- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Children Born To First Cousins Are At A Higher Risk Of Genetic Disorder

Credits: Canva
Children who are born to first cousins are usually at a higher risk of developing certain genetic disorders and health complications. This happens due to the increase probability of inheriting recessive genes from both the parents. While cousin marriages have been practiced in various cultures and historical periods, modern medical research has highlighted the potential risk that can be associated with consanguinity. This happens when close relatives have children together.
What Are The Genetic Risks
The primary concern with cousin marriage is the higher likelihood of recessive genetic disorder. Every person carries some recessive genes that do not usually manifest because they are paired with dominant and healthy genes from the other parent. However, when both the parents share the same ancestry, it gives the baby a greater chance of carrying the same recessive genes. This also increases the probability that their child will inherit two copies of the faulty gene, which could lead to a genetic disorder.
Some of the most well-documented recessive disorders associated with cousin marriages include:
Cystic Fibrosis: A condition that leads to severe lung infections and digestive issues.
Sickle Cell Disease: A blood disorder that affects oxygen transport in the body, causing pain and organ damage.
Thalassemia: A disorder leading to anemia and requiring regular blood transfusions.
Tay-Sachs Disease: A fatal neurological disorder affecting infants, common in certain populations that practice endogamy.
Metabolic Disorders: Conditions affecting how the body processes food and nutrients, which can lead to severe developmental issues.
Findings from Medical Studies
Extensive research has been conducted to understand the health impacts of consanguineous marriages. One notable study, the Born in Bradford study, has followed thousands of children born in the UK city of Bradford, where first cousin marriage is relatively common. The study found that:
- Children of first cousins have double the risk of being born with a recessive genetic disorder compared to children of unrelated parents.
- They are more likely to experience speech and language developmental delays.
- They visit primary healthcare facilities more frequently, suggesting a higher prevalence of general health concerns.
- Infant mortality rates are significantly higher due to congenital disorders.
Beyond Genetic Disorders: Broader Health Concerns
While recessive genetic conditions are a major concern, other health issues have also been observed among children of first cousins:
Weakened Immune System: Some studies indicate that these children may have weaker immune responses, making them more susceptible to infections and chronic illnesses.
Neurological and Cognitive Impairments: Studies suggest a higher risk of intellectual disabilities and developmental delays.
Cardiac Issues: Congenital heart defects are more common in children of consanguineous parents.
Endogamy and Its Role in Health Risks
While first cousin marriage is a direct cause of increased genetic risks, researchers have also pointed out that endogamy—the practice of marrying within the same ethnic or cultural group—can have similar effects. Over generations, small gene pools lead to a higher concentration of harmful genetic mutations. This has been observed in various communities worldwide, including the Amish, French Canadians, and certain Jewish populations.
Addressing the Risks: Education and Genetic Counseling
Rather than outright bans, many experts advocate for genetic literacy and counseling. In communities where cousin marriage is prevalent, genetic counseling can help couples understand their risks and make informed decisions about family planning. Pre-marital and pre-conception genetic testing can identify potential recessive disorders, allowing couples to consider medical interventions or alternative reproductive options.
In countries like the UK, where cousin marriage remains legal, efforts have been made to improve awareness within affected communities. Initiatives such as:
- Genetic screening programs before marriage or pregnancy.
- Educational campaigns within high-risk communities to inform families about potential health risks.
- Expanded healthcare support for children born with genetic disorders.
The Ongoing Debate
While some European countries have chosen to ban cousin marriage, others argue that a more effective approach is increased awareness and medical intervention rather than legal restrictions. Critics of a ban highlight that forced restrictions may not prevent cousin marriages but could drive them underground, making access to genetic counseling more difficult.
The discussion around cousin marriage is complex, intertwining cultural traditions, ethical considerations, and public health concerns. While medical research underscores the risks, the key to addressing them lies in education, access to healthcare, and informed decision-making for prospective parents.
Maternal Vaccination During Pregnancy Can Prevent COVID-related Hospitalization In Babies: Study

Credit: iStock/Canva
Maternal vaccination with the COVID-19 vaccine during pregnancy can be effective against severe disease and hospitalization from the SARS-CoV-2 virus in babies, according to a large study.
The study, published in the journal Pediatrics, revealed that COVID vaccination during pregnancy can protect the children against hospitalization for COVID during the first six months of life.
Also Read: COVID-19 Cicada Variant: Will It Become The Dominant Strain In The US? Know All About The Virus
Amid continuing COVID cases, babies under six months old continue to have one of the highest rates of hospitalization — one in five — due to the COVID virus in the US, as per a 2024 study.
As currently no vaccines against COVID are available for neonates and babies, the American College of Obstetricians and Gynecologists (ACOG) recommends maternal vaccination during pregnancy.
Maternal COVID Vaccination Prevented Other Infections
The retrospective study included 146,031 infants born in Norway between March 2021 and December 2023. Of these, 37, 013 (25 percent) were exposed to COVID-19 vaccination in utero.
The findings showed that babies exposed to the vaccine before birth were no more likely to visit the hospital for overall infections (of any kind) than those whose mothers did not get vaccinated in pregnancy.
However, infants whose mothers were vaccinated were about half as likely to visit the hospital specifically for COVID in their first two months of life compared to babies not exposed to the vaccine in utero.
Also Read: Olivia Munn Opens Up About Detecting No-Symptom Breast Cancer With Lifetime Risk Assessment Test
Among 3 to 5-month-old babies, the risk of a hospital visit for COVID was 24 percent lower in those exposed to the vaccine, but the vaccine's protection against COVID wore off by the time infants were older than 6 months.
