- Health Conditions A-Z
- Health & Wellness
- Nutrition
- Fitness
- Health News
- Ayurveda
- Videos
- Medicine A-Z
- Parenting
Peripartum Cardiomyopathy: What Kills Women During Childbirth?
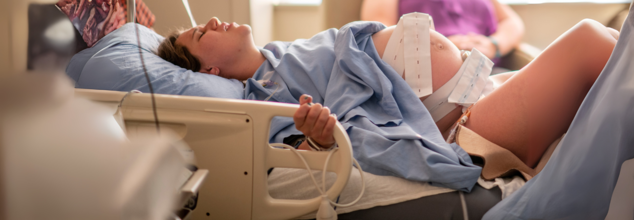
Credits: Canva
Childbirth is usually considered a moment of happiness and beginnings, but for numerous women worldwide, it could become a life-or-death situation. Though excessive bleeding, infection, and hypertensive complications are well-known reasons for maternal mortality, an underemphasized yet life-threatening condition—peripartum cardiomyopathy (PPCM)—is slowly emerging as a silent killer. This unusual but dangerous manifestation of heart failure occurs in women late in pregnancy or shortly after delivery, frequently with symptoms that are indistinguishable from usual pregnancy discomforts.
According to the most recent UN global estimates, 303,000 women annually lose their lives as a result of complications in pregnancy or childbirth—an average of 830 women per day, or approximately one every two minutes. Most of these deaths could be averted with proper and timely medical attention. But extremes of inequality exist: two-thirds of maternal deaths happen in sub-Saharan Africa, with India and Nigeria alone contributing one-third of the world total.
Although the number of deaths worldwide has decreased by 44% since 1990, from 532,000 to 303,000, the achievement has not been commensurate with the size of global commitments over decades to cut down these figures. Most of the deaths remain underreported, especially in areas with weak healthcare systems and inadequate data collection mechanisms.
What Is Peripartum Cardiomyopathy?
Peripartum cardiomyopathy is a form of heart failure that occurs in the final month of pregnancy or within five months after delivery. It compromises the function of the heart muscle, making it less efficient at circulating blood throughout the body. Clinically, it appears as heart failure with low ejection fraction (EF < 45%) without any other established cause. Although the specific etiology of PPCM is not known, risk factors are advanced maternal age, Afro-American heritage, pre-eclampsia, chronic hypertension, and multiparity.
Although PPCM is uncommon—affecting between 1 in 1,000 and 1 in 4,000 pregnancies in the United States—it's a significant health risk when it does occur. It has been found to be more common in the southern parts of the U.S., but worldwide estimates are uncertain due to under-reporting and under-diagnosis.
One of the most perilous features of PPCM is how readily it can be confused with normal pregnancy symptoms. Fatigue, shortness of breath, swelling in the feet and ankles, and mild chest pain are all normal pregnancy occurrences. But for women with PPCM, these symptoms can indicate a heart in distress. Severer forms cause difficulty in lying down due to breathing (orthopnea), night-time breathing distress (paroxysmal nocturnal dyspnea), palpitations of the heart, and even decreased blood pressure or cardiogenic shock.
"The PPCM clinical syndrome is easily likely to be mistaken for late-gestational complains," states Consultant – Gynecology Dr. Madhu Bindhu. "It usually brings delays in diagnosis, which, being critical at times, causes anxiety. Earlier recognition, notably via echocardiographic screening, is responsible for better outcome improvement."
How Is PPCM Diagnosed and Treated?
Diagnosis often starts with a 12-lead ECG and a chest X-ray, but the definitive test is a 2D echocardiogram, which can verify left ventricular dysfunction. In complicated cases, a cardiac MRI may be performed to exclude other structural or inflammatory causes of heart failure.
Treatment is with a typical heart failure regimen, adjusted for pregnancy or postpartum status. This can be diuretics to decrease fluid accumulation, beta-blockers to manage heart rate, and ACE inhibitors, utilized postpartum. Anticoagulants can be given to avoid blood clots, a frequent complication in PPCM.
