- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
'Biased' Danish Parenting Test Has Separated Babies From Their Mothers; Parents Are Now Fighting Back

Credits: Canva, iStock
Parenting test that ensures that individuals are ready to take responsibility of a child sounds good, until its turns into a trauma of lifetime, where not scoring enough or failing that test leads to separation of the child from his parents. So is the case of many parents in Denmark, who have to undergo this parental scrutiny. Keira, being one of them, had just given birth to her daughter last November, but she knew that she only had two hours before her newborn would be taken into care.
She tells BBC, “Right when she came out, I started counting the minutes,” she recalls, adding that she couldn’t stop looking at the clock to see how long they had together. When the moment came, Keira says she sobbed uncontrollably, whispering “sorry” to her baby. “It felt like a part of my soul died”
She is a Greenlandic parent, among many, living in Denmark, who are now fighting to get their children back after they were removed by social services. In many of these cases, authorities have relied on the competency assessments, known as FKUs. This test determines where parents are fit to raise their children.
What Is the Danish Parenting Competency Test?
The FKU, or “parenting competency test,” was a psychometric assessment used by Danish child protection authorities to evaluate whether parents were fit to raise their children. In theory, the test aimed to protect children by identifying families in crisis or parents unable to provide adequate care. In practice, however, it became a tool of controversy—especially when applied to Greenlandic families.
The test assessed parents in a series of areas, such as their responses to imagined scenarios, self-concept, physical and mental well-being, outlook on life, and plans for the future. Most importantly, it was based on Western conception of good parenthood and delivered in Danish, with minimal attention to Greenlandic language, customs, or kinship systems. This incompatibility resulted in regular misinterpretations of the capacity of Greenlandic parents and sometimes led to children being taken from their parents.
Greenlandic children have traditionally been disproportionately represented in Denmark's child welfare system. Approximately 7% of Greenland-born children and 5% of children who have at least one Greenlandic parent are placed out-of-home. That's in sharp contrast to only 1% of the general Danish child population.
"Not Civilized Enough To Act Like A Human Being"
These assessments, which were banned for use on Greenlandic families in May after decades of criticism, remain legal for Danish families. They often take months and involve cognitive exercises, personality testing, interviews, memory challenges, and general knowledge questions.
According to Keira, some of the questions she faced felt irrelevant and culturally disconnected. “Who is Mother Teresa?” and “How long does it take for the sun’s rays to reach the Earth?” were among the things she was asked. She also recalls being made to play with a doll and criticized for not making enough eye contact. Keira alleges a psychologist even told her the test was meant to determine “if you are civilized enough, if you can act like a human being”.
While defenders of FKUs say they offer an objective framework, critics argue the tests cannot reliably predict parenting ability and are designed around Danish cultural norms. They are administered in Danish, not Kalaallisut, Greenland’s primary language, something many say leads to miscommunication and unfair evaluations.
A Disproportionate Impact
Greenlanders are Danish citizens, and thousands live on the mainland for work, education, and healthcare. Yet studies highlight stark disparities. Greenlandic parents in Denmark are 5.6 times more likely to have their children taken into care compared to Danish parents, according to the Danish Centre for Social Research.
The Danish government announced plans to review around 300 cases involving Greenlandic children, including those shaped by FKU results. But as of October, the BBC found only 10 cases involving the tests had been reviewed—and not a single child had been returned.
Keira’s own assessment concluded she lacked “sufficient parental competencies to care for the newborn independently”. Despite the ruling, she keeps cots in her home, along with baby clothes and framed photos of Zammi. She visits her daughter once a week, bringing flowers or traditional Greenlandic dishes—“just so a little part of her culture can be with her,” she says.
No Chance Of Reviewing The Test
Unlike Keira, some parents will never see their cases reconsidered. Johanne and Ulrik, whose son was adopted in 2020, have been told their case will not be reopened. Johanne had undergone an FKU in 2019 that labelled her “narcissistic” and described her as having “mental retardation,” based on criteria then used by the WHO claims she rejects.
Their baby was also meant to be taken immediately after birth, but because he arrived prematurely on Boxing Day while social workers were on holiday, the couple spent 17 days with him. “It was the happiest time of my life as a father,” Ulrik says, describing those days of feeding, changing nappies, and helping Johanne pump milk.
When authorities eventually arrived, two social workers and two police officers, the couple begged them not to take their son. Johanne asked to breastfeed him one last time. Ulrik remembers dressing his child before handing him to foster parents: “I felt the most horrific heartbreak”.
The couple no longer have access to their son but hope to take their case to the European Court of Human Rights. Denmark’s social affairs minister told the BBC the government will not revisit adoption cases because each child is now with a “loving and caring family.”
Experts disagree sharply on the validity of FKUs. Former test administrator Isak Nellemann says the assessments “are very important, about the most important thing,” claiming that when results are poor, “in about 90% [of cases] they will lose their children”. He also argues that some components lack scientific validity.
However, Turi Frederiksen, a senior psychologist, told BBC that while imperfect, the tests remain “valuable, extensive psychological tools” and denies they are biased against Greenlanders.