Importantly, the mothers' vaccine also prevented the risk of other infections in children.
"There is often an increased risk for a subsequent infection after a viral infection, such as an increased risk of pneumonia after influenza infection, so we wanted to study whether protection against COVID-19 could influence the risk of other infections as well," said lead author Dr. Helena Niemi Eide, from the University of Oslo in Norway, the NPR reported.
"But we found that COVID vaccination in pregnancy protected the infant against COVID and had no apparent effect on other infections," Eide added.
Maternal Vaccine Recommendation in the US
Last week, the American College of Obstetricians and Gynecologists reiterated its recommendation for COVID vaccination during pregnancy.
Despite changes in federal vaccine recommendations due to the US Health Secretary Robert F. Kennedy Jr.’s anti-vaccine stance, the ACOG urged COVID vaccination for
- people who are pregnant,
- recently pregnant,
- considering pregnancy,
- lactating.
Also read: Bipolar Disorder: How Early Detection Can Help Prevent Serious Complications
"Accumulated safety data from millions of administered doses show no increased risk of adverse maternal, fetal, or neonatal outcomes associated with COVID-19 vaccination in pregnancy,” the ACOG said.
'Husband Stitch': A Medical Necessity Or Just A Tool To Objectify Women's Bodies?
Credits: AI-generated and iStock
When 36-year-old mom Angela Sanford, from Fort Mill, SC, went for an appointment for a Pap smear five years after she had her first child in 2008, her nurse midwife, who she has never seen before asked her a question she did not expect. "Who stitched you up after your first birth?"
Speaking to Healthline, Sanford shared that she just started crying when the nurse said, "This is not right." Sanford said that this was the first time she ever heard the term 'husband stitch'. Sanford was told that her stich was "too tight" by the hospitalist who managed her after her first delivery.
Also Read: US CDC Warns Of New Immune-Evasive COVID Variant In 23 Countries
“He gave you what some people call a husband stitch,” Sanford recalled the midwife telling her.
“I couldn’t connect in my mind why it would be called that. My midwife said, ‘They think that some men find it more pleasurable,’” she recalled. “My husband has been worried about me and fearful of hurting me. He would never have asked for this.”
A 'Husband Stich' - What Is It?
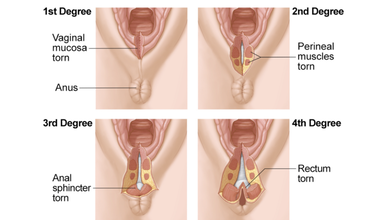
During vaginal delivery, a woman undergoes perineal tears or vaginal lacerations which means tears between the vaginal opening and anus. This causes pain, and requires stitches for grades two and higher. It also takes 4 to 6 weeks to heal. Women can experience from first to fourth degree tears.
Sometimes, a surgical incision is made in the perineum during childbirth to enlarge the vaginal opening, this is called an episiotomy. However, it is not medically necessary or a routine procedure, unless it is a case of emergency.
Stiches are required in such cases that dissolves on its own. However, a 'husband stitch', also known as "daddy stitch" is an unethical practice where an extra stitch is given during the repair process that 'tightens the vagina' to increase sexual pleasure for a male partner. While it is considered a medical malpractice, it is still done to women after vaginal delivery.
Many women face difficulty after the extra stich is given to them. In Sanford's case, she felt "excruciating" pain during sex afterwards.
Read: Romanticization And The Silent Dismissal Of Women’s Pain
When Objectifying Women's Bodies Is Made A Medical Practice
Stephanie Tillman, CNM, a certified nurse midwife at the University of Illinois at Chicago and blogger at The Feminist Midwife told Healthline: “The fact that there is even a practice called the husband stitch is a perfect example of the intersection of the objectification of women’s bodies and healthcare. As much as we try to remove the sexualization of women from appropriate obstetric care, of course the patriarchy is going to find its way in there."
Harkins, 37, said that she "kind of" laughed it off when an "old, crusty Army doctor" overstitched her so she could give her husband more pleasure. In many cases, doctors do it as a routine practice without even being told by anyone. “I couldn’t even process [it], but I kind of laughed, like what else do you do when someone says that? I had just had a baby. I didn’t think much about it because the whole birth experience was so traumatizing, but now that I think about it differently, the implications of that are just crazy.”
Episiotomy Is An Excuse For 'Husband Stitch'
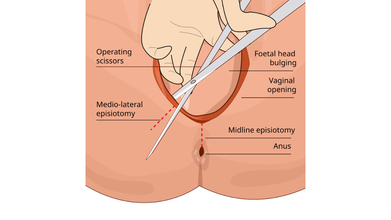
Dr Robert Barbieri, chair of obstetrics and gynecology and reproductive biology at Brigham and Women’s Hospital in Boston, told the Huffington Post that doctors were taught in the 50s and 60s that "routine episiotomy was good for women".
“What they thought is that if they did a routine episiotomy, they’d have a chance to repair it and that during the repair, they could actually create a better perineum than if they hadn’t done it. The idea [was] that we could ‘tighten things up,’” explains doctor.
However, a 2005 systematic review in the Journal of the American Medical Association found no benefit to routine episiotomy use. A 2017 Cochrane review “could not identify any benefits of routine episiotomy for the baby or the mother.” In 2016, the American College of Obstetricians and Gynecologists (ACOG) recommended that clinicians “prevent and manage” delivery lacerations through strategies like massage and warm compresses rather than making cuts on the perineum. Yet, this practice still continues inside the labor rooms.
© 2024 Bennett, Coleman & Company Limited