A treatment that is under investigation and shows promise is Bromocriptine, a prolactin inhibitor with disease-modifying effects. In severely ill patients, more advanced treatments like ECMO (extracorporeal membrane oxygenation), intra-aortic balloon pumps, or LVADs (left ventricular assist devices) are options.
Pregnancy, Delivery, and the Cardiomyopathy Equation
For pregnant women diagnosed with PPCM, delivery plans need to be tailored. Vaginal delivery is favored for hemodynamically stable patients, states Dr. Bindhu. But those with critical cardiac decompensation are advised to have cesarean sections at any gestational age.
Significantly, a multidisciplinary approach by cardiologists, obstetricians, and intensive care specialists is vital. Pregnancy heart teams dedicated to caring for complex PPCM cases can make a life-changing difference and lower mortality risks.
Outcome in PPCM is variable. Many women recover if treated appropriately, but some might have chronic heart failure or potentially life-threatening complications. Poor prognostic indicators are an ejection fraction less than 30%, dilatation of the left ventricle, biventricular dysfunction, prolongation of the QT interval, and non-Caucasian ethnicity.
Public education, early diagnosis, and enhanced access to prenatal care are the pillars of preventing maternal mortality due to PPCM. In resource-poor countries, enhancing diagnostic capacity and educating clinicians to diagnose PPCM is crucial.
Peripartum cardiomyopathy is still one of the least talked-about but most perilous maternal medical conditions in the world. As we continue to aim to decrease maternal death rates, particularly in low-resource environments, it is important that PPCM be part of the discussion. Every pregnant woman should have the means and attention that can identify and treat the condition in time—so motherhood can start in hope, not heartbreak.
Dr Madhu Bindhu is a Consultant – Gynecology at Manipal Hospital, Vijayawada in India
The Working Mother’s Double Shift: Office Deadlines, Baby Duties and Endless Guilt | Women’s Day Special

Credit: Canva
Imagine standing at the starting line of a race, dressed properly with the best running shoes and ready to give your best. Yet, as the race begins, you notice that while half of the runners beside you have a clear path ahead, yours is filled with obstacles -- a dirty diaper, a crying baby, piles of laundry, a sink full of dishes, an empty fridge, cooking to be done, and countless other responsibilities.
If you pictured that correctly, you have just imagined the race of a man (with a clear road) and a woman’s race — more precisely, the race of a mother.
In 2019, the chairman of the Mahindra Group, Anand Mahindra, famously posted on the social media platform X, featuring the race of a working man and a woman, sparking a conversation on gender equality.
On International Women’s Day, women are given flowers, cake, or chocolates as a matter of appreciation for their seemingly multi-talented roles, but hardly does that go into consideration by families, partners, and workplaces.
Sanjana (name changed), a marketing professional from Bengaluru, was overjoyed as she held her first baby after a bout of four years of trying, several treatments, and constant pressure from family and society.
Speaking to HealthandMe, she said that the joy, however, was short-lived when she decided to get back to work.
“I had to figure out the support system -- what will I do, what will my husband do, and from what time to what time I need to keep a nanny. When I joined, I realized there was zero flexibility. I couldn’t leave work before completing a nine-hour shift and had to travel two hours back and forth. I was exhausted by the time I got back home, but nothing was ever ready for me to relax. It felt like the beginning of another shift after getting home.
"The baby would be eagerly awaiting me, and my mother's guilt was at its peak, so even though I was physically exhausted, I would still want to give him my time. Since I could never pick my baby up or get him or his meals ready for daycare, I felt guilty asking my husband to do more,” she told HealthandMe.
Shopping for groceries, refilling the baby’s necessities, making sure food is cooked as per everyone’s taste, and ensuring the baby’s routine isn’t disturbed are major responsibilities of most mothers.