Rare Union That Is The Only Ray Of Hope Of Childless Parents
Among the few who have successfully regained custody is Pilinguaq, whose daughter was returned more than four years after being placed into care. The mother still struggles to rebuild trust; even briefly leaving the room can cause her daughter to panic. “If I go to the bathroom and close the door, she will have a panic attack,” she told BBC.
Her two older children are expected to return home soon as well, decisions made by local authorities, not the national review.
Keira continues to prepare for Zammi’s first birthday by building a traditional Greenlandic sleigh decorated with a polar bear. Earlier this month she was informed that her daughter will not be coming home yet—but she refuses to give up.
“I will not stop fighting for my children,” she says. “If I don’t finish this fight, it will be my children’s fight in the future”.
Maternal Vaccination During Pregnancy Can Prevent COVID-related Hospitalization In Babies: Study

Credit: iStock/Canva
Maternal vaccination with the COVID-19 vaccine during pregnancy can be effective against severe disease and hospitalization from the SARS-CoV-2 virus in babies, according to a large study.
The study, published in the journal Pediatrics, revealed that COVID vaccination during pregnancy can protect the children against hospitalization for COVID during the first six months of life.
Amid continuing COVID cases, babies under six months old continue to have one of the highest rates of hospitalization — one in five — due to the COVID virus in the US, as per a 2024 study.
As currently no vaccines against COVID are available for neonates and babies, the American College of Obstetricians and Gynecologists (ACOG) recommends maternal vaccination during pregnancy.
Maternal COVID Vaccination Prevented Other Infections
The retrospective study included 146,031 infants born in Norway between March 2021 and December 2023. Of these, 37, 013 (25 percent) were exposed to COVID-19 vaccination in utero.
The findings showed that babies exposed to the vaccine before birth were no more likely to visit the hospital for overall infections (of any kind) than those whose mothers did not get vaccinated in pregnancy.
However, infants whose mothers were vaccinated were about half as likely to visit the hospital specifically for COVID in their first two months of life compared to babies not exposed to the vaccine in utero.
Among 3 to 5-month-old babies, the risk of a hospital visit for COVID was 24 percent lower in those exposed to the vaccine, but the vaccine's protection against COVID wore off by the time infants were older than 6 months.
Importantly, the mothers' vaccine also prevented the risk of other infections in children.
"There is often an increased risk for a subsequent infection after a viral infection, such as an increased risk of pneumonia after influenza infection, so we wanted to study whether protection against COVID-19 could influence the risk of other infections as well," said lead author Dr. Helena Niemi Eide, from the University of Oslo in Norway, the NPR reported.
"But we found that COVID vaccination in pregnancy protected the infant against COVID and had no apparent effect on other infections," Eide added.
Maternal Vaccine Recommendation in the US
Last week, the American College of Obstetricians and Gynecologists reiterated its recommendation for COVID vaccination during pregnancy.
Despite changes in federal vaccine recommendations due to the US Health Secretary Robert F. Kennedy Jr.’s anti-vaccine stance, the ACOG urged COVID vaccination for
- people who are pregnant,
- recently pregnant,
- considering pregnancy,
- lactating.
Also read: US Judge Blocks RFK Jr.’s Vaccine Schedule, Says Government Ignored Science
"Accumulated safety data from millions of administered doses show no increased risk of adverse maternal, fetal, or neonatal outcomes associated with COVID-19 vaccination in pregnancy,” the ACOG said.
'Husband Stitch': A Medical Necessity Or Just A Tool To Objectify Women's Bodies?
Credits: AI-generated and iStock
When 36-year-old mom Angela Sanford, from Fort Mill, SC, went for an appointment for a Pap smear five years after she had her first child in 2008, her nurse midwife, who she has never seen before asked her a question she did not expect. "Who stitched you up after your first birth?"
Speaking to Healthline, Sanford shared that she just started crying when the nurse said, "This is not right." Sanford said that this was the first time she ever heard the term 'husband stitch'. Sanford was told that her stich was "too tight" by the hospitalist who managed her after her first delivery.
Also Read: US CDC Warns Of New Immune-Evasive COVID Variant In 23 Countries
“He gave you what some people call a husband stitch,” Sanford recalled the midwife telling her.
“I couldn’t connect in my mind why it would be called that. My midwife said, ‘They think that some men find it more pleasurable,’” she recalled. “My husband has been worried about me and fearful of hurting me. He would never have asked for this.”
A 'Husband Stich' - What Is It?
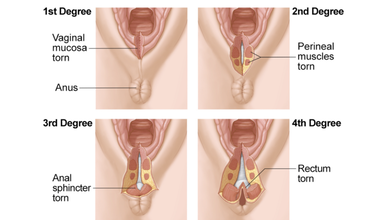
During vaginal delivery, a woman undergoes perineal tears or vaginal lacerations which means tears between the vaginal opening and anus. This causes pain, and requires stitches for grades two and higher. It also takes 4 to 6 weeks to heal. Women can experience from first to fourth degree tears.
