approach to all women, regardless of individual risk.
Traditional screening tools use genetics, breast density, and questionnaires to estimate breast cancer risk. On the other hand, new AI-based screening tools, such as BRAIx personalizes screening by gathering information already present in breast scan images to better identify who is at higher risk.
“Our results show that conventional mammographic density is a far weaker predictor of breast cancer risk than the BRAIx risk score, even for interval cancers,” the researchers said in the paper. Interval cancers are aggressive tumors diagnosed after a negative mammogram.
The BRAIx Tool
The BRAIx risk score was developed using mammograms from nearly 400,000 women. To prove its efficacy, the AI tool was tested on data from almost 96,000 women from Australia and then confirmed in an independent Swedish population of over 4,500 women.
The findings showed that:
- The BRAIx risk score estimated breast cancer risk more accurately than the traditional risk factors, such as breast density, country of birth, and even family history.
- For the top 2 percent of women with the highest BRAIx risk score, the probability of a cancer diagnosis within 4 years was 9.7 percent -- a risk level exceeding that typically seen in women with inherited BRCA1 or BRCA2 mutations.
The BRAIx risk score can:
- Make breast screening more personalised,
- Improve early cancer detection,
- Reduce false alarms,
- Save lives without increasing costs
Global Breast Cancer Burden
Breast cancer continues to be the most common cancer among women worldwide.
A recent study published in The Lancet Oncology journal predicted that the number of new cases of the deadly disease will reach more than 3.5 million globally in 2050 -- rising by a third from 2.3 million in 2023.
Annual deaths from the disease will also rise by 44 percent -- from around 764,000 to 1.4 million.
However, not smoking, getting sufficient physical activity, lowering red meat consumption, and having a healthy weight can help prevent over a quarter of healthy years lost to illness and premature death from breast cancer.
COVID Survivors At Nearly Fivefold Risk Of Kidney Failure: Study
Credit: Canva
People who survived a COVID-19 infection can be at significant risk for kidney disease, acute kidney injury, and chronic kidney disease. compared to individuals who were not infected, according to a study.
The study, published online in the journal Communications Medicine, revealed that COVID patients have
- a 2.3-times higher risk of acute kidney injury
- a 1.4-times higher risk of chronic kidney disease
- a 4.7 times higher risk of kidney failure
“While we’re in the post-pandemic era, this shows that COVID-19 history is an important variable when considering the long-term impact of the infection on kidney function and disease,” said first author Yue Zhang, who was at Pennsylvania State University, US, while conducting the study. Zhang is currently a postdoctoral scholar at Johns Hopkins Bloomberg School of Public Health.
How Was The Study Conducted?
For the study, data on over 3 million working-age adults in the United States were analyzed.
The team compared the effect of influenza, another common viral infection that affects kidney health, and people with a history of COVID infection on kidney infections.
Using a machine learning model, the individuals were followed between 180 and 540 days for the emergence of new acute or sudden kidney disease.
The results showed that:
- Both COVID and the flu can worsen kidney health
- Flu caused a mild and temporary effect
- COVID increased the risk of acute kidney injury for a longer duration
- COVID survivors developed kidney disease within a few hours to a few days
- COVID patients had a longer-term chronic and end-stage kidney disease.
How COVID Worsens Kidneys Health
The Penn State researchers explained that kidney cells express high levels of the primary protein receptors that SARS-CoV-2 uses to enter and infect cells. Kidney cells also produce specialized enzymes that help viruses enter cells.
According to Kidney Health Australia, an acute COVID infection can impact the kidneys with fevers and respiratory symptoms, and/or worsening blood sugar control.
The US National Institutes of Health stated that renal dysfunction is an increasing clinical indicator of COVID propagation.
Citing several studies, the NIH said that the most common clinical manifestation is proteinuria -- found in more than half of the COVID patients. In addition, hematuria, elevated blood urea nitrogen, and elevated serum creatinine are other common features in Covid survivors with poor kidney health.
Nasr Ghahramani, Professor of Medicine at Penn State College of Medicine, stressed the need for COVID survivors, especially those with diabetes and high blood pressure, to take "more frequent and more prolonged monitoring of their kidney function" to enable early detection and better outcomes.
© 2024 Bennett, Coleman & Company Limited