“For a new-age mother, every day is a battle between love and responsibility. She meets deadlines with sleepless eyes and hugs her child with a tired heart. Judged at work, questioned at home -- yet she shows up. Not perfect, not rested, but relentless,” said Shivangi (name changed), an IT professional from Delhi.
While a woman’s quiet strength is often marked as victory, facing warzone-like situations every day -- from boardrooms to bedtime stories, meeting deadlines and doctor visits, balancing ambition, and affection -- takes a heavy toll on her mental and physical health.
HealthandMe spoke to Mimansa Singh Tanwar, Clinical Psychologist and Head of the Fortis School Mental Health Program at Fortis Healthcare, on the struggles of new mothers.
“New mothers often find themselves stretched thin while balancing the constant nurturing needs of the child and trying to realign their life with a change in their self-identity. This is a period of huge transition, both emotionally and physically, where new mothers tend to experience feelings of guilt for not being able to do enough for the child or not doing it the ‘right’ way. They often find themselves divided between work and the child’s needs once they resume work. It’s important to be gentle with yourself and accept that you don’t have to do everything perfectly,” Tanwar said.
“Being a mother is itself a moment of pure joy, but for many new mothers, it is also the beginning of a relentless balancing act. There are significant underlying hormonal and neurochemical changes that affect mood and behavior. Sleepless nights, multiple feeding schedules, household expectations, multitasking, and trying to match the ‘ideal perfect mother’ image can have a significant impact on the mind.
"Mothers often put their own needs quietly at the bottom of the list, which affects their overall well-being,” Dr. Sameer Malhotra, Principal Director - Department of Mental Health and Behavioral Sciences, Max Super Specialty Hospital, Saket, told HealthandMe.
Is There a Motherhood Penalty?
Several studies have pointed out how returning to the workplace as a new mother can be a vulnerable time for women. Many are likely to face baby blues, characterized by feeling weepy or anxious. Maternal labor force participation also sees a dip after motherhood.
A 2021 study published in the Journal of Development Economics showed that motherhood caused a sharp decline in employment in Chile, with 38 percent of working women leaving the workforce and 37 percent still out a decade later.
Global estimates by UN Women and the International Labor Organization (ILO) showed that more than 2 million mothers left the labor force in 2020.
During the pandemic, about 113 million women aged 25–54 with partners and small children were out of the workforce in 2020. This figure is astonishing, particularly when compared to their male peers (13 million of whom were out of the workforce, up from 8 million before COVID-19).
A 2007 study published in the American Journal of Sociology found that mothers face penalties in hiring, starting salaries, and perceived competence, while fathers can benefit from being a parent. Mothers were six times less likely than childless women and 3.35 times less likely than childless men to be recommended for hire. Mothers were also recommended a 7.9 percent lower starting salary than non-mothers.
How Mothers Can Help Themselves
Tanwar urged women to “be gentle with yourself and accept that you don’t have to do everything perfectly.”
Other measures include:
- Setting small, realistic goals
- Resting whenever possible
- Asking for help
- Sharing responsibilities with family members
- Staying connected with supportive family or friends
- Talking openly about your feelings to ease the load
“Simple self-care, even a few quiet moments each day, helps restore calm and energy. It is important to remember that looking after yourself is a key part of caring well for your baby,” Tanwar said.
Karnataka’s Social Media Ban To Help Children Find Life Beyond Screens

Credit: Canva
Chief Minister Siddaramaiah’s announcement during his presentation of the Karnataka State Budget 2026-27, proposing a ban on social media for children under 16 years of age, has sparked intense interest among parents and professionals alike. As the first state in India to attempt such a sweeping measure, the government has invited us to reflect upon this proposal.
We are in an age where technological advancements have blurred the lines between online and offline worlds, blending them seamlessly. While this is the norm in the world of adults, it has silently reshaped childhood with increased screentime.