Sometimes, a surgical incision is made in the perineum during childbirth to enlarge the vaginal opening, this is called an episiotomy. However, it is not medically necessary or a routine procedure, unless it is a case of emergency.
Stiches are required in such cases that dissolves on its own. However, a 'husband stitch', also known as "daddy stitch" is an unethical practice where an extra stitch is given during the repair process that 'tightens the vagina' to increase sexual pleasure for a male partner. While it is considered a medical malpractice, it is still done to women after vaginal delivery.
Many women face difficulty after the extra stich is given to them. In Sanford's case, she felt "excruciating" pain during sex afterwards.
Read: Romanticization And The Silent Dismissal Of Women’s Pain
When Objectifying Women's Bodies Is Made A Medical Practice
Stephanie Tillman, CNM, a certified nurse midwife at the University of Illinois at Chicago and blogger at The Feminist Midwife told Healthline: “The fact that there is even a practice called the husband stitch is a perfect example of the intersection of the objectification of women’s bodies and healthcare. As much as we try to remove the sexualization of women from appropriate obstetric care, of course the patriarchy is going to find its way in there."
Harkins, 37, said that she "kind of" laughed it off when an "old, crusty Army doctor" overstitched her so she could give her husband more pleasure. In many cases, doctors do it as a routine practice without even being told by anyone. “I couldn’t even process [it], but I kind of laughed, like what else do you do when someone says that? I had just had a baby. I didn’t think much about it because the whole birth experience was so traumatizing, but now that I think about it differently, the implications of that are just crazy.”
Episiotomy Is An Excuse For 'Husband Stitch'
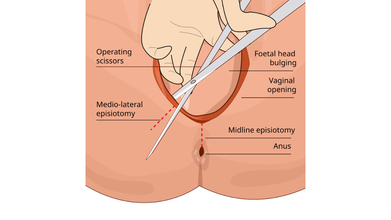
Dr Robert Barbieri, chair of obstetrics and gynecology and reproductive biology at Brigham and Women’s Hospital in Boston, told the Huffington Post that doctors were taught in the 50s and 60s that "routine episiotomy was good for women".
“What they thought is that if they did a routine episiotomy, they’d have a chance to repair it and that during the repair, they could actually create a better perineum than if they hadn’t done it. The idea [was] that we could ‘tighten things up,’” explains doctor.
However, a 2005 systematic review in the Journal of the American Medical Association found no benefit to routine episiotomy use. A 2017 Cochrane review “could not identify any benefits of routine episiotomy for the baby or the mother.” In 2016, the American College of Obstetricians and Gynecologists (ACOG) recommended that clinicians “prevent and manage” delivery lacerations through strategies like massage and warm compresses rather than making cuts on the perineum. Yet, this practice still continues inside the labor rooms.
Your Kids’ Fast-fashion Clothing May Be Laced With High Levels of Toxic Lead

Credit: iStock
While you may be buying fast-fashion clothes that are easy on your pocket and also give your children trendy looks, a new study highlights the risk of being laced with a highly toxic ingredient: lead.
The preliminary research, based on lab tests of several shirts from different retailers in the US, found that all the samples exceeded the country’s federal regulatory lead limits.
The US Consumer Product Safety Commission currently has a 100 parts per million (ppm) lead limit for children's products like toys and clothing.
"I started to see many articles about lead in clothing from fast fashion, and I realized not too many parents knew about the issue," said Kamila Deavers, principal investigator of the study, at Marian University in the US.
Deavers began the study after her young daughter’s lab reports showed elevated levels of lead in her blood from toy coatings.
How was study conducted?
The team tested 11 shirts that spanned the rainbow—red, pink, orange, yellow, gray, and blue. All brightly colored fabrics, particularly reds and yellows, showed higher levels of lead compared to more muted tones.
"We saw that the shirts we tested were all over the allowed limit for lead of 100 ppm," said Priscila Espinoza, from Marina.
The researchers explained that some manufacturers use lead (II) acetate as an inexpensive way to help dyes stick to the materials and produce bright, long-lasting color.
Children At Greater Risk
The researchers found the risk is particularly higher among younger kids as they tend to playfully suck or chew their clothes during play.
"Even briefly chewing these fabrics could expose children to dangerous lead levels,” they found in the study, to be presented at the forthcoming meeting of the American Chemical Society.
According to the US Environmental Protection Agency (EPA), lead exposure can lead to behavior problems, brain and central nervous system damage, as well as other negative health effects in children.
The agency considers children under six years old to be most at risk from exposure. Even low levels of lead in the blood of children can result in:
- Behavior and learning problems
- Lower IQ and Hyperactivity
- Slowed growth
- Hearing Problems
- Anemia
The researchers also pointed out safer alternatives to lead-based dyeing agents that already exist. These include natural and less harmful substances such as:
- Plant-based tannins (e.g., oak bark, pomegranate peel)
- Rosemary
- Alum.
© 2024 Bennett, Coleman & Company Limited