Concerns about digital dependency, anxiety disorders in children, and reduced focus in academic and non-academic tasks have already made it to research papers and therapy rooms.
But Karnataka has now shifted the focus from debate to discussion and action. While a ban may reduce certain risks of social media exposure, children’s psychological needs like social connection, belonging, peer group and individual identity, besides guidance, must be nurtured if such protections are to be meaningful.
The Pediatric Perspective: A Medical Minefield
From a psychological perspective, the idea of an age-based social media ban is both promising and complex. On the brighter side, reducing screen usage can help address problems of poor sleep schedules, heightened anxiety, and trouble concentrating in studies or tasks. These problems have become increasingly common among not only adolescents, but very young children too.
However, age alone cannot be used as the single measure of readiness to implement this proposal. Two children of the same age may differ vastly in maturity levels, coping skills, and the ability to use technology responsibly.
The deeper issue is not simply “how much time” children spend online, but “what they do there”. Creative exploration, learning, and connection can be enriching, while endless scrolling reinforces dependency and stress.
A ban can reduce such harmful patterns, but in order to have real impact, such a move should be paired with support for children’s psychological needs to help them combat loneliness, handle peer pressure, and guiding their search for identity. Addressing these issues along with the ban can make the protection well intended, more meaningful and long-lasting.
The Silent Crisis: Nocturnal Anxiety And Doom-scrolling
Late-night scrolling (doom scrolling) is more than just a disruption of sleep. It is a psychological trigger for worry and overthinking. In the quiet of the night, children are left alone with a flood of unfiltered information, which can heighten anxiety, and unwanted exposure to inappropriate content.
An effective way to combat the dangers of unsupervised social media access could be “digital sundowning” i.e. setting clear screen time guidelines for children. Families can create screen-free zones, especially in bedrooms, bathrooms, and at dining tables, or create “phone parking zones” – a specific place in the house to keep all phones so no one is carrying them around all the time. This can encourage children towards healthier routines.
Unlike government-imposed bans, household practices can set healthy and firm boundaries, reinforce self-regulation and reduce the anxiety that comes from constant connectivity and information overload.
Symptoms In The Clinic: Beyond The Screen
In therapy rooms and schools, counsellors are addressing more and more concerns about children and adolescents spending excessive time with their screens. Some of the common ones are highlighted here:
- Social Isolation in Hyper Connectivity: Children may appear socially active online but withdraw from face-to-face interactions, leaving them paradoxically isolated.
- Body Image Concerns: Exposure to curated images on social media can fuel anxiety about appearance among growing children, who are already socially awkward during adolescence. This goes beyond normal teenage insecurity and can spiral into unhealthy self-image or self-criticism.
- Academic Fatigue: Digital content trains the brain to expect constant novelty and quick changes within a short time span of seconds or minutes, which makes textbooks and traditional classroom driven problem-solving feel slow and tiring. This leads to academic fatigue, where children struggle to sustain focus for deeper learning.
- Fear of Missing Out (FOMO): Constant checking of devices reflects a deep-seated need for validation and belonging. FOMO keeps children’s nervous systems on a constant loop of high alert, thus undermining emotional stability.
What Comes Next: The Prioritization Framework
For this ban to have a lasting impact, it needs to draw on psychological principles. Restrictions work best when paired with meaningful alternatives, as children are known to engage positively when they feel supported rather than restricted or scolded. A framework needs to be set up where learning and guidance is prioritized and alternatives offered are strengthened. Some pointers:
Digital Literacy in Schools: Children should be taught not only to limit screen time but also to understand how online platforms work. Lessons on algorithms, advertising, and curated content help them understand and evaluate what they see, so they become more resilient to digital influence.
Parental Guidance Programs: As with other trained behaviors, parents play a central role in shaping healthy digital habits too. Guidance programs can provide resources and strategies for families to showcase balanced device use. When adults demonstrate mindful online usage and behavior, children are likely to follow.
Physical and Social Alternatives: If digital spaces are restricted, offline opportunities must be strengthened. Sports, arts, and community activities help children gain a sense of belonging and enjoyment beyond screens, thus building confidence and social skills in real life.
Collaboration with Tech Companies: Lasting change requires cooperation of technology providers and social media platforms. Stricter age verification systems and design changes at the source are needed, rather than placing usage responsibility on children. By remodeling platforms, risk of unsupervised penetration of digital content can be mitigated so children may still be allowed safe, and age appropriate engagement on social media.
As Karnataka moves into this new territory, one thing is certain – the intention is noble. However, the execution of such a ban will require a fine balance of protection and empowerment, as it attempts to re-imagine childhood experiences in an age where the “virtual” and the “real” are meshed together. Whether this becomes a guiding model for the rest of the country, will depend entirely on how thoughtfully it is carried out.
Karnataka’s proposed ban is a bold first step, but its true impact will depend on how parents, teachers, and policymakers align on this, because healthy childhoods thrive not on restrictions, but through resilience, support, guidance, and strong offline connections that nurture growth and belonging.
Giant 99th Percentile Baby Of 5.9Kg Born In New York Has Taken The Internet By Storm

Credits: Canva
A giant baby weighing 5.9 kg was born to a mother in New York. She was left in shock and amaze when she saw that she had delivered a boy much bigger than she expected. The newborn baby weighed almost twice as much as an average baby. The baby is born to Terrica and Shawn on January 31 in Cayuga Medical Center. His weigh has made him the heaviest baby ever born at the Ithaca-based hospital, reported the NY Post.
The mother of four said she knew her son would be a little heavy, however did not know he would be this big. She said he is already wearing three-to-six month old baby clothes and diaper. She feels like she has given birth to a three-month-old.
The hospital also posted a photo of the baby on Facebook, comparing him with another newborn baby alongside. The other baby too was born on the same day, whose name is Margot and weighs only 1.8 kg.
Robyn Torgalski, System Director of Maternal and Child Health at Centralus Health, described the two births as a powerful reminder that every newborn and every birth story is unique. She noted that whether a baby weighs four pounds or thirteen, the medical team is fully equipped to deliver the highest level of care to both mother and child. Torgalski added that she is proud of the maternity services at Cayuga Health and feels privileged to support families during such an important life event.
Read: 99th Percentile Baby: What It Means, Risks, And What Parents Should Know
Giant Babies: All About Them
As per the Guinness World Records, the heaviest recorded baby ever was 9.97 kg born in Italy in 1955.
Dr Sermed Mezher, a digital health content creator, and a London based GP, shared: "Babies in the womb who measure in the 99th percentile for weight are referred to as macrosomic baby, meaning they are significantly larger than average for their gestational age. While most macrosomic babies are healthy, their larger size can increase the risk of certain complications during pregnancy and delivery."
What Does It Mean To Be A 99th Percentile Baby?
Babies in the 99th percentile for weight are larger than 99% of babies at the same gestational age. This may lead to birth complications such as shoulder dystocia—when the baby’s shoulders become stuck during delivery—or increase the likelihood of cesarean section. Mothers may also experience a higher risk of perineal tearing, postpartum hemorrhage, and greater pregnancy weight gain. Contributing factors include maternal diabetes, genetics, or excess weight gain during pregnancy.
This larger birth size is medically categorized under fetal macrosomia, which refers to babies in the top 10% of weight for gestational age—with the 99th percentile representing the most extreme cases.
What Causes A Baby To Be a 99th Percentile Baby?
While we do not know the cause in this case, there are certain reason a baby may fall into the category, which includes:
- You have a large fundal height (a measurement of fetal growth)
- Significant weight gain during pregnancy
- Gestational diabetes or pre-existing diabetes
- History of delivering large babies
- Prolonged pregnancy past due date
- Parental genetics (you were a large baby yourself)
© 2024 Bennett, Coleman & Company Limited

